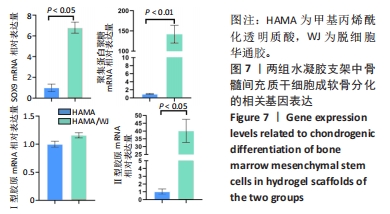
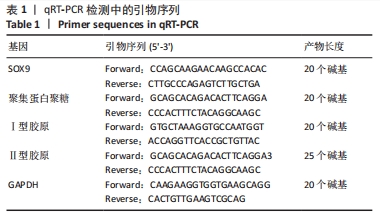
[1] JIANG S, TIAN G, YANG Z, et al. Enhancement of acellular cartilage matrix scaffold by Wharton’s jelly mesenchymal stem cell-derived exosomes to promote osteochondral regeneration. Bioact Mater. 2021;6(9):2711-2728.
[2] MADRY H, GRÜN UW, KNUTSEN G. Cartilage repair and joint preservation: medical and surgical treatment options. Dtsch Arztebl Int. 2011;108(40):669-677.
[3] YANG Z, CAO F, LI H, et al. Microenvironmentally optimized 3D-printed TGFβ-functionalized scaffolds facilitate endogenous cartilage regeneration in sheep. Acta Biomater. 2022;150:181-198.
[4] DALY AC, FREEMAN FE, GONZALEZ-FERNANDEZ T, et al. 3D Bioprinting for Cartilage and Osteochondral Tissue Engineering. Adv Healthc Mater, 2017;6(22).doi: 10.1002/adhm.201700298.
[5] LEE A, HUDSON AR, SHIWARSKI DJ, et al. 3D bioprinting of collagen to rebuild components of the human heart. Science. 2019;365(6452): 482-487.
[6] WANG S, ZHAO S, YU J, et al. Advances in Translational 3D Printing for Cartilage, Bone, and Osteochondral Tissue Engineering. Small. 2022; 18(36):e2201869.
[7] LIU Y, PENG L, LI L, et al. 3D-bioprinted BMSC-laden biomimetic multiphasic scaffolds for efficient repair of osteochondral defects in an osteoarthritic rat model. Biomaterials. 2021;279:121216.
[8] SCHUURMANS C, MIHAJLOVIC M, HIEMSTRA C, et al. Hyaluronic acid and chondroitin sulfate (meth)acrylate-based hydrogels for tissue engineering: Synthesis, characteristics and pre-clinical evaluation. Biomaterials. 2021;268:120602.
[9] LEE JM, YEONG WY. Design and Printing Strategies in 3D Bioprinting of Cell-Hydrogels: A Review. Adv Healthc Mater. 2016;5(22):2856-2865.
[10] JONIDI SHARIATZADEH F, SOLOUK A, BAGHERI KHOULENJANI S, et al. Injectable and reversible preformed cryogels based on chemically crosslinked gelatin methacrylate (GelMA) and physically crosslinked hyaluronic acid (HA) for soft tissue engineering. Colloids Surf B Biointerfaces. 2021;203:111725.
[11] YANG C, WANG X, YAO X, et al. Hyaluronic acid nanogels with enzyme-sensitive cross-linking group for drug delivery. J Control Release. 2015; 205:206-217.
[12] SCOTT JM, WILKINSON R. Further studies on the umbilical cord and its water content. J Clin Pathol. 1978;31(10):944-948.
[13] CHAN RW, RODRIGUEZ ML, MCFETRIDGE PS. The human umbilical vein with Wharton’s jelly as an allogeneic, acellular construct for vocal fold restoration. Tissue Eng Part A. 2009;15(11):3537-3546.
[14] VALIYAVEETTIL M, ACHUR RN, MUTHUSAMY A, et al. Characterization of chondroitin sulfate and dermatan sulfate proteoglycans of extracellular matrices of human umbilical cord blood vessels and Wharton’s jelly. Glycoconj J. 2004;21(6):361-375.
[15] WU J, FU L, YAN Z, et al. Hierarchical porous ECM scaffolds incorporating GDF-5 fabricated by cryogenic 3D printing to promote articular cartilage regeneration. Biomater Res. 2023;27(1):7.
[16] GOGIEL T, BAŃKOWSKI E, JAWORSKI S. Proteoglycans of Wharton’s jelly. Int J Biochem Cell Biol. 2003;35(10):1461-1469.
[17] XU HQ, LIU JC, ZHANG ZY, et al. A review on cell damage, viability, and functionality during 3D bioprinting. Mil Med Res. 2022;9(1):70.
[18] SHEN Y, TANG H, HUANG X, et al. DLP printing photocurable chitosan to build bio-constructs for tissue engineering. Carbohydr Polym. 2020; 235:115970.
[19] 殷瀚,吴江,严子能,等.基于低温沉积打印技术构建分级多孔脱细胞华通胶支架[J].中国医药生物技术,2022,17(6):488-496.
[20] 杨振,李浩,付力伟,等. 3D生物打印负载转化生长因子β3的软骨复合支架[J].中国组织工程研究,2021,25(34):5445-5452.
[21] LEE S, SANI ES, SPENCER AR, et al. Human-Recombinant-Elastin-Based Bioinks for 3D Bioprinting of Vascularized Soft Tissues. Adv Mater. 2020;32(45):e2003915.
[22] 吴江,殷瀚,严子能,等.低温沉积3D打印负载基质细胞衍生因子1的分级多孔软骨复合支架[J].中国组织工程研究,2023,27(30): 4776-4782.
[23] SHI W, SUN M, HU X, et al. Structurally and Functionally Optimized Silk-Fibroin-Gelatin Scaffold Using 3D Printing to Repair Cartilage Injury In Vitro and In Vivo. Adv Mater. 2017;29(29).doi: 10.1002/adma. 201701089.
[24] RAIO L, CROMI A, GHEZZI F, et al. Hyaluronan content of Wharton’s jelly in healthy and Down syndrome fetuses. Matrix Biol. 2005;24(2):166-174.
[25] LIU J, LI L, SUO H, et al. 3D printing of biomimetic multi-layered GelMA/nHA scaffold for osteochondral defect repair. ScienceDirect. 2019;171:107708-107708.
[26] QI J, CHEN A, YOU H, et al. Proliferation and chondrogenic differentiation of CD105-positive enriched rat synovium-derived mesenchymal stem cells in three-dimensional porous scaffolds. Biomed Mater. 2011;6(1):015006.
[27] LIU L, XIONG Z, YAN YN, et al. Porous morphology, porosity, mechanical properties of poly(α-hydroxy acid)–tricalcium phosphate composite scaffolds fabricated by low-temperature deposition. J Biomed Mater Res A. 2007;82A(3):618-629.
[28] MIAO X, TAN DM, LI J, et al. Mechanical and biological properties of hydroxyapatite/tricalcium phosphate scaffolds coated with poly(lactic-co-glycolic acid). Acta Biomater. 2008;4(3):638-645.
[29] CHEN M, LI Y, LIU S, et al. Hierarchical macro-microporous WPU-ECM scaffolds combined with Microfracture Promote in Situ Articular Cartilage Regeneration in Rabbits. Bioact Mater. 2021;6(7):1932-1944.
[30] TOLABI H, DAVARI N, KHAJEHMOHAMMADI M, et al. Progress of Microfluidic Hydrogel-Based Scaffolds and Organ-on-Chips for the Cartilage Tissue Engineering. Adv Mater. 2023;35(26):e2208852.
[31] GRIFFIN DR, ARCHANG MM, KUAN CH, et al. Activating an adaptive immune response from a hydrogel scaffold imparts regenerative wound healing. Nat Mater. 2021;20(4):560-569.
[32] JIANG G, LI S, YU K, et al. A 3D-printed PRP-GelMA hydrogel promotes osteochondral regeneration through M2 macrophage polarization in a rabbit model. Acta Biomater. 2021;128:150-162.
[33] SHI W, FANG F, KONG Y, et al. Dynamic hyaluronic acid hydrogel with covalent linked gelatin as an anti-oxidative bioink for cartilage tissue engineering. Biofabrication. 2021;14(1). doi: 10.1088/1758-5090/ac42de.
[34] FENG Y, XIAO K, CHEN J, et al. Immune-microenvironment modulatory polyurethane-hyaluronic acid hybrid hydrogel scaffolds for diabetic wound treatment. Carbohydr Polym. 2023;320:121238.
[35] GUO C, CAO Z, PENG Y, et al. Subchondral bone-inspired hydrogel scaffold for cartilage regeneration. Colloids Surf B Biointerfaces. 2022;218:112721.
[36] LI M, YIN H, YAN Z, et al. The immune microenvironment in cartilage injury and repair. Acta Biomater. 2022;140:23-42.
[37] YANG Z, ZHAO T, GAO C, et al. 3D-Bioprinted Difunctional Scaffold for In Situ Cartilage Regeneration Based on Aptamer-Directed Cell Recruitment and Growth Factor-Enhanced Cell Chondrogenesis. ACS Appl Mater Interfaces. 2021;13(20):23369-23383.
[38] HULL SM, BRUNEL LG, HEILSHORN SC. 3D Bioprinting of Cell-Laden Hydrogels for Improved Biological Functionality. Adv Mater. 2022;34(2):e2103691.
[39] KRUJATZ F, DANI S, WINDISCH J, et al. Think outside the box: 3D bioprinting concepts for biotechnological applications -recent developments and future perspectives. Biotechnol Adv. 2022;58: 107930.
[40] XU J, ZHANG M, DU W, et al. Chitosan-based high-strength supramolecular hydrogels for 3D bioprinting. Int J Biol Macromol. 2022;219:545-557.
[41] LI M, SUN D, ZHANG J, et al. Application and development of 3D bioprinting in cartilage tissue engineering. Biomater Sci. 2022;10(19): 5430-5458.
|