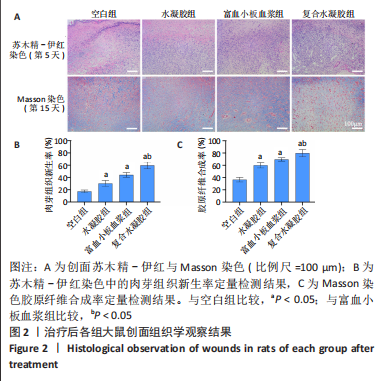
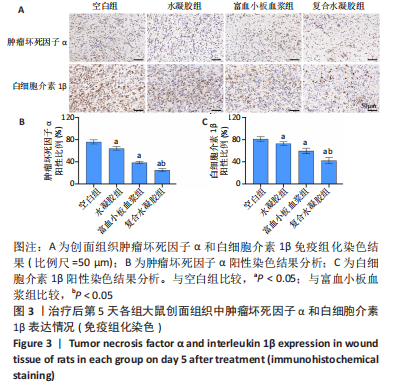
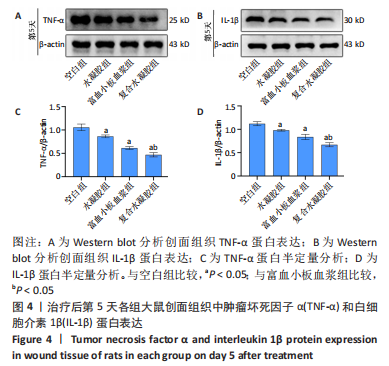
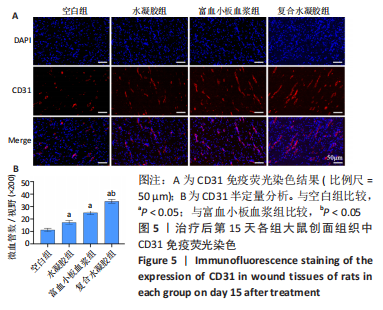
[1] LIU C, GE HM, LIU BH, et al. Targeting pericyte-endothelial cell crosstalk by circular RNA-cPWWP2A inhibition aggravates diabetes-induced microvascular dysfunction. Proc Natl Acad Sci U S A. 2019; 116(15):7455-7464.
[2] SHI Q, QIAN Z, LIU D, et al. GMSC-Derived Exosomes Combined with a Chitosan/Silk Hydrogel Sponge Accelerates Wound Healing in a Diabetic Rat Skin Defect Model. Front Physiol. 2017;8:904.
[3] Zarei F, Soleimaninejad M. Role of growth factors and biomaterials in wound healing. Artif Cells Nanomed Biotechnol. 2018;46(sup1):906-911.
[4] MARTÍ-CARVAJAL AJ, GLUUD C, NICOLA S, et al. Growth factors for treating diabetic foot ulcers. Cochrane Database Syst Rev. 2015; 2015(10):CD008548.
[5] SHEN YI, CHO H, PAPA AE, et al. Engineered human vascularized constructs accelerate diabetic wound healing. Biomaterials. 2016;102: 107-119.
[6] SEIDEL D, STORCK M, LAWALL H, et al. Negative pressure wound therapy compared with standard moist wound care on diabetic foot ulcers in real-life clinical practice: results of the German DiaFu-RCT. BMJ Open. 2020;10(3):e026345.
[7] HAN G, CEILLEY R. Chronic Wound Healing: A Review of Current Management and Treatments. Adv Ther. 2017;34(3):599-610.
[8] CAKIN MC, OZDEMIR B, KAYA-DAGISTANLI F, et al. Evaluation of the in vivo wound healing potential of the lipid fraction from activated platelet-rich plasma. Platelets. 2020;31(4):513-520.
[9] HESSELER MJ, SHYAM N. Platelet-rich plasma and its utility in the treatment of acne scars: A systematic review. J Am Acad Dermatol. 2019;80(6):1730-1745.
[10] SHAIK JA, ESTHARABADI N, FARAH RS, et al. Heterogeneity in amount of growth factors secreted by platelets in platelet-rich plasma samples from alopecia patients. Exp Dermatol. 2020;29(10):1004-1011.
[11] OUDELAAR BW, PEERBOOMS JC, HUIS IN ‘T VELD R, et al. Concentrations of Blood Components in Commercial Platelet-Rich Plasma Separation Systems: A Review of the Literature. Am J Sports Med. 2019;47(2):479-487.
[12] SUTHAR M, GUPTA S, BUKHARI S, et al. Treatment of chronic non-healing ulcers using autologous platelet rich plasma: a case series. J Biomed Sci. 2017;24(1):16.
[13] LI S, DONG Q, PENG X, et al. Self-Healing Hyaluronic Acid Nanocomposite Hydrogels with Platelet-Rich Plasma Impregnated for Skin Regeneration. ACS Nano. 2022;16(7):11346-11359.
[14] LIU X, YANG Y, NIU X, et al. An in situ photocrosslinkable platelet rich plasma - Complexed hydrogel glue with growth factor controlled release ability to promote cartilage defect repair. Acta Biomater. 2017;62:179-187.
[15] CAO J, WU P, CHENG Q, et al. Ultrafast Fabrication of Self-Healing and Injectable Carboxymethyl Chitosan Hydrogel Dressing for Wound Healing. ACS Appl Mater Interfaces. 2021;13(20):24095-24105.
[16] LV X, LIU Y, SONG S, et al. Influence of chitosan oligosaccharide on the gelling and wound healing properties of injectable hydrogels based on carboxymethyl chitosan/alginate polyelectrolyte complexes. Carbohydr Polym. 2019;205:312-321.
[17] ALINEJAD Y, ADOUNGOTCHODO A, HUI E, et al. An injectable chitosan/chondroitin sulfate hydrogel with tunable mechanical properties for cell therapy/tissue engineering. Int J Biol Macromol. 2018;113:132-141.
[18] SHARMA S, SWETHA KL, ROY A. Chitosan-Chondroitin sulfate based polyelectrolyte complex for effective management of chronic wounds. Int J Biol Macromol. 2019;132:97-108.
[19] ZHOU L, FAN L, ZHANG FM, et al. Hybrid gelatin/oxidized chondroitin sulfate hydrogels incorporating bioactive glass nanoparticles with enhanced mechanical properties, mineralization, and osteogenic differentiation. Bioact Mater. 2020;6(3):890-904.
[20] LI H, CHENG F, WEI X, et al. Injectable, self-healing, antibacterial, and hemostatic N,O-carboxymethyl chitosan/oxidized chondroitin sulfate composite hydrogel for wound dressing. Mater Sci Eng C Mater Biol Appl. 2021;118:111324.
[21] FAN M, MA Y, TAN H, et al. Covalent and injectable chitosan-chondroitin sulfate hydrogels embedded with chitosan microspheres for drug delivery and tissue engineering. Mater Sci Eng C Mater Biol Appl. 2017; 71:67-74.
[22] AYUK SM, ABRAHAMSE H, HOURELD NN. The Role of Matrix Metalloproteinases in Diabetic Wound Healing in relation to Photobiomodulation. J Diabetes Res. 2016;2016:2897656.
[23] YANG S, HU L, HAN R, et al. Neuropeptides, Inflammation, Biofilms, and diabetic Foot Ulcers. Exp Clin Endocrinol Diabetes. 2022;130(7): 439-446.
[24] QIAN Z, WANG H, BAI Y, et al. Improving Chronic Diabetic Wound Healing through an Injectable and Self-Healing Hydrogel with Platelet-Rich Plasma Release. ACS Appl Mater Interfaces. 2020;12(50):55659-55674.
[25] TOTTOLI EM, DORATI R, GENTA I, et al. Skin Wound Healing Process and New Emerging Technologies for Skin Wound Care and Regeneration. Pharmaceutics. 2020;12(8):735.
[26] ZHANG Y, WANG ZL, DENG ZP, et al. Emerging Delivery Strategies of Platelet-Rich Plasma with Hydrogels for Wound Healing. Adv Polym Technol. 2022;(2022):5446291.
[27] ZHAO R, LIANG H, CLARKE E, et al. Inflammation in Chronic Wounds. Int J Mol Sci. 2016;17(12):2085.
[28] LIAO X, LIANG JX, LI SH, et al. Allogeneic Platelet-Rich Plasma Therapy as an Effective and Safe Adjuvant Method for Chronic Wounds. J Surg Res. 2020;246:284-291.
[29] ORTOLANI E, GUERRIERO M, COLI A, et al. Effect of PDGF, IGF-1 and PRP on the implant osseointegration. An histological and immunohistochemical study in rabbits. Ann Stomatol (Roma). 2014; 5(2):66-68.
[30] ZHANG X, YAO D, ZHAO WY, et al. Engineering platelet-rich plasma based dual-network hydrogel as a bioactive wound dressing with potential clinical translational value. Adv Funct Mater. 2020;31(8):2009258.
[31] EVERTS P, ONISHI K, JAYARAM P, et al. Platelet-Rich Plasma: New Performance Understandings and Therapeutic Considerations in 2020. Int J Mol Sci. 2020;21(20):7794.
[32] IRMAK G, GÜMÜŞDERELIOĞLU M. Patients- and tissue-specific bio-inks with photoactivated PRP and methacrylated gelatin for the fabrication of osteochondral constructs. Mater Sci Eng C Mater Biol Appl. 2021; 125:112092.
[33] GROWNEY EA, LINDER HR, GARG K, et al. Bio-conjugation of platelet-rich plasma and alginate through carbodiimide chemistry for injectable hydrogel therapies. J Biomed Mater Res B Appl Biomater. 2020;108(5): 1972-1984.
[34] MEDEIROS LHC, VASCONCELOS BMF, SILVA MB, et al. Chondroitin sulfate from fish waste exhibits strong intracellular antioxidant potential. Braz J Med Biol Res. 2021;54(10):e10730.
[35] CHANG SH, WU CH, TSAI GJ. Effects of chitosan molecular weight on its antioxidant and antimutagenic properties. Carbohydr Polym. 2018;181:1026-1032.
[36] LIU F, LI HY, WANG Z, et al. Carboxymethyl chitosan reduces inflammation and promotes osteogenesis in a rabbit knee replacement model. BMC Musculoskelet Disord. 2020;21(1):775.
[37] KHARKAR PM, KIICK KL, KLOXIN AM. Designing degradable hydrogels for orthogonal control of cell microenvironments. Chem Soc Rev. 2013;42(17):7335-7372.
[38] CHEN YR, ZHOU ZX, ZHANG JY, et al. Low-Molecular-Weight Heparin-Functionalized Chitosan-Chondroitin Sulfate Hydrogels for Controlled Release of TGF-β3 and in vitro Neocartilage Formation. Front Chem. 2019;7:745.
[39] LI HL, LIU XT, HUANG SM, et al. Repair function of essential oil from Crocodylus Siamensis (Schneider, 1801) on the burn wound healing via up-regulated growth factor expression and anti-inflammatory effect. J Ethnopharmacol. 2021;264:113286.
[40] MARTIN P, NUNAN R. Cellular and molecular mechanisms of repair in acute and chronic wound healing. Br J Dermatol. 2015;173(2):370-378.
[41] KAKUDO N, MORIMOTO N, OGAWA T, et al. Angiogenic effect of platelet-rich plasma combined with gelatin hydrogel granules injected into murine subcutis. J Tissue Eng Regen Med. 2017;11(7):1941-1948.
[42] WEI S, XU P, YAO Z, et al. A composite hydrogel with co-delivery of antimicrobial peptides and platelet-rich plasma to enhance healing of infected wounds in diabetes. Acta Biomater. 2021;24:205-218. |