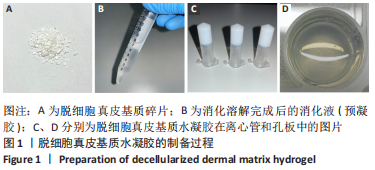
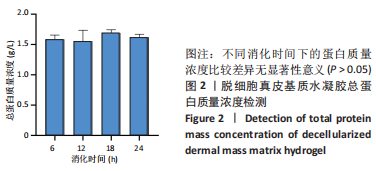
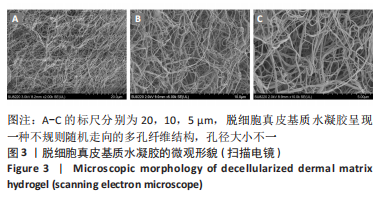
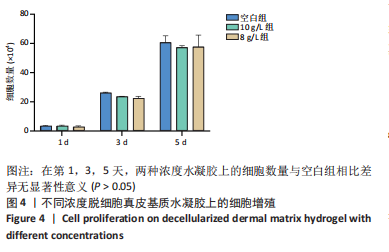
[1] BAYER IS. Hyaluronic Acid and Controlled Release: A Review. Molecules. 2020;25(11):2649.
[2] CHOW KV, URMAN DS, CABRAL ES, et al. Hyaluronic Acid Filler Incidentally Found During Mohs Micrographic Surgery: Observations in 36 Patients Regarding Skin Depth, Degradation Size, and Estimated Persistence Time. Dermatol Surg. 2022;48(4):401-405.
[3] 杨彪,郭学平,臧恒昌,等.交联透明质酸凝胶修饰度的测定方法研究进展[J].药物生物技术,2015,22(2):177-180.
[4] TANG S, CHI K, XU H, et al. A covalently cross-linked hyaluronic acid/bacterial cellulose composite hydrogel for potential biological applications. Carbohydr Polym. 2021;252:117123.
[5] ZERBINATI N, SOMMATIS S, MACCARIO C, et al. Toward Physicochemical and Rheological Characterization of Different Injectable Hyaluronic Acid Dermal Fillers Cross-Linked with Polyethylene Glycol Diglycidyl Ether. Polymers (Basel). 2021;13(6):948.
[6] KENNE L, GOHIL S, NILSSON EM, et al. Modification and cross-linking parameters in hyaluronic acid hydrogels--definitions and analytical methods. Carbohydr Polym. 2013;91(1):410-418.
[7] RZANY B, CONVERSET-VIETHEL S, HARTMANN M, et al. Efficacy and Safety of 3 New Resilient Hyaluronic Acid Fillers, Crosslinked With Decreased BDDE, for the Treatment of Dynamic Wrinkles: Results of an 18-Month, Randomized Controlled Trial Versus Already Available Comparators. Dermatol Surg. 2019;45(10):1304-1314.
[8] CECCHI R, SPOTA A, FRATI P, et al. Migrating granulomatous chronic reaction from hyaluronic acid skin filler (Restylane): review and histopathological study with histochemical stainings. Dermatology. 2014;228(1):14-17.
[9] SHOME D, DOSHI K, VADERA S, et al. Delayed hypersensitivity reaction to hyaluronic acid dermal filler post-COVID-19 viral infection. J Cosmet Dermatol. 2021;20(5):1549-1550.
[10] SUN W, GREGORY DA, TOMEH MA, et al. Silk Fibroin as a Functional Biomaterial for Tissue Engineering. Int J Mol Sci. 2021;22(3):1499.
[11] CHEN D, ZHOU X, CHANG L, et al. Hemostatic Self-Healing Hydrogel with Excellent Biocompatibility Composed of Polyphosphate-Conjugated Functional PNIPAM-Bearing Acylhydrazide. Biomacromolecules. 2021; 22(5):2272-2283.
[12] HINDERER S, LAYLAND SL, SCHENKE-LAYLAND K. ECM and ECM-like materials - Biomaterials for applications in regenerative medicine and cancer therapy. Adv Drug Deliv Rev. 2016;97:260-269.
[13] KOU L, SUN R, BHUTIA YD, et al. Emerging advances in P-glycoprotein inhibitory nanomaterials for drug delivery. Expert Opin Drug Deliv. 2018;15(9):869-879.
[14] HOGANSON DM, OWENS GE, MEPPELINK AM, et al. Decellularized extracellular matrix microparticles as a vehicle for cellular delivery in a model of anastomosis healing. J Biomed Mater Res A. 2016;104(7): 1728-1735.
[15] HWANG J, SULLIVAN MO, KIICK KL. Targeted Drug Delivery via the Use of ECM-Mimetic Materials. Front Bioeng Biotechnol. 2020;8:69.
[16] PISHAVAR E, KHOSRAVI F, NASERIFAR M, et al. Multifunctional and Self-Healable Intelligent Hydrogels for Cancer Drug Delivery and Promoting Tissue Regeneration In Vivo. Polymers (Basel). 2021;13(16):2680.
[17] FREYTES DO, MARTIN J, VELANKAR SS, et al. Preparation and rheological characterization of a gel form of the porcine urinary bladder matrix. Biomaterials. 2008;29(11):1630-1637.
[18] WASEEQ UR REHMAN, ASIM M, HUSSAIN S, et al. Hydrogel: A Promising Material in Pharmaceutics. Curr Pharm Des. 2020;26(45):5892-5908.
[19] CASCONE S, LAMBERTI G. Hydrogel-based commercial products for biomedical applications: A review. Int J Pharm. 2020;573:118803.
[20] ALI F, KHAN I, CHEN J, et al. Emerging Fabrication Strategies of Hydrogels and Its Applications. Gels. 2022;8(4):205.
[21] KAMOUN EA, LOUTFY SA, HUSSEIN Y, et al. Recent advances in PVA-polysaccharide based hydrogels and electrospun nanofibers in biomedical applications: A review. Int J Biol Macromol. 2021;187: 755-768.
[22] ARKABAN H, BARANI M, AKBARIZADEH MR, et al. Polyacrylic Acid Nanoplatforms: Antimicrobial, Tissue Engineering, and Cancer Theranostic Applications. Polymers (Basel). 2022;14(6):1259.
[23] STEPANOVSKA J, SUPOVA M, HANZALEK K, et al. Collagen Bioinks for Bioprinting: A Systematic Review of Hydrogel Properties, Bioprinting Parameters, Protocols, and Bioprinted Structure Characteristics. Biomedicines. 2021;9(9):1137.
[24] GOODARZI K, RAO SS. Hyaluronic acid-based hydrogels to study cancer cell behaviors. J Mater Chem B. 2021;9(31):6103-6115.
[25] ZOU Z, ZHANG B, NIE X, et al. A sodium alginate-based sustained-release IPN hydrogel and its applications. RSC Adv. 2020;10(65): 39722-39730.
[26] RAO F, WANG Y, ZHANG D, et al. Aligned chitosan nanofiber hydrogel grafted with peptides mimicking bioactive brain-derived neurotrophic factor and vascular endothelial growth factor repair long-distance sciatic nerve defects in rats. Theranostics. 2020;10(4):1590-1603.
[27] ZHONG G, YAO J, HUANG X, et al. Injectable ECM hydrogel for delivery of BMSCs enabled full-thickness meniscus repair in an orthotopic rat model. Bioact Mater. 2020;5(4):871-879.
[28] VOYTIK-HARBIN SL, BRIGHTMAN AO. Small intestinal submucosa: a tissue derived extracellular matrix that promotes tissue-specifific growth and differentiation of cells in vitro. Tissue Eng. 1998;4(2): 157-174.
[29] GIOBBE GG, CROWLEY C, LUNI C, et al. Extracellular matrix hydrogel derived from decellularized tissues enables endodermal organoid culture. Nat Commun. 2019;10(1):5658.
[30] XU Y, ZHOU J, LIU C, et al. Understanding the role of tissue-specific decellularized spinal cord matrix hydrogel for neural stem/progenitor cell microenvironment reconstruction and spinal cord injury. Biomaterials. 2021;268:120596.
[31] CHEN Z, ZHANG B, SHU J, et al. Human decellularized adipose matrix derived hydrogel assists mesenchymal stem cells delivery and accelerates chronic wound healing. J Biomed Mater Res A. 2021; 109(8):1418-1428.
[32] BORDBAR S, LOTFI BAKHSHAIESH N, KHANMOHAMMADI M, et al. Production and evaluation of decellularized extracellular matrix hydrogel for cartilage regeneration derived from knee cartilage. J Biomed Mater Res A. 2020;108(4):938-946.
[33] YAZDANPANAH G, SHAH R, RAGHURAMA R, et al. In-situ porcine corneal matrix hydrogel as ocular surface bandage. Ocul Surf. 2021;21:27-36.
[34] GOLDFRACHT I, EFRAIM Y, SHINNAWI R, et al. Engineered heart tissue models from hiPSC-derived cardiomyocytes and cardiac ECM for disease modeling and drug testing applications. Acta Biomater. 2019;92:145-159.
[35] FARNEBO S, WOON CY, SCHMITT T, et al. Design and characterization of an injectable tendon hydrogel: a novel scaffold for guided tissue regeneration in the musculoskeletal system. Tissue Eng Part A. 2014; 20(9-10):1550-1561.
[36] FU W, XU P, FENG B, et al. A hydrogel derived from acellular blood vessel extracellular matrix to promote angiogenesis. J Biomater Appl. 2019;33(10):1301-1313.
[37] LEE JS, SHIN J, PARK HM, et al. Liver extracellular matrix providing dual functions of two-dimensional substrate coating and three-dimensional injectable hydrogel platform for liver tissue engineering. Biomacromolecules. 2014;15(1):206-218.
[38] BANKOTI K, RAMESHBABU AP, DATTA S, et al. Dual Functionalized Injectable Hybrid Extracellular Matrix Hydrogel for Burn Wounds. Biomacromolecules. 2021;22(2):514-533.
[39] 梁成宵,古瑞,李婷,等.肝脏基质水凝胶的制备及其细胞相容性研究[J].解放军医学杂志,2018,43(5):409-413.
[40] WOLF MT, DALY KA, BRENNAN-PIERCE EP, et al. A hydrogel derived from decellularized dermal extracellular matrix. Biomaterials. 2012; 33(29):7028-7038.
[41] KADLER KE, HILL A, CANTY-LAIRD EG. Collagen fibrillogenesis: fibronectin, integrins, and minor collagens as organizers and nucleators. Curr Opin Cell Biol. 2008;20(5):495-501.
[42] OZUDOGRU E, ISIK M, EYLEM CC, et al. Decellularized spinal cord meninges extracellular matrix hydrogel that supports neurogenic differentiation and vascular structure formation. J Tissue Eng Regen Med. 2021;15(11):948-963.
|