中国组织工程研究 ›› 2021, Vol. 25 ›› Issue (29): 4735-4742.doi: 10.12307/2021.177
• 组织构建综述 tissue construction review • 上一篇 下一篇
早期脂肪移植物血管化的调节及机制
刘家杰,赵 娴
- 昆明医科大学,云南省昆明市 650031
-
收稿日期:2020-10-31修回日期:2020-11-03接受日期:2020-12-07出版日期:2021-10-18发布日期:2021-07-22 -
通讯作者:赵娴,博士,博士生导师,副教授,昆明医科大学,云南省昆明市 650031 -
作者简介:刘家杰,男,1990 年生,陕西省汉中市人,汉族,昆明医科大学在读硕士,主要从事面部年轻化及脂肪移植相关研究。 -
基金资助:国家自然科学基金(81860343);云南省医学学科带头人(D-2019026)的支持,项目负责人:赵娴
Early vascularization of fat transplantation: regulation and mechanism
Liu Jiajie, Zhao Xian
- Kunming Medical University, Kunming 650031, Yunnan Province, China
-
Received:2020-10-31Revised:2020-11-03Accepted:2020-12-07Online:2021-10-18Published:2021-07-22 -
Contact:Zhao Xian, MD, Doctoral supervisor, Associate professor, Kunming Medical University, Kunming 650031, Yunnan Province, China -
About author:Liu Jiajie, Master candidate, Kunming Medical University, Kunming 650031, Yunnan Province, China -
Supported by:fat transplantation; vascularization; autologous fat; vascular growth factor; stem cells; endothelial progenitor cells; tissue engineering; review
摘要:
文题释义:
自体脂肪移植:是指将从供区通过手术切取或负压抽吸等方式获取的自体脂肪组织,在体外经过一定加工处理(包括漂洗、提纯、添加自体干细胞或异体细胞因子、药物等方式)后移植于受区,以达到增加组织容积、促进组织再生或改善组织质地等目的的组织移植技术。
血管形成:是微血管以出芽的方式从血管床中长出并形成新的血管分支及毛细血管丛,是经过完全分化的内皮细胞增殖、迁移和重塑的结果。
背景:组织移植是整形外科最常用的治疗手段,移植后组织存活的最基本条件是在组织耐缺血时限内建立血液循环,移植物的存活率和质量与血运重建的时间相关。
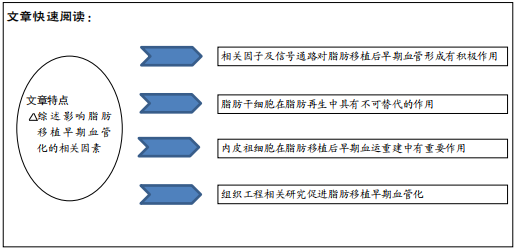
目的:从细胞因子、脂肪干细胞、外泌体、组织工程、信号通路以及不同部位来源脂肪等方向对促进早期脂肪移植物血管化的调节及机制进行综述。
方法:以“fat graft, fat grafting,vascularization,vascularize,cytokines,exosomes,VEGF,ADSCs,EPC,SVF,mechanisms,signal pathway”等为英文检索词;以“脂肪移植;血管化;外泌体;血管内皮生长因子;脂肪干细胞;内皮祖细胞;基质血管成分;信号通路”为中文检索词,检索PubMed、Google Scholar、EMBASE、中国知网、万方、重庆维普等数据库1995年至2020年的相关文献,排除与文章内容无关、低质量或重复性高的文章,最后选取73篇文献进行综述。
结果与结论:①发现添加各种细胞因子或细胞、干细胞、不同部位脂肪细胞的选择、相关信号通路、预处理脂肪、组织工程、外泌体和其他相关处理等,都有助于脂肪移植物早期血管化,从而提高脂肪移植物的存活率;②脂肪干细胞可以通过 VEGF-PLCγ-ERK1/ERK2途径调节血管生成,并抑制炎症反应,通过内皮祖细胞的募集和分化来促进早期血管形成;③不同部位脂肪干细胞在血管化和存活率方面存在差异,使用基质血管组分是提高脂肪移植物存活的高效技术;④脂肪干细胞促进脂肪移植物存活和血管再生的可能机制在于脂肪干细胞的旁分泌产物,其可以促进新血管形成并减轻炎症反应,从而提高脂肪移植物体积保留率。
https://orcid.org/0000-0002-7834-4853 (刘家杰)
中国组织工程研究杂志出版内容重点:组织构建;骨细胞;软骨细胞;细胞培养;成纤维细胞;血管内皮细胞;骨质疏松;组织工程
中图分类号:
引用本文
刘家杰, 赵 娴. 早期脂肪移植物血管化的调节及机制[J]. 中国组织工程研究, 2021, 25(29): 4735-4742.
Liu Jiajie, Zhao Xian. Early vascularization of fat transplantation: regulation and mechanism[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(29): 4735-4742.
2.1.1 内皮祖细胞在血管形成中的作用 内皮祖细胞又被称为血管内皮干细胞,目前被视为成血管必不可少的细胞,它可能来自骨髓、周围组织和脂肪移植物并且有助于其融入周围组织,可以被基质衍生因子1α诱导,在短期内迁移到缺血部位,将其与脂肪来源干细胞共培养,在早期可促进移植脂肪组织再生和血管形成[3]。GEEROMS等[4]证明了脂肪移植物内血管和功能性微血管系统形成的关键细胞是血管内皮细胞。脂肪移植物的血管化需要骨髓来源的内皮祖细胞,它可以促进移植物内有功能的微血管系统形成,并促进其与周围的组织融合[5]。据报道,血管内皮细胞在脂肪移植物内形成有功能的微血管和血管化,并促进其与周围组织融合。这些内皮细胞可起源于脂肪移植体、周围组织或骨髓来源的内皮祖细胞,在3个潜在来源中,内皮祖细胞可能是最重要的,因为它们对移植物新血管形成和存活至关重要。相关研究表明,在健康个体自体脂肪移植后的6个月内,由于早期缺血,多达80%的脂肪移植物会被吸收,研究报道内皮祖细胞可以诱导新血管生成来提高脂肪移植的存活率[5]。因此,脂肪移植后早期内皮祖细胞的增殖、募集和迁移对新血管形成至关重要,是组织工程领域重要的种子细胞。
2.1.2 成纤维细胞在血管形成中的作用 孟文霞等[6]研究证明,活化的成纤维细胞可以调控血管生成,促进血管内皮细胞迁移。另外,成纤维细胞表型的改变受转化生长因子β1调控,其中被标记为α-SMA的肌成纤维细胞可以表达各种促血管生成因子,例如:环氧化酶2、血管内皮生长因子
(vascular endothelial growth factor,VEGF)A 和肝细胞生长因子等,而环氧化酶2又可以促进VEGFA的表达,而VEGFA是组织新生血管形成过程中最重要的细胞因子之一,它可以促进血管内皮细胞增殖、分化并诱导其形成小管样结构[7]。因此,成纤维细胞在转化生长因子β1调控下对血管再生有重要作用。
2.1.3 淋巴细胞在血管形成中的作用 血管生成性T淋巴细胞是可以表达CD31的T细胞亚群,其中CD3+、CD31+阳性T细胞可以显著提高缺血部位血管密度,具有促进血管新生和血管内皮修复的功能。近年来,相关研究显示血管生成性T细胞可以诱导缺血组织血管再生,即通过对血管发生和血管再生的调节来实现血管平衡,从而实现血管再生。
2.1.4 巨噬细胞对血运重建的影响 研究发现基质血管组分细胞是具有高转化生长因子β表达的巨噬细胞[8],巨噬细胞及其极化可引发显性分泌因子水平的变化[9],并影响血源性干细胞浸润,阐明了巨噬细胞对组织血运重建的重要性。
2.1.5 VEGF对成血管的影响 HAMED等[10]发现基质细胞衍生因子1α能够介导内皮祖细胞诱导表达VEGF来刺激血管形成,是因为其具有较强的趋化作用。VEGF是血管生成的主要刺激因子[11-12],如:VEGF165,121,189,206,碱性成纤维细胞生长因子2、胰岛素样生长因子、瘦素、肿瘤坏死因子等,但以VEGF最为重要,其促进血管再生是明确的。
2.1.6 富血小板血浆对血管再生的影响 LEI等[13]发现富含血小板的血浆包含许多生长因子,包括血小板衍生生长因子、转化生长因子β和VEGF都是重要的促血管再生的生长因子,可以促进血管形成[14]。此外,富血小板血浆可以通过其抗菌和抗炎特性促进组织和血管再生[15],已证明富血小板血浆可以促进脂肪干细胞的生长并保持其分化潜能。
2.1.7 碱性成纤维细胞生长因子促进血管再生 碱性成纤维细胞生长因子是成纤维细胞生长因子的一员,它可以调节细胞自我更新、分化和生存,重要的是,有证据支持碱性成纤维细胞生长因子参与了血管生成和血管重塑的过程[16]。研究显示,将2.0 μg的碱性成纤维细胞生长因子与脂肪移植物混合,可以显著提高脂肪移植物的存活率和血管数量[17]。
2.1.8 白细胞介素8在血管形成中的作用 白细胞介素8是一种趋化因子,可以促进内皮细胞迁移和血管形成,增加组织中VEGF和VEGF受体的表达[18],进而促进新生血管形成。BLANDINIERES等[19]研究表明,白细胞介素8可以通过自分泌或旁分泌来刺激内皮集落形成细胞,从而促进血管生成。而白细胞介素8 增强内皮集落形成细胞的血管生成特性取决于其受体的表达。
2.1.9 胰岛素及胰岛素样生长因子1促进血管再生 作为一种多功能激素,胰岛素具有多种生理调节功能,可以促进有丝分裂,促进脂肪细胞增殖分化,研究发现胰岛素是通过胰岛素受体1和胰岛素受体3来促进细胞增殖分化[20]。胰岛素样生长因子1能促进细胞增殖、分化和成熟,具有多种调节功能,但最主要是通过自分泌和旁分泌来发挥作用[21]。
2.1.10 肝细胞生长因子对血管再生的作用 肝细胞生长因子最初被纯化为原代培养中成熟肝细胞的有效促分裂原,是一种与纤溶酶原结构同源的含环蛋白多肽。它是间充质衍生的多效性因子,可调节细胞生长、细胞运动和各种类型细胞形态的发生,被认为是上皮间质相互作用的体液介质,负责胚胎发生发展过程中的形态发生及组织相互作用和器官发生。散射因子、肿瘤细胞毒性因子和肺成纤维细胞衍生的上皮有丝分裂原的表征和分子克隆表明,肝细胞生长因子最近已显示出在体内诱导血管生成[22],在血管生成级联反应中充当旁分泌介质。
2.2 干细胞对脂肪移植物血管化的重要作用
2.2.1 脂肪干细胞调控生长因子对血管生成的影响 基于细胞的组织工程技术已被证明是再生医学最有前途的替代疗法之一。这种方法由反应细胞、支持基质和促进分化、再生的生物活性分子组成的相互作用三联体构成。干细胞凭借可再生能力和多能性将成为一种极有前途的细胞。脂肪干细胞是成人间充质干细胞的丰富来源地,具有分化为脂肪细胞、肌细胞、骨细胞、软骨细胞和内皮细胞等多种细胞类型的能力,在畸形、缺损等疾病中应用极为广泛[23]。CHEN等[24]发现脂肪干细胞可以促进血管化并提高脂肪移植物存活率,其机制是通过脂肪干细胞富集脂肪移植物来抑制炎性细胞因子产生,促进血管生长因子表达,提高脂肪移植物存活率和远期体积保留率。DOORNAERT等[25]研究表明脂肪干细胞可以释放VEGF、肝细胞生长因子等多种促进血管再生的因子来促进血管生成[26],促进脂肪形成,促进移植物滞留,还证明其能在体外引发胶原凝胶中的血管形成。除此之外,脂肪干细胞还可以通过旁分泌作用分泌各种生长因子和外泌体[27- 28],在抗凋亡、抗炎、血管生成和免疫调节中起重要作用[29]。
2.2.2 毛囊干细胞促进血管形成的机制 最新研究发现,毛囊干细胞可以被VEGF165诱导分化为内皮细胞[30],将VEGF165修饰的毛囊干细胞包被在3D支架中移植到体内,可以使种子细胞更好地附着生长,可以明显促进血管化,这种创新性思路为脂肪移植早期血管化提供了理论依据。
2.3 不同部位来源的脂肪组织或脂肪干细胞存在差异 有文献报道,不同部位脂肪干细胞在血管化和存活率方面存在差异,AHMADI等[31]分别比较来自大腿和腹部脂肪干细胞,发现来自腹部脂肪干细胞在向血管内皮细胞分化和分泌VEGF方面有更多的优势,有利于血管生成。其相关机制可能是不同部位脂肪干细胞功能存在差异、不同部位脂肪组织结构和体积也存在差别以及分化为血管内皮细胞的生长因子存在差异。另一项研究表明,从腹部浅表脂肪组织分离出的脂肪干细胞比从其他部位分离出的脂肪干细胞对细胞凋亡的刺激更不敏感。移植后脂肪干细胞的存活是再生移植技术的关键挑战之一,因此,腹部脂肪干细胞的这一特征使该贮藏库成为收获脂肪组织或细胞的有利地点,源自腹部皮下脂肪组织的脂肪干细胞具有更有利的特性,与腹部内脏脂肪组织相比,来自腹部皮下脂肪组织的脂肪干细胞具有更高的增殖速率和更高的成脂潜能[32]。似乎两种脂肪干细胞表型都随深度和位置而变化,因此在选择合适的解剖部位进行脂肪干细胞收获是极为关键的。
2.4 预处理脂肪组织可以提高成活率 文献报道A型肉毒毒素在改善血管形成中有一定作用,SHI等[33]发现A型肉毒毒素治疗的脂肪移植物可以固定周围肌肉,改善血管和成熟脂肪细胞密度、脂肪移植物组织学特征以及移植到肌肉中脂肪移植物的保留率来促进血管生成。CAI等[34]发现他莫昔芬处理腹股沟脂肪可以使UCP-1和VEGF表达增强,影响脂肪代谢并导致脂肪组织褐变,从而改善血管化。据报道,选择性β1阻滞剂美托洛尔有助于脂肪移植血管化,OKYAY等[35]比较了胰岛素、美托洛尔和去铁胺对脂肪移植物存活的影响,结果显示,美托洛尔组脂肪移植成活的脂肪细胞比对照组和胰岛素组多30%(分别为P < 0.05和P < 0.01),差异有统计学意义。因此,选择性β1阻滞剂美托洛尔处理脂肪移植物可以加速脂肪移植物新生血管形成。SARI等[36]发现低剂量甲氨蝶呤可以增加移植脂肪组织血管形成。KIM和LEE等[37]研究发现分数CO2激光预处理可增加脂肪移植后初始阶段VEGF的表达及微血管密度,有助于脂肪移植早期血管化,能有效解决缺血问题,并提高脂肪存活率。但这些方法和技术对机体多少都会存在有害性,最新一项研究表明,迷迭香酸(多酚化合物)是一种抗氧化剂,可以减少脂质过氧化和膜降解,增加脂肪移植物的保留率[38],该研究还表明乙醇对脂肪移植物保留率也有积极作用,这项研究在PubMed和Google Scholar数据库中都未能检索到,如果可预测,将对脂肪移植存活率有重大贡献。
2.5 基质血管组分辅助脂肪移植血管化 近年来,对基质血管部分凝胶(SVF-gel)的研究成果显著。基质血管组分凝胶是一种脂肪组织提取物,富含前再生基质血管组分细胞和细胞外基质蛋白[39]。通过掺入脂肪细胞基质发现其有利于血管生成[40]。ZHU等[41]还发现,基质血管组分通过其血管生成特性促进脂肪移植后移植物的保留,基质血管组分辅助组表现出更高的白细胞介素6和肿瘤坏死因子α表达水平,以及更低水平的白细胞介素10表达。基质血管组分是通过众所周知的促血管生成机制(旁分泌功能和参与新血管再生)以及通过基质血管组分抗炎特性促进脂肪移植物后期的保留(表达和抑制各种细胞因子及转化巨噬细胞表型)来加速血管形成。相关研究显示,通过胶原酶消化从脂肪组织中分离出的基质血管组分移植的脂肪组织比没有基质血管组分移植的脂肪组织存活更好;还证明了脂肪移植物和基质血管组分之间的相互作用可显著延长基质血管组分存活时间,这有助于通过基质血管组分分化为结构细胞来促进脂肪移植物的存活和血管再生[40]。这表明脂肪来源的基质血管组分的移植可通过以下两个步骤来改善局部缺血:①全身性炎症反应从骨髓中转移出炎症细胞;②脂肪来源的干/基质细胞移植和炎症性转移细胞协同诱导血管生成[42]。因此,使用基质血管组分是提高脂肪移植物存活的高效技术。
2.6 组织工程体系
2.6.1 脂肪干细胞联合支架材料的应用 组织工程学和再生医学的最新进展是采用细胞生物支架来模仿天然的体内微环境,将高分子材料作为支架,使种子细胞更好地附着、增殖和迁移。ZHANG等[43]将壳聚糖纳米球作为载体,在载有人脂肪干细胞的胶原-壳聚糖支架中植入含有VEGF的聚乳酸-共-乙醇酸/聚乙二醇(PLGA/PEG)微球,经体外培养,再植入裸鼠体内离散血管蒂周围的隔离室中,8周后发现裸鼠体内血管蒂周围血管密度明显增高。
2.6.2 细胞外基质对脂肪移植血管化的作用 近年来,对细胞外基质的研究也不断深入,细胞外基质是血管壁和脂肪组织的重要结构,内皮细胞的黏附、增殖和迁移都会依赖细胞外基质的生物结构,其最主要的成分是胶原蛋白,具有良好的3D多孔隙结构及化学、物理性能,生物相容性好,且有能力促进细胞黏附和增殖,为种子细胞提供适宜的微环境[44]。利用天然聚合物(例如胶原蛋白或透明质酸)重建而成的生物材料更有潜力。胶原蛋白的良好生物性能和多孔隙结构允许脂肪干细胞在体外和体内分化为成熟的脂肪细胞[45]。另外,失活的天然细胞外基质被认为是用于组织重建的合适支架材料,以组织特异性方式嵌入天然生化刺激物以促进细胞黏附、增殖和分化[46-47]。使用这种方法对小动物(小鼠、兔子和大鼠)进行的体内临床前研究证明了脂肪干细胞的能力,种子细胞植入支架后,可通过结缔组织和新生血管再生形成脂肪组
织[48-49],这对脂肪移植早期血管化有重要意义。
2.7 外泌体对脂肪移植物血管化的促进作用 脂肪干细胞来源外泌体(adipose stem cell derived exosomes,ADSC-exos)是一种新型脂肪因子,其获取方便、低免疫原性、结构稳定、血管化良好、与亲本细胞功能相似,并且在早期(4周前)具有更强的脂肪再生能力[50]。将剪碎的脂肪组织分别与外泌体、源细胞(细胞辅助脂质转移)或生理盐水混合,植入小鼠皮下,10周后,发现外泌体组中的脂肪移植和细胞辅助脂质转移显示出更好的脂肪完整性,更少的油囊肿,并减少了纤维化。对巨噬细胞、炎性因子、血管生成因子、脂肪形成因子和细胞外基质的进一步研究表明,这些外泌体促进血管生成并上调了早期炎症[51-52],而在脂肪移植的中后期,他们发挥了脂肪形成作用,还提高了胶原蛋白合成水平[52]。脂肪间充质干细胞来源的细胞外囊泡能够通过改善血管生成和调节免疫反应来增强脂肪移植物的体积保留能力[53]。脂肪间充质干细胞来源的细胞外囊泡转移到巨噬细胞中,并利用胞外囊泡携带的活性STAT3.28反式激活精氨酸酶1来诱导抗炎性 M2表型。许多研究表明,M2巨噬细胞分泌各种促血管生成因子(例如VEGF)并表达高水平的白细胞介素12,表明 M2巨噬细胞在炎症抑制和伤口愈合中起着重要作用。M2巨噬细胞还具有修复能力,因此也可以提高脂肪移植物的保留率。假设脂肪间充质干细胞来源的细胞外囊泡可以增强M2样的极化激活,这可能在提高脂肪移植物的保留率方面起重要作用。因此,脂肪干细胞来源的外泌体通过上调早期炎症反应和增强血管再生来改善移植物保留。HAN等[54]研究发现来自缺氧处理的人脂肪来源干细胞外泌体通过调节VEGF/VEGFR信号传导而具有更高增强脂肪移植中血管生成的能力及更高的体外和体内成血管能力[55],至少部分通过VEGF/VEGFR信号传导。另外,最新研究显示脂肪干细胞衍生的外泌体对脂肪移植物存活的影响。ADSC-Exos的共移植可以有效地促进脂肪移植物存活、新血管形成,减轻炎症,而缺氧治疗可以进一步增强ADSC-Exos的有益作用[56]。此前,还未有相关文献报道ADSC-Exos共移植在脂肪移植中应用的研究。与细胞辅助脂肪移植术相比,间充质干细胞外来体的共移植具有许多优势,例如非免疫原性、非致瘤性和易储存和运输。因此,ADSC-Exos的共移植是脂肪移植的可行策略。这些特征可使外泌体成为再生医学中最有吸引力的无细胞替代物。
2.8 通过Nrf2和TLR4途径来调节血管生成 自体脂肪移植是一种有效的重建手段,然而,其成功率受到移植物保留不一致、氧化应激、炎症反应以及早期血管化不足的限制。脂肪干细胞可以促进脂肪移植物的存活率,尽管其潜在机制尚不清楚。CHEN等[24]探讨了TLR4和 Nrf2信号通路调节氧化应激和炎症反应对脂肪干细胞体外和体内活力和功能的影响。
2.9 其他 近年来,有学者提出一种新理论,脂肪提取物可以促进血管生成[57]。脂肪提取物是将纳米脂肪通过机械加工处理而成的无细胞结构成分,在理论上可以避免与细胞有关的问题,并且可以更成功地长期储存。利用纳米脂肪和脂肪提取物,一种新的脂肪处理策略,可以通过对脂肪干细胞的促血管生成、抗凋亡和促增殖作用来改善脂肪移植物存活率。

| [1] DOLDERER JH, MEDVED F, HAAS RM, et al. Angiogenesis and vascularisation in adipose tissue engineering. Handchir Mikrochir Plast Chir. 2013;45(2):99-107. [2] TAN SS, ZHAN W, POON CJ, et al. Investigating the effects of non-vascularized free fat transplantation and cell assisted lipotransfer in vivo: A useful animal model. J Plast Reconstr Aesthet Surg. 2016;69(12): 1713-1714. [3] STRASSBURG S, NIENHUESER H, STARK GB, et al. Human adipose-derived stem cells enhance the angiogenic potential of endothelial progenitor cells, but not of human umbilical vein endothelial cells. Tissue Eng Part A. 2013;19(1-2):166-174. [4] GEEROMS M, HAMDI M, HIRANO R, et al. Quality and Quantity-Cultured Murine Endothelial Progenitor Cells Increase Vascularization and Decrease Fibrosis in the Fat Graft. Plast Reconstr Surg. 2019;143(4): 744e-755e. [5] HAMED S, BEN-NUN O, EGOZI D, et al. Treating fat grafts with human endothelial progenitor cells promotes their vascularization and improves their survival in diabetes mellitus. Plast Reconstr Surg. 2012; 130(4): 801-811. [6] 孟文霞,冯璐,刘曙光,等.口腔扁平苔藓活化成纤维细胞对血管内皮细胞迁移及成管特性的影响[J].口腔医学研究,2019,35(8): 806-809. [7] 毛熙贤,王伟,李德卫.TGF-1信号在成纤维细胞促血管生成中作用的研究[J].中国细胞生物学学报,2016,38(5):479-486. [8] CAI J, FENG J, LIU K, et al. Early Macrophage Infiltration Improves Fat Graft Survival by Inducing Angiogenesis and Hematopoietic Stem Cell Recruitment. Plast Reconstr Surg. 2018;141(2):376-386. [9] MASHIKO T, YOSHIMURA K. How does fat survive and remodel after grafting? Clin Plast Surg. 2015;42(2):181-190. [10] HAMED S, EGOZI D, DAWOOD H, et al. The chemokine stromal cell-derived factor-1alpha promotes endothelial progenitor cell-mediated neovascularization of human transplanted fat tissue in diabetic immunocompromised mice. Plast Reconstr Surg. 2013;132(2): 239e-250e. [11] HU Y, JIANG Y, WANG M, et al. Concentrated Growth Factor Enhanced Fat Graft Survival: A Comparative Study. Dermatol Surg. 2018;44(7): 976-984. [12] ORANGES CM, STRIEBEL J, TREMP M, et al. The Preparation of the Recipient Site in Fat Grafting: A Comprehensive Review of the Preclinical Evidence. Plast Reconstr Surg. 2019;143(4):1099-1107. [13] LEI X, LIU H, PANG M, et al. Effects of Platelet-Rich Plasma on Fat and Nanofat Survival:An Experimental Study on Mice. Aesthetic Plast Surg. 2019;43(4):1085-1094. [14] MOTOSKO CC, KHOURI KS, POUDRIER G, et al .Evaluating Platelet-Rich Therapy for Facial Aesthetics and Alopecia: A Critical Review of the Literature. Plast Reconstr Surg. 2018;141(5):1115-1123. [15] FISHER J. Commentary on: Platelet-Rich Plasma and Stem Cells for Hair Growth: A Review of the Literature. Aesthet Surg J. 2020;40(4): NP189-NP190. [16] YAN L, WU W, WANG Z, et al. Comparative study of the effects of recombinant human epidermal growth factor and basic fibroblast growth factor on corneal epithelial wound healing and neovascularization in vivo and in vitro. Ophthalmic Res. 2013;49(3): 150-160. [17] 仇利红,韩悦,郑惠,等.碱性成纤维细胞生长因子联合血管内皮生长因子促进自体脂肪移植成活的动物实验研究[J].中国美容整形外科杂志,2016,27(12):759-762. [18] NIU X, CHEN Y, QI L, et al. Hypoxia regulates angeogenic-osteogenic coupling process via up-regulating IL-6 and IL-8 in human osteoblastic cellsthrough hypoxia-induciblefactor-1alphapathway. Cytokine. 2019; 113:117-127. [19] BLANDINIERES A, HONG X, PHILIPPE A, et al. Interleukin-8 Receptors CXCR1 and CXCR2 Are Not Expressed by Endothelial Colony-forming Cells. Stem Cell Rev Rep. 2020.doi: 10.1007/s12015-020-10081-y. [20] SARFSTEIN R, NAGARAJ K, LEROITH D, et al. Differential effects of insulin and igf1 receptors on erk and akt subcellular distribution in breast cancer cells. Cells. 2019;8(12):1499. [21] 唐 毅,朱国强,蒋军健.胰岛素样生长因子-1促进移植颗粒脂肪组织血管增生的实验研究[J].山西医药杂志,2007,36(7):604-605. [22] MATSUMORI A. Roles of Hepatocyte Growth Factor and Mast Cells in Thrombosis and Angiogenesis. Cardiovasc Drugs Ther. 2004;18(3): 321-326 [23] PLOCK JA,SCHNIDER JT,ZHANG W, et al. Adipose- and bone marrow-derived mesenchymal stem cells prolong graft survival in vascularized composite allotransplantation. Transplantation. 2015;99(9):1765-1773. [24] CHEN X, AN L, GUO Z, et al .Adipose-derived mesenchymal stem cells promote the survival of fat grafts via crosstalk between the Nrf2 and TLR4 pathways. Cell Death Dis. 2016;7(9):e2369. [25] DOORNAERT M, COLLE J, DE MAERE E, et al. Autologous fat grafting: Latest insights. Ann Med Surg (Lond). 2019;37:47-53. [26] KHAN S, VILLALOBOS MA, CHORON RL, et al. Fibroblast growth factor and vascular endothelial growth factor play a critical role in endotheliogenesis from human adipose-derived stem cells. J Vasc Surg. 2017;65(5):1483-1492. [27] KIM H, HAN SH, KOOK YM, et al. A novel 3D indirect co-culture system based on a collagen hydrogel scaffold for enhancing the osteogenesis of stem cells. J Mater Chem B. 2020;8(41):9481-9491. [28] GEEROMS M, HAMDI M, HIRANO R, et al.Quality and quantity–cultured murine endothelial progenitor cells increase vascularization and decrease fibrosis in the fat graft. Plast Reconstr Surg. 2019;143(4): 744e-755e. [29] ZOU ML, LIU SY, SUN ZL, et al. Insights into the role of adipose‐derived stem cells: Wound healing and clinical regenerative potential. J Cell Physiol. 2020. doi: 10.1002/jcp.30019. [30] QUAN R, DU W, ZHENG X, et al.VEGF165 induces differentiation of hair follicle stem cells into endothelial cells and plays a role in in vivo angiogenesis. J Cell Mol Med. 2017;21(8):1593-1604. [31] AHMADI S, MUJAHID AM, KHAN H, Et al. Comparison of Graft Survival between Fat Harvested from Abdomen and Medial Thigh for Facial Contour Deformity: A Randomised Control Trial. J Coll Physicians Surg Pak. 2019;29(5):440-443. [32] TREVOR LV, RICHES-SUMAN K, MAHAJAN AL, et al. Adipose Tissue: A Source of Stem Cells with Potential for Regenerative Therapies for Wound Healing. J Clin Med. 2020;9(7):2161. [33] SHI N, SU Y, GUO S, et al. Improving the Retention Rate of Fat Grafts in Recipient Areas via Botulinum Toxin A Treatment. Aesthet Surg J. 2019;39(12):1436-1444. [34] CAI J, LI B, WANG J, et al. Tamoxifen-Prefabricated Beige Adipose Tissue Improves Fat Graft Survival in Mice. Plast Reconstr Surg. 2018;141(4): 930-940. [35] OKYAY MF, KOMURCU H, BAGHAKI S, et al. Effects of Insulin, Metoprolol and Deferoxamine on Fat Graft Survival. Aesthetic Plast Surg. 2019; 43(3):845-852. [36] SARI E, BAKAR B, SARKARATI B, et al. The effect of low-dose methotrexate on autologous fat graft survival. Turk J Med Sci. 2016; 46(4):1215-1222. [37] KIM SE, LEE JH, KIM TG, et al. Fat Graft Survival After Recipient Site Pretreatment With Fractional Carbon Dioxide Laser. Ann Plast Surg. 2017;79(6):552-557. [38] CIN B, CILOGLU NS, OMAR S, et al. Effect of Rosmarinic Acid and Alcohol on Fat Graft Survival in Rat Model. Aesthetic Plast Surg. 2020;44(1): 177-185. [39] FENG J, HU W, FANAI ML, et al. Mechanical process prior to cryopreservation of lipoaspirates maintains extracellular matrix integrity and cell viability: evaluation of the retention and regenerative potential of cryopreserved fat-derived product after fat grafting. Stem Cell Res Ther. 2019;10(1):283. [40] HE Y, YU X, CHEN Z, et al. Stromal vascular fraction cells plus sustained release VEGF/Ang-1-PLGA microspheres improve fat graft survival in mice. J Cell Physiol. 2019;234(5):6136-6146. [41] ZHU M, XUE J, LU S, et al. Anti-inflammatory effect of stromal vascular fraction cells in fat transplantation. Exp Ther Med. 2019;17(2):1435-1439. [42] KISHIMOTO S, INOUE KI, SOHMA R, et al. Surgical Injury and Ischemia Prime the Adipose Stromal Vascular Fraction and Increase Angiogenic Capacity in a Mouse Limb Ischemia Model. Stem Cells Int. 2020;2020:7219149. [43] ZHANG Q, HUBENAK J, IYYANKI T, et al.Engineering vascularized soft tissue flaps in an animal model using human adipose-derived stem cells and VEGF+PLGA/PEG microspheres on a collagen-chitosan scaffold with a flow-through vascular pedicle. Biomaterials. 2015;73:198-213. [44] Zhu Y, Liu T, Song K, et al. Collagen–chitosan polymer as a scaffold for the proliferation of human adipose tissue-derived stem cells. J Mater Sci: Mater Med. 2009;20(3):799-808. [45] LOUIS F, KITANO S, MANO JF, et al. 3D collagen microfibers stimulate the functionality of preadipocytes and maintain the phenotype of mature adipocytes for long term cultures. Acta Biomater. 2019;84:194-207. [46] ROSSI E, GUERRERO J, APRILE P, et al. Decoration of RGD-mimetic porous scaffolds with engineered and devitalized extracellular matrix for adipose tissue regeneration. Acta Biomater. 2018;73:154-166. [47] SHARATH SS, RAMU J, NAIR SV, et al. Human Adipose Tissue Derivatives as a Potent Native Biomaterial for Tissue Regenerative Therapies. Tissue Eng Regen Med. 2020;17(2):123-140. [48] ITOI Y, TAKATORI M, HYAKUSOKU H, et al. Comparison of readily available scaffolds for adipose tissue engineering using adipose-derived stem cells. J Plast Reconstr Aesthet Surg. 2010;63(5):858-864. [49] NURNBERGER S, LINDNER C, MAIER J, et al. Adipose-tissue-derived therapeutic cells in their natural environment as an autologous cell therapy strategy: the microtissue-stromal vascular fraction. Eur Cell Mater. 2019;37:113-133. [50] SIMONACCI F, BERTOZZI N, GRIECO MP, et al. Autologous fat transplantation for breast reconstruction: A literature review. Ann Med Surg (Lond). Ann Med Surg (Lond). 2016;12:94-100. [51] XIONG M, ZHANG Q, HU W, et al. Exosomes From Adipose-Derived Stem Cells: The Emerging Roles and Applications in Tissue Regeneration of Plastic and Cosmetic Surgery. Front Cell Dev Biol. 2020;8:574223. [52] CHEN B, CAI J, WEI Y, et al. Exosomes Are Comparable to Source Adipose Stem Cells in Fat Graft Retention with Up-Regulating Early Inflammation and Angiogenesis. Plast Reconstr Surg. 2019;144(5): 816e-827e. [53] MOU S, ZHOU M, LI Y, et al. Extracellular Vesicles from Human Adipose-Derived Stem Cells for the Improvement of Angiogenesis and Fat-Grafting Application. Plast Reconstr Surg. 2019;144(4):869-880. [54] HAN Y, REN J, BAI Y, et al. Exosomes from hypoxia-treated human adipose-derived mesenchymal stem cells enhance angiogenesis through VEGF/VEGF-R. Int J Biochem Cell Biol. 2019;109:59-68. [55] Hutton DL, Grayson WL. Hypoxia Inhibits De Novo Vascular Assembly of Adipose-derived Stromal/Stem Cell Populations but Promotes Growth Of Pre-Formed Vessels. Tissue Eng Part A. 2016; 22(1-2):161-169. [56] HAN YD, BAI Y, YAN XL, et al. Co-transplantation of exosomes derived from hypoxia-preconditioned adipose mesenchymal stem cells promotes neovascularization and graft survival in fat grafting. Biochem Biophys Res Commun. 2018;497(1):305-312. [57] YU Z, CAI Y, DENG M, et al. Fat extract promotes angiogenesis in a murine model of limb ischemia: a novel cell-free therapeutic strategy. Stem Cell Res Ther. 2018;9(1):294. [58] HAIDER KH, AZIZ S, AL-RESHIDI MA. Endothelial progenitor cells for cellular angiogenesis and repair: lessons learned from experimental animal models. Regen Med. 2017;12(8):969-982. [59] BAUER SM, GOLDSTEIN LJ, BAUER RJ, et al. The bone marrow-derived endothelial progenitor cell response is impaired in delayed wound healing from ischemia. J Vasc Surg. 2006;43(1):134-141. [60] CHEN L, ZHENG Q, LIU Y, et al.Adipose-derived stem cells promote diabetic wound healing via the recruitment and differentiation of endothelial progenitor cells into endothelial cells mediated by the VEGF-PLCγ-ERK pathway. Arch Biochem Biophys. 2020;692:108531. [61] ZHU Z, YUAN ZQ, HUANG C, et al. Pre-culture of adipose-derived stem cells and heterologous acellular dermal matrix: paracrine functions promote post-implantation neovascularization and attenuate inflammatory response. Biomedical Materials. 2019;14(3):035002. [62] PETZELBAUER P, WATSON CA, PFAU SE, et al.IL-8 and angiogenesis: Evidencen that human endothelial cells lack receptors and do not respone to IL-8 in vitro. Cytokine. 1995;7(3):267-272. [63] SANADA F, TANIYAMA Y, AZUMA J, et al. Hepatocyte growth factor, but not vascular endothelial growth factor, attenuates angiotensin II-induced endothelial progenitor cell senescence. Hypertension. 2009;53(1):77-82. [64] MIN JK, LEE YM, KIM JH, et al. Hepatocyte growth factor suppresses vascular endothelial growth factor-induced expression of endothelial ICAM-1 and VCAM-1 by inhibiting the nuclear factor-kappaB pathway. Circ Res. 2005;96(3):300-307. [65] KRAEMER WJ, RATAMESS NA, HYMER WC, et al. Growth Hormone(s), Testosterone, Insulin-Like Growth Factors, and Cortisol: Roles and Integration for Cellular Development and Growth With Exercise. Front Endocrinol (Lausanne). 2020;11:33. [66] AHMADI S, MUJAHID AM, KHAN H, et al. Comparison of Graft Survival between Fat Harvested from Abdomen and Medial Thigh for Facial Contour Deformity: A Randomised Control Trial. J Coll Physicians Surg Pak. 2019;29(5):440-443. [67] TAHA S, SALLER MM, HAAS E, et al. Adipose-derived stem/progenitor cells from lipoaspirates: A comparison between the Lipivage200-5 liposuction system and the Body-Jet liposuction system. J Plast Reconstr Aesthet Surg. 2020;73(1):166-175. [68] PAPADOPULOS NA, WIGAND S, KUNTZ N, et al. The Impact of Harvesting Systems and Donor Characteristics on Viability of Nucleated Cells in Adipose Tissue: A First Step Towards a Manufacturing Process. J Craniofac Surg. 2019;30(3): 716-720. [69] ROSS RJ, SHAYAN R, MUTIMER KL, et al. Autologous fat grafting: current state of the art and critical review. Ann Plast Surg. 2014;73(3):352-357. [70] SESE B, SANMARTIN JM, ORTEGA B, et al. Nanofat Cell Aggregates: A Nearly Constitutive Stromal Cell Inoculum for Regenerative Site-Specific Therapies. Plast Reconstr Surg. 2019;144(5):1079-1088. [71] ETO H, SUGA H, MATSUMOTO D, et al. Characterization of structure and cellular components of aspirated and excised adipose tissue. Plast Reconstr Surg. 2009;124(4):1087-1097. [72] CHEN X, WU Y, LIU G. Influence of Recipient Site on the Function and Survival of Fat Grafts. Ann Plast Surg. 2019;82(1):110-115. [73] LAI JY, CHAN EC, KUO SM, et al. Three Dimensional Collagen Scaffold Promotes Intrinsic Vascularisation for Tissue Engineering Applications. Plos One. 2016;11(2):e0149799. (责任编辑:WZH,ZN,DL) |
| [1] | 林清凡, 解一新, 陈婉清, 叶振忠, 陈幼芳. 人胎盘源间充质干细胞条件培养液可上调缺氧状态下BeWo细胞活力和紧密连接因子的表达[J]. 中国组织工程研究, 2021, 25(在线): 4970-4975. |
| [2] | 蒲 锐, 陈子扬, 袁凌燕. 不同细胞来源外泌体保护心脏的特点与效应[J]. 中国组织工程研究, 2021, 25(在线): 1-. |
| [3] | 张同同, 王中华, 文 杰, 宋玉鑫, 刘 林. 3D打印模型在颈椎肿瘤手术切除与重建中的应用[J]. 中国组织工程研究, 2021, 25(9): 1335-1339. |
| [4] | 张 超, 吕 欣. 髋臼骨折固定后的异位骨化:危险因素、预防及其治疗进展[J]. 中国组织工程研究, 2021, 25(9): 1434-1439. |
| [5] | 周继辉, 李新志, 周 游, 黄 卫, 陈文瑶. 髌骨骨折修复内植物选择的多重问题[J]. 中国组织工程研究, 2021, 25(9): 1440-1445. |
| [6] | 王德斌, 毕郑刚. 尺骨鹰嘴骨折-脱位解剖力学、损伤特点、固定修复及3D技术应用的相关问题[J]. 中国组织工程研究, 2021, 25(9): 1446-1451. |
| [7] | 姬志祥, 蓝常贡. 尿酸盐转运蛋白在痛风中的多态性和治疗相关性[J]. 中国组织工程研究, 2021, 25(8): 1290-1298. |
| [8] | 袁 美, 张新新, 郭祎莎, 毕 霞. 循环microRNA在血管性认知障碍诊断中的应用[J]. 中国组织工程研究, 2021, 25(8): 1299-1304. |
| [9] | 张秀梅, 翟运开, 赵 杰, 赵 萌. 类器官模型国内外数据库近10年文献研究热点分析[J]. 中国组织工程研究, 2021, 25(8): 1249-1255. |
| [10] | 王正东, 黄 娜, 陈婧娴, 郑作兵, 胡鑫宇, 李 梅, 苏 晓, 苏学森, 颜 南. 丁酸钠抑制氟中毒可诱导小胶质细胞活化及炎症因子表达增多[J]. 中国组织工程研究, 2021, 25(7): 1075-1080. |
| [11] | 汪显耀, 关亚琳, 刘忠山. 提高间充质干细胞治疗难愈性创面的策略[J]. 中国组织工程研究, 2021, 25(7): 1081-1087. |
| [12] | 万 然, 史 旭, 刘京松, 王岩松. 间充质干细胞分泌组治疗脊髓损伤的研究进展[J]. 中国组织工程研究, 2021, 25(7): 1088-1095. |
| [13] | 廖成成, 安家兴, 谭张雪, 王 倩, 刘建国. 口腔鳞状细胞癌干细胞的治疗靶点及应用前景[J]. 中国组织工程研究, 2021, 25(7): 1096-1103. |
| [14] | 赵 敏, 冯柳祥, 陈 垚, 顾 霞, 王平义, 李一梅, 李文华. 低氧环境下外泌体可作为疾病的标志物[J]. 中国组织工程研究, 2021, 25(7): 1104-1108. |
| [15] | 谢文佳, 夏天娇, 周卿云, 刘羽佳, 顾小萍. 小胶质细胞介导神经元损伤在神经退行性疾病中的作用[J]. 中国组织工程研究, 2021, 25(7): 1109-1115. |
中国组织工程研究杂志出版内容重点:组织构建;骨细胞;软骨细胞;细胞培养;成纤维细胞;血管内皮细胞;骨质疏松;组织工程
ADSCs,EPC,SVF,mechanisms,signal pathway”为英文检索词;以“脂肪移植;血管化;外泌体;血管内皮生长因子;脂肪干细胞;内皮祖细胞;基质血管成分;信号通路”为中文检索词;检索的文献类型有综述性论文、研究性论文及论著等。
1.2 入选标准
1.2.1 纳入标准 ①研究内容与脂肪移植相关;②与脂肪移植血管化相关的研究。
1.2.2 排除标准 ①与主题相关性不高的文献;②证据等级不高、质量较低的文献,内容重复的文献;③在PubMed、Google Scholar数据库检索不到全文的文献。
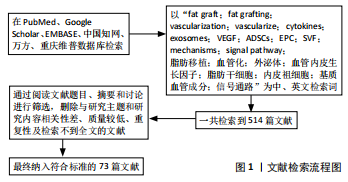
1.3 质量评估 按照上述纳入标准和排除标准共检索到文献514篇。通过阅读文献题目、摘要和讨论进行筛选,最后采用EndNote软件进行归纳整理,最终纳入73篇符合标准的文献进行综述。
1.4 数据的提取 研究内容由刘家杰进行提取,并通过与赵娴讨论解决分歧,分别探讨各种细胞因子或细胞、干细胞、不同部位脂肪细胞的选择、相关信号通路、预处理脂肪、组织工程、外泌体和其他相关处理在促进脂肪移植血管化中的应用。文献筛选流程图见 图1。
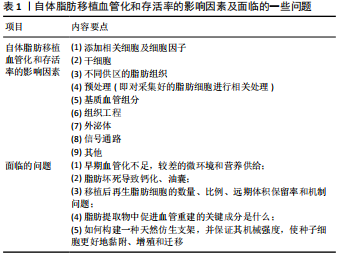
 大部分研究显示,脂肪移植后其体积会经历一个先减小后增加的过程。有大量研究探讨脂肪移植血管化问题,并取得了一定成效,但上面陈述的关键问题还未找到答案。
大部分研究显示,脂肪移植后其体积会经历一个先减小后增加的过程。有大量研究探讨脂肪移植血管化问题,并取得了一定成效,但上面陈述的关键问题还未找到答案。目前大部分学者一致认为,在生理和病理状态下血管形成的关键细胞是内皮祖细胞,也是血管内皮细胞的前体细胞,又名血管内皮干细胞[58]。可是,内皮祖细胞在生理情况下,极少存在于外周且在体外生长缓慢,很难在体外培养,即使可以体外培养,但长时间培养后易分化,便失去成血管能力。大量数据表明,内皮祖细胞可以被具有强大趋化作用的基质细胞衍生因子1α趋化,应该思考如何构建一种载体来诱导脂肪来源干细胞分泌基质细胞衍生因子1α,从而趋化内皮祖细胞进入移植区参与血管重建,加速移植物早期血管形成,提高移植脂肪存活率[59];脂肪细胞外泌体为什么在早期具有成血管能力;脂肪移植受区如何高效处理;骨髓间充质干细胞和脂肪源性干细胞向内皮细胞分化的机制;以及VEGF165定向分化为血管的机制,这些关键环节都值得继续去探索和思考。文章提到的细胞外基质、软组织工程为脂肪移植提供了新思路,为提高脂肪移植成活率提供新策略。
脂肪干细胞主要通过释放VEGF、肝细胞生长因子等来促进血管再生,并抑制炎症反应。最新研究结果表明,脂肪干细胞可以通过 VEGF-PLCγ-ERK1/ERK2途径调节血管生成,并抑制炎症反应,通过内皮祖细胞的募集和分化来促进早期血管形成[60]。脂肪干细胞促进脂肪移植物存活和血管再生的可能机制在于脂肪干细胞的旁分泌产物,其可以促进新血管形成并减轻炎症反应[61],从而提高脂肪移植物体积保留率。因此,脂肪干细胞将在再生医学领域发挥突出的作用。
白细胞介素8 是促炎细胞因子家族(趋化因子)的成员,并且已被确定为人类嗜中性粒细胞的重要趋化因子和激活剂,它可以刺激内皮细胞来介导新血管形成,而且可以募集白细胞并释放血管生成因子[62]。
VEGF在血管新生中的作用是肯定的。近年来,越来越清楚的是,VEGF不仅是促进血管生成的因子,还是促炎性细胞因子。VEGF导致单核细胞与内皮细胞的黏附增加,这是由ROS(rac1)-核因子kB激活介导的[63]。肝细胞生长因子与VEGF都有促进血管新生的作用,但具体表现特征不尽相同,肝细胞生长因子的作用是独特的,因为已知肝细胞生长因子可以起到抗炎性细胞因子的作用和抗氧化应激的作用。MIN等[64]研究显示,肝细胞生长因子可能通过减少氧化应激而抑制VEGF诱导的炎症,这对早期血管再生有重要作用。
胰岛素样生长因子是小的多肽激素(有70个氨基酸的胰岛素样生长因子1和67个氨基酸的胰岛素样生长因子2),与胰岛素在结构上相关,其中胰岛素样生长因子1(7 kD)负责代谢,促有丝分裂和合成代谢,它是在组织和细胞局部产生(即自分泌和旁分泌机制)。胰岛素样生长因子1既是细胞,又是细胞周期起始和进展因子,其影响包括卫星细胞激活、增殖、存活和分化[65],进而促进脂肪移植早期血管形成。
不同部位来源的脂肪组织在移植后表现出的成活率存在差异,对于脂肪收获的有利供体部位,存在广泛争议。目前脂肪组织的主要来源部位有腹部、大腿、臀部等,研究认为大腿来源的脂肪组织存活率更高[66],而主要的观点是与哈德森等一致。还有观点认为臀股骨区域是一个更好的供体部位,因为该区域的脂肪组织由较大的脂肪细胞组成,并且比腹部、胸部或面部具有更高的成脂活性。在一项针对乳房再造的研究中,从大腿和腹部注射脂肪得出结论,无论注射量或组织来源部位如何,都不会影响脂肪移植物的体积保留。也有人认为,脂肪移植是重建、再生和美容手术的自然选择,需要长期的研究来评估脂肪移植后脂肪移植物的稳定性。这项研究通过超声检查评估了体积损失,比较了两个最常用的脂肪组织来源部位,即大腿和腹部,以检查皮下组织的术前和术后厚度。由于大腿的脂肪组织中细胞数量更多,因此与腹部相比,两组之间的平均厚度和最终体积的差异非常显著,结论为大腿来源脂肪组织中脂肪细胞寿命更长,这间接证明不同部位脂肪组织或细胞的存活率存在差异。
获取脂肪的技术对成活率及血管化的影响。近年来,脂肪来源的干/祖细胞的再生潜力已成为再生医学和组织工程领域中一个有趣的关注点。人们已经比较了多种脂肪收集方法的临床特性,例如手术时间、收获量、失血量、皮肤反应和使用成本,但是就保存细胞特性而言,不同吸脂技术存在很大的差距。关键问题是,用不同的吸脂技术收获的脂肪组织产生的脂肪来源的干/祖细胞的细胞功能是否具有可比性或显著不同[67],如:套管的尺寸、压力或外科医生运动的力量和频率起着关键作用,这是未来研究的热点[68]。组织学研究发现,与其他供体部位(上腹部和下腹部、大腿、膝盖和转子附近、侧面)相比,小腹中脂肪来源的干细胞明显更多,但是吸脂套管口径没有受到控制。尽管这项研究表明脂肪干细胞的丰度可能会发生特定位置变化,但诸如收获技术之类的因素也可能会影响这一结果。研究发现移植后即刻生存能力和转移脂肪移植的结局与供体位点相关性无显著差异。相反,从膝内侧、髋部等部位获取的脂肪组织较其他部位存活率更高[69],表明不同部位收获的脂肪组织或细胞在存活率方面存在差异。
脂肪移植基本可划分为脂肪组织块、颗粒脂肪(包括纳米脂肪)、基质血管组分等。纳米脂肪样品中的机械分解不会改变细胞活力[70],其含有较多的基质血管组分和脂肪干细胞,而基质血管组分中含有不同类型促进血管形成的细胞,如内皮细胞,是血管形成的重要细胞之一。不管是团块脂肪、颗粒脂肪(纳米脂肪)还是基质血管组分的移植,保持脂肪组织结构的完整性才是最重要的[71]。选择何种类型的脂肪组织移植受到移植受区面积及结构的影响。
研究提示,单次脂肪移植的量、移植方法对脂肪移植物体积保留率、血管化和成活率影响很大,每次移植量少于0.1 mL的小等分试样的方式注射[72]。有研究提倡使用1.0-2.0 mL带有17号针头的Luer-Lok注射器,并多次通过使用较小的移植物体积,从而产生多个小的移植物部
位[69]。即使在大体积区域中也要使用每次通过量较小的溶液,最高可达1 mL。但不同部位脂肪移植的量也存在差异,应根据临床需要来评估,但总的原则应遵循少量、多次、多隧道进行填充,保证脂肪组织有充足的血运和营养供给。
用脂肪干细胞富集脂肪移植物可抑制炎性细胞因子的产生,增加生长因子水平,增加脂肪移植物的存活率,下调NADPH 氧化酶(NOX)1和 4 的表达,增加血管形成并以Toll样受体(TLR)4的方式减少活性氧的产生和核因子E 2 相关因子2(Nrf2)的表达。免疫组织化学分析表明,低氧暴露促进了脂肪干细胞的生长并促进了脂肪干细胞向血管内皮细胞的分化。缺氧诱导的炎症细胞因子、生长因子和NOX1/4的上调,以及脂肪干细胞中活性氧的产生和凋亡均依赖于TLR4和 Nrf2,这也调节了脂肪干细胞促进内皮祖细胞迁移和血管生成。缺氧对脂肪干细胞的影响受Nrf2 抗氧化剂反应与核因子κB和TLR4介导的炎症反应之间串扰的调节。脂肪干细胞可以通过调节Nrf2 和 TLR4引起的炎症和氧化反应来增加脂肪移植的存活率,从而提出了改善脂肪干细胞用于细胞治疗的潜在策略。
近年来,随着组织工程领域的兴起,脂肪细胞生长的微环境成为关注的焦点,研究发现细胞外基质是脂肪细胞生长必不可少的微环境,而细胞外基质的主要成分是胶原蛋白,胶原蛋白支架可能会为浸润细胞(包括内源性内皮细胞)、诱导血管的血管化植入物提供适宜的微环境。胶原蛋白支架的多孔结构允许营养物质的扩散,为细胞的迁移提供基本结构[73],并诱导血管生成。
综上,脂肪移植血管化和成活率在不断提高,但仍没有取得突破性的进展,仍具有挑战性,相信在广大医生和科研人员的共同努力下,会早日攻克脂肪移植血管化不足和成活率低的难题。

文题释义:#br# 自体脂肪移植:是指将从供区通过手术切取或负压抽吸等方式获取的自体脂肪组织,在体外经过一定加工处理(包括漂洗、提纯、添加自体干细胞或异体细胞因子、药物等方式)后移植于受区,以达到增加组织容积、促进组织再生或改善组织质地等目的的组织移植技术。#br# 血管形成:是微血管以出芽的方式从血管床中长出并形成新的血管分支及毛细血管丛,是经过完全分化的内皮细胞增殖、迁移和重塑的结果。
近年来,随着自体脂肪移植技术的不断发展,脂肪移植已经广泛应用于整形外科、修复重建外科、医学美容科等领域。然而,自体脂肪移植早期易液化、感染、坏死、形成油囊,限制其在临床中的应用。因此,早期血管化是脂肪移植成功的关键,这也是广大临床医生面临的亟待解决的问题。
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||