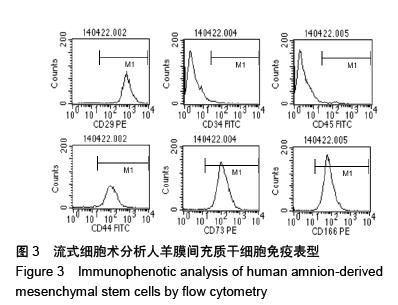
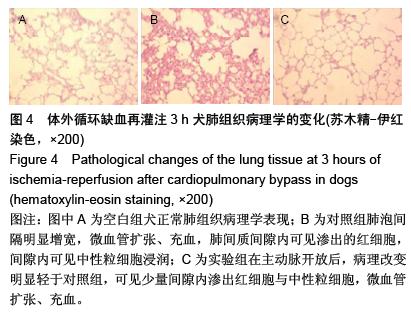
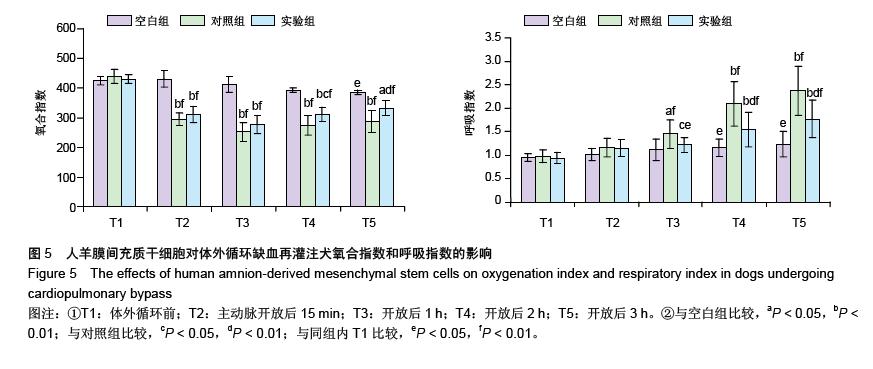
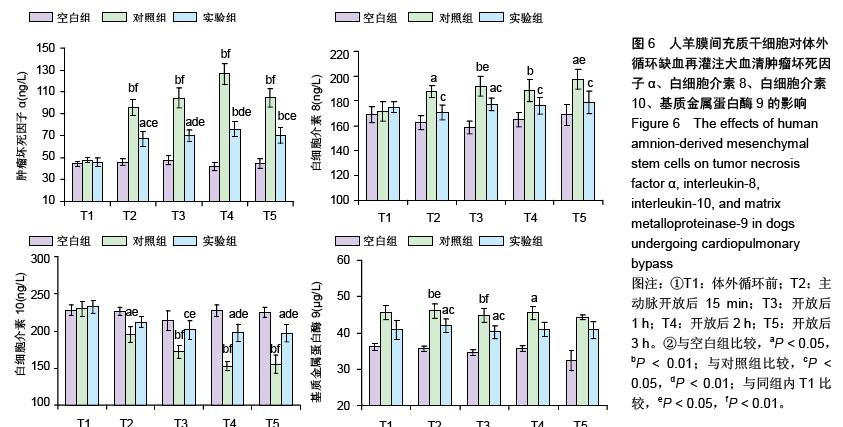
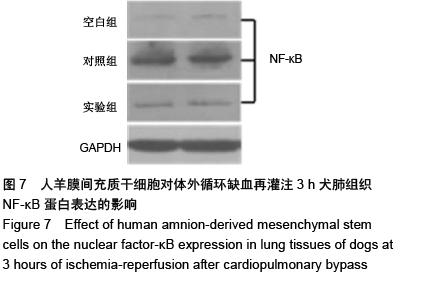
| [1] Sevuk U, Cakil N, Altindag R, et al. Relationship between nadir hematocrit during cardiopulmonary bypass and postoperative hyperglycemia in nondiabetic patients. Heart Surg Forum. 2014;17(6):E302-307.
[2] Engels M, Bilgic E, Pinto A, et al. A cardiopulmonary bypass with deep hypothermic circulatory arrest rat model for the investigation of the systemic inflammation response and induced organ damage. J Inflamm (Lond). 2014;11:26.
[3] Ranucci M, Isgrò G, Carlucci C, et al. Central venous oxygen saturation and blood lactate levels during cardiopulmonary bypass are associated with outcome after pediatric cardiac surgery. Crit Care. 2010;14(4):R149.
[4] Chen H, Cheng ZB, Yu RG. Procalcitonin as a predictor of moderate to severe acute respiratory distress syndrome after cardiac surgery with cardiopulmonary bypass: a study protocol for a prospective cohort study. BMJ Open. 2014; 4(10):e006344.
[5] Nakamura H, Yamaguchi H, Amano A, et al. Venovenous extracorporeal membrane oxygenation is effective against post-cardiotomy acute respiratory failure in adults. Gen Thorac Cardiovasc Surg. 2013;61(7):402-408.
[6] Cheng C, Li S, Wang Y, et al. Ischemic postconditioning alleviates lung injury and maintains a better expression of aquaporin-1 during cardiopulmonary bypass.Chin Med J (Engl). 2014;127(23):4012-4018.
[7] Dolkart O, E A, S S, et al. Temporal determination of lung NO system and COX-2 upregulation following ischemia-reperfusion injury. Exp Lung Res. 2014;40(1):22-29.
[8] Gu YJ, Boonstra PW, Graaff R, et al. Pressure drop, shear stress, and activation of leukocytes during cardiopulmonary bypass: a comparison between hollow fiber and flat sheet membrane oxygenators.Artif Organs. 2000;24(1):43-48.
[9] Banz Y, Rieben R, Zobrist C, et al. Addition of dextran sulfate to blood cardioplegia attenuates reperfusion injury in a porcine model of cardiopulmonary bypass. Eur J Cardiothorac Surg. 2008;34(3):653-660.
[10] Liakopoulos OJ, Schmitto JD, Kazmaier S, et al. Cardiopulmonary and systemic effects of methylprednisolone in patients undergoing cardiac surgery. Ann Thorac Surg. 2007;84(1):110-118.
[11] Warren O, Darzi A, Athanasiou T. What is the role of leukocyte depletion in cardiac surgery.Heart Lung Circ. 2007;16(5): 398-399.
[12] Eisses MJ, Velan T, Aldea GS, et al. Strategies to reduce hemostatic activation during cardiopulmonary bypass. Thromb Res. 2006;117(6):689-703.
[13] Williams GD, Ramamoorthy C, Chu L, et al. Modified and conventional ultrafiltration during pediatric cardiac surgery: clinical outcomes compared. J Thorac Cardiovasc Surg. 2006;132(6):1291-1298.
[14] Manuelpillai U, Moodley Y, Borlongan CV, et al. Amniotic membrane and amniotic cells: potential therapeutic tools to combat tissue inflammation and fibrosis. Placenta. 2011;32 Suppl 4:S320-325.
[15] Chang CJ, Yen ML, Chen YC, et al. Placenta-derived multipotent cells exhibit immunosuppressive properties that are enhanced in the presence of interferon-gamma. Stem Cells. 2006;24(11):2466-2477.
[16] Banas RA, Trumpower C, Bentlejewski C, et al. Immunogenicity and immunomodulatory effects of amnion-derived multipotent progenitor cells. Hum Immunol. 2008;69(6):321-328.
[17] Dominici M, Le Blanc K, Mueller I, et al. Minimal criteria for defining multipotent mesenchymal stromal cells. The International Society for Cellular Therapy position statement. Cytotherapy. 2006;8(4):315-317.
[18] Bailo M, Soncini M, Vertua E, et al. Engraftment potential of human amnion and chorion cells derived from term placenta. Transplantation. 2004;78(10):1439-1448.
[19] 丛姗,白立恒,李岩,等.人羊膜间充质干细胞移植对CCl4诱导的小鼠损伤肝HGF、SIRT-1、α-SMA及P27kip1表达的影响[J].中国生物化学与分子生物学报, 2015, 31(3):292-300.
[20] Zhao P, Ise H, Hongo M, et al. Human amniotic mesenchymal cells have some characteristics of cardiomyocytes. Transplantation. 2005;79(5):528-535.
[21] Kim J, Kang HM, Kim H, et al. Ex vivo characteristics of human amniotic membrane-derived stem cells. Cloning Stem Cells. 2007;9(4):581-594.
[22] Kim J, Lee Y, Kim H, et al. Human amniotic fluid-derived stem cells have characteristics of multipotent stem cells. Cell Prolif. 2007;40(1):75-90.
[23] Han K, Lee JE, Kwon SJ, et al. Human amnion-derived mesenchymal stem cells are a potential source for uterine stem cell therapy. Cell Prolif. 2008;41(5):709-725.
[24] 丛姗,宋瑾,张惠娟,等.人羊膜间充质干细胞(hAMSCs)的分离、体外培养及诱导分化[J]. 农业生物技术学报,2015,23(1): 20-31.
[25] Gibbon JH Jr. Application of a mechanical heart and lung apparatus to cardiac surgery.Minn Med. 1954;37(3): 171-185.
[26] 张贺,王承利,王洋,等.犬体外循环模型建立及麻醉处理[J].中国比较医学杂志,2010,20(10):44-47.
[27] Halter J, Steinberg J, Fink G, et al. Evidence of systemic cytokine release in patients undergoing cardiopulmonary bypass. J Extra Corpor Technol. 2005;37(3):272-277.
[28] Zhou E, Li Y, Wei Z, et al. Schisantherin A protects lipopolysaccharide-induced acute respiratory distress syndrome in mice through inhibiting NF-κB and MAPKs signaling pathways. Int Immunopharmacol. 2014;22(1): 133-140.
[29] Shembade N, Harhaj NS, Liebl DJ, et al. Essential role for TAX1BP1 in the termination of TNF-alpha-, IL-1- and LPS-mediated NF-kappaB and JNK signaling. EMBO J. 2007;26(17):3910-3922.
[30] Karlsson H, Samarasinghe S, Ball LM, et al. Mesenchymal stem cells exert differential effects on alloantigen and virus-specific T-cell responses. Blood. 2008;112(3):532-541.
[31] Miyazawa T, Matsumoto K, Ohmichi H, et al. Protection of hippocampal neurons from ischemia-induced delayed neuronal death by hepatocyte growth factor: a novel neurotrophic factor. J Cereb Blood Flow Metab. 1998;18(4): 345-348.
[32] Matsumoto K, Nakamura T. Hepatocyte growth factor: renotropic role and potential therapeutics for renal diseases. Kidney Int. 2001;59(6):2023-2038.
[33] Sharma HS. Neuroprotective effects of neurotrophins and melanocortins in spinal cord injury: an experimental study in the rat using pharmacological and morphological approaches. Ann N Y Acad Sci. 2005;1053:407-421.
[34] Fares RC, Gomes Jde A, Garzoni LR, et al. Matrix metalloproteinases 2 and 9 are differentially expressed in patients with indeterminate and cardiac clinical forms of Chagas disease. Infect Immun. 2013;81(10):3600-3608.
[35] Välimäki J, Uusitalo H. Matrix metalloproteinases (MMP-1, MMP-2, MMP-3 and MMP-9, and TIMP-1, TIMP-2 and TIMP-3) and markers for vascularization in functioning and non-functioning bleb capsules of glaucoma drainage implants. Acta Ophthalmol. 2015;93(5):450-456.
[36] Toufaily C, Charfi C, Annabi B, et al. A Role for the Cavin-3/Matrix Metalloproteinase-9 Signaling Axis in the Regulation of PMA-Activated Human HT1080 Fibrosarcoma Cell Neoplastic Phenotype. Cancer Growth Metastasis. 2014; 7:43-51.
[37] Petrovska-Cvetkovska D, Dolnenec-Baneva N, Nikodijevik D, et al. Correlative study between serum matrix metalloproteinase 9 values and neurologic deficit in acute, primary, supratentorial, intracerebral haemorrhage. Prilozi. 2014;35(2):39-44.
[38] Wang C, Li D, Qian Y, et al. Increased matrix metalloproteinase-9 activity and mRNA expression in lung injury following cardiopulmonary bypass. Lab Invest. 2012; 92(6):910-916.
[39] Eichler W, Bechtel JF, Schumacher J, et al. A rise of MMP-2 and MMP-9 in bronchoalveolar lavage fluid is associated with acute lung injury after cardiopulmonary bypass in a swine model. Perfusion. 2003;18(2):107-113.
[40] Bours V, Bentires-Alj M, Hellin AC, et al. Nuclear factor-kappa B, cancer, and apoptosis. Biochem Pharmacol. 2000;60(8): 1085-1089.
[41] Xiao W. Advances in NF-kappaB signal ling transduction and transcription. Cell Mol Immunology. 2004;1(6):425-435.
[42] Fei XJ, Zhu LL, Xia LM, et al. Acanthopanax senticosus attenuates inflammation in lipopolysaccharide-induced acute lung injury by inhibiting the NF-κB pathway. Genet Mol Res. 2014;13(4):10537-10544. |
.jpg)
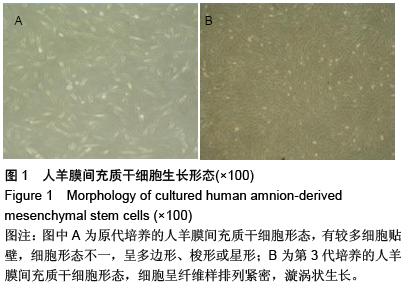
.jpg)