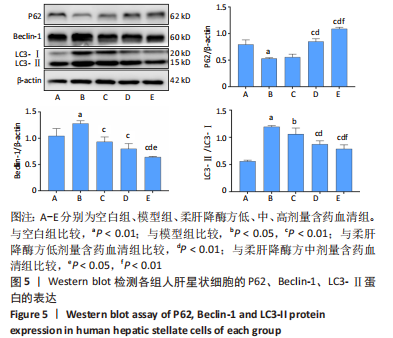
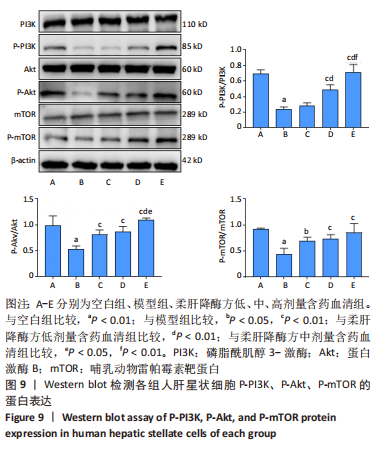
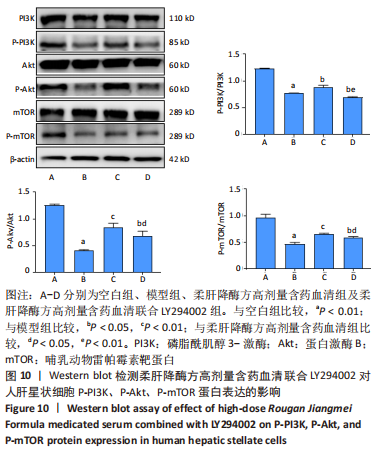
[1] TRAUTWEIN C, FRIEDMAN SL, SCHUPPAN D, et al. Hepatic fibrosis: Concept to treatment. J Hepatol. 2015;62(1 Suppl):S15-S24.
[2] 池晓玲, 萧焕明. 病毒性肝炎防治新形势下对中医药防治肝纤维化的思考[J]. 临床肝胆病杂志,2018,34(4):694-697.
[3] VERMA AK, SHARMA A, SUBRAMANIYAM N, et al. Augmenter of liver regeneration: Mitochondrial function and steatohepatitis. J Hepatol. 2022;77(5):1410-1421.
[4] KRIZHANOVSKY V, YON M, DICKINS RA, et al. Senescence of activated stellate cells limits liver fibrosis. Cell. 2008;134(4):657-667.
[5] LEI L, BRUNEAU A, EL MOURABIT H, et al. Portal fibroblasts with mesenchymal stem cell features form a reservoir of proliferative myofibroblasts in liver fibrosis. Hepatology. 2022;76(5):1360-1375.
[6] VARGAS JNS, HAMASAKI M, KAWABATA T, et al. The mechanisms and roles of selective autophagy in mammals. Nat Rev Mol Cell Biol. 2022;1038(10):s41580-022-00542-2.
[7] CHEN S, HE Z, XIE W, et al. Ginsenoside Rh2 attenuates CDAHFD-induced liver fibrosis in mice by improving intestinal microbial composition and regulating LPS-mediated autophagy. Phytomedicine. 2022;101(7):154121.
[8] HOU LS, ZHANG YW, LI H, et al. The regulatory role and mechanism of autophagy in energy metabolism-related hepatic fibrosis. Pharmacol Ther. 2022;234(6):108117.
[9] FUKUDA T, WADA-HIRAIKE O. The Two-Faced Role of Autophagy in Endometrial Cancer. Front Cell Dev Biol. 2022;31(10):839416.
[10] WU L, ZHANG Q, MO W, et al. Quercetin prevents hepatic fibrosis by inhibiting hepatic stellate cell activation and reducing autophagy via the TGF-β1/Smads and PI3K/Akt pathways. Sci Rep. 2017;7(1):9289.
[11] 张倩璐, 旷昕. 丙泊酚对转化生长因子-β1诱导肝星状细胞激活的影响及其机制[J]. 中国应用生理学杂志,2020,36(3):273-278.
[12] 陈普艳, 姜锦林, 杨强. 柔肝降酶合剂对大鼠四氯化碳诱导肝损害的防治作用[J]. 世界科学技术-中医药现代化,2014,16(4):811-816.
[13] 张千娥, 谢洪武, 刘福水. 柔肝降酶合剂治疗慢性乙型肝炎40例临床观察[J]. 中医杂志,2014,55(22):1929-1932.
[14] 范丽丽, 陈雄, 邹忠兰, 等. 亚砷酸钠对人肝星状细胞活化及细胞外基质分泌的影响[J].中华预防医学杂志,2018,52(10):983-987.
[15] 吴朕, 马微, 臧成昊, 等. 三七皂苷R1保护四氯化碳诱导肝纤维化模型大鼠的作用[J].中国组织工程研究,2020,24(26):4213-4217.
[16] ZHANG D, ZHANG Y, SUN B. The Molecular Mechanisms of Liver Fibrosis and Its Potential Therapy in Application. Int J Mol Sci. 2022;23(20): 12572.
[17] SCHUPPAN D, SURABATTULA R, WANG XY. Determinants of fibrosis progression and regression in NASH. J Hepatol. 2018;68(2):238-250.
[18] FRIEDMAN SL, PINZANI M. Hepatic fibrosis 2022: Unmet needs and a blueprint for the future. Hepatology. 2022;75(2):473-488.
[19] 徐列明, 刘平, 沈锡中, 等. 肝纤维化中西医结合诊疗指南(2019年版)[J]. 中国中西医结合杂志,2019,39(11):1286-1295.
[20] SKRZYPCZAK-WIERCIOCH A, SAŁAT K. Lipopolysaccharide-Induced Model of Neuroinflammation: Mechanisms of Action, Research Application and Future Directions for Its Use. Molecules. 2022;27(17): 5481.
[21] WANG T, LU Z, QU XH, et al. Chrysophanol-8-O-glucoside protects mice against acute liver injury by inhibiting autophagy in hepatic stellate cells and inflammatory response in liver-resident macrophages. Front Pharmacol. 2022;13:951521.
[22] CHEN M, LIU J, YANG W, et al. Lipopolysaccharide mediates hepatic stellate cell activation by regulating autophagy and retinoic acid signaling. Autophagy. 2017;13(11):1813-1827.
[23] LI J, DENG X, WANG S, et al. Resolvin D1 attenuates CCl4 Induced Liver Fibrosis by Inhibiting Autophagy-Mediated HSC activation via PI3K/Akt/mTOR Pathway. Front Pharmacol. 2021;12:792414.
[24] 李佳行, 杨胜乾, 刘娟娟, 等. 连翘苷对脂多糖诱导肝脏星状细胞活化的抑制作用[J]. 第三军医大学学报,2020,42(4):342-349.
[25] 杨如会, 刘丙进, 吴松泉. 淫羊藿苷通过FXR降低LPS/TLR4诱导的肝星状细胞自噬和活化[J]. 中国药学杂志,2016,51(9):708-714.
[26] 刘云洁, 程玮, 李丽, 等. IRF3抑制LPS诱导肝星状细胞LX-2的炎症因子的分泌[J]. 安徽医科大学学报,2019,54(2):178-182.
[27] RAVIKUMAR B, SARKAR S, DAVIES JE, et al. Regulation of mammalian autophagy in physiology and pathophysiology. Physiol Rev. 2010;90(4): 1383-1435.
[28] RONG Z, ZHENG K, CHEN J, et al. Function and regulation of ULK1: From physiology to pathology. Gene. 2022;840:146772.
[29] KTISTAKIS NT, TOOZE SA. Digesting the Expanding Mechanisms of Autophagy. Trends Cell Biol. 2016;26(8):624-635.
[30] SHI Q, JIN X, ZHANG P, et al. SPOP mutations promote P62/SQSTM1-dependent autophagy and Nrf2 activation in prostate cancer. Cell Death Differ. 2022;29(6):1228-1239.
[31] CHENG D, CHAI J, WANG H, et al. Hepatic macrophages: Key players in the development and progression of liver fibrosis. Liver Int. 2021; 41(10):2279-2294.
[32] 安祯祥, 何远利, 唐东昕, 等. 扶脾柔肝颗粒对肝纤维化模型大鼠的改善作用机制研究[J]. 中国药房,2021,32(21):2587-2592.
[33] MOHANASUNDARAM P, COELHO-RATO LS, MODI MK, et al. Cytoskeletal vimentin regulates cell size and autophagy through mTORC1 signaling. PLoS Biol. 2022;20(9):e3001737.
[34] YOSHIDA S, PACITTO R, INOKI K, et al. Macropinocytosis, mTORC1 and cellular growth control. Cell Mol Life Sci. 2018;75(7):1227-1239.
[35] WANG R, SONG F, LI S, et al. Salvianolic acid A attenuates CCl4-induced liver fibrosis by regulating the PI3K/PI3K/Akt/mTOR, Bcl-2/Bax and caspase-3/cleaved caspase-3 signaling pathways. Drug Des Devel Ther. 2019;13:1889-1900.
[36] WANG H, LIU Y, WANG D, et al. The Upstream Pathway of mTOR-Mediated Autophagy in Liver Diseases. Cells. 2019;8(12):1597.
[37] XIU A Y, DING Q, LI Z, et al. Doxazosin Attenuates Liver Fibrosis by Inhibiting Autophagy in Hepatic Stellate Cells via Activation of the PI3K/Akt/mTOR Signaling Pathway. Drug Des Devel Ther. 2021;15:3643-3659.
[38] LEI Y, WANG Q, SHEN L, et al. MicroRNA-101 suppresses liver fibrosis by downregulating PI3K/Akt/mTOR signaling pathway. Clin Res Hepatol Gastroenterol. 2019;43(5):575-584.
[39] JI D, ZHAO Q, QIN Y, et al. Germacrone improves liver fibrosis by regulating the PI3K/AKT/mTOR signalling pathway. Cell Biol Int. 2021; 45(9):1866-1875.
|