[1] GUERRA A, BELINHA J, JORGE RN. Modelling skin wound healing angiogenesis: A review. J Theor Biol. 2018;459:1-17.
[2] CHEN KY, LIAO WJ, KUO SM, et al. Asymmetric chitosan membrane containing collagen I nanospheres for skin tissue engineering. Biomacromolecules. 2009;10(6):1642-1649.
[3] SIMÕES D, MIGUEL SP, RIBEIRO MP, et al. Recent advances on antimicrobial wound dressing: A review. Eur J Pharm Biopharm. 2018; 127:130-141.
[4] LIANG Y, HE J, GUO B. Functional hydrogels as wound dressing to enhance wound healing. ACS Nano. 2021;15(8):12687-12722.
[5] XUE J, WANG X, WANG E, et al. Bioinspired multifunctional biomaterials with hierarchical microstructure for wound dressing. Acta Biomater. 2019;100:270-279.
[6] OP’T VELD RC, WALBOOMERS XF, JANSEN JA, et al. Design considerations for hydrogel wound dressings: strategic and molecular advances. Tissue Eng Part B Rev. 2020;26(3):230-248.
[7] GÓRSKA A, DOROŻYŃSKI P, WĘGLARZ WP, et al. Spatiotemporal characterization of hydration process of asymmetric polymeric wound dressings for decubitus ulcers. J Biomed Mater Res B Appl Biomater. 2018;106(2):843-853.
[8] DUOLIKUN T, GHAZALI N, LEO BF, et al. Asymmetric Cellulosic Membranes: Current and Future Aspects. Symmetry. 2020;12(7):1160.
[9] FENG L, SHI W, CHEN Q, et al. Smart Asymmetric Hydrogel with Integrated Multi‐Functions of NIR‐Triggered Tunable Adhesion, Self‐Deformation, and Bacterial Eradication. Adv Healthc Mater. 2021; 2100784.
[10] WU J, QIU Q, WANG Y, et al. Asymmetric water affinity on antibacterial electrospun sub-micro cellulose acetate Janus membrane. Materials Letters. 2019;256:126607.
[11] MI FL, SHYU SS, WU YB, et al. Fabrication and characterization of a sponge-like asymmetric chitosan membrane as a wound dressing. Biomaterials. 2001;22(2):165-173.
[12] LEI M, QU X, LIU H, et al. Programmable electrofabrication of porous janus films with tunable janus balance for anisotropic cell guidance and tissue regeneration. Advanced Functional Materials. 2019;29(18): 1900065.
[13] GRAÇA MFP, DE MELO-DIOGO D, CORREIA IJ, et al. Electrospun Asymmetric Membranes as Promising Wound Dressings: A Review. Pharmaceutics. 2021;13(2):183.
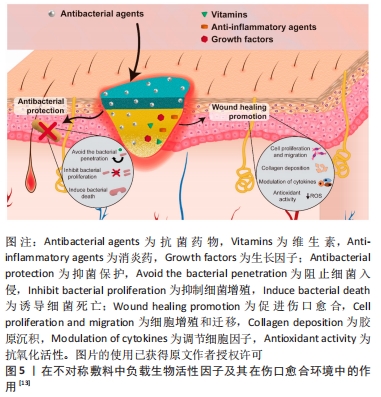
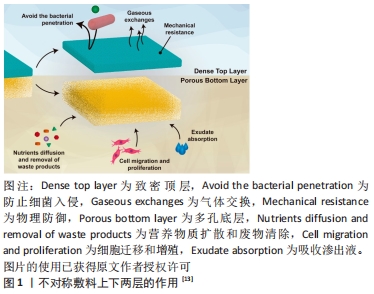
[14] 唐川,关怡新,姚善泾,等.超临界溶液浸渍法制备负载磺胺嘧啶银不对称壳聚糖膜伤口敷料研究[J].高分子学报,2014(6):774-781.
[15] FEDERICO S, PITARRESI G, PALUMBO FS, et al. An asymmetric electrospun membrane for the controlled release of ciprofloxacin and FGF-2: Evaluation of antimicrobial and chemoattractant properties. Mat Sci Eng C. 2021;123:112001.
[16] LI Y, ZHU C, FAN D, et al. Construction of porous sponge-like PVA-CMC-PEG hydrogels with pH-sensitivity via phase separation for wound dressing. Int J Polym Mater Po. 2020;69(8):505-515.
[17] MIGUEL SP, MOREIRA AF, CORREIA IJ. Chitosan based-asymmetric membranes for wound healing: A review. Int J Biol Macromol. 2019; 127:460-475.
[18] MIGUEL SP, RIBEIRO MP, COUTINHO P, et al. Electrospun polycaprolactone/aloe vera_chitosan nanofibrous asymmetric membranes aimed for wound healing applications. Polymers. 2017;9(5):183.
[19] YIN X, WEN Y, LI Y, et al. Facile fabrication of sandwich structural membrane with a hydrogel nanofibrous mat as inner layer for wound dressing application. Front Chem. 2018;6:490.
[20] MIGUEL SP, SIMÕES D, MOREIRA AF, et al. Production and characterization of electrospun silk fibroin based asymmetric membranes for wound dressing applications. Int J Biol Macromol. 2019;121:524-535.
[21] POONGUZHALI R, BASHA SK, KUMARI VS. Novel asymmetric chitosan/PVP/nanocellulose wound dressing: In vitro and in vivo evaluation. Int J Biol Macromol. 2018;112:1300-1309.
[22] FEIZ S, NAVARCHIAN AH, JAZANI OM. Poly (vinyl alcohol) membranes in wound-dressing application: microstructure, physical properties, and drug release behavior. Iran Polym J. 2018;27(3):193-205.
[23] XIA G, ZHAI D, SUN Y, et al. Preparation of a novel asymmetric wettable chitosan-based sponge and its role in promoting chronic wound healing. Carbohydr Polym. 2020;227:115296.
[24] WANG Q, QIAN Z, LIU B, et al. In vitro and in vivo evaluation of new PRP antibacterial moisturizing dressings for infectious wound repair. J Biomater Sci Polym Ed. 2019;30(6):462-485.
[25] RIBBA L, TAMAYO L, FLORES M, et al. Asymmetric biphasic hydrophobic/hydrophilic poly (lactic acid)–polyvinyl alcohol meshes with moisture control and noncytotoxic effects for wound dressing applications. J Appl Polym Sci. 2019;136(17):47369.
[26] NAPAVICHAYANUN S, BONANI W, YANG Y, et al. Fibroin and polyvinyl alcohol hydrogel wound dressing containing silk sericin prepared using high-pressure carbon dioxide. Adv Wound Care. 2019;(9):452-462.
[27] MOUSAVI S M, ZAREI M, HASHEMI S A, et al. Asymmetric membranes: a potential scaffold for wound healing applications. Symmetry. 2020; 12(7):1100.
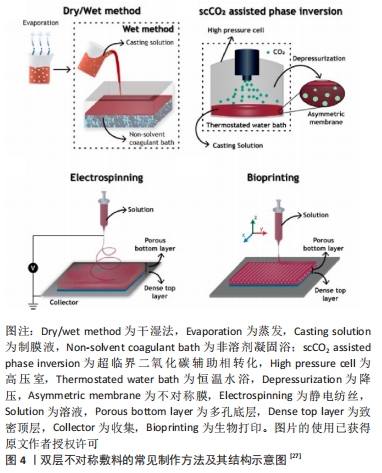
[28] ARAGON J, COSTA C, COELHOSO I, et al. Electrospun asymmetric membranes for wound dressing applications. Mater Sci Eng C Mater Biol Appl. 2019;103:109822.
[29] LI TT, ZHONG Y, PENG HK, et al. Multiscale composite nanofiber membranes with asymmetric wetability: preparation, characterization, and applications in wound dressings. J Mater Sci. 2021;56(6):4407-4419.
[30] REIS TC, CASTLEBERRY S, REGO AMB, et al. Three-dimensional multilayered fibrous constructs for wound healing applications. Biomater Sci. 2016;4(2) 319-330.
[31] DU W, ZHANG Z, FAN W, et al. Fabrication and evaluation of polydimethylsiloxane modified gelatin/silicone rubber asymmetric bilayer membrane with porous structure. Mater Design. 2018;158:28-38.
[32] DU W, ZHANG Z, LI Z. Influence of the weight ratio of polydimethylsiloxane modified gelatin to silicone rubber on the potential performance of asymmetric bilayer membranes as wound dressings. Polym Int. 2019;68(10):1739-1747.
[33] GENEVRO GM, NETO RJG, DE ALMEIDA PAULO L, et al. Glucomannan asymmetric membranes for wound dressing. J Mater Res. 2019;34(4): 481-489.
[34] MIGUEL SP, CABRAL CSD, MOREIRA AF, et al. Production and characterization of a novel asymmetric 3D printed construct aimed for skin tissue regeneration. Colloid Surface B. 2019;181:994-1003.
[35] GAO Y, JIN X. Needle-punched three-dimensional nonwoven wound dressings with density gradient from biocompatible calcium alginate fiber. Text Res J. 2019;89(14):2776-2788.
[36] QI L, OU K, HOU Y, et al. Unidirectional water-transport antibacterial trilayered nanofiber-based wound dressings induced by hydrophilic-hydrophobic gradient and self-pumping effects. Mater Design. 2021; 201:109461.
[37] SU C, ZHAO H, YANG H, et al. Stearic acid-modified starch/chitosan composite sponge with asymmetric and gradient wettability for wound dressing. ACS Appl Bio Mater. 2018;2(1):171-181.
[38] XU Q, SIGEN A, GAO Y, et al. A hybrid injectable hydrogel from hyperbranched PEG macromer as a stem cell delivery and retention platform for diabetic wound healing. Acta Biomater. 2018;75:63-74.
[39] MARCANO A, BOU HAIDAR N, MARAIS S, et al. Designing biodegradable PHA-based 3D scaffolds with antibiofilm properties for wound dressings: optimization of the microstructure/nanostructure. ACS Biomater Sci Eng. 2017;3(12):3654-3661.
[40] WANG Y, XIAO D, ZHONG Y, et al. Facile fabrication of carboxymethyl chitosan/paraffin coated carboxymethylated cotton fabric with asymmetric wettability for hemostatic wound dressing. Cellulose. 2020; 27(6):3443-3453.
[41] GÁMEZ-HERRERA E, GARCÍA-SALINAS S, SALIDO S, et al. Drug-eluting wound dressings having sustained release of antimicrobial compounds. Eur J Pharm Biopharm. 2020;152:327-339.
[42] CHAGAS PAM, SCHNEIDER R, DOS SANTOS DM, et al. Bilayered electrospun membranes composed of poly (lactic-acid)/natural rubber: A strategy against curcumin photodegradation for wound dressing application. React Funct Polym. 2021;163:104889.
[43] HAIDAR N B, MARAIS S, DÉ E, et al. Chronic wound healing: A specific antibiofilm protein-asymmetric release system. Mater Sci Eng C Mater Biol Appl. 2020;106:110130.
[44] YU B, HE C, WANG W, et al. Asymmetric wettable composite wound dressing prepared by electrospinning with bioinspired micropatterning enhances diabetic wound healing. ACS Applied Bio Materials. 2020; 3(8):5383-5394.
[45] ZHANG K, JIAO X, ZHOU L, et al. Nanofibrous composite aerogel with multi-bioactive and fluid gating characteristics for promoting diabetic wound healing. Biomaterials. 2021;276:121040.
[46] LIANG D, LU Z, YANG H, et al. Novel asymmetric wettable AgNPs/chitosan wound dressing: in vitro and in vivo evaluation. ACS Appl Mater Interfaces. 2016;8(6):3958-3968.
[47] QIAN Z, BAI Y, ZHOU J, et al. A moisturizing chitosan-silk fibroin dressing with silver nanoparticles-adsorbed exosomes for repairing infected wounds. J Mater Chem B. 2020;8(32):7197-7212.
[48] LIU M, WANG Y, HU X, et al. Janus N, N-dimethylformamide as a solvent for a gradient porous wound dressing of poly (vinylidene fluoride) and as a reducer for in situ nano-silver production: anti-permeation, antibacterial and antifouling activities against multi-drug-resistant bacteria both in vitro and in vivo. RSC Adv. 2018;8(47):26626-26639.
[49] LIANG Y, ZHAO X, HU T, et al. Adhesive hemostatic conducting injectable composite hydrogels with sustained drug release and photothermal antibacterial activity to promote full‐thickness skin regeneration during wound healing. Small. 2019;15(12):1900046.
[50] PILEHVAR-SOLTANAHMADI Y, DADASHPOUR M, MOHAJERI A, et al. An overview on application of natural substances incorporated with electrospun nanofibrous scaffolds to development of innovative wound dressings. Mini Rev Med Chem. 2018;18(5):414-427.
[51] ASHFAQ M, VERMA N, KHAN S. Highly effective Cu/Zn-carbon micro/nanofiber-polymer nanocomposite-based wound dressing biomaterial against the P. aeruginosa multi-and extensively drug-resistant strains. Mater Sci Eng C Mater Biol Appl. 2017;77:630-641.
[52] WANG H, NIU H, ZHOU H, et al. Multifunctional directional water transport fabrics with moisture sensing capability. ACS applied materials & interfaces. 2019;11(25):22878-22884.
[53] GU J, GU H, ZHANG Q, et al. Sandwich-structured composite fibrous membranes with tunable porous structure for waterproof, breathable, and oil-water separation applications. J Colloid Interface Sci. 2018;514: 386-395.
|