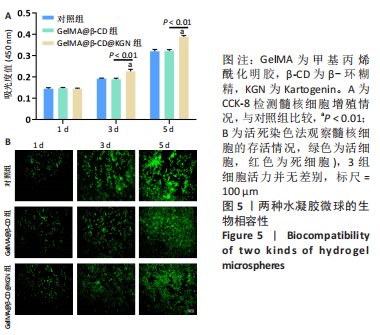
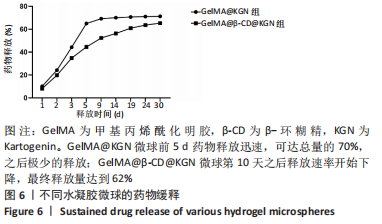
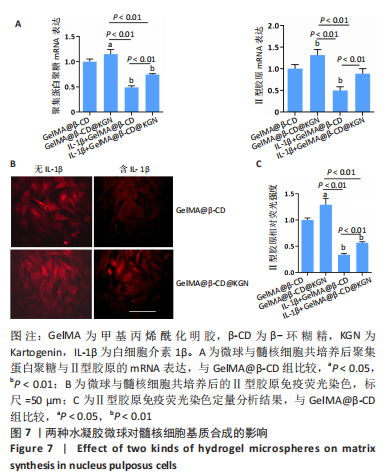
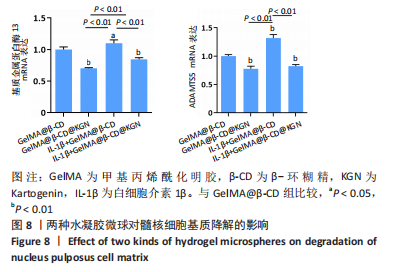
[1] DEYO RA, WEINSTEIN JN. Low back pain. N Engl J Med. 2001;344(5):363-370.
[2] HARTVIGSEN J, HANCOCK MJ, KONGSTED A, et al. What low back pain is and why we need to pay attention. Lancet. 2018;391(10137):2356-2367.
[3] FRANCISCO V, PINO J, GONZÁLEZ-GAY MÁ, et al. A new immunometabolic perspective of intervertebral disc degeneration. Nat Rev Rheumatol. 2022; 18(1):47-60.
[4] ANTONIOU J, STEFFEN T, NELSON F, et al. The human lumbar intervertebral disc: evidence for changes in the biosynthesis and denaturation of the extracellular matrix with growth, maturation, ageing, and degeneration. J Clin Invest. 1996;98(4):996-1003.
[5] BINCH ALA, RATCLIFFE LPD, MILANI AH, et al. Site-Directed Differentiation of Human Adipose-Derived Mesenchymal Stem Cells to Nucleus Pulposus Cells Using an Injectable Hydroxyl-Functional Diblock Copolymer Worm Gel. Biomacromolecules. 2021;22(2):837-845.
[6] JOHNSON K, ZHU S, TREMBLAY MS, et al. A stem cell-based approach to cartilage repair. Science. 2012;336(6082):717-721.
[7] YU C, LI D, WANG C, et al. Injectable kartogenin and apocynin loaded micelle enhances the alleviation of intervertebral disc degeneration by adipose-derived stem cell. Bioact Mater. 2021;6(10):3568-3579.
[8] VAN DEN BULCKE AI, BOGDANOV B, DE ROOZE N, et al. Structural and rheological properties of methacrylamide modified gelatin hydrogels. Biomacromolecules. 2000;1(1):31-38.
[9] DONG Z, MENG X, YANG W, et al. Progress of gelatin-based microspheres (GMSs) as delivery vehicles of drug and cell. Mater Sci Eng C Mater Biol Appl. 2021;122:111949.
[10] XU J, LI J, LIN S, et al. Nanocarrier-mediated codelivery of small molecular drugs and siRNA to enhance chondrogenic differentiation and suppress hypertrophy of human mesenchymal stem cells. Adv Funct Mater. 2016;26: 2463-2472.
[11] MURA P. Advantages of the combined use of cyclodextrins and nanocarriers in drug delivery: A review. Int J Pharm. 2020;579:119181.
[12] XU J, FENG Q, LIN S, et al. Injectable stem cell-laden supramolecular hydrogels enhance in situ osteochondral regeneration via the sustained co-delivery of hydrophilic and hydrophobic chondrogenic molecules. Biomaterials. 2019;210:51-61.
[13] YUE K, TRUJILLO-DE SANTIAGO G, ALVAREZ MM, et al. Synthesis, properties, and biomedical applications of gelatin methacryloyl (GelMA) hydrogels. Biomaterials. 2015;73:254-271.
[14] XU X, LIANG Y, LI X, et al. Exosome-mediated delivery of kartogenin for chondrogenesis of synovial fluid-derived mesenchymal stem cells and cartilage regeneration. Biomaterials. 2021;269:120539.
[15] FRAPIN L, CLOUET J, CHÉDEVILLE C, et al. Controlled release of biological factors for endogenous progenitor cell migration and intervertebral disc extracellular matrix remodelling. Biomaterials. 2020;253:120107.
[16] ZHOU W, DUAN Z, ZHAO J, et al. Glucose and MMP-9 dual-responsive hydrogel with temperature sensitive self-adaptive shape and controlled drug release accelerates diabetic wound healing. Bioact Mater. 2022;17:1-17.
[17] RIBEIRO JS, BORDINI EAF, FERREIRA JA, et al. Injectable MMP-Responsive Nanotube-Modified Gelatin Hydrogel for Dental Infection Ablation. ACS Appl Mater Interfaces. 2020;12(14):16006-16017.
[18] CAI C, ZHANG X, LI Y, et al. Self-Healing Hydrogel Embodied with Macrophage-Regulation and Responsive-Gene-Silencing Properties for Synergistic Prevention of Peritendinous Adhesion. Adv Mater. 2022;34(5): e2106564.
[19] CHANG H, CAI F, ZHANG Y, et al. Silencing Gene-Engineered Injectable Hydrogel Microsphere for Regulation of Extracellular Matrix Metabolism Balance. Small Methods. 2022;6(4):e2101201.
[20] LI L, DU Y, XIONG Y, et al. Injectable negatively charged gelatin microsphere-based gels as hemostatic agents for intracavitary and deep wound bleeding in surgery. J Biomater Appl. 2018;33(5):647-661.
[21] BIAN J, CAI F, CHEN H, et al. Modulation of Local Overactive Inflammation via Injectable Hydrogel Microspheres. Nano Lett. 2021;21(6):2690-2698.
[22] YANG J, LIANG J, ZHU Y, et al. Fullerol-hydrogel microfluidic spheres for in situ redox regulation of stem cell fate and refractory bone healing. Bioact Mater. 2021;6(12):4801-4815.
[23] ZHANG C, GULLBRAND SE, SCHAER TP, et al. Combined Hydrogel and Mesenchymal Stem Cell Therapy for Moderate-Severity Disc Degeneration in Goats. Tissue Eng Part A. 2021;27(1-2):117-128.
[24] SAKAI D, ANDERSSON GB. Stem cell therapy for intervertebral disc regeneration: obstacles and solutions. Nat Rev Rheumatol. 2015;11(4):243-256.
[25] MWALE F, ROUGHLEY P, ANTONIOU J. Distinction between the extracellular matrix of the nucleus pulposus and hyaline cartilage: a requisite for tissue engineering of intervertebral disc. Eur Cell Mater. 2004;8:58-63.
[26] HUGHES SP, FREEMONT AJ, HUKINS DW, et al. The pathogenesis of degeneration of the intervertebral disc and emerging therapies in the management of back pain. J Bone Joint Surg Br. 2012;94(10):1298-1304.
[27] LE MAITRE CL, POCKERT A, BUTTLE DJ, et al. Matrix synthesis and degradation in human intervertebral disc degeneration. Biochem Soc Trans. 2007;35(Pt 4):652-655.
[28] LIU T, LI X, WANG T, et al. Kartogenin mediates cartilage regeneration by stimulating the IL-6/Stat3-dependent proliferation of cartilage stem/progenitor cells. Biochem Biophys Res Commun. 2020;532(3):385-392.
[29] BAHARLOU HOUREH A, MASAELI E, NASR-ESFAHANI MH. Chitosan/polycaprolactone multilayer hydrogel: A sustained Kartogenin delivery model for cartilage regeneration. Int J Biol Macromol. 2021;177:589-600.
[30] ZHANG M, HU W, CAI C, et al. Advanced application of stimuli-responsive drug delivery system for inflammatory arthritis treatment. Mater Today Bio. 2022;14:100223.
[31] HUANG Y, JIANG T, CHEN J, et al. Effects of kartogenin on the attenuated nucleus pulposus cell degeneration of intervertebral discs induced by interleukin-1β and tumor necrosis factor-α. Int J Mol Med. 2018;41(2): 749-756.
[32] HOU M, ZHANG Y, ZHOU X, et al. Kartogenin prevents cartilage degradation and alleviates osteoarthritis progression in mice via the miR-146a/NRF2 axis. Cell Death Dis. 2021;12(5):483.
[33] FENG Q, LI D, LI Q, et al. Dynamic Nanocomposite Microgel Assembly with Microporosity, Injectability, Tissue-Adhesion, and Sustained Drug Release Promotes Articular Cartilage Repair and Regeneration. Adv Healthc Mater. 2022;11(8):e2102395.
[34] ZHANG YJ, YIN WL, LIU Y, et al. Dynamic protein hydrogel with supramolecularly enveloped kartogenin promotes cartilage regeneration through mitochondrial activation. Compos B Eng. 2022;246:1359-8368.
[35] MA CJ, LIU X, CHE L, et al. Stem Cell Therapies for Intervertebral Disc Degeneration: Immune Privilege Reinforcement by Fas/FasL Regulating Machinery. Curr Stem Cell Res Ther. 2015;10(4):285-295.
[36] XU H, SUN M, WANG C, et al. Growth differentiation factor-5-gelatin methacryloyl injectable microspheres laden with adipose-derived stem cells for repair of disc degeneration. Biofabrication. 2020;13(1):015010.
[37] RUOSLAHTI E. RGD and other recognition sequences for integrins. Annu Rev Cell Dev Biol. 1996;12:697-715.
[38] RUTGES J, CREEMERS LB, DHERT W, et al. Variations in gene and protein expression in human nucleus pulposus in comparison with annulus fibrosus and cartilage cells: potential associations with aging and degeneration. Osteoarthritis Cartilage. 2010;18(3):416-423. |