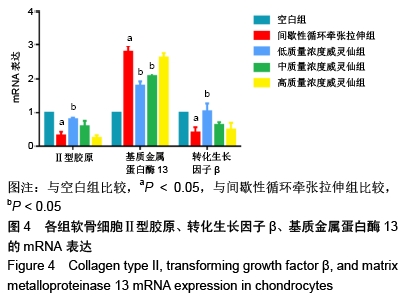
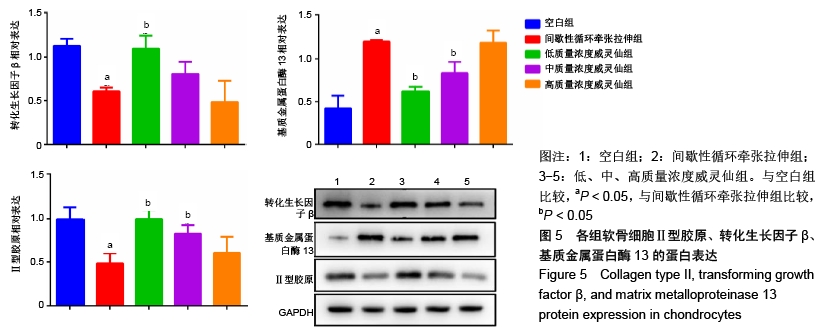
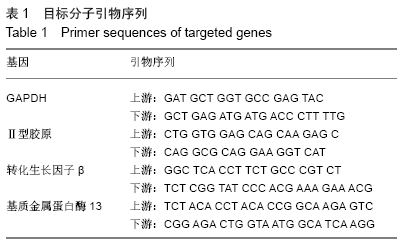
[1] JØRGENSEN AEM, KJÆR M, HEINEMEIER KM. The Effect of Aging and Mechanical Loading on the Metabolism of Articular Cartilage. J Rheumatol. 2017;44(4):410-417.
[2] BLEUEL J, ZAUCKE F, BRÜGGEMANN GP, et al. Effects of cyclic tensile strain on chondrocyte metabolism: a systematic review. PLoS One. 2015;10(3):e0119816.
[3] SALINAS EY, HU JC, ATHANASIOU K. A Guide for Using Mechanical Stimulation to Enhance Tissue-Engineered Articular Cartilage Properties. Tissue Eng Part B Rev. 2018;24(5):345-358.
[4] HOSSEINI SM, VELDINK MB, ITO K, et al. Is collagen fiber damage the cause of early softening in articular cartilage. Osteoarthritis Cartilage. 2013;21(1):136-143.
[5] MARIANI E, PULSATELLI L, FACCHINI A. Signaling pathways in cartilage repair. Int J Mol Sci. 2014;15(5):8667-8698.
[6] MARTIN JA, BUCKWALTER JA. The role of chondrocyte senescence in the pathogenesis of osteoarthritis and in limiting cartilage repair. J Bone Joint Surg Am. 2003;85-A Suppl 2: 106-110.
[7] FU Q, ZAN K, ZHAO M, et al. Triterpene saponins from Clematis chinensis and their potential anti-inflammatory activity. J Nat Prod. 2010;73(7):1234-1239.
[8] FU Q, ZAN K, ZHAO MB, et al. Three new triterpene saponins from Clematis chinensis. J Asian Nat Prod Res. 2013;15(6): 610-618.
[9] PAN T, CHENG TF, JIA YR, et al. Anti-rheumatoid arthritis effects of traditional Chinese herb couple in adjuvant-induced arthritis in rats. J Ethnopharmacol. 2017;205:1-7.
[10] PAN YL,MA Y, GUO Y, et al. Effects of Clematis chinensis Osbeck mediated by low-intensity pulsed ultrasound on transforming growth factor-beta/Smad signaling in rabbit articular chondrocytes. Journal of Medical Ultrasonics. 2019;46(2):177-186.
[11] WU W, XU X, DAI Y, et al. Therapeutic effect of the saponin fraction from Clematis chinensis Osbeck roots on osteoarthritis induced by monosodium iodoacetate through protecting articular cartilage. Phytother Res. 2010;24(4):538-546.
[12] CORREA D, LIETMAN SA. Articular cartilage repair: Current needs, methods and research directions. Semin Cell Dev Biol. 2017;62:67-77.
[13] HELMARK IC, MIKKELSEN UR, BØRGLUM J, et al. Exercise increases interleukin-10 levels both intraarticularly and peri-synovially in patients with knee osteoarthritis: a randomized controlled trial. Arthritis Res Ther. 2010;12(4):R126.
[14] MUSUMECI G, CASTROGIOVANNI P, TROVATO FM, et al. Physical activity ameliorates cartilage degeneration in a rat model of aging: a study on lubricin expression. Scand J Med Sci Sports. 2015;25(2): e222-230.
[15] MUSUMECI G, LORETO C, LEONARDI R, et al. The effects of physical activity on apoptosis and lubricin expression in articular cartilage in rats with glucocorticoid-induced osteoporosis. J Bone Miner Metab. 2013;31(3):274-284.
[16] MONONEN ME, TANSKA P, ISAKSSON H, et al. A Novel Method to Simulate the Progression of Collagen Degeneration of Cartilage in the Knee: Data from the Osteoarthritis Initiative. Sci Rep. 2016;6:21415.
[17] MARIANI E, PULSATELLI L, FACCHINI A. Signaling pathways in cartilage repair. Int J Mol Sci. 2014;15(5):8667-8698.
[18] HWANG HS, PARK SJ, CHEON EJ, et al. Fibronectin fragment-induced expression of matrix metalloproteinases is mediated by MyD88-dependent TLR-2 signaling pathway in human chondrocytes. Arthritis Res Ther. 2015;17:320.
[19] KOIKE M, NOJIRI H, OZAWA Y, et al. Mechanical overloading causes mitochondrial superoxide and SOD2 imbalance in chondrocytes resulting in cartilage degeneration. Sci Rep. 2015;5:11722.
[20] XU HG, GAO Z, MA MM, et al. P120-Catenin Mediates Intermittent Cyclic Mechanical Tension-Induced Inflammation in Chondrocytes. J Cell Biochem. 2017;118(12):4508-4516.
[21] XU HG, ZHANG XH, WANG H, et al. Intermittent Cyclic Mechanical Tension-Induced Calcification and downregulation of ankh gene expression of end plate chondrocytes. Spine (Phila Pa 1976). 2012;37(14):1192-1197.
[22] XU HG, ZHENG Q, SONG JX, et al. Intermittent cyclic mechanical tension promotes endplate cartilage degeneration via canonical Wnt signaling pathway and E-cadherin/β-catenin complex cross-talk. Osteoarthritis Cartilage. 2016;24(1):158-168.
[23] XIAO L, XU S, XU Y, et al. TGF-β/SMAD signaling inhibits intermittent cyclic mechanical tension-induced degeneration of endplate chondrocytes by regulating the miR-455-5p/RUNX2 axis. J Cell Biochem. 2018;119(12):10415-10425.
[24] ZHU M, ZHOU S, HUANG Z, et al. Ca2+-Dependent Endoplasmic Reticulum Stress Regulates Mechanical Stress-Mediated Cartilage Thinning. J Dent Res. 2016;95(8):889-896
[25] LI C, WANG Q, WANG JF. Transforming growth factor-β (TGF-β) induces the expression of chondrogenesis-related genes through TGF-β receptor II (TGFRII)-AKT-mTOR signaling in primary cultured mouse precartilaginous stem cells. Biochem Biophys Res Commun. 2014;450(1):646-651.
[26] YIN F, CAI J, ZEN W, et al. Cartilage Regeneration of Adipose-Derived Stem Cells in the TGF-β1-Immobilized PLGA-Gelatin Scaffold. Stem Cell Rev. 2015;11(3):453-459.
[27] 周效思,周凯,谭安雄,等.威灵仙对兔膝骨关节炎结构和功能的影响[J].时珍国医国药,2011,22(10):2454-2456.
[28] 孙必强,张鸣,李美珍,等. 威灵仙注射液关节腔离子导入对骨关节炎软骨和滑膜组织形态以及软骨MMP-1的影响[J].中医临床研究, 2014,6(17):1-3.
[29] 徐扬,桂鉴超,高峰,等.威灵仙提取物干预膝骨关节炎软骨细胞的生长活力[J].中国组织工程研究,2013,17(2):241-246.
[30] 马勇,张允申,陈金飞,等.威灵仙干预体外培养兔膝关节软骨细胞增殖及转化生长因子β1mRNA基因的表达[J].中国组织工程研究与临床康复, 2010,14(11):1901-1906.
[31] 马勇,陈金飞,张允申,等.可注射性壳聚糖/β-甘油磷酸二钠凝胶复合同种异体软骨细胞修复兔膝关节软骨缺损及威灵仙的干预效应[J]. 中国组织工程研究与临床康复,2010,14(16):2864-2869.
|