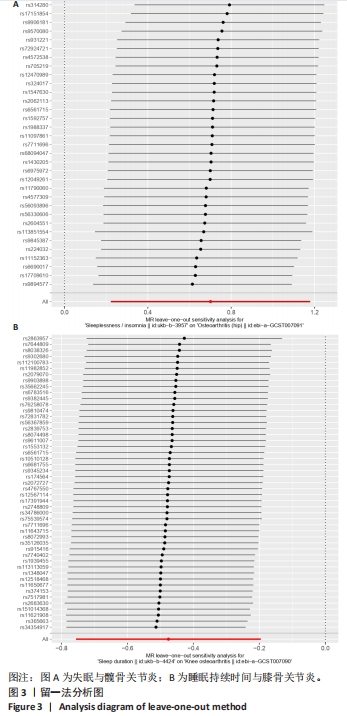
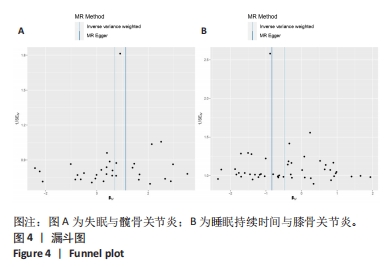
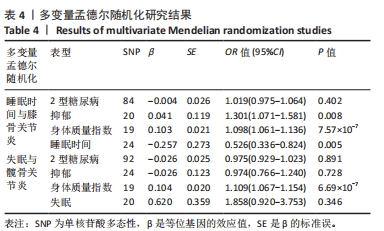
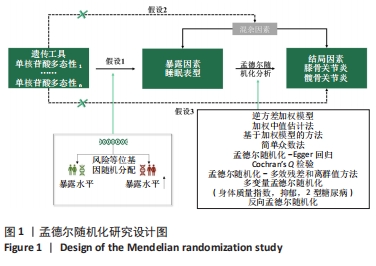
[1] KOLASINSKI SL, NEOGI T, HOCHBERG MC, et al. 2019 American College of Rheumatology/Arthritis Foundation Guideline for the Management of Osteoarthritis of the Hand, Hip, and Knee. Arthritis Rheumatol. 2020;72(2):220-233.
[2] SHARMA L. Osteoarthritis of the Knee. N Engl J Med. 2021;384(1):51-59.
[3] SCHÄFER N, GRÄSSEL S. Targeted therapy for osteoarthritis: progress and pitfalls. Nat Med. 2022;28(12):2473-2475.
[4] TONG L, YU H, HUANG X, et al. Current understanding of osteoarthritis pathogenesis and relevant new approaches. Bone Res. 2022;10(1):60.
[5] XIE J, WANG Y, LU L, et al. Cellular senescence in knee osteoarthritis: molecular mechanisms and therapeutic implications. Ageing Res Rev. 2021;70:101413.
[6] YAO Q, WU X, TAO C, et al. Osteoarthritis: pathogenic signaling pathways and therapeutic targets. Signal Transduct Target Ther. 2023;8(1):56.
[7] MCKENNA S, LARKIN L, DONNELLY A, et al. OP0267-HPR “I NEVER THOUGHT EXERCISE COULD HELP IMPROVE MY SLEEP”: Experiences of people with rheumatoid arthritis on the impact of exercise on sleep. Ann Rheum Dis. 2020; 79(Suppl 1): 161-167.
[8] JACOB L, SMITH L, KONRAD M, et al. Association between sleep disorders and osteoarthritis: A case-control study of 351,932 adults in the UK. J Sleep Res. 2021;30(6):e13367.
[9] JUNG JH, SEOK H, CHOI SJ, et al. The association between osteoarthritis and sleep duration in Koreans: a nationwide cross-sectional observational study. Clin Rheumatol. 2018;37(6):1653-1659.
[10] PARK HM, KWON YJ, KIM HS, et al. Relationship between Sleep Duration and Osteoarthritis in Middle-Aged and Older Women: A Nationwide Population-Based Study. J Clin Med. 2019;8(3):356.
[11] LATORRE D, SALLUSTO F, BASSETTI CLA, et al. Narcolepsy: a model interaction between immune system, nervous system, and sleep-wake regulation. Semin Immunopathol. 2022;44(5):611-623.
[12] IRWIN MR, STRAUB RH, SMITH MT. Heat of the night: sleep disturbance activates inflammatory mechanisms and induces pain in rheumatoid arthritis. Nat Rev Rheumatol. 2023;19(9):545-559.
[13] XING X, WANG Y, PAN F, et al. Osteoarthritis and risk of type 2 diabetes: A two-sample Mendelian randomization analysis. J Diabetes. 2023 Jul 31. doi: 10.1111/1753-0407.13451.
[14] ZHANG L, ZHANG W, WU X, et al. A sex- and site-specific relationship between body mass index and osteoarthritis: evidence from observational and genetic analyses. Osteoarthritis Cartilage. 2023;31(6):819-828.
[15] BAROWSKY S, JUNG JY, NESBIT N, et al. Cross-Disorder Genomics Data Analysis Elucidates a Shared Genetic Basis Between Major Depression and Osteoarthritis Pain. Front Genet. 2021;12:687687.
[16] NAZARZADEH M, PINHO-GOMES AC, BIDEL Z, et al. Plasma lipids and risk of aortic valve stenosis: a Mendelian randomization study. Eur Heart J. 2020;41(40):3913-3920.
[17] LAWLOR DA, HARBORD RM, STERNE JA, et al. Mendelian randomization: using genes as instruments for making causal inferences in epidemiology. Stat Med. 2008;27(8):1133-1163.
[18] CLAYTON GL, SOARES AG, GOULDING N, et al. A framework for assessing selection and misclassification bias in mendelian randomisation studies: an illustrative example between body mass index and covid-19. BMJ. 2023;381:e072148.
[19] SKRIVANKOVA VW, RICHMOND RC, WOOLF BAR, et al. Strengthening the reporting of observational studies in epidemiology using mendelian randomisation (STROBE-MR): explanation and elaboration. BMJ. 2021;375:n2233.
[20] FABER BG, FRYSZ M, BOER CG, et al. The identification of distinct protective and susceptibility mechanisms for hip osteoarthritis: findings from a genome-wide association study meta-analysis of minimum joint space width and Mendelian randomisation cluster analyses. EBioMedicine. 2023;95:104759.
[21] YANG J, LIU P, WANG S, et al. Causal relationship between sarcopenia and osteoarthritis: a bi-directional two-sample mendelian randomized study. Eur J Med Res. 2023;28(1):327.
[22] SU D, AI Y, ZHU G, et al. Genetically predicted circulating levels of cytokines and the risk of osteoarthritis: A mendelian randomization study. Front Genet. 2023;14:1131198.
[23] ZHANG Y, XIE J, WEN S, et al. Evaluating the causal effect of circulating proteome on the risk of osteoarthritis-related traits. Ann Rheum Dis. 2023 Aug 18. doi: 10.1136/ard-2023-224459.
[24] TACHMAZIDOU I, HATZIKOTOULAS K, SOUTHAM L, et al. Identification of new therapeutic targets for osteoarthritis through genome-wide analyses of UK Biobank data. Nat Genet. 2019;51(2):230-236.
[25] HOWARD DM, ADAMS MJ, CLARKE TK, et al. Genome-wide meta-analysis of depression identifies 102 independent variants and highlights the importance of the prefrontal brain regions. Nat Neurosci. 2019;22(3):343-352.
[26] XUE A, WU Y, ZHU Z, et al. Genome-wide association analyses identify 143 risk variants and putative regulatory mechanisms for type 2 diabetes. Nat Commun. 2018;9(1):2941.
[27] BURGESS S, DAVEY SMITH G, DAVIES NM, et al. Guidelines for performing Mendelian randomization investigations: update for summer 2023. Wellcome Open Res. 2023;4:186.
[28] SKRIVANKOVA VW, RICHMOND RC, WOOLF BAR, et al. Strengthening the Reporting of Observational Studies in Epidemiology Using Mendelian Randomization: The STROBE-MR Statement. JAMA. 2021;326(16):1614-1621.
[29] QIU S, ZHENG K, HU Y, et al. Genetic correlation, causal relationship, and shared loci between vitamin D and COVID-19: A genome-wide cross-trait analysis. J Med Virol. 2023;95(5):e28780.
[30] LEVIN MG, JUDY R, GILL D, et al. Genetics of height and risk of atrial fibrillation: A Mendelian randomization study. PLoS Med. 2020;17(10):e1003288.
[31] CODD V, NELSON CP, ALBRECHT E, et al. Identification of seven loci affecting mean telomere length and their association with disease. Nat Genet. 2013;45(4):422-427.
[32] LI W, LU Q, QIAN J, et al. Assessing the causal relationship between genetically determined inflammatory biomarkers and low back pain risk: a bidirectional two-sample Mendelian randomization study. Front Immunol. 2023;14:1174656.
[33] YUAN S, MIAO Y, RUAN X, et al. Therapeutic role of interleukin-1 receptor antagonist in pancreatic diseases: mendelian randomization study. Front Immunol. 2023;14:1240754.
[34] HAN Y, ZHANG Y, ZENG X. Assessment of causal associations between uric acid and 25-hydroxyvitamin D levels. Front Endocrinol (Lausanne). 2022;13:1024675.
[35] DOBRIJEVIC E, VAN ZWIETEN A, KIRYLUK K, et al. Mendelian randomization for nephrologists. Kidney Int. 2023 Sep 30. doi: 10.1016/j.kint.2023.09.016.
[36] LI J, BAI H, QIAO H, et al. Causal effects of COVID-19 on cancer risk: A Mendelian randomization study. J Med Virol. 2023;95(4):e28722.
[37] YAO S, ZHANG M, DONG SS, et al. Bidirectional two-sample Mendelian randomization analysis identifies causal associations between relative carbohydrate intake and depression. Nat Hum Behav. 2022;6(11):1569-1576.
[38] SHANG W, ZHANG S, QIAN H, et al. Association of gut microbiota with COVID-19 susceptibility and severity: A two-sample Mendelian randomization study. J Med Virol. 2023;95(4):e28734.
[39] MAZIDI M, SHEKOOHI N, KATSIKI N, et al. Impact of lifetime concentration of mannose on renal function: insights from Mendelian randomization. Eur Heart J. 2022;43(S2):ehac544.2612.
[40] ZHOU F, LI S, XU H. Insomnia, sleep duration, and risk of anxiety: A two-sample Mendelian randomization study. J Psychiatr Res. 2022;155:219-225.
[41] LEE MS, SHIN JS, LEE J, et al. The association between mental health, chronic disease and sleep duration in Koreans: a cross-sectional study. BMC Public Health. 2015;15:1200.
[42] GONZALEZ C, KUSKO D, SIBILLE K, et al. Clinical pain, pain catastrophizing, and sleep quality in Ethnic/Race Groups with or at risk for Knee Osteoarthritis: A moderated mediation model. J Pain. 2021;22(5):598.
[43] WANG Y, LI X, ZHANG Y, et al. Association of Sleep Disturbance With Catastrophizing and Knee Pain: Data From the Osteoarthritis Initiative. Arthritis Care Res (Hoboken). 2023;75(10):2134-2141.
[44] VITIELLO MV, ZHU W, VON KORFF M, et al. Long-term improvements in sleep, pain, depression, and fatigue in older adults with comorbid osteoarthritis pain and insomnia. Sleep. 2022;45(2):zsab231.
[45] IRWIN MR, OPP MR. Sleep Health: Reciprocal Regulation of Sleep and Innate Immunity. Neuropsychopharmacology. 2017;42(1):129-155.
[46] WOODELL-MAY JE, SOMMERFELD SD. Role of Inflammation and the Immune System in the Progression of Osteoarthritis. J Orthop Res. 2020;38(2):253-257.
[47] NA HS, PARK JS, CHO KH, et al. Interleukin-1-Interleukin-17 Signaling Axis Induces Cartilage Destruction and Promotes Experimental Osteoarthritis. Front Immunol. 2020;11:730.
[48] ROHLEDER N, ARINGER M, BOENTERT M. Role of interleukin-6 in stress, sleep, and fatigue. Ann N Y Acad Sci. 2012;1261:88-96.
[49] WU J, LI Q, DENG J, et al. Association between IL-33 and other inflammatory factors in patients with rheumatoid arthritis and in fibroblast-like synoviocytes in vitro. Exp Ther Med. 2021;21(2):161.
[50] HOSSAIN FM, HONG Y, JIN Y, et al. Physiological and Pathological Role of Circadian Hormones in Osteoarthritis: Dose-Dependent or Time-Dependent? J Clin Med. 2019;8(9):1415.
[51] CHAPUT JP, MCHILL AW, COX RC, et al. The role of insufficient sleep and circadian misalignment in obesity. Nat Rev Endocrinol. 2023;19(2):82-97.
[52] MULUGETA A, ESHETIE TC, KASSIE GM, et al. Association Between Metabolically Different Adiposity Subtypes and Osteoarthritis: A Mendelian Randomization Study. Arthritis Care Res (Hoboken). 2023;75(4):885-892.
[53] LI W, WANG Z, CAO J, et al. Melatonin improves the homeostasis of mice gut microbiota rhythm caused by sleep restriction. Microbes Infect. 2023;25(6): 105121.
[54] ZHANG M, ZHANG M, KOU G, et al. The relationship between gut microbiota and inflammatory response, learning and memory in mice by sleep deprivation. Front Cell Infect Microbiol. 2023;13:1159771.
[55] LIU L, TIAN F, LI GY, et al. The effects and significance of gut microbiota and its metabolites on the regulation of osteoarthritis: Close coordination of gut-bone axis. Front Nutr. 2022;9:1012087.
[56] GUAN Z, JIN X, GUAN Z, et al. The gut microbiota metabolite capsiate regulate SLC2A1 expression by targeting HIF-1α to inhibit knee osteoarthritis-induced ferroptosis. Aging Cell. 2023;22(6):e13807.
[57] BIRNEY E. Mendelian Randomization. Cold Spring Harb Perspect Med. 2022;12(4): a041302.
[58] WEITH M, BEYER A. The next step in Mendelian randomization. Elife. 2023;12: e86416. |