[1] EL-FARRASH RA, ALI RH, BARAKAT NM. Post-natal bone physiology. Semin Fetal Neonatal Med. 2020;25(1):101077.
[2] DATTA HK, NG WF, WALKER JA, et al. The cell biology of bone metabolism. J Clin Pathol. 2008;61(5):577-587.
[3] GOULD NR, TORRE OM, LESER JM, et al. The cytoskeleton and connected elements in bone cell mechano-transduction. Bone. 2021;149:115971.
[4] UDA Y, AZAB E, SUN N, et al. Osteocyte Mechanobiology. Curr Osteoporos Rep. 2017;15(4):318-325.
[5] CHEN X, WANG Z, DUAN N, et al. Osteoblast-osteoclast interactions. Connect Tissue Res. 2018;59(2):99-107.
[6] GORI F, SUPERTI-FURGA A, BARON R. Bone Formation and the Wnt Signaling Pathway. N Engl J Med. 2016;375(19):1902-1903.
[7] CHEN G, DENG C, LI YP. TGF-β and BMP signaling in osteoblast differentiation and bone formation. Int J Biol Sci. 2012;8(2):272-288.
[8] CHAN WCW, TAN Z, TO MKT, et al. Regulation and Role of Transcription Factors in Osteogenesis. Int J Mol Sci. 2021;22(11):5445.
[9] ZHANG K, LIU X, WANG L, et al. The mechanosensory and mechanotransductive processes mediated by ion channels and the impact on bone metabolism: A systematic review. Arch Biochem Biophys. 2021;711:109020.
[10] HENSLEY AP, MCALINDEN A. The role of microRNAs in bone development. Bone. 2021;143:115760.
[11] 姚依村,梁伟国,叶冬平. 细胞骨架与力学信号传导[J]. 中国组织工程研究,2014,18(7):1109-1114.
[12] XIONG J, ONAL M, JILKA RL, et al. Matrix-embedded cells control osteoclast formation. Nat Med. 2011;17(10):1235-1241.
[13] COLLET P, UEBELHART D, VICO L, et al. Effects of 1- and 6-month spaceflight on bone mass and biochemistry in two humans. Bone. 1997;20(6):547-551.
[14] FAN C, WU Z, COOPER DML, et al. Activation of Focal Adhesion Kinase Restores Simulated Microgravity-Induced Inhibition of Osteoblast Differentiation via Wnt/Β-Catenin Pathway. Int J Mol Sci. 2022;23(10):5593.
[15] BRAVEBOY-WAGNER J, LELKES PI. Impairment of 7F2 osteoblast function by simulated partial gravity in a Random Positioning Machine. NPJ Microgravity. 2022;8(1):20.
[16] MORABITO C, GUARNIERI S, CUCINA A, et al. Antioxidant Strategy to Prevent Simulated Microgravity-Induced Effects on Bone Osteoblasts. Int J Mol Sci. 2020;21(10):3638.
[17] XU H, WU F, ZHANG H, et al. Actin cytoskeleton mediates BMP2-Smad signaling via calponin 1 in preosteoblast under simulated microgravity. Biochimie. 2017;138:184-193.
[18] ROLVIEN T, AMLING M. Disuse Osteoporosis: Clinical and Mechanistic Insights. Calcif Tissue Int. 2022;110(5):592-604.
[19] WOODCOCK EM, GIRVAN P, ECKERT J, et al. Measuring Intracellular Viscosity in Conditions of Hypergravity. Biophys J. 2019;116(10):1984-1993.
[20] MIWA M, KOZAWA O, TOKUDA H, et al. Effects of hypergravity on proliferation and differentiation of osteoblast-like cells. Bone Miner. 1991; 14(1):15-25.
[21] ZHOU S, YANG X, HU J, et al. Continuous hypergravity alters the cytoplasmic elasticity of MC3T3-E1 osteoblasts via actin filaments. J Biomech. 2018;72: 222-227.
[22] KAWAO N, MORITA H, IEMURA S, et al. Roles of Dkk2 in the Linkage from Muscle to Bone during Mechanical Unloading in Mice. Int J Mol Sci. 2020; 1(7):2547.
[23] ALFORD AI, KOZLOFF KM, HANKENSON KD. Extracellular matrix networks in bone remodeling. Int J Biochem Cell Biol. 2015;65:20-31.
[24] YANG X, JIANG J, ZHOU L, et al. Osteogenic and angiogenic characterization of mandible and femur osteoblasts. J Mol Histol. 2019; 50(2):105-117.
[25] SONG F, WANG Y, JIANG D, et al. Cyclic Compressive Stress Regulates Apoptosis in Rat Osteoblasts: Involvement of PI3K/Akt and JNK MAPK Signaling Pathways. PLoS One. 2016;11(11):e0165845.
[26] SHEN XQ, GENG YM, LIU P, et al. Magnitude-dependent response of osteoblasts regulated by compressive stress. Sci Rep. 2017;7:44925.
[27] YONG J, VON BREMEN J, RUIZ-HEILAND G, et al. Adiponectin as Well as Compressive Forces Regulate in vitro β-Catenin Expression on Cementoblasts via Mitogen-Activated Protein Kinase Signaling Activation. Front Cell Dev Biol. 2021;9:645005.
[28] CHEN X, GUO J, YUAN Y, et al. Cyclic compression stimulates osteoblast differentiation via activation of the Wnt/β-catenin signaling pathway. Mol Med Rep. 2017;15(5):2890-2896.
[29] SOMEMURA S, KUMAI T, YATABE K, et al. Physiologic Mechanical Stress Directly Induces Bone Formation by Activating Glucose Transporter 1 (Glut 1) in Osteoblasts, Inducing Signaling via NAD+-Dependent Deacetylase (Sirtuin 1) and Runt-Related Transcription Factor 2 (Runx2). Int J Mol Sci. 2021;22(16):9070.
[30] INOUE A, NAKAO-KUROISHI K, KOMETANI-GUNJIGAKE K, et al. VNUT/SLC17A9, a vesicular nucleotide transporter, regulates osteoblast differentiation. FEBS Open Bio. 2020;10(8):1612-1623.
[31] XU W, LU Y, YUE J, et al. Occlusal trauma inhibits osteoblast differentiation and bone formation through IKK-NF-κB signaling. J Periodontol. 2020; 91(5):683-692.
[32] LU Q, XU W, LIU L, et al. Traumatic compressive stress inhibits osteoblast differentiation through long chain non-coding RNA Dancr. J Periodontol. 2020;91(11):1532-1540.
[33] ŞEN S, LUX CJ, ERBER R. A Potential Role of Semaphorin 3A during Orthodontic Tooth Movement. Int J Mol Sci. 2021;22(15):8297.
[34] TANG LL, WANG YL, PAN J, et al. The effect of step-wise increased stretching on rat calvarial osteoblast collagen production. J Biomech. 2004;37(1):157-161.
[35] SONG CX, LIU SY, ZHU WT, et al. Excessive mechanical stretchmediated osteoblasts promote the catabolism and apoptosis of chondrocytes via the Wnt/βcatenin signaling pathway. Mol Med Rep. 2021;24(2):593.
[36] YU KW, YAO CC, JENG JH, et al. Periostin inhibits mechanical stretch-induced apoptosis in osteoblast-like MG-63 cells. J Formos Med Assoc. 2018;117(4):292-300.
[37] BHATT KA, CHANG EI, WARREN SM, et al. Uniaxial mechanical strain: an in vitro correlate to distraction osteogenesis. J Surg Res. 2007;143(2):329-336.
[38] TANG L, LIN Z, LI YM. Effects of different magnitudes of mechanical strain on Osteoblasts in vitro. Biochem Biophys Res Commun. 2006;344(1):122-128.
[39] XIAO X, ZOU S, CHEN J. Cyclic tensile force modifies calvarial osteoblast function via the interplay between ERK1/2 and STAT3. BMC Mol Cell Biol. 2023;24(1):9.
[40] GONG X, SUN S, YANG Y, et al. Osteoblastic STAT3 Is Crucial for Orthodontic Force Driving Alveolar Bone Remodeling and Tooth Movement. J Bone Miner Res. 2023;38(1):214-227.
[41] DANCIU TE, ADAM RM, NARUSE K, et al. Calcium regulates the PI3K-Akt pathway in stretched osteoblasts. FEBS Lett. 2003;536(1-3):193-197.
[42] ZENG Z, JING D, ZHANG X, et al. Cyclic mechanical stretch promotes energy metabolism in osteoblast-like cells through an mTOR signaling-associated mechanism. Int J Mol Med. 2015;36(4):947-956.
[43] WANG D, CAI J, ZENG Z, et al. The interactions between mTOR and NF-κB: A novel mechanism mediating mechanical stretch-stimulated osteoblast differentiation. J Cell Physiol. 2020. doi: 10.1002/jcp.30184.
[44] KUMAR R, TIWARI AK, TRIPATHI D, et al. Anatomical variations in cortical bone surface permeability: Tibia versus femur. J Mech Behav Biomed Mater. 2021;113:104122.
[45] PRICE C, ZHOU X, LI W, et al. Real-time measurement of solute transport within the lacunar-canalicular system of mechanically loaded bone: direct evidence for load-induced fluid flow. J Bone Miner Res. 2011;26(2):277-285.
[46] LEI X, LIU Q, LI S, et al. Effects of fluid shear stress on expression of focal adhesion kinase in MG-63 human osteoblast-like cells on different surface modification of titanium. Bioengineered. 2021;12(1):4962-4971.
[47] JIN J, JASPERS RT, WU G, et al. Shear Stress Modulates Osteoblast Cell and Nucleus Morphology and Volume. Int J Mol Sci. 2020;21(21):8361.
[48] YU L, WANG X, GAO X, et al. The calcium transient characteristics induced by fluid shear stress affect the osteoblast proliferation. Exp Cell Res. 2018; 362(1):51-62.
[49] DING N, GENG B, LI Z, et al. Fluid shear stress promotes osteoblast proliferation through the NFATc1-ERK5 pathway. Connect Tissue Res. 2019; 60(2):107-116.
[50] ZHANG B, AN L, GENG B, et al. ERK5 negatively regulates Kruppel-like factor 4 and promotes osteogenic lineage cell proliferation in response to MEK5 overexpression or fluid shear stress. Connect Tissue Res. 2021;62(2):194-205.
[51] WANG X, HE J, WANG H, et al. Fluid shear stress regulates osteoblast proliferation and apoptosis via the lncRNA TUG1/miR-34a/FGFR1 axis. J Cell Mol Med. 2021;25(18):8734-8747.
[52] PRODANOV L, SEMEINS CM, VAN LOON JJ, et al. Influence of nanostructural environment and fluid flow on osteoblast-like cell behavior: a model for cell-mechanics studies. Acta Biomater. 2013;9(5):6653-6662.
[53] SALERNO E, ORLANDI G, ONGARO C, et al. Liquid flow in scaffold derived from natural source: experimental observations and biological outcome. Regen Biomater. 2022;9:rbac034.
[54] HENSTOCK JR, ROTHERHAM M, ROSE JB, et al. Cyclic hydrostatic pressure stimulates enhanced bone development in the foetal chick femur in vitro. Bone. 2013;53(2):468-477.
[55] TAKAI E, MAUCK RL, HUNG CT, et al. Osteocyte viability and regulation of osteoblast function in a 3D trabecular bone explant under dynamic hydrostatic pressure. J Bone Miner Res. 2004;19(9):1403-1410.
[56] SINGH R, SINGH D, SINGH A. Radiation sterilization of tissue allografts: A review. World J Radiol. 2016;8(4):355-369.
[57] TOSOUNIDIS TH, GIANNOUDIS PV. Biological Facet of Segmental Bone Loss Reconstruction. J Orthop Trauma. 2017;31 Suppl 5:S27-S31.
[58] WALETZKO-HELLWIG J, POHL C, RIESE J, et al. Effect of High Hydrostatic Pressure on Human Trabecular Bone Regarding Cell Death and Matrix Integrity. Front Bioeng Biotechnol. 2021;9:730266.
[59] XU L, ZHANG X, LI G, et al. Inhibition of SIRT1 by miR-138-5p provides a mechanism for inhibiting osteoblast proliferation and promoting apoptosis under simulated microgravity. Life Sci Space Res (Amst). 2023;36:59-69.
[60] SUN Z, LI Y, WANG H, et al. miR-181c-5p mediates simulated microgravity-induced impaired osteoblast proliferation by promoting cell cycle arrested in the G2 phase. J Cell Mol Med. 2019;23(5):3302-3316.
[61] SUN Z, CAO X, HU Z, et al. MiR-103 inhibits osteoblast proliferation mainly through suppressing Cav1.2 expression in simulated microgravity. Bone. 2015;76:121-128.
[62] QIN W, LIU L, WANG Y, et al. Mir-494 inhibits osteoblast differentiation by regulating BMP signaling in simulated microgravity. Endocrine. 2019; 65(2):426-439.
[63] LIU J, LENG FF, GAO YH, et al. Protection of primary cilia is an effective countermeasure against the impairment of osteoblast function induced by simulated microgravity. J Cell Mol Med. 2023;27(1):36-51.
[64] ZENG Q, WANG Y, GAO J, et al. miR-29b-3p regulated osteoblast differentiation via regulating IGF-1 secretion of mechanically stimulated osteocytes. Cell Mol Biol Lett. 2019;24:11.
[65] 林维龙,吴晓沛,王晓明,等. miR-199a调控IGF1表达对机械刺激下成骨细胞分化的影响[J]. 上海口腔医学,2022,31(2):132-137.
[66] WANG X, GENG B, WANG H, et al. Fluid shear stress-induced down-regulation of microRNA-140-5p promotes osteoblast proliferation by targeting VEGFA via the ERK5 pathway. Connect Tissue Res. 2022;63(2): 156-168.
[67] SCHRÖDER M, RESELAND JE, HAUGEN HJ. Osteoblasts in a Perfusion Flow Bioreactor-Tissue Engineered Constructs of TiO2 Scaffolds and Cells for Improved Clinical Performance. Cells. 2022;11(13):1995.
[68] ATIF AR, PUJARI-PALMER M, TENJE M, et al. A microfluidics-based method for culturing osteoblasts on biomimetic hydroxyapatite. Acta Biomater. 2021;127:327-337.
[69] LUO X, ZHANG S, LUO B, et al. Engineering collagen fiber templates with oriented nanoarchitecture and concerns on osteoblast behaviors. Int J Biol Macromol. 2021;185:77-86
[70] AW YONG KM, HORST E, NEALE D, et al. A Bioreactor for 3D In Vitro Modeling of the Mechanical Stimulation of Osteocytes. Front Bioeng Biotechnol. 2022;10:797542. |
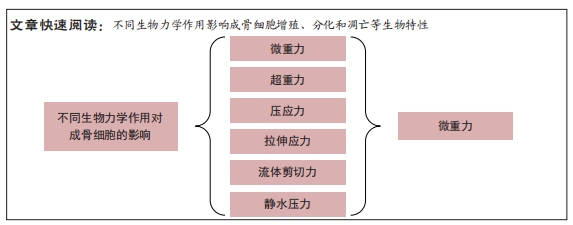
 3.2 作者综述区别于他人他篇的特点 相比其他文章,此文着重从不同生物力学作用入手,分别讨论其对成骨细胞的影响,包括力学信号对细胞形态、应力分布、基因表达等方面的影响。研究不同的生物力学作用对成骨细胞的影响,对于深入理解骨生长和维护机制具有重要意义,未来的研究可以从更深入的层面探究不同的生物力学作用对成骨细胞的影响,从而发现更多的机制和应用价值。
3.2 作者综述区别于他人他篇的特点 相比其他文章,此文着重从不同生物力学作用入手,分别讨论其对成骨细胞的影响,包括力学信号对细胞形态、应力分布、基因表达等方面的影响。研究不同的生物力学作用对成骨细胞的影响,对于深入理解骨生长和维护机制具有重要意义,未来的研究可以从更深入的层面探究不同的生物力学作用对成骨细胞的影响,从而发现更多的机制和应用价值。