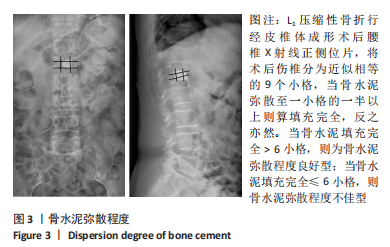
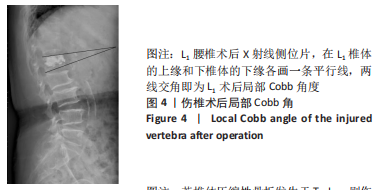
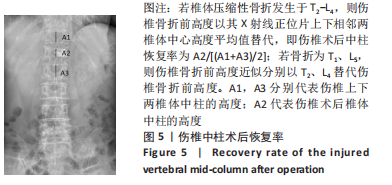
[1] BIAN FC, BIAN GY, AN YS, et al. Establishment and Validation of a Nomogram for the Risk of New Vertebral Compression Fractures After Percutaneous Vertebroplasty in Patients With Osteoporotic Vertebral Compression Fractures: A Retrospective Study. Geriatr Orthop Surg Rehabil. 2022;13:21514593221098620.
[2] ZHANG H, HU Y, CHEN X, et al. Expert consensus on the bone repair strategy for osteoporotic fractures in China. Front Endocrinol (Lausanne). 2022;13:989648.
[3] LIN S, CAI X, CHENG Q, et al. Association between bone turnover markers, BMD and height loss of cemented vertebrae after percutaneous vertebroplasty in patients with osteoporotic vertebral compression fractures. J Orthop Surg Res. 2022;17(1):1-9.
[4] Roux C, Cortet B, Bousson V, et al. Vertebroplasty for osteoporotic vertebral fracture. RMD Open. 2021;7(2):e001655.
[5] Liu Z, Zhang X, Liu H, et al. A nomogram for short-term recurrent pain after percutaneous vertebroplasty for osteoporotic vertebral compression fractures. Osteoporosis Int. 2022;33(4):851-860.
[6] Deibert CP, Gandhoke GS, Paschel EE, et al. A longitudinal cohort investigation of the development of symptomatic adjacent level compression fractures following balloon-assisted kyphoplasty in a series of 726 patients. Pain Phys. 2016;19:E1167-E1172.
[7] Zhang B, Li T, Wang Z. Efficacy and complications of different surgical modalities of treating osteoporotic spinal compression fracture in the elderly. Am J Trans Res. 2022;14(1): 364.
[8] Yang W, Yang J, Liang M. Percutaneous vertebroplasty does not increase the incidence of new fractures in adjacent and nonadjacent vertebral bodies. Clin Spine Surg. 2019;32(2):E99.
[9] Han SL, Wan SL, Li QT, et al. Is vertebroplasty a risk factor for subsequent vertebral fracture, meta-analysis of published evidence? Osteoporos Int. 2015;26:113-122.
[10] 管华清,郭炯炯,姜为民,等. 椎体强化术治疗脊柱骨质疏松性三明治骨折术后夹心椎再骨折的影响因素分析[J].中华创伤杂志, 2018,34(9):793-798.
[11] Mao W, Dong F, Huang G, et al. Risk factors for secondary fractures to percutaneous vertebroplasty for osteoporotic vertebral compression fractures: a systematic review. J Orthop Surg Res. 2021;16(1):1-10.
[12] Bian F, Bian GY, An YS, et al. Establishment and Validation of a Nomogram for the Risk of New Vertebral Compression Fractures After Percutaneous Vertebroplasty in Patients With Osteoporotic Vertebral Compression Fractures: A Retrospective Study. Geriatr Orthop Surg Rehabil. 2022;13:21514593221098620.
[13] Martikos K, Greggi T, Faldini C, et al. Osteoporotic thoracolumbar compression fractures: long-term retrospective comparison between vertebroplasty and conservative treatment. Eur Spine J. 2018;27(2): 244-247.
[14] Patel N, Jacobs D, John J, et al. Balloon Kyphoplasty vs Vertebroplasty: A Systematic Review of Height Restoration in Osteoporotic Vertebral Compression Fractures. J Pain Res. 2022;15: 1233.
[15] Joyce DM, Granville M, Berti A, et al. Vertebral Augmentation Compared to Conservative Treatment of Vertebra Plana and High-Degree Osteoporotic Vertebral Fractures: A Review of 110 Fractures in 100 Patients. Cureus, 2022;14(2):e22006.
[16] akahara K, Kamimura M, Moriya H, et al. Risk factors of adjacent vertebral collapse after percutaneous vertebroplasty for osteoporotic vertebral fracture in postmenopausal women. BMC Musculoskelet Disord. 2016;17:12.
[17] Tan WL, Low SL, Shen L, et al. Osteoporotic hip fractures: 10-year review in a Singaporean hospital. J Orthop Surg (Hong Kong). 2015;23: 150-154.
[18] Lin S, Cai X, Cheng Q, et al. Association between bone turnover markers, BMD and height loss of cemented vertebrae after percutaneous vertebroplasty in patients with osteoporotic vertebral compression fractures. J Orthop Surg Res. 2022;17(1):1-9.
[19] An Z, Chen C, Wang J, et al. Logistic regression analysis on risk factors of augmented vertebra recompression after percutaneous vertebral augmentation. J Orthop Surg Res. 2021;16(1):1-8.
[20] Hou Y, Yao Q, Zhang G, et al. Polymethylmethacrylate distribution is associated with recompression after vertebroplasty or kyphoplasty for osteoporotic vertebral compression fractures: A retrospective study. PloS One. 2018;13(6):e0198407.
[21] Yin H, He X, Yi H, et al. Analysis of the Causes on Poor Clinical Efficacy of Kyphoplasty Performed in Unilateral Transpedicular Puncture for the Treatment of Senile Osteoporotic Vertebral Compression Fractures. Sci Rep. 2019;9(1):1-9.
[22] Yang S, Liu Y, Yang H, et al. Risk factors and correlation of secondary adjacent vertebral compression fracture in percutaneous kyphoplasty. Int J Surg. 2016;36:138-142.
[23] 刘群,孙东东,高丽兰,等.经皮椎体后凸成形后再发骨折相关因素的Meta分析[J].中国组织工程研究,2020,24(6):976-984.
[24] Chang JZ, Bei MJ, Shu DP, et al. Comparison of the clinical outcomes of percutaneous vertebroplasty vs. kyphoplasty for the treatment of osteoporotic Kümmell’s disease: a prospective cohort study. BMC Musculoskelet Disord. 2020;21(1):1-8.
[25] Zhang L, Wang Q, Wang L, et al. Bone cement distribution in the vertebral body affects chances of recompression after percutaneous vertebroplasty treatment in elderly patients with osteoporotic vertebral compression fractures. Clin Int Aging. 2017;12:431.
[26] 陈荣彬,白杰,李勇,等. 骨水泥弥散类型影响胸腰段椎体成形后相邻椎体应力的三维有限元分析[J]. 中国组织工程研究,2020, 24(30):4775-4781.
[27] 沈松,徐彬. 经皮椎体成形骨水泥呈弥散型分布可减少邻近椎体再骨折的发生率[J]. 中国组织工程研究,2022,26(4):499-503.
[28] Chien HY, Yang YC, Hsieh MH, et al. Early Percutaneous Vertebroplasty Improves Bone-Cement Integration and Reduces Adjacent Fractures. World Neurosurg. 2021;156:e283-e290. |