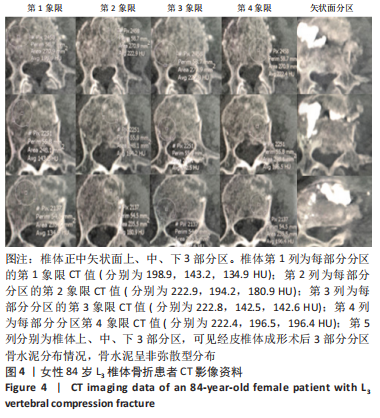
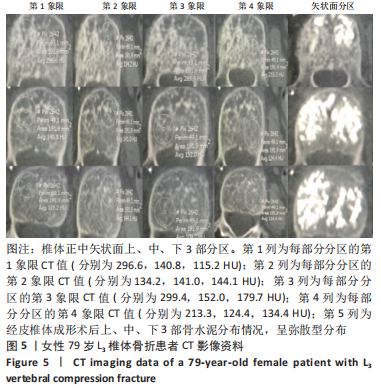
[1] YANG EZ, XU JG, HUANG GZ, et al. Percutaneous vertebroplasty versus conservative treatment in aged patients with acute osteoporotic vertebral compression fractures: a prospective randomized controlled clinical study. Spine (Phila Pa 1976). 2016;41(8):653-660.
[2] LAINEZ AJ, LOPEZ D, RUIZ F. Percutaneous vertebroplasty versus conservative treatment and placebo in osteoporotic vertebral fractures: meta-analysis and critical review of the literature. Eur Radiol. 2021;31(11):8542-8553.
[3] PROST S, PESENTI S, FUENTES S, et al. Treatment of osteoporotic vertebral fractures. Orthop Traumatol Surg Res. 2021;107(1S):102779.
[4] CHEN Z, CHEN Z, WU Y, et al. Risk factors of secondary vertebral compression fracture after percutaneous vertebroplasty or kyphoplasty: a retrospective study of 650 patients. Med Sci Monit. 2019;25:9255-9261.
[5] RHO YJ, CHOE WJ, CHUN YI. Risk factors predicting the new symptomatic vertebral compression fractures after percutaneous vertebroplasty or kyphoplasty. Eur Spine J. 2012;21(5):905-911.
[6] MO L, WU Z, LIANG D, et al. Influence of bone cement distribution on outcomes following percutaneous vertebroplasty: a retrospective matched-cohort study. J Int Med Res. 2021;49(7):3000605211022287.
[7] LV B, JI P, FAN X, et al. Clinical Efficacy of Different Bone Cement Distribution Patterns in Percutaneous Kyphoplasty: A Retrospective Study. Pain Physician. 2020;23(4):E409-E416.
[8] TAN L, WEN B, GUO Z, et al. The effect of bone cement distribution on the outcome of percutaneous Vertebroplasty: a case cohort study. BMC Musculoskelet Disord. 2020;21(1):541.
[9] CHEN JB, XIAO YP, CHEN D, et al. Clinical observation of two bone cement distribution modes of percutaneous vertebroplasty in the treatment of thoracolumbar Kummell’s disease. J Orthop Surg Res. 2020;15(1):250.
[10] PICKHARDT PJ, LEE LJ, DEL RA, et al. Simultaneous screening for osteoporosis at CT colonography: bone mineral density assessment using MDCT attenuation techniques compared with the DXA reference standard. J Bone Miner Res. 2011;26(9):2194-2203.
[11] PAPAIOANNOU A, MORIN S, CHEUNG AM, et al. 2010 clinical practice guidelines for the diagnosis and management of osteoporosis in Canada: summary. CMAJ. 2010;182(17):1864-1873.
[12] SCHREIBER JJ, ANDERSON PA, ROSAS HG, et al. Hounsfield units for assessing bone mineral density and strength: a tool for osteoporosis management. J Bone Joint Surg Am. 2011;93(11):1057-1063.
[13] MARINOVA M, EDON B, WOLTER K, et al. Use of routine thoracic and abdominal CT scans for assessing bone mineral density and detecting osteoporosis. Curr Med Res Opin. 2015;31(10):1871-1881.
[14] ZOU D, MUHEREMU A, SUN Z, et al. Computed tomography Hounsfield unit-based prediction of pedicle screw loosening after surgery for degenerative lumbar spine disease. J Neurosurg Spine. 2020:1-6.doi: 10.3171/2019.11.SPINE19868.
[15] 廖亦佳,舒启航,王程.胸腰椎骨折三维有限元模型构建的研究进展[J].中南医学科学杂志,2022,50(1):153-156.
[16] WONG CP, GANI LU, CHONG LR. Dual-energy X-ray absorptiometry bone densitometry and pitfalls in the assessment of osteoporosis: a primer for the practicing clinician. Arch Osteoporos. 2020;15(1):135.
[17] 王晨光,肖湘生,陈星荣,等.人腰椎体标本的区域骨密度分布特征[J].中华放射学杂志,1998,32(8):53-56.
[18] 刘云,李培岭,郭永杰,等.中老年骨质疏松症患者腰1-3椎体骨密度值与CT值相关性研究[J].风湿病与关节炎,2021,10(6):29-31.
[19] JOHANNESDOTTIR F, ALLAIRE B, KOPPERDAHL DL, et al. Bone density and strength from thoracic and lumbar CT scans both predict incident vertebral fractures independently of fracture location. Osteoporos Int. 2021;32(2): 261-269.
[20] ROSKI F, HAMMEL J, MEI K, et al. Opportunistic osteoporosis screening: contrast-enhanced dual-layer spectral CT provides accurate measurements of vertebral bone mineral density. Eur Radiol. 2021;31(5):3147-3155.
[21] ZHANG X, ZHU CX, HE JQ, et al. Correlation of CT Values and Bone Mineral Density in Elderly Chinese Patients with Proximal Humeral Fractures. Orthop Surg. 2021;13(8):2271-2279.
[22] 杨欣建,王正国,朱佩芳,等.胸腰段脊柱爆裂骨折瞬态损伤机制及节段稳定性研究[J].中华创伤杂志,1999,15(2):103-106.
[23] GERETY EL, BEARCROFT PW. L1 vertebral density on CT is too variable with different scanning protocols to be a useful screening tool for osteoporosis in everyday practice. Br J Radiol. 2018;91(1084):20170395.
[24] ABBOUCHIE H, RAJU N, LAMANNA A, et al. Screening for osteoporosis using L1 vertebral density on abdominal CT in an Australian population. Clin Radiol. 2022;77(7):e540-e548.
[25] ZOU D, YE K, TIAN Y, et al. Characteristics of vertebral CT Hounsfield units in elderly patients with acute vertebral fragility fractures. Eur Spine J. 2020; 29(5):1092-1097.
[26] DE NEGRI P, TIRRI T, PATERNOSTER G, et al. Treatment of painful osteoporotic or traumatic vertebral compression fractures by percutaneous vertebral augmentation procedures: a nonrandomized comparison between vertebroplasty and kyphoplasty. Clin J Pain. 2007;23(5):425-430.
[27] FILIPPIADIS DK, MARCIA S, MASALA S, et al. Percutaneous Vertebroplasty and Kyphoplasty: Current Status, New Developments and Old Controversies. Cardiovasc Intervent Radiol. 2017;40(12):1815-1823.
[28] WANG B, ZHAO CP, SONG LX, et al. Balloon kyphoplasty versus percutaneous vertebroplasty for osteoporotic vertebral compression fracture: a meta-analysis and systematic review. J Orthop Surg Res. 2018;13(1):264.
[29] ZHANG H, XU C, ZHANG T, et al. Does Percutaneous Vertebroplasty or Balloon Kyphoplasty for Osteoporotic Vertebral Compression Fractures Increase the Incidence of New Vertebral Fractures? A Meta-Analysis. Pain Physician. 2017;20(1):E13-E28.
[30] LI Y, FENG X, PAN J, et al. Percutaneous Vertebroplasty Versus Kyphoplasty for Thoracolumbar Osteoporotic Vertebral Compression Fractures in Patients with Distant Lumbosacral Pain. Pain Physician. 2021;24(3):E349-E356.
[31] ROUSING R, KIRKEGAARD AO, NIELSEN M, et al. Percutaneous vertebroplasty as treatment of malignant vertebral lesions: a systematic review and GRADE evaluation resulting in a Danish national clinical guideline. Eur Spine J. 2020; 29(7):1573-1579.
[32] KYRIAKOU C, MOLLOY S, VRIONIS F, et al. The role of cement augmentation with percutaneous vertebroplasty and balloon kyphoplasty for the treatment of vertebral compression fractures in multiple myeloma: a consensus statement from the International Myeloma Working Group (IMWG). Blood Cancer J. 2019;9(3):27.
[33] WANG H, SRIBASTAV SS, YE F, et al. Comparison of Percutaneous Vertebroplasty and Balloon Kyphoplasty for the Treatment of Single Level Vertebral Compression Fractures: A Meta-analysis of the Literature. Pain Physician. 2015;18(3):209-222.
[34] LI W, WANG J, LIU W, et al. Machine Learning Applications for the Prediction of Bone Cement Leakage in Percutaneous Vertebroplasty. Front Public Health. 2021;9:812023.
[35] XIE L, ZHAO ZG, ZHANG SJ, et al. Percutaneous vertebroplasty versus conservative treatment for osteoporotic vertebral compression fractures: An updated meta-analysis of prospective randomized controlled trials. Int J Surg. 2017;47:25-32.
[36] DAI SQ, QIN RQ, SHI X, et al. Percutaneous vertebroplasty versus kyphoplasty for the treatment of neurologically intact osteoporotic Kümmell’s disease. BMC Surg. 2021;21(1):65.
[37] STEVENSON M, GOMERSALL T, LLOYD JONES M, et al. Percutaneous vertebroplasty and percutaneous balloon kyphoplasty for the treatment of osteoporotic vertebral fractures: a systematic review and cost-effectiveness analysis. Health Technol Assess. 2014;18(17):1-290.
[38] ZUO XH, ZHU XP, BAO HG, et al. Network meta-analysis of percutaneous vertebroplasty, percutaneous kyphoplasty, nerve block, and conservative treatment for nonsurgery options of acute/subacute and chronic osteoporotic vertebral compression fractures (OVCFs) in short-term and long-term effects. Medicine (Baltimore). 2018;97(29):e11544.
[39] XIE LL, CHEN XD, YANG CY, et al. Efficacy and complications of 125I seeds combined with percutaneous vertebroplasty for metastatic spinal tumors: A literature review. Asian J Surg. 2020;43(1):29-35.
[40] SEMAAN H, OBRI T, BAZERBASHI M, et al. Clinical outcome and subsequent sequelae of cement extravasation after percutaneous kyphoplasty and vertebroplasty: a comparative review. Acta Radiol. 2018;59(7):861-868.
[41] WU XF, PING Y, ZENG XQ, et al. Percutaneous Vertebroplasty with Side-Opening Cannula or Front-Opening Cannula in the Treatment of Kummell Disease? Orthop Surg. 2020;12(4):1190-1198.
[42] GRIFFONI C, LUKASSEN JNM, BABBI L, et al. Percutaneous vertebroplasty and balloon kyphoplasty in the treatment of osteoporotic vertebral fractures: a prospective randomized comparison. Eur Spine J. 2020;29(7):1614-1620.
[43] 徐宝山,胡永成,闫广辉,等.经皮椎体成形术和后凸成形术的相关问题探讨[J].中华骨科杂志,2009,29(5):430-435.
[44] PARK J S, PARK YS. Survival analysis and risk factors of new vertebral fracture after vertebroplasty for osteoporotic vertebral compression fracture. Spine J. 2021;21(8):1355-1361.
[45] 周永春,肖培芬,罗婧,等.椎体骨密度与PVP骨水泥弥散体积的关系[J].中国骨与关节损伤杂志,2019,34(1):9-12.
[46] LEE BG, CHOI JH, KIM DY, et al. Risk factors for newly developed osteoporotic vertebral compression fractures following treatment for osteoporotic vertebral compression fractures. Spine J. 2019;19(2):301-305.
[47] SUN G, TANG H, LI M, et al. Analysis of risk factors of subsequent fractures after vertebroplasty. Eur Spine J. 2014;23(6):1339-1345.
[48] ZHANG T, WANG Y, ZHANG P, et al. What Are the Risk Factors for Adjacent Vertebral Fracture After Vertebral Augmentation? A Meta-Analysis of Published Studies. Global Spine J. 2022;12(1):130-141.
[49] YI X, LU H, TIAN F, et al. Recompression in new levels after percutaneous vertebroplasty and kyphoplasty compared with conservative treatment. Arch Orthop Trauma Surg. 2014;134(1):21-30.
[50] WANG M, WU Y, ZHOU Y, et al. Application of Dual-Energy Spectral Computed Tomography in Bone Mineral Density Measurement: Phantom and Clinical Research. Int J Gen Med. 2022;15(29):6887-6896.
[51] JANG S, GRAFFY PM, ZIEMLEWICZ TJ, et al. Opportunistic Osteoporosis Screening at Routine Abdominal and Thoracic CT: Normative L1 Trabecular Attenuation Values in More than 20 000 Adults. Radiology. 2019;291(2): 360-367. |