[1] American Diabetes Association. (2) Classification and diagnosis of diabetes. Diabetes Care. 2015;38 Suppl:S8-S16.
[2] WILLIAMS R, KARURAGA S, MALAND B, et al. Global and regional estimates and projections of diabetes-related health expenditure: Results from the International Diabetes Federation Diabetes Atlas, 9th edition. Diabetes Res Clin Pract. 2020;162:108072.
[3] EVERETT E, MATHIOUDAKIS N. Update on management of diabetic foot ulcers. Ann N Y Acad Sci. 2018;1411(1):153-165.
[4] RAGHURAM AC, YU RP, LO AY, et al. Role of stem cell therapies in treating Chronic wounds: A systematic review. World J Stem Cells. 2020;12(7):659-675.
[5] OBENDORF J, FABIAN C, THOME UH, et al. Paracrine stimulation of perinatal lung functional and structural maturation by mesenchymal stem cells. Stem Cell Res Ther. 2020;11(1):525.
[6] ZHAO L, HU C, ZHANG P, et al. Preconditioning strategies for improving the survival rate and paracrine ability of mesenchymal stem cells in acute kidney injury. J Cell Mol Med. 2019;23(2):720-730.
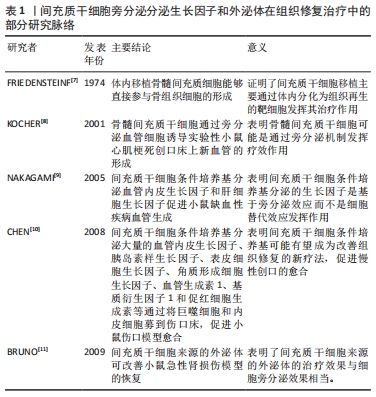
[7] FRIEDENSTEIN AJ, CHAILAKHYAN RK, LATSINIK NV, et al. Stromal cells responsible for transferring the microenvironment of the hemopoietic tissues. Cloning in vitro and retransplantation in vivo. Transplantation. 1974;17(4):331-340.
[8] KOCHER AA, SCHUSTER MD, SZABOLCS, et al. Neovascularization of ischemic myocardium by human bone-marrow-derived angioblasts prevents cardiomyocyte apoptosis, reduces remodeling and improves cardiac function. Nat Med. 2001;7(4):430-436.
[9] NAKAGAMI H, MADA K, MORISHITA R, et al. Novel autologous cell therapy in ischemic limb disease through growth factor secretion by cultured adipose tissue-derived stromal cells. Arterioscler Thromb Vasc Biol. 2005;25(12):2542-2547.
[10] CHEN L, TEDGET EE, WUPY, et al. Paracrine factors of mesenchymal stem cells recruit macrophages and endothelial lineage cells and enhance wound healing. PLoS One. 2008;3(4):e1886
[11] BRUNO S, GRANGE C, DEREGIBUS, et al. Mesenchymal stem cell-derived microvesicles protect against acute tubular injury. J Am Soc Nephrol. 2009;20(5):1053-1067.
[12] SHI Q, QIAN Z, LIU D, et al. GMSC-Derived Exosomes Combined with a Chitosan/Silk Hydrogel Sponge Accelerates Wound Healing in a Diabetic Rat Skin Defect Model. Front Physiol. 2017;8:904.
[13] ALTABS V. Diabetes, Endothelial Dysfunction, and Vascular Repair: What Should a Diabetologist Keep His Eye on? . Int J Endocrinol. 2015; 2015:848272.
[14] OKONKWO UA, CHEN L, MA D, et al. Compromised angiogenesis and vascular Integrity in impaired diabetic wound healing. PLoS One. 2020; 15(4):e0231962.
[15] GUO Y, LIN C, XU P, et al. AGEs Induced Autophagy Impairs Cutaneous Wound Healing via Stimulating Macrophage Polarization to M1 in Diabetes. Sci Rep. 2016;6:36416.
[16] AHWA R, GOYAL A, BANSAL P, et al. Chronic Inflammation//StatPearls. FL2021.
[17] LOBMANN R, LOUISELLE AE, NIEMIEC SM, et al. Macrophage polarization and diabetic wound healing. Transl Res. 2021;236:109-116.
[18] HOSSEINI MANSOUB N. The role of keratinocyte function on the defected diabetic wound healing. Int J Burns Trauma. 2021;11(6):430-441.
[19] JHAMB S, VANGAVETI VN, MALABU UH. Genetic and molecular basis of diabetic foot ulcers: Clinical review. Tissue Viability. 2016;25(4):229-236.
[20] PASTAR I, STOJADINPVIC O, YIN NC, et al. Epithelialization in Wound Healing: A Comprehensive Review. Adv Wound Care (New Rochelle). 2014;3(7):445-464.
[21] HSU EL, STOCK SR. Growth Factors, Carrier Materials, and Bone Repair. Handb Exp Pharmacol. 2020;262:121-156.
[22] PARK JW, HWANG SR, YOON IS. Advanced Growth Factor Delivery Systems in Wound Management and Skin Regeneration. Molecules. 2017;22(8):1259.
[23] ZUBAIR M, AHMAD J. Role of growth factors and cytokines in diabetic foot ulcer healing: A detailed review. Rev Endocr Metab Disord. 2019; 20(2):207-217.
[24] OKIZAKI S, LTO Y, HOSONO K, et al. Suppressed recruitment of alternatively activated macrophages reduces TGF-β1 and impairs wound healing in streptozotocin-induced diabetic mice. Biomed Pharmacother. 2015;70:317-325.
[25] PATEL S, SRIVATAVA S, SINGH MR, et al. Mechanistic insight into diabetic wounds: Pathogenesis, molecular targets and treatment strategies to pace wound healing. Biomed Pharmacother. 2019;112:108615.
[26] HU C, LI D, PANG Z, et al. Effect of vacuum sealing drainage on expressions of transforming growth factor β1 and its receptor in diabetic foot wound. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2018; 32(8):1061-1065.
[27] GILLGAN AM, WAYCASTER CR, MOTLEY TA. Cost-effectiveness of becaplermin gel on wound healing of diabetic foot ulcers. Wound Repair Regen. 2015;23(3):353-360.
[28] COHEN MA, EAGLSTEIN WH. Recombinant human platelet-derived growth factor gel speeds healing of acute full-thickness punch biopsy wounds. J Am Acad Dermatol. 2001;45(6):857-862.
[29] NEVINS M, CAMELO M, NEVINS ML, et al. Periodontal regeneration in humans using recombinant human platelet-derived growth factor-BB (rhPDGF-BB) and allogenic bone. J Periodontol. 2003;74(9):1282-1292.
[30] ZHANG J, GUAN M, XIE C, et al. Increased growth factors play a role in wound healing promoted by noninvasive oxygen-ozone therapy in diabetic patients with foot ulcers. Oxid Med Cell Longev. 2014; 2014:273475.
[31] OLIVEIRA BC, DE OLIVEIRA BC, DEUTSCH G, et al. Effectiveness of a synthetic human recombinant epidermal growth factor in diabetic patients wound healing: Pilot, double-blind, randomized clinical controlled trial. Wound Repair Regen. 2021;29(6):920-926.
[32] FALANGA V,EAGLSTEIN WH, BUCALO B, et al. Topical use of human recombinant epidermal growth factor (h-EGF) in venous ulcers. J Dermatol Surg Oncol. 1992;18(7):604-606.
[33] ZHANG JB, LI H, ZHANG L, et al. Observation of curative effect of recombinant human basic fibroblast growth factor combined with compound polymyxin B ointment and local application of insulin on wound healing of deep second-degree burn in diabetes mellitus: a randomized study. Eur Rev Med Pharmacol Sci. 2019;23(13): 5987-5993.
[34] MATSUMOTO S, TANAKA R, OKADA K, et al. The Effect of Control-released Basic Fibroblast Growth Factor in Wound Healing: Histological Analyses and Clinical Application. Plast Reconstr Surg Glob Open. 2013; 1(6):e44.
[35] ROBSON MC, PHILLIPS TJ, FALANGA V, et al. Randomized trial of topically applied repifermin (recombinant human keratinocyte growth factor-2) to accelerate wound healing in venous ulcers. Wound Repair Regen. 2001;9(5):347-352.
[36] LEE CH, LIU KS, CHENG CW, et al. Codelivery of Sustainable Antimicrobial Agents and Platelet-Derived Growth Factor via Biodegradable Nanofibers for Repair of Diabetic Infectious Wounds. ACS Infect Dis. 2020;6(10):2688-2697.
[37] AN Y, LIU WJ, XUE P, et al. Autophagy promotes MSC-mediated vascularization in cutaneous wound healing via regulation of VEGF secretion. Cell Death Dis. 2018;9(2):58.
[38] OKIZAKI S, LTO Y, HOSONO K, et al. Vascular Endothelial Growth Factor Receptor Type 1 Signaling Prevents Delayed Wound Healing in Diabetes by Attenuating the Production of IL-1β by Recruited Macrophages. Am J Pathol. 2016;186(6):1481-1498.
[39] KULWAS A, DRELA E, JUNDZILL, et al. Circulating endothelial progenitor cells and angiogenic factors in diabetes complicated diabetic foot and without foot complications. Diabetes Complications. 2015;29(5):686-690.
[40] GANGADARAM P, RAJENDRAN RL,LEE HW, et al. Extracellular vesicles from mesenchymal stem cells activates VEGF receptors and accelerates recovery of hindlimb ischemia. Control Release. 2017;264:112-126.
[41] LONG H, LIU D, HE X, et al. A dual functional collagen scaffold coordinates angiogenesis and inflammation for diabetic wound healing. Biomater Sci. 2020;8(22):6337-6349.
[42] WHITE MJV, BRIQUEZ PS, WHITE DA, et al.VEGF-A, PDGF-BB and HB-EGF engineered for promiscuous super affinity to the extracellular matrix improve wound healing in a model of type 1 diabetes. NPJ Regen Med. 2021;6(1):76.
[43] HEENDRAWAN S, KUSNADI Y, LAGONDA CA, et al. Wound healing potential of human umbilical cord mesenchymal stem cell conditioned medium: An in vitro and in vivo study in diabetes-induced rats. Vet World. 2021;14(8):2109-2117.
[44] EI-HATTAB MY, NAGUMO Y, GOURRONC FA, et al. Human Adipocyte Conditioned Medium Promotes In Vitro Fibroblast Conversion to Myofibroblasts. Sci Rep. 2020;10(1):10286.
[45] XIN Y, XU P, WANG X, et al.Human foreskin-derived dermal stem/progenitor cell-conditioned medium combined with hyaluronic acid promotes extracellular matrix regeneration in diabetic wounds. Stem Cell Res Ther. 2021;12(1):49.
[46] LPK, KANDOI, MISRA R, et al. The mesenchymal stem cell secretome: A new paradigm towards cell-free therapeutic mode in regenerative medicine. Cytokine Growth Factor Rev. 2019;46:1-9.
[47] FUI LW, LOK MPW, GOVINDASAMY V, et al. Understanding the multifaceted mechanisms of diabetic wound healing and therapeutic application of stem cells conditioned medium in the healing process. J Tissue Eng Regen Med. 2019;13(12):2218-2233.
[48] GUNAWARDENA TNA, RAHMAN MT, ABDULLAH BJJ, et al. Conditioned media derived from mesenchymal stem cell cultures: The next generation for regenerative medicine. J Tissue Eng Regen Med. 2019;13(4):569-586.
[49] HUANG SM, WU CS, CHIU MH, et al. High-glucose environment induced intracellular O-GlcNAc glycosylation and reduced galectin-7 expression in keratinocytes: Implications on impaired diabetic wound healing. J Dermatol Sci. 2017;87(2):168-175.
[50] HU SC, LAN CE. High-glucose environment disturbs the physiologic functions of keratinocytes: Focusing on diabetic wound healing. J Dermatol Sci. 2016;84(2):121-127.
[51] SAHELI M, BAYAT M, GANJI R, et al. Human mesenchymal stem cells-conditioned medium improves diabetic wound healing mainly through modulating fibroblast behaviors. Arch Dermatol Res. 2020;312(5):325-336.
[52] LUO H, WANG Y, SU Y, et al. Paracrine effects of adipose-derived stem cells in cutaneous wound healing in streptozotocin-induced diabetic rats. J Wound Care. 2022;31:S29-S38.
[53] JOSEPH A, BAIJU I,BHAT IA, et al. Mesenchymal stem cell-conditioned media: A novel alternative of stem cell therapy for quality wound healing. Cell Physiol. 2020;235(7-8):5555-5569.
[54] TAKAHASHI H, OHNISHI S,YAMAOTO Y, et al. Topical Application of Conditioned Medium from Hypoxically Cultured Amnion-Derived Mesenchymal Stem Cells Promotes Wound Healing in Diabetic Mice. Plast Reconstr Surg. 2021;147(6):1342-1352.
[55] VEITH AP, HENDER SON K, SPENCER A, et al.Therapeutic strategies for enhancing angiogenesis in wound healing. Adv Drug Deliv Rev. 2019;146:97-125.
[56] ZHANG S, CHENL, ZHANG G, et al. Umbilical cord-matrix stem cells induce the functional restoration of vascular endothelial cells and enhance skin wound healing in diabetic mice via the polarized macrophages. Stem Cell Res Ther. 2020;11(1):39.
[57] YAMAGUCHI J, KUSANO KF, MASUO O, et al. Stromal cell-derived factor-1 effects on ex vivo expanded endothelial progenitor cell recruitment for ischemic neovascularization. Circulation. 2003;107(9): 1322-1328.
[58] GALLAGHER KA, LIU ZJ, XIAO M, et al. Diabetic impairments in NO-mediated endothelial progenitor cell mobilization and homing are reversed by hyperoxia and SDF-1 alpha. Clin Invest. 2007;117(5):1249-1259.
[59] FRIDONI M, KOUHKHEIL R, ABDLLHIFAR MA, et al. Improvement in infected wound healing in type 1 diabetic rat by the synergistic effect of photobiomodulation therapy and conditioned medium. Cell Biochem. 2019;120(6):9906-9916.
[60] HU CH, TSENG YW,CHIOU CY, et al. Bone marrow concentrate-induced mesenchymal stem cell conditioned medium facilitates wound healing and prevents hypertrophic scar formation in a rabbit ear model. Stem Cell Res Ther. 2019;10(1):275.
[61] KOUREMBANAS S. Exosomes: vehicles of intercellular signaling, biomarkers, and vectors of cell therapy . Annu Rev Physiol. 2015;77: 13-27.
[62] CORRADO C, RAIMONO S, CHIESI A, et al. Exosomes as intercellular signaling organelles involved in health and disease: basic science and clinical applications. Int J Mol Sci. 2013;14(3):5338-5366.
[63] HYLDIG K, RIIS S, PENNISI CP, et al. Implications of Extracellular Matrix Production by Adipose Tissue-Derived Stem Cells for Development of Wound Healing Therapies. Int J Mol Sci. 2017;18(6):1167.
[64] HAN G, CEILLEY R. Chronic Wound Healing: A Review of Current Management and Treatments. Adv Ther. 2017;34(3):599-610.
[65] THAN UTT, GUANZON D, LEAVESLEYD, et al. Association of Extracellular Membrane Vesicles with Cutaneous Wound Healing. Int J Mol Sci. 2017;18(5):956.
[66] SCHWAB A, MEYERING SS, LEPENE B, et al. Extracellular vesicles from infected cells: potential for direct pathogenesis. Front Microbiol. 2015; 6:1132.
[67] HUANG C, LUO W, WANG Q, et al. Human mesenchymal stem cells promote ischemic repairment and angiogenesis of diabetic foot through exosome miRNA-21-5p. Stem Cell Res. 2021;52:102235.
[68] LI X, LIU L, YANG J, et al. Exosome Derived From Human Umbilical Cord Mesenchymal Stem Cell Mediates MiR-181c Attenuating Burn-induced Excessive Inflammation. EBio Medicine. 2016;8:72-82.
[69] YU M, LIU W, LI J, et al. Exosomes derived from atorvastatin-pretreated MSC accelerate diabetic wound repair by enhancing angiogenesis via AKT/eNOS pathway. Stem Cell Res Ther. 2020;11(1):350.
[70] LI X, XIE X, LIAN W, et al. Exosomes from adipose-derived stem cells overexpressing Nrf2 accelerate cutaneous wound healing by promoting vascularization in a diabetic foot ulcer rat model. Exp Mol Med. 2018; 50(4):1-14.
[71] ZHAO B, ZHANG X,ZHANG Y, et al. Human Exosomes Accelerate Cutaneous Wound Healing by Promoting Collagen Synthesis in a Diabetic Mouse Model. Stem Cells Dev. 2021;30(18):922-933.
[72] YAN C, XV Y , LIN Z, et al. Human Umbilical Cord Mesenchymal Stem Cell-Derived Exosomes Accelerate Diabetic Wound Healing via Ameliorating Oxidative Stress and Promoting Angiogenesis. Front Bioeng Biotechnol. 2022;10:829868.
[73] SHEN YI, CHO H, PAPA AE,et al. Engineered human vascularized constructs accelerate diabetic wound healing. Biomaterials. 2016;102: 107-119.
[74] WANG C, WANG M, XU T, et al. Engineering Bioactive Self-Healing Antibacterial Exosomes Hydrogel for Promoting Chronic Diabetic Wound Healing and Complete Skin Regeneration. Theranostics. 2019; 9(1):65-76.
[75] YANG J,CHEN Z,PAN D, et alUmbilical Cord-Derived Mesenchymal Stem Cell-Derived Exosomes Combined Pluronic F127 Hydrogel Promote Chronic Diabetic Wound Healing and Complete Skin Regeneration. Int J Nanomedicine. 2020;15:5911-5926.
|