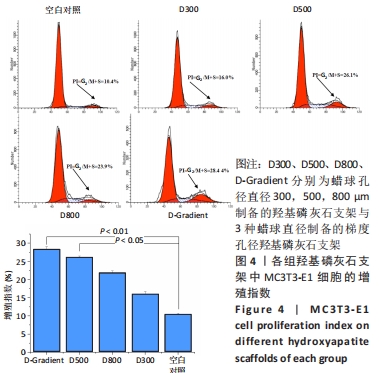
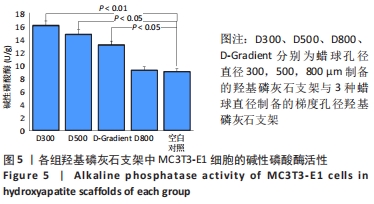
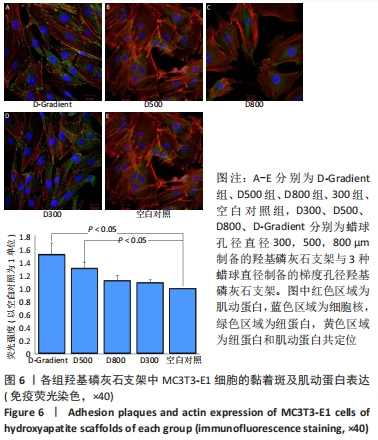
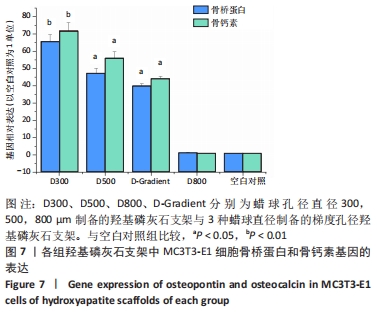
[1] LEE JW, AHN G, KIM JY, et al. Evaluating cell proliferation based on internal pore size and 3D scaffold architecture fabricated using solid freeform fabrication technology. J Mater Sci Mater Med. 2010;21(12): 3195-3205.
[2] AMINI AR, NUKAVARAPU SP. Oxygen-tension controlled matrices for enhanced osteogenic cell survival and performance. Ann Biomed Eng. 2014;42(6):1261-1270.
[3] PEREZ RA, MESTRES G. Role of pore size and morphology in musculo-skeletal tissue regeneration. Mater Sci Eng C Mater Biol Appl. 2016;61: 922-939.
[4] BAINO F, FIORILLI S, VITALE-BROVARONE C. Bioactive glass-based materials with hierarchical porosity for medical applications: Review of recent advances. Acta Biomater. 2016;42:18-32.
[5] ZHANG Q, LU H, KAWAZOE N, et al. Preparation of collagen porous scaffolds with a gradient pore size structure using ice particulates. Mater Lett. 2013;107:280-283.
[6] SHI D, SHEN J, ZHANG Z, et al. Preparation and properties of dopamine-modified alginate/chitosan-hydroxyapatite scaffolds with gradient structure for bone tissue engineering. J Biomed Mater Res A. 2019; 107(8):1615-1627.
[7] MA H, XUE L, NIE T. Fabrication of PLLA scaffold with gradient macro/micro/nano structure by electrophoretic deposition of carbon nanotube. Mater Lett. 2015;159:185-188.
[8] WILLIAMS JM, ADEWUNMI A, SCHEK RM, et al. Bone tissue engineering using polycaprolactone scaffolds fabricated via selective laser sintering. Biomaterials. 2005;26(23):4817-4827.
[9] DI LUCA A, OSTROWSKA B, LORENZO-MOLDERO I, et al. Gradients in pore size enhance the osteogenic differentiation of human mesenchymal stromal cells in three-dimensional scaffolds. Sci Rep. 2016;6:22898.
[10] LEE SJ, LEE IW, LEE YM, et al. Macroporous biodegradable natural/synthetic hybrid scaffolds as small intestine submucosa impregnated poly(D,L-lactide-co-glycolide) for tissue-engineered bone. J Biomater Sci Polym Ed. 2004;15(8):1003-1017.
[11] SOBRAL JM, CARIDADE SG, SOUSA RA, et al. Three-dimensional plotted scaffolds with controlled pore size gradients: Effect of scaffold geometry on mechanical performance and cell seeding efficiency. Acta Biomater. 2011;7(3):1009-1018.
[12] LIU B, CUI L, LIU GP, et al. [Tissue-engineering bone with ADSCs and coral scaffold for repairing of cranial bone defect in canine]. Zhonghua Zheng Xing Wai Ke Za Zhi. 2009;25(3):204-208.
[13] FU R, LIU C, YAN Y, et al. Bone defect reconstruction via endochondral ossification: A developmental engineering strategy. J Tissue Eng. 2021; 12:20417314211004211.
[14] GAO C, SOW WT, WANG Y, et al. Hydrogel composite scaffolds with an attenuated immunogenicity component for bone tissue engineering applications. J Mater Chem B. 2021;9(8):2033-2041.
[15] WANG C, YUE H, HUANG W, et al. Cryogenic 3D printing of heterogeneous scaffolds with gradient mechanical strengths and spatial delivery of osteogenic peptide/TGF-β1 for osteochondral tissue regeneration. Biofabrication. 2020;12(2):025030.
[16] SU X, WANG T, GUO S. Applications of 3D printed bone tissue engineering scaffolds in the stem cell field. Regen Ther. 2021;16:63-72.
[17] CHANG BS, LEE CK, HONG KS, et al. Osteoconduction at porous hydroxyapatite with various pore configurations. Biomaterials. 2000; 21(12):1291-1298.
[18] BOBYN JD, PILLIAR RM, CAMERON HU, et al. The optimum pore size for the fixation of porous-surfaced metal implants by the ingrowth of bone.Clin Orthop Relat Res. 1980;(150):263-270.
[19] BAI F, WANG Z, LU J, et al. The correlation between the internal structure and vascularization of controllable porous bioceramic materials in vivo: a quantitative study. Tissue Eng Part A. 2010;16(12): 3791-3803.
[20] XIAO X, WANG W, LIU D, et al. The promotion of angiogenesis induced by three-dimensional porous beta-tricalcium phosphate scaffold with different interconnection sizes via activation of PI3K/Akt pathways. Sci Rep. 2015;5:9409.
[21] ITÄLÄ AI, YLÄNEN HO, EKHOLM C, et al. Pore diameter of more than 100 microm is not requisite for bone ingrowth in rabbits. J Biomed Mater Res. 2001;58(6):679-683.
[22] KUBOKI Y, JIN Q, TAKITA H. Geometry of carriers controlling phenotypic expression in BMP-induced osteogenesis and chondrogenesis. J Bone Joint Surg Am. 2001;83-A Suppl 1(Pt 2):S105-115.
[23] 郑威,董学明,何阳,等.生物活性聚合物及其复合材料在骨组织工程中的应用进展[J].哈尔滨工业大学学报,2021,53(8):1-16.
[24] YEUNG M, ABDULMAJEED A, CARRICO CK, et al. Accuracy and precision of 3D-printed implant surgical guides with different implant systems: An in vitro study. J Prosthet Dent. 2020;123(6):821-828.
[25] GOH YQ, OOI CP. Fabrication and characterization of porous poly(L-lactide) scaffolds using solid-liquid phase separation. J Mater Sci Mater Med. 2008;19(6):2445-2452.
[26] 廖欣宇,王福科,王国梁.骨组织工程支架的进展与挑战[J].中国组织工程研究,2021,25(28):4553-4560.
[27] 王启帆,马志勇,钟林娜,等.PCL/ZrO2骨组织工程支架3D打印制备方法及其性能研究[J].北京生物医学工程,2020,39(4):418-424.
[28] LO DICO G, NUÑEZ ÁP, CARCELÉN V, et al. Machine-learning-accelerated multimodal characterization and multiobjective design optimization of natural porous materials. Chem Sci. 2021;12(27):9309-9317.
[29] WU Z, LUO J, ZHANG J, et al. Silver-Releasing Micro-/Nanoporous Coating on Additively Manufactured Macroporous Ti-Ta-Nb-Zr Scaffolds with High Osseointegration and Antibacterial Properties. Coatings. 2021;11(6):716.
[30] CABALLERO-FLORES H, NABESHIMA CK, SARRA G, et al. Development and characterization of a new chitosan-based scaffold associated with gelatin, microparticulate dentin and genipin for endodontic regeneration. Dent Mater. 2021;37(7):e414-e425.
[31] XUE G, ZHANG Y, XIE T, et al. Cell Adhesion-Mediated Piezoelectric Self-Stimulation on Polydopamine-Modified Poly(vinylidene fluoride) Membranes. ACS Appl Mater Interfaces. 2021;13(15):17361-17371.
[32] BLAINE J, DYLEWSKI J. Regulation of the Actin Cytoskeleton in Podocytes. Cells. 2020;9(7):1700.
[33] SUN Y, LIU X, TAN J, et al. Strontium ranelate incorporated 3D porous sulfonated PEEK simulating MC3T3-E1 cell differentiation. Regen Biomater. 2020;8(1):rbaa043.
[34] WANG X, CHEN T, DENG Z, et al. Melatonin promotes bone marrow mesenchymal stem cell osteogenic differentiation and prevents osteoporosis development through modulating circ_0003865 that sponges miR-3653-3p. Stem Cell Res Ther. 2021;12(1):150.
[35] LI Q, LU F, CHEN T, et al. VPS4B mutation impairs the osteogenic differentiation of dental follicle cells derived from a patient with dentin dysplasia type I. Int J Oral Sci. 2020;12(1):22.
[36] CHEN Y, HU Y, YANG L, et al. Effects of Different Concentrations of Glucose on the Osteogenic Differentiation of Orofacial Bone Mesenchymal Stem Cells. Sichuan Da Xue Xue Bao Yi Xue Ban. 2016; 47(5):679-684.
[37] JAFARY F, HANACHI P, GORJIPOUR K. Osteoblast Differentiation on Collagen Scaffold with Immobilized Alkaline Phosphatasec Int J Organ Transplant Med. 2017;8(4):195-202.
[38] VARMA SR, SHARATH KUMAR LM, VIDYASHANKAR S, et al. Water Soluble Components of ‘Osteocare’ Promote Cell Proliferation, Differentiation, and Matrix Mineralization in Human Osteoblast-Like SaOS-2 Cells. Sci Pharm. 2014;82(2):375-391.
[39] HUH JE, YANG HR, PARK DS, et al. Puerariae radix promotes differentiation and mineralization in human osteoblast-like SaOS-2 cells. J Ethnopharmacol. 2006;104(3):345-350.
[40] CHIEN HH, LIN WL, CHO MI. Expression of TGF-beta isoforms and their receptors during mineralized nodule formation by rat periodontal ligament cells in vitro. J Periodontal Res. 1999;34(6):301-309.
[41] YE G, LI C, XIANG X, et al. Bone morphogenetic protein-9 induces PDLSCs osteogenic differentiation through the ERK and p38 signal pathways. Int J Med Sci. 2014;11(10):1065-1072.
|