中国组织工程研究 ›› 2022, Vol. 26 ›› Issue (4): 597-603.doi: 10.12307/2022.098
• 生物材料综述 biomaterial review • 上一篇 下一篇
生物支架材料促进骨髓间充质干细胞成骨分化的研究热点
康坤龙,王新涛
- 哈尔滨医科大学附属第二医院骨科,黑龙江省哈尔滨市 150001
-
收稿日期:2020-09-24修回日期:2020-09-28接受日期:2020-11-09出版日期:2022-02-08发布日期:2021-12-06 -
通讯作者:王新涛,主任医师,教授,博士生导师,硕士生导师,哈尔滨医科大学附属第二医院骨科,黑龙江省哈尔滨市 150001 -
作者简介:康坤龙,男,1994年生,陕西省渭南市人,汉族,哈尔滨医科大学在读硕士,主要从事骨组织工程研究。 -
基金资助:国家自然科学基金(81772362),项目负责人:王新涛
Research hotspot of biological scaffold materials promoting osteogenic differentiation of bone marrow mesenchymal stem cells
Kang Kunlong, Wang Xintao
- Department of Orthopedics, The 2nd Affiliated Hospital of Harbin Medical University, Harbin 150001, Heilongjiang Province, China
-
Received:2020-09-24Revised:2020-09-28Accepted:2020-11-09Online:2022-02-08Published:2021-12-06 -
Contact:Wang Xintao, Chief physician, Professor, Doctoral supervisor, Master’s supervisor, Department of Orthopedics, The 2nd Affiliated Hospital of Harbin Medical University, Harbin 150001, Heilongjiang Province, China -
About author:Kang Kunlong, Master candidate, Department of Orthopedics, The 2nd Affiliated Hospital of Harbin Medical University, Harbin 150001, Heilongjiang Province, China -
Supported by:the National Natural Science Foundation of China, No. 81772362 (to WXT)
摘要:
文题释义:
生物支架材料:目前单一支架材料难以满足骨组织工程的成骨需要,生物支架材料研究将集中于通过不同的制造技术将生物支架材料进行复合,并添加生长因子及具有趋化作用的多肽,将骨组织工程3要素集成一体,制成具有最优良的成骨作用的生物支架。
骨髓间充质干细胞:是一种中胚层来源的多能干细胞,具有易获取、易培养、低免疫原性和易于外源基因转染并长期表达等特点,并具有优良的成骨分化能力,是目前骨组织工程应用最广泛的干细胞。
背景:目前单一生物支架材料难以满足骨组织工程的成骨需要,骨髓间充质干细胞具有优良的成骨特点,复合支架材料及复合生长因子的支架具有更优良的成骨能力,是目前研究的热点。
目的:对不同生物支架材料及其改型后促进骨髓间充质干细胞成骨分化进行综述。
方法:由第一作者通过检索中国知网、万方、维普、PubMed、Embase数据库 2014年1月至2020年7月发表的相关文献,检索词为“骨髓间充质干细胞,支架,成骨分化,羟基磷灰石,胶原,壳聚糖;Bone marrow mesenchymal stem cells,scaffold,osteogenic,hydroxyapatite,collagen,chitosan”,最终选取符合标准的文献69篇。
结果与结论:骨组织工程的飞速发展可有效解决骨缺损修复的难题,种子细胞和生物支架材料是骨组织工程的核心内容。骨髓间充质干细胞具有优良的成骨分化能力,被广泛应用于骨组织工程。将不同的支架材料复合,利用先进的制备工艺或者进行支架的表面修饰、添加生长因子等可充分结合各种生物支架材料的优点,诱导骨髓间充质干细胞的成骨分化和支架血管的形成,达到修复骨缺损的目的,是骨组织工程的研究热点。
https://orcid.org/0000-0002-6598-9660 (康坤龙)
中国组织工程研究杂志出版内容重点:生物材料;骨生物材料; 口腔生物材料; 纳米材料; 缓释材料; 材料相容性;组织工程
中图分类号:
引用本文
康坤龙, 王新涛. 生物支架材料促进骨髓间充质干细胞成骨分化的研究热点[J]. 中国组织工程研究, 2022, 26(4): 597-603.
Kang Kunlong, Wang Xintao. Research hotspot of biological scaffold materials promoting osteogenic differentiation of bone marrow mesenchymal stem cells[J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 597-603.
2.1.1 羟基磷灰石 羟基磷灰石是最常见的生物活性材料,硬度大,骨传导性强,承重能力强,具有良好的生物相容性、生物活性和骨传导性,与天然骨中的无机盐成分非常接近,是骨缺损修复及相关替代材料的主要研究方向。
从仿生学的角度出发,充分模拟松质骨的层次结构,引入仿生纳米羟基磷灰石颗粒可以显著提高材料的生物学性能。与纯羟基磷灰石相比,纳米复合材料在骨修复的模量、强度和刚度等性能上都有所改善,增强了细胞与材料的相互作用和羟基磷灰石的生物活性,对蛋白质黏附、细胞黏附、增殖和骨整合有积极作用[7-8]。WANG等[9]实验结果表明相较于单纯的磷酸三钙支架,纳米羟基磷灰石涂层的磷酸三钙可显著促进碱性磷酸酶、Ⅰ型胶原蛋白、骨钙素等成骨因子的表达,同时进一步促进BMP/Smad成骨信号通路中的特异性生物因子表达,证明纳米羟基磷灰石涂层的磷酸三钙能促进骨髓间充质干细胞的成骨分化,并且其成骨分化能力与BMP/Smad信号通路有关。
纯羟基磷灰石支架在骨组织工程中的应用受到其硬度、脆性和柔韧性的限制,并且羟基磷灰石粉末容易从植入部位迁移,导致不适当的骨化。相比于单纯的无机材料羟基磷灰石,由天然或合成聚合物制成的基于纳米羟基磷灰石的复合支架可弥补无机材料硬度、脆性等缺点。与纳米羟基磷灰石-壳聚糖纳米复合材料共培养的骨髓间充质干细胞有更好的细胞形态和增殖能力,并且Smad1、骨形态发生蛋白2、骨形态发生蛋白4、Runx2、碱性磷酸酶、骨钙素等成骨相关基因显著上调,整合素亚基和肌球蛋白的mRNA水平显著上调,整合素可介导细胞黏附,结果表明纳米羟基磷灰石-壳聚糖纳米复合材料支架支持骨髓间充质干细胞的黏附、扩散、增殖,并诱导了骨髓间充质干细胞整合素、骨形态发生蛋白信号通路的激活和随后的成骨分化[10]。采用超低温凝胶法制备的冷冻明胶/纳米羟基磷灰石复合支架,在提升弹性模量、稳定性及孔隙率的同时,进一步促进了骨髓间充质干细胞的细胞反应。与冷冻明胶/纳米羟基磷灰石支架共培养的骨髓间充质干细胞呈现良好的增殖,在培养期间也表现出较高的碱性磷酸酶活性、矿化的结节生成、骨钙素及成骨相关基因的表达,证实了冷冻明胶/纳米羟基磷灰石支架可更快地将骨髓间充质干细胞分化为成骨细胞,并且在骨髓间充质干细胞成骨中具有协同作用[11]。CHUENJITKUNTAWORN等[12]在聚已内酯支架中添加羟基磷灰石以改善其生物活性和力学性能,并减少某些合成聚合物(如聚L-丙交酸、聚乳酸、聚甲基丙烯酸甲酯等)降解带来的不利影响,采用MTT细胞活性测定、反转录聚合酶链反应、碱性磷酸酶活性测定和茜素红染色检测成骨分化情况,聚已内酯/羟基磷灰石支架增加骨髓间充质干细胞的成骨分化相关基因Runx2、Ⅰ型胶原蛋白、骨钙素的表达与碱性磷酸酶活性,以及体外钙化。
传统支架在制作过程中很难完全符合骨缺损形状和获得均匀一致的孔径及孔隙率,三维打印技术可以优化传统的骨替代材料,控制支架的孔隙率和孔径连通性,使支架易于加工成不同的物理结构[13]。利用3D打印技术制作三维打印聚乳酸/羟基磷灰石支架,羟基磷灰石作为增强材料改善聚合物的机械性能,提高支架的生物活性和骨传导性。ZHANG等[14]观察了骨髓间充质干细胞在不同支架上的黏附、增殖、碱性磷酸酶活性和成骨基因表达情况,3D打印聚乳酸/羟基磷灰石支架可促进骨髓间充质干细胞的增殖、碱性磷酸酶活性和成骨相关基因的表达;3D打印聚乳酸/羟基磷灰石支架具有良好的生物相容性,可促进骨髓间充质干细胞增殖和成骨细胞分化。
羟基磷灰石的成骨能力较弱,影响骨缺损的修复能力[15],通过加入中药中具有成骨能力的成分可显著提高羟基磷灰石的成骨能力。墨旱莲属植物的主要成分蟛蜞菊内酯能够促进骨髓间充质干细胞的骨钙素和Runx2的表达,促进骨髓间充质干细胞的成骨分化[16-17]。将蟛蜞菊内酯与羟基磷灰石联合应用可以弥补羟基磷灰石在成骨能力较弱的缺陷,与骨髓间充质干细胞共培养后,联合使用蟛蜞菊内酯和羟基磷灰石可以更显著地增加骨矿化及碱性磷酸酶活性,显著增加Runx2、骨钙素mRNA的表达,表明羟基磷灰石联合蟛蜞菊内酯对成骨细胞分化、矿化和成骨细胞形成相关标志物基因表达均有增强作用[18]。王德欣等[19]将羟基磷灰石与聚乳酸-羟基乙酸共聚物共混的方式制备了羟基磷灰 石/聚乳酸-羟基乙酸共聚物支架,并加入不同浓度的淫羊藿苷形成淫羊藿苷/羟基磷灰石/聚乳酸-羟基乙酸共聚物复合支架,该方法制备的支架具有双尺寸微孔结构,当淫羊藿苷溶液浓度为 1.00 μmol/L时,淫羊藿苷/羟基磷灰石/聚乳酸-羟基乙酸共聚物支架上骨髓间充质干细胞的碱性磷酸酶和骨钙素活性最高,对细胞的成骨诱导作用最明显,并且Runx2和Ⅰ型胶原蛋白在mRNA和蛋白水平上均表达最高,结果表明,淫羊藿苷/羟基磷灰石/聚乳酸-羟基乙酸共聚物复合支架具有良好的力学性能,且可以促进骨髓间充质干细胞增殖和成骨分化。
2.1.2 磷酸三钙 磷酸三钙按结构分为α-磷酸三钙和β-磷酸三钙,是一种可降解的生物支架,具有良好的生物相容性、生物活性和骨引导作用,在骨缺损修复中应用广泛[6]。磷酸三钙可通过释放钙磷离子促进组织矿化,显著增强钙结节生成和新骨的形成,是骨组织工程的潜力支架材料。
β-磷酸三钙因其降解速度过快、可塑性较差、机械性能不稳定而常与其他物质复合应用。三维互连的多孔β-磷酸三钙/Ⅰ型胶原蛋白支架,具有高孔隙率和大孔径,具有良好的生物降解性和生物相容性,为骨髓间充质干细胞生长提供物理框架,同时具有生物活性调节作用,提高成骨生物标志物的表达,从而刺激骨髓间充质干细胞的成骨分化[20]。LIN等[21]利用细胞片技术将骨髓间充质干细胞渗入β-磷酸三钙/Ⅰ型胶原蛋白支架,并通过层状结构相互连接,细胞片技术的应用不仅可以显著提高骨髓间充质干细胞的利用率和生物活性,还能提供丰富的细胞外基质,传递调控骨形成的生物信号[22];共培养后,骨髓间充质干细胞形态由长梭形变为多边形或方形,提示向成骨细胞分化,碱性磷酸酶、骨钙素和骨桥蛋白的基因表达和蛋白水平均显著上调。
相较于β-磷酸三钙,α-磷酸三钙颗粒大小均匀、纯度更高、溶解度和/或吸收速率更高[23]。利用共沉淀法制备α-磷酸三钙,将α-磷酸三钙与大鼠骨髓间充质干细胞在成骨诱导培养基培养条件下孵育,7 d后细胞达到融合,各种成骨相关基因包括碱性磷酸酶、Runx2、Ⅰ型胶原蛋白的表达水平明显升高[23]。将3D打印技术应用于α-磷酸三钙的制备,形成的α-磷酸三钙多孔支架具有三维物理多孔结构,提供更大的表面积,改善了细胞分布,增强了细胞外基质的产生,允许细胞黏附和增殖与组织再生[24]。生物因子与支架的结合已经是当前支架促进干细胞成骨分化的研究热点,CAO等[25]将骨形态发生蛋白2多肽E7结构域通过静电力辅助锚定在3D打印的α-磷酸三钙生物支架材料上,构建了E7骨形态发生蛋白2多肽递送系统。蛋白检测试剂盒检测结果表明,E7骨形态发生蛋白2肽在α-磷酸三钙3D多孔支架上呈较高负载,并稳定释放,实现了骨形态发生蛋白2多肽的缓释。利用RT-qPCR检测成骨分化生物因子,Runx2和碱性磷酸酶早期表达、骨钙素表达水平明显增高,表明多孔α-磷酸三钙支架复合E7骨形态发生蛋白2肽缓释系统具有更好和更有效的诱导成骨能力。
2.1.3 生物活性玻璃 生物活性玻璃作为生物陶瓷材料的一种,具有高磷灰石形成的生物活性、成骨和血管生成等优良特性。将生物活性玻璃植入骨缺损时,释放出的离子溶解产物可以创造有利于细胞聚集、增殖和分化的局部环境,并能促进成骨细胞相关基因的表达,从而结合宿主骨并刺激新骨生长[26-27]。
改变材料结构可增加材料的比表面积、孔隙率及孔的连通性。纳米颗粒生物活性玻璃具有更大的比表面积,一方面,大的比表面积提供了更多的表面吸附位,使得纳米生物活性玻璃具有更高的生物活性;另一方面,大的比表面积有利于纳米生物活性玻璃释放离子,促进其表面形成磷灰石[28-29],从而具有好的生物学性能。“放射状”球形纳米生物活性颗粒提高了纳米生物活性玻璃的表面积,使离子更快地释放到溶解产物中,并且在材料表面提供更多的蛋白质结合位点,增强了蛋白质吸附,提高生物活性玻璃的成骨能力。“放射状”球形纳米生物活性颗粒提高细胞增殖能力、成骨相关基因(Runx2、Ⅰ型胶原蛋白)的表达、细胞外基质矿化程度、钙结节的密度[30]。介孔生物活性玻璃因其生物活性、生物相容性和骨传导性而备受关注,介孔生物活性玻璃相互连接的大孔网络有利于细胞的黏附和迁移,但同时也增加了支架的降解。ZHANG等[31]利用粉末加工技术来制备一种新型的具有足够机械强度的介孔生物活性玻璃支架,并通过氨基或羧基官能团修饰使介孔生物活性玻璃的比表面积和孔体积减小,降低了介孔生物活性玻璃的降解率同时提升了机械强度;与骨髓间充质干细胞共培养后促进了细胞黏附、增殖,碱性磷酸酶活性及Runx2、碱性磷酸酶、骨涎蛋白和骨钙素的表达均增强。
微量元素掺杂在引导骨髓间充质干细胞分化方面发挥重要作用。稀土元素铕(Eu)不仅可以引导骨髓间充质干细胞的分化,也可用于标记新的骨组织和体内的支架降解。将稀土元素铕与生物活性玻璃纳米颗粒复合制作支架,可以进一步增加生物活性玻璃纳米颗粒的细胞黏附及成骨分化,共培养实验表明随着培养时间的延长,少量的Eu掺杂可以显著促进骨髓间充质干细胞的增殖,显著上调碱性磷酸酶、Ⅰ型胶原蛋白、骨桥蛋白和Runx2基因的表达[32]。通过原位共模板方法将铕引入介孔生物活性玻璃支架中,以获得具有生物标记和骨再生的双功能生物材料Eu-介孔生物活性玻璃支架,Eu-介孔生物活性玻璃支架具有高度互联的孔隙、高比表面积、有序的介孔及均匀分布的Eu,实验结果表明,Eu-介孔生物活性玻璃支架显著促进大多数成骨相关基因骨桥蛋白、Ⅰ型胶原蛋白、骨钙素和骨涎蛋白表达[33]。
无机生物支架材料具有较高的机械强度、极佳的生物相容性、生物可降解性及良好的空间结构等优点,但质地脆和高孔隙率带来的强度差的问题限制了其在组织工程中的应用。目前的研究趋势是通过将无机生物支架材料与有机材料或聚合物等混合,在机械强度和韧性、生物活性、空间结构等方面进行综合改善,增加材料成骨分化的能力的同时增加强度和韧性。
2.2 天然高分子材料 天然高分子材料的生物相容性好,有利于促进细胞的各项生理功能。目前常应用于骨组织工程的有胶原、明胶、丝素蛋白、壳聚糖、纤维素、纤维蛋白原、藻酸盐、脂质体和细胞外基质等[6]。
2.2.1 胶原 胶原是人体内含量最丰富的蛋白质,构成了细胞外基质的主要骨架,其功能主要是连接组织和器官、保护机体等。由于胶原具有亲水特性,可促进细胞的黏附,对于细胞生长能够起到很好的诱导作用,是一种常用的骨移植基质。水解鱼胶原蛋白富含甘氨酸、脯氨酸、谷氨酸、天冬氨酸及多种多肽,这些成分具有主动调节细胞功能的能力。实验证明,水解鱼胶原蛋白可提高骨髓间充质干细胞的存活率,增强碱性磷酸酶的表达,显著上调成骨标志物(Runx2、碱性磷酸酶、骨桥蛋白和骨钙素)的表达;进一步的实验结果表明,水解鱼胶原蛋白不仅可诱导骨髓间充质干细胞的成骨分化,并且诱导作用与MAPK/ERK信号通路有关[34]。
由于单一胶原支架降解速率高、机械性能较差,通常需要结合羟基磷灰石、生物活性玻璃等无机生物支架制成矿化胶原支架,以改善机械性能、降解速率、骨传导性、骨诱导性和生物相容性。胶原/羟基磷灰石作为骨的类似物为更好地促进成骨分化提供了最合适的微环境,从而促进干细胞的成骨分化[35-36]。将大鼠骨髓间充质干细胞接种于胶原、胶原/羟基磷灰石、羟基磷灰石和双相磷酸钙材料上,观察大鼠骨髓间充质干细胞在4组材料的成骨分化情况,胶原/羟基磷灰石复合材料被报道具有良好的体外成骨作用,细胞增殖率均高于其他3组,胶原/羟基磷灰石复合材料培养骨髓间充质干细胞表达Runx2、碱性磷酸酶活性和骨钙素的表达高于其他3组[37]。在真空条件下采用胶原浸渍生物玻璃支架,使得支架中胶原含量增加,利用无机材料与有机材料的结合以模拟骨组织,在骨形成和修复方面具有更高的生物学性能,骨髓间充质干细胞与胶原浸渍生物玻璃支架生物相容性好,无细胞毒性,细胞存活率高,成骨能力及钙矿化也得到改善[38]。
2.2.2 丝素蛋白 丝素蛋白是蚕丝中的主要成分,作为一种天然生物材料具有良好的机械性能和理化特性(如透气透湿性和缓释性等),无毒性,体内外降解率可控,在骨组织工程中应用广泛。
丝素蛋白支架对骨的吸附能力有限,支架性能不够理想,可通过改变制备工艺来调节支架性能,以满足骨组织工程的不同需求。静电纺丝技术生成的静电纺丝素蛋白纳米纤维支架,能够模拟细胞外基质的天然结构和生物功能,具有高比表面积和孔隙率[39]。WU等[40]用聚多巴胺对丝素蛋白进行表面改性,将E7短肽接枝到电纺支架,制作成复合丝素蛋白-聚多巴胺-E7电纺支架。聚多巴胺具有活性官能团,促进钙离子的富集,有利于支架表面矿化[41],E7多肽在保持丝素蛋白支架理化性能的同时,改善了亲水性,使得复合电纺支架能有效地原位募集骨髓间充质干细胞,促进细胞黏附和增殖,从而有效促进组织再生[42]。与骨髓间充质干细胞共培养后,显微镜观察显示,丝素蛋白-聚多巴胺-E7支架中的细胞铺展充分,骨架清晰,碱性磷酸酶活性、成骨标志物基因Ⅰ型胶原蛋白、骨钙素、Runx2和碱性磷酸酶基因表达显著升高,表明丝素蛋白-聚多巴胺-E7具有最佳的成骨分化能力。
单一的丝素蛋白成骨性能低、韧性不足,并且对骨的吸附能力不佳,骨诱导能力有限,很难同时满足骨组织工程中对支架各种不同性质的要求。因此在改变丝素蛋白制备工艺的同时,可与其他材料相结合来制备丝素蛋白复合生物支架材料,以满足骨组织工程的不同需求。静电纺丝技术使复合支架具有相当大的孔隙率,并充分将有机和无机材料结合,模仿骨细胞外基质来促进骨再生。采用静电纺丝技术制备含有纳米羟基磷灰石和纳米纤维丝素的复合支架,并用骨形态发生蛋白2处理支架表面,丝素蛋白/羟基磷灰石支架比丝素蛋白支架具有更高的机械强度和弹性模量;骨髓间充质干细胞培养实验结果表明,细胞在支架上黏附和铺展良好,培养在丝素蛋白/羟基磷灰石/骨形态发生蛋白2支架上的细胞碱性磷酸酶表达、钙结节升高明显,表明复合支架具有更好的成骨分化能力,促进了骨髓间充质干细胞的成骨分化[43]。利用生物活性玻璃刺激成骨分化的特性和丝素蛋白的易加工性,通过3D打印技术制成生物活性玻璃/丝素蛋白复合支架,丝素蛋白的加入使得复合支架具有更加优良的生物相容性及缓慢降解特性,并保留生物活性玻璃的促进成骨分化特点[44]。MIDHA等[45]将明胶与丝素蛋白混合后加入生物活性玻璃,利用3D打印技术制成的丝素蛋白-明胶-生物活性玻璃支架,接种在支架上的骨髓间充质干细胞存活良好,细胞呈现致密堆积,细胞基质覆盖了支架丝状结构和孔隙,碱性磷酸酶和Runx2、骨桥蛋白、骨连接蛋白和整合素骨涎蛋白、骨钙素分化均增高明显。
2.2.3 壳聚糖 壳聚糖是甲壳素的脱乙酰基衍生物,是自然界中发现的一种稀有的带正电荷的碱性多糖。壳聚糖具有良好的生物相容性及抗菌性、无毒、无刺激性、优良的降解性及可塑性等特点,被广泛应用于医学领域。
壳聚糖的机械性能较差、抗剪切能力不足、骨传导性能不佳,难以独立用作骨组织工程支架中,与其他仿生材料复合后可优势互补,在骨组织工程中发挥更大的作用[46-47]。采用乳液电纺法制备了壳聚糖/纯聚乳酸共混纳米纤维支架,纯聚乳酸纳米纤维可模拟细胞外基质的结构,形成的亲水胶体,促进组织液和营养物质的扩散,增加了支架的生物相容性;与骨髓间充质干细胞共培养后,附着在该支架上的细胞具有良好的黏附性和活性,促进了细胞的增殖,显示出明显的基质矿化,提高了Runx2、Ⅰ型胶原蛋白等基因的表达水平[48]。WANG等[49]通过冷冻干燥和交联法制备壳聚糖/明胶/脂肪源性细胞外基质支架,保留了脂肪源性细胞外基质支架促进细胞黏附和增殖的能力,以及壳聚糖促进成骨分化的能力,提高了支架的生物活性,克服了抗压强度低的缺点,实验结果表明,壳聚糖/明胶/脂肪源性细胞外基质支架的平均细胞贴壁率增高,细胞在支架上分布良好,碱性磷酸酶活性及骨桥蛋白、Runx2、碱性磷酸酶基因表达的比值均随时间的延长而增加。
将壳聚糖适当处理后能够形成具有缓释促成骨药物的结构,壳聚糖由于其正电荷与带负电荷的黏膜表面相互作用,使得药物更容易被跨黏膜吸收。ZHANG等[50]将载阿司匹林的壳聚糖纳米粒包埋在不对称胶原-壳聚糖膜中,载阿司匹林壳聚糖纳米颗粒可以使阿司匹林从复合颗粒中缓慢且可控地释放。载阿司匹林的壳聚糖纳米粒-不对称胶原-壳聚糖膜横截面具有致密层和疏松层,不对称膜的疏松层可促进细胞黏附,致密层可有效隔离骨缺损与周围结缔组织介入;CCK-8检测结果显示,细胞在该支架上生长良好,壳聚糖纳米粒-不对称胶原-壳聚糖膜组第7天碱性磷酸酶活性较高,表明壳聚糖纳米粒-不对称胶原-壳聚糖膜具有良好的生物相容性和骨传导作用。
天然高分子材料虽然具有优良的生物相容性和可控的生物降解性,但却有机械强度不足、韧性差等缺点,往往需制备成复合支架材料以弥补不足,提高支架的生物活性,使骨组织再生水平进一步优化。丝素蛋白应用在骨组织工程中存在较低的机械性能和有限的骨诱导能力缺点,虽然目前的研究从不同方面来改善丝素蛋白性能,但改性丝素蛋白依然不能满足骨组织工程所需要的机械强度兼具成骨性能,仍需要大量研究来进一步增强丝素蛋白等天然高分子材料的成骨活性。
2.3 合成高分子材料 人工合成有机高分子材料性质稳定,降解周期可以调节,易于加工,有着良好的生物兼容性,能满足骨组织工程的要求,在实验研究中也有良好的成骨效能[51],其中应用较为广泛的有聚己内酯、聚乳酸、聚乙醇酸等。
2.3.1 聚乳酸 聚乳酸具有低密度、易加工、机械性能良好及生物相容性优等优点,但其降解速率快,降解后容易引起周围组织的无菌性炎症反应。鉴于这些方面的局限性,常常将聚乳酸和其他生物材料制成复合生物材料充分发挥促进成骨分化的优点。锶(Sr)可有效抑制骨吸收,增加骨形成相关基因的表达和碱性磷酸酶活性,抑制破骨细胞的分化,促进骨形成[52]。采用电沉积法制备了不同量锶掺杂的羟基磷灰石矿化电纺聚乳酸纳米纤维膜,培养骨髓间充质干细胞后,羟基磷灰石矿化的Sr/聚乳酸纳米纤维膜能促进骨髓基质细胞的增殖,提高碱性磷酸酶活性、钙结节和骨钙素生成及成骨相关基因表达[53]。
聚乳酸和明胶复合纤维电纺丝支架可模拟天然细胞基质中胶原纤维网络的微观结构,用CaCl2溶液处理后,明胶将钙离子预吸附到纤维表面,形成Ca-聚乳酸-明胶复合纤维电纺丝支架。预吸附的钙离子可加速矿物沉积,使得Ca-聚乳酸-明胶复合纤维电纺丝支架具有较高的蛋白质吸附潜力和较快的矿化速率。将骨髓间充质干细胞接种于聚乳酸-明胶复合纤维电纺丝支架和Ca-聚乳酸-明胶复合纤维电纺丝支架上,细胞呈持续增殖状态,并且在两种纤维上都清楚地观察到矿化和钙沉积,Ca-聚乳酸-明胶复合纤维电纺丝支架比聚乳酸-明胶复合纤维电纺丝支架具有更强的矿化诱导能力,并且显著促进碱性磷酸酶和Ⅰ型胶原蛋白的表达[54]。
2.3.2 聚己内酯 聚己内酯具有生物相容性、可降解性、良好的易加工和可塑性,是可吸收材料研究的重点,但同时柔性和弹性过强,难以满足生物支架材料所需的机械强度,目前研究主要集中于通过表面涂层或与其他材料复合来满足其在骨组织工程的需要。
POH等[55]以聚己内酯结合生物活性玻璃或锶(Sr)替代生物活性玻璃颗粒制作复合支架(聚已内酯/生物活性玻璃支架和聚已内酯/Sr/生物活性玻璃支架),聚已内酯/生物活性玻璃支架和聚已内酯/Sr/生物活性玻璃支架显示出广泛的跨越支架微丝结构的细胞桥接形成和细胞增殖,聚已内酯/生物活性玻璃支架和聚已内酯/Sr/生物活性玻璃支架组骨钙素基因表达水平高于聚已内酯/磷酸钙和聚已内酯组。WANG等[56]研制了羟基磷灰石/胶原涂层的聚已内酯支架,羟基磷灰石和胶原涂层的支架兼具两者的优点,胶原涂层明显促进了细胞的生长和植入时的生物反应,改善了骨细胞的增殖、黏附,促进了成骨分化[57]。结果证实了成骨细胞分化激活的关键因子Runx2、碱性磷酸酶、骨钙素等mRNA和蛋白水平在羟基磷灰石/胶原涂层的聚己内酯支架中均显著增高。
以聚乙烯吡咯烷酮/牛血清白蛋白/骨形态发生蛋白2衍生多肽复合物为核心溶液,聚己内酯/Ⅰ型胶原复合物为壳液,采用同轴静电纺丝技术构建了微纤维支架,并通过骨髓间充质干细胞亲和肽(E7)的共价接枝形成复合功能化支架,聚乙烯吡咯烷酮和牛血清白蛋白分别作为塑形剂和稳定剂保存骨形态发生蛋白2肽。骨形态发生蛋白2衍生肽持续释放并保持生物活性,显著促进了骨髓间充质干细胞的成骨分化。并且聚已内酯和Ⅰ型胶原蛋白构成同轴纤维的外壳,起到了很好的控制蛋白质释放和支持细胞生长的保护作用。在模拟体液中,支架上培养的骨髓间充质干细胞分布均匀,生长旺盛,几乎覆盖支架表面,碱性磷酸酶活性显著增高,碱性磷酸酶、骨桥蛋白、骨桥蛋白和Runx2等成骨标志物的表达水平随时间增加,钙结节形成最高[58]。
合成高分子材料的生物相容性和生物可降解性良好,然而亲水性低、机械性能差,使其在细胞黏附和成骨分化方面不能满足骨组织工程的需求。目前研究致力于将合成高分子材料表面改性和复合其他材料提高其机械性能、亲水性和成骨性能。
2.4 钛金属支架材料 目前临床最为常用的金属植入材料为钛及其合金。钛材料机械强度高,具有良好的力学性能和弹性模量,抗腐蚀性好,生物相容性高,钛及其钛合金被认为是最有前途的骨替代植入物。然而,天然钛基材料不会激活周围细胞,引起一系列有利于体内成骨的生理反应。此外,钛基体的表面惰性会延迟愈合时间,导致种植体松动。因此,许多表面改性方法被用来提高钛基种植体的骨整合和骨愈合能力。
单一功能钛材料支架已不能满足当前临床需要,钛支架材料也面临着生物反应慢、细胞黏附率低及可能的局部定植菌感染等问题[59-60]。除了具有良好的骨诱导性能外,具有促进血管化、抗菌等生物医学功能的骨替代材料有较高的临床应用价值。ZHANG等[61]在钛支架表面构建了一种负载万古霉素的聚多巴胺修饰的白蛋白纳米颗粒和细胞黏附肽的硅磷酸钙复合涂层,形成Van-pBNPs/PEP@pSiCaP-Ti支架,以模拟天然骨的细胞外基质促进支架表面成骨,硅磷酸钙可作为成骨细胞矿化的螯合剂和功能离子库,而负载万古霉素的聚多巴胺修饰的白蛋白纳米颗粒不仅具有良好的生物相容性和无免疫性,而且作为载体材料具有很高的载药效率,有效延缓药物在体内的循环期。聚多巴胺含有大量的酚羟基,可以为含有氨基或硫醇官能团的各种生物分子提供固定位点。细胞黏附肽可以刺激细胞膜上的整合素受体,促进骨髓间充质干细胞的早期黏附和成骨分化,从而加速骨缺损的愈合,提高钛种植体的成骨能力。将该支架与骨髓间充质干细胞共培养后,功能化的涂层不仅改善了早期细胞的黏附、铺展、增殖,提高了碱性磷酸酶活性,RT-qPCR和Western-Blot检测结果也表明支架促进了细胞Runx2、Ⅰ型胶原、骨钙素的表达,抗菌实验表明支架对表皮葡萄球菌有较强的抗菌能力,结果证明支架促进成骨分化的同时具有较强的抗菌能力。
材料表面的物理、化学和生物特性可调节细胞的增殖、黏附、生长和分化。对钛种植体表面进行适当的改性以引导细胞的生物学行为,从而改善钛金属的骨整合和种植体的性能。LI等[62]利用具有生物活性、良好骨诱导潜能的氧化石墨烯改良钛种植体的表面,氧化石墨烯表面含有大量的羧基和羟基等含氧活性官能团,易于对生物材料进行功能化修饰[63-64]。经氧化石墨烯改性后钛表面的亲水性得到了改善,更有利于细胞外基质蛋白的吸附,从而促进细胞的初始黏附、增殖、分化和骨组织矿化,并且提高了支架的蛋白质吸附;接种骨髓间充质干细胞后显著促进了细胞的增殖和黏附,碱性磷酸酶活性更高,表面的矿化程度明显增高;碱性磷酸酶、Runx2、骨钙素、骨桥蛋白等成骨相关基因表达明显增高,表明氧化石墨烯修饰明显促进了骨髓间充质干细胞的早期成骨分化[62]。DING等[65]在钛表面制备了含锶的溶菌酶纳米膜,溶菌酶纳米膜涂层功能化的钛表面不仅具有良好的抗菌性能,并且增强了钛基质的细胞相容性。锶(Sr)的加入也可以刺激细胞膜上的受体,从而促进新骨形成和抑制骨吸收。细胞形态学观察、细胞活力测定、碱性磷酸酶染色和定量分析结果表明,负载Sr离子的溶菌酶纳米膜涂层功能化的钛可促进骨髓基质细胞的早期黏附、增殖和成骨分化;实时定量聚合酶链反应检测证实,负载Sr离子的溶菌酶纳米膜涂层功能化的钛在分子水平上调骨髓间充质干细胞成骨相关基因(骨形态发生蛋白2、Runx2和Ⅰ型胶原)的表达。负载Sr离子的溶菌酶纳米膜涂层功能化的钛的制备在骨科和牙科植入物的表面改性方面具有很大的潜力。
钛材料机械强度高、耐腐蚀性高,是骨科和牙科领域的首选植入物,但金属材料的生物惰性及弹性模量较高等问题仍需大量的研究来解决,钛基体的表面惰性会延迟愈合时间,导致种植体松动。通过改性提高钛材料与骨组织的结合,可以进一步拓宽钛基质材料在骨组织工程中的应用。
2.5 支架材料特性因素 除了将不同支架材料复合可极大改进支架材料的成骨性能,支架的孔隙率/孔径大小、材料的亲水性/疏水性、表面能/润湿性、表面拓扑结构/粗糙程度、基底刚度/弹性模量等材料特性都也会影响骨髓间充质干细胞的黏附、细胞信号表达和成骨分化。
支架的孔径和孔隙率不仅在细胞的黏附、增殖和分化中发挥重要的作用,还显著影响支架的物理性质,从而进一步影响细胞的生物学行为。相互连通的多孔支架允许细胞的迁移、增殖及营养物质和代谢产物的交换,从而有利于骨组织的再生,大孔径的材料能获得更高的细胞密度,利于细胞的增殖。较高的孔隙率增加支架材料的比表面积,利于细胞的黏附和增殖,以及生长因子释放和对细胞的生物反应[66]。支架表面的粗糙程度不仅可增加支架的比表面积,而且粗糙的表面有利于组织在支架的嵌入、干细胞的黏附,使得支架与组织、细胞更充分地连接,有利于随后的生物反应和新骨的生成。在亲水性高的支架材料表面细胞的附着与增殖增强。聚乳酸亲水性差、缺乏天然分子识别位点等缺点,限制了其在组织工程中的应用,通过低温等离子表面处理技术对材料表面进行持续改性,在增加亲水的同时也增加了材料表面的粗糙程度,更加有利于细胞的黏附[67]。研究表明,坚硬基质支架更利于骨髓间充质干细胞生物因子的表达和成骨分化;较高弹性模量的生物材料可提升支架刚度,有利于成骨细胞的培养,可促进骨髓间充质干细胞的成骨分化;强韧的支架表面有利于张力纤维的排布、细胞的扩展和分化,在调节骨髓间充质干细胞的黏附、增殖和成骨分化中发挥至关重要的作用[68-69]。

| [1] LIU W, CHEN D, JIANG G, et al. A lithium-containing nanoporous coating on entangled titanium scaffold can enhance osseointegration through Wnt/β-catenin pathway. Nanomedicine. 2018;14(1):153-164. [2] SONG K, HUANG M, SHI Q, et al. Cultivation and identification of rat bone marrow-derived mesenchymal stem cells. Mol Med Rep. 2014;10(2):755-760. [3] LI X, WANG M, JING X, et al. Bone Marrow-and Adipose Tissue-Derived Mesenchymal Stem Cells: Characterization,Differentiation,and Applications in Cartilage Tissue Engineering. Crit Rev Eukaryot Gene Expr. 2018;28(4):285-310. [4] POLYMERI A, GIANNOBILE WV, KAIGLER D. Bone Marrow Stromal Stem Cells in Tissue Engineering and Regenerative Medicine. Horm Metab Res. 2016; 48(11):700-713. [5] 刘相杰,宋科官.生物支架材料及间充质干细胞在骨组织工程中的研究与应用[J].中国组织工程研究,2018,22(10):1618-1624. [6] 张圣敏,刘超.生物支架材料诱导脂肪来源干细胞成骨分化的最新热点[J].中国组织工程研究,2020,24(7):1107-1116. [7] UTARA S, KLINKAEWNARONG J. Sonochemical synthesis of nano-hydroxyapatite using natural rubber latex as a templating agent. Ceram Int. 2015;41(10):14860-14867. [8] SU Y, KOMASA S, LI P, et al. Synergistic effect of nanotopography and bioactive ions on peri-implant bone response. Int J Nanomed. 2017;12:925-934. [9] WANG J, WANG M, CHEN F, et al. Nano-Hydroxyapatite Coating Promotes Porous Calcium Phosphate Ceramic-Induced Osteogenesis Via BMP/Smad Signaling Pathway. Int J Nanomedicine. 2019;14:7987-8000. [10] LIU H, PENG H, WU Y, et al. The promotion of bone regeneration by nanofibroushydroxyapatite/chitosan scaffolds by effects on integrin-BMP/Smad signaling pathway in BMSCs. Biomaterials. 2013;34(18):4404-4417. [11] SHALUMON KT, LIAO HT, KUO CY, et al. Rational design of gelatin/nanohydroxyapatite cryogel scaffolds for bone regeneration by introducing chemical and physical cues to enhance osteogenesis of bone marrow mesenchymal stem cells. Mater Sci Eng C Mater Biol Appl. 2019;104: 109855. [12] CHUENJITKUNTAWORN B, OSATHANON T, NOWWAROTE N, et al. The efficacy of polycaprolactone/hydroxyapatite scaffold in combination with mesenchymal stem cells for bone tissue engineering. J Biomed Mater Res A. 2016;104(1):264-271. [13] DU MC, CHEN B, MENG QY, et al. 3D bioprinting of BMSC-laden methacrylamide gelatin scaffolds with CBD-BMP2-collagen microfibers. Biofabrication. 2015;7(4):1-10. [14] ZHANG H, MAO X, DU Z, et al. Three dimensional printed macroporous polylactic acid/hydroxyapatite composite scaffolds for promoting bone formation in a critical-size rat calvarial defect model. Sci Technol Adv Mater. 2016;17(1):136-148. [15] HU JX, ZHU YJ, TONG H, et al. A detailed study of homogeneous agarose/hydroxyapatite nanocomposites for load-bearing bone tissue. Int J Biol Macromol. 2016;82(1):134-143. [16] LIU YQ, HONG ZL, ZHAN LB, et al. Wedelolactone enhances osteoblastogenesis by regulating Wnt/β-catenin signaling pathway but suppresses osteoclastogenesis by NF-κB/c-fos/NFATc1 pathway. Sci Rep. 2016;6:32260. [17] LIU YQ, HAN XF, BO JX, et al. Wedelolactone Enhances Osteoblastogenesis but Inhibits Osteoclastogenesis through Sema3A/NRP1/PlexinA1 Pathway. Front Pharmacol. 2016;7:375. [18] DONG P, ZHU D, DENG X, et al. Effect of hydroxyapatite nanoparticles and wedelolactone on osteoblastogenesis from bone marrow mesenchymal stem cells. J Biomed Mater Res A. 2019;107(1):145-153. [19] 王德欣,许战武,裴国献.骨髓间充质干细胞在淫羊藿苷/羟基磷灰石/聚乳酸-羟基乙酸共聚物支架上的成骨[J].中国组织工程研究, 2020,24(25):3974-3980. [20] LEE MH, YOU C, KIM KH. Combined Effect of a Microporous Layer and Type I Collagen Coating on a Biphasic Calcium Phosphate Scaffold for Bone Tissue Engineering. Materials (Basel). 2015;8(3):1150-1161. [21] LIN J, SHAO J, JUAN L, et al. Enhancing bone regeneration by combining mesenchymal stem cell sheets with β-TCP/COL-I scaffolds. J Biomed Mater Res B Appl Biomater. 2018;106(5):2037-2045. [22] CHEN T, WANG Y, BU L, et al. Construction of functional tissue-engineered bone using cell sheet technology in a canine model. Exp Ther Med. 2014; 7(4):958-962. [23] LIU J, ZHAO L, NI L, et al. The effect of synthetic α-tricalcium phosphate on osteogenic differentiation of rat bone mesenchymal stem cells. Am J Transl Res. 2015;7(9):1588-1601. [24] WÓJTOWICZ J, LESZCZYŃSKA J, CHRÓŚCICKA A, et al. Comparative in vitro study of calcium phosphate ceramics for their potency as scaffolds for tissue engineering. Biomed Mater Eng. 2014;24(3):1609-1623. [25] CAO Q, HE Z, SUN WQ, et al. Improvement of calcium phosphate scaffold osteogenesis in vitro via combination of glutamate-modified BMP-2 peptides. Mater Sci Eng C Mater Biol Appl. 2019;96:412-418. [26] OJANSIVU M, HYVÄRI L, KELLOMÄKI M, et al. Bioactive glass induced osteogenic differentiation of human adipose stem cells is dependent on cell attachment mechanism and mitogen-activated protein kinases. Eur Cell Mater. 2018;35:54-72. [27] BAINO F, NOVAJRA G, MIGUEZ-PACHECO V, et al. Bioactive glasses: special applications outside the skeletal system. J Non Cryst Solids. 2016;432:15-30. [28] VICHERY C, NEDELEC JM. Bioactive Glass Nanoparticles: From Synthesis to Materials Design for Biomedical Applications. Materials (Basel). 2016; 9(4):288. [29] BUSH JR, LIANG H, DICKINSON M, eta l. Xylan hemicellulose improves chitosan hydrogel for bone tissue regeneration. Polym Adv Technol. 2016;27(8):1050-1055. [30] WANG L, YAN J, HU X, et al. Effect of nanoscale bioactive glass with radial spherical particles on osteogenic differentiation of rat bone marrow mesenchymal stem cells. J Mater Sci Mater Med. 2020;31(3):29. [31] ZHANG X, ZENG D, LI N, et al. Functionalized mesoporous bioactive glass scaffolds for enhanced bone tissue regeneration. Sci Rep. 2016;6:19361. [32] LI F, WANG M, PI G, et al. Europium Doped Monodispersed Bioactive Glass Nanoparticles Regulate the Osteogenic Differentiation of Human Marrow Mesenchymal Stem Cells. J Biomed Nanotechnol. 2018;14(4):756-764. [33] WU C, XIA L, HAN P, et al. Europium-Containing Mesoporous Bioactive Glass Scaffolds for Stimulating in Vitro and in Vivo Osteogenesis. ACS Appl Mater Interfaces. 2016;8(18):11342-11354. [34] LIU C, SUN J. Potential application of hydrolyzed fish collagen for inducing the multidirectional differentiation of rat bone marrow mesenchymal stem cells. Biomacromolecules. 2014;15(1):436-443. [35] XU SJ, QIU ZY, WU JJ, et al. Osteogenic Differentiation Gene Expression Profiling of hMSCs on Hydroxyapatite and Mineralized Collagen. Tissue Eng Part A. 2016;22(1-2):170-181. [36] SU W, MA X, SUN X, et al. Physicochemical characterisation and thermal decomposition of synthetic collagen based nanocomposites in comparison with natural bone. Adv Appl Ceramics. 2015;115:29-35. [37] SUN X, SU W, MA X, et al. Comparison of the osteogenic capability of rat bone mesenchymal stem cells on collagen,collagen/hydroxyapatite, hydroxyapatite and biphasic calcium phosphate. Regen Biomater. 2018;5(2): 93-103. [38] KIDO HW, GABBAI-ARMELIN PR, AVANZI IR, et al. Vacuumed collagen-impregnated bioglass scaffolds: Characterization and influence on proliferation and differentiation of bone marrow stromal cells. J Biomed Mater Res B Appl Biomater. 2019;107(2):211-222. [39] LIU G, GU Z, HONG Y, et al. Electrospun starch nanofibers: Recent advances, challenges, and strategies for potential pharmaceutical applications. J Control Release. 2017;252:95-107. [40] WU J, CAO L, LIU Y, et al. Functionalization of Silk Fibroin Electrospun Scaffolds via BMSC Affinity Peptide Grafting through Oxidative Self-Polymerization of Dopamine for Bone Regeneration. ACS Appl Mater Interfaces. 2019;11(9): 8878-8895. [41] BATUL R, TAMANNA T, KHALIQ A, et al. Recent progress in the biomedical applications of polydopamine nanostructures. Biomater Sci. 2017;5(7):1204-1229. [42] LI Q, XING D, MA L, et al. Synthesis of E7 peptide-modified biodegradable polyester with the improving affinity to mesenchymal stem cells. Mater Sci Eng C Mater Biol Appl. 2017;73:562-568. [43] NIU B, LI B, GU Y, et al. In vitro evaluation of electrospun silk fibroin/nano-hydroxyapatite/BMP-2 scaffolds for bone regeneration. J Biomater Sci Polym Ed. 2017;28(3):257-270. [44] MIDHA S, MURAB S, GHOSH S. Osteogenic signaling on silk-based matrices. Biomaterials. 2016;97:133-153. [45] MIDHA S, KUMAR S, SHARMA A, et al. Silk fibroin-bioactive glass based advanced biomaterials: towards patient-specific bone grafts. Biomed Mater. 2018;13(5):055012. [46] KHAN G, YADAV SK, PATEL RR, et al. Development and Evaluation of Biodegradable Chitosan Films of Metronidazole and Levofloxacin for the Management of Periodontitis. AAPS Pharm Sci Tech. 2016;17(6):1312-1325. [47] HPS AK, SAURABH CK, ADNAN A, et al. A review on chitosan-cellulose blends and nanocellulose reinforced chitosan biocomposites: Properties and their applications. Carbohydr Polym. 2016;150:216-226. [48] SHEN R, XU W, XUE Y, et al. The use of chitosan/PLA nano-fibers by emulsion eletrospinning for periodontal tissue engineering. Artif Cells Nanomed Biotechnol. 2018;46(sup2):419-430. [49] WANG X, YU T, CHEN G, et al. Preparation and Characterization of a Chitosan/Gelatin/Extracellular Matrix Scaffold and Its Application in Tissue Engineering. Tissue Eng Part C Methods. 2017;23(3):169-179. [50] ZHANG J, MA S, LIU Z, et al. Guided bone regeneration with asymmetric collagen-chitosan membranes containing aspirin-loaded chitosan nanoparticles. Int J Nanomedicine. 2017;12:8855-8866. [51] LIAO J, SHI K, DING Q, et al. Recent developments in scaffold-guided cartilage tissue regeneration. J Biomed Nanotechnol. 2014;10(10):3085-3104. [52] LUO Y, CHEN S, SHI Y, et al. 3D printing of strontium-doped hydroxyapatite based composite scaffolds for repairing critical-sized rabbit calvarial defects. Biomed Mater. 2018;13(6):065004. [53] HAN X, ZHOU X, QIU K, et al. Strontium-incorporated mineralized PLLA nanofibrous membranes for promoting bone defect repair. Colloids Surf B Biointerfaces. 2019;179:363-373. [54] CAO M, ZHOU Y, MAO J, et al. Promoting osteogenic differentiation of BMSCs via mineralization of polylactide/gelatin composite fibers in cell culture medium. Mater Sci Eng C Mater Biol Appl. 2019;100:862-873. [55] POH PSP, HUTMACHER DW, HOLZAPFEL BM, et al. In vitro and in vivo bone formation potential of surface calcium phosphate-coated polycaprolactone and polycaprolactone/bioactive glass composite scaffolds. Acta Biomater. 2016;30:319-333. [56] WANG T, YANG X, QI X, et al. Osteoinduction and proliferation of bone-marrow stromal cells in three-dimensional poly (ε-caprolactone)/ hydroxyapatite/collagen scaffolds. J Transl Med. 2015;13:152. [57] VANDROVCOVÁ M, DOUGLAS T, HAUK D, et al. Influence of collagen and chondroitin sulfate (CS) coatings on poly-(lactide-co-glycolide) (PLGA) on MG 63 osteoblast-like cells. Physiol Res. 2011;60(5):797-813. [58] CHI H, JIANG A, WANG X, et al. Dually optimized polycaprolactone/collagen I microfiber scaffolds with stem cell capture and differentiation-inducing abilities promote bone regeneration. J Mater Chem B. 2019;7(44):7052-7064. [59] JIANG N, GUO Z, SUN D, et al. Promoting Osseointegration of Ti Implants through Micro/Nanoscaled Hierarchical Ti Phosphate/Ti Oxide Hybrid Coating. ACS Nano. 2018;12(8):7883-7891. [60] ZHOU W, WANG T, GAN Y, et al. Effect of micropore/microsphere topography and a silicon-incorporating modified titanium plate surface on the adhesion and osteogenic differentiation of BMSCs. Artif Cells Nanomed Biotechnol. 2020;48(1):230-241. [61] ZHANG B, LI J, HE L, et al. Bio-surface coated titanium scaffolds with cancellous bone-like biomimetic structure for enhanced bone tissue regeneration. Acta Biomater. 2020;114:431-448. [62] LI Q, WANG Z. Involvement of FAK/P38 Signaling Pathways in Mediating the Enhanced Osteogenesis Induced by Nano-Graphene Oxide Modification on Titanium Implant Surface. Int J Nanomedicine. 2020;15:4659-4676. [63] GURUNATHAN S, KIM JH. Synthesis,toxicity,biocompatibility,and biomedical applications of graphene and graphene-related materials. Int J Nanomedicine. 2016;11:1927-1945. [64] SHIN SR, LI YC, JANG HL, et al. Graphene-based materials for tissue engineering. Adv Drug Deliv Rev. 2016;105(Pt B):255-274. [65] DING Y, YUAN Z, LIU P, et al. Fabrication of strontium-incorporated protein supramolecular nanofilm on titanium substrates for promoting osteogenesis. Mater Sci Eng C Mater Biol Appl. 2020;111:110851. [66] KNYCHALA J, BOUROPOULOS N, CATT CJ, et al. Pore geometry regulates early stage human bone marrow cell tissue formation and organisation. Ann Biomed Eng. 2013;41(5):917-930. [67] 莫志超,刘青,时东陆,等.低温等离子接枝改性聚乳酸支架的亲水性[J].青岛科技大学学报(自然科学版),2017,38(2):54-58. [68] WITKOWSKA-ZIMNY M, WROBEL E, MROWKA P. α2β1 integrin-mediated mechanical signals during osteodifferentiation of stem cells from the Wharton’s jelly of the umbilical cord. Folia Histochem Cytobiol. 2014;52(4): 297-307. [69] SUN M, CHI G, XU J, et al. Extracellular matrix stiffness controls osteogenic differentiation of mesenchymal stem cells mediated by integrin α5. Stem Cell Res Ther. 2018;9(1):52. |
| [1] | 谭新访, 郭艳幸, 秦晓飞, 张斌清, 赵东亮, 潘琨琨, 李瑜卓, 陈皓宇. 顺轴疲劳运动对兔髌股关节软骨损伤的影响[J]. 中国组织工程研究, 2022, 26(在线): 1-6. |
| [2] | 李灿辉, 吴征杰, 曾焰辉, 何影浩, 司徒晓鹏, 杜雪莲, 洪 石, 何家雄. 骨科手术机器人辅助与传统透视下经皮骶髂螺钉置入的优劣分析[J]. 中国组织工程研究, 2022, 26(9): 1434-1438. |
| [3] | 朱 婵, 韩栩珂, 姚承佼, 周 倩, 张 强, 陈 秋. 人体唾液成分与骨质疏松/骨量低下[J]. 中国组织工程研究, 2022, 26(9): 1439-1444. |
| [4] | 金 涛, 刘 林, 朱晓燕, 史宇悰, 牛建雄, 张同同, 吴树金, 杨青山. 骨关节炎与线粒体异常[J]. 中国组织工程研究, 2022, 26(9): 1452-1458. |
| [5] | 靖金鹏, 张 玥, 刘效敏, 刘 壹. 活血类中药注射剂预防骨科术后深静脉血栓形成的网状Meta分析[J]. 中国组织工程研究, 2022, 26(9): 1467-1476. |
| [6] | 许新忠, 吴钟汉, 余水生, 赵 耀, 徐春归, 张 鑫, 郑嵋戈, 荆珏华. 斯氏针置入股骨头不同方式的生物力学分析[J]. 中国组织工程研究, 2022, 26(9): 1313-1317. |
| [7] | 魏国强, 李云峰, 王 一, 牛晓芬, 车丽芳, 王海燕, 李志军, 史国鹏, 白 灵, 莫 凯, 张晨晨, 许阳阳, 李筱贺. 非均匀材料股骨在不同负荷情况下的生物力学分析[J]. 中国组织工程研究, 2022, 26(9): 1318-1322. |
| [8] | 李 获, 王 鹏, 高健明, 蒋浩然, 鲁晓波, 彭 江. 股骨头坏死血运重建与内部微观结构改变的关系[J]. 中国组织工程研究, 2022, 26(9): 1323-1328. |
| [9] | 李 睿, 史 文, 杨士彩, 吕林蔚, 张春秋. 夹板外固定与散巴布剂对桡骨骨折模型兔骨愈合的影响[J]. 中国组织工程研究, 2022, 26(9): 1329-1333. |
| [10] | 袁加斌, 朱宗东, 唐孝明, 魏 丹, 谭 波, 肖成伟, 赵淦琳炜, 廖 锋. 难复性股骨转子间骨折的解剖分型与复位策略[J]. 中国组织工程研究, 2022, 26(9): 1341-1345. |
| [11] | 张吉超, 董跃福, 牟志芳, 张 震, 李冰言, 徐祥钧, 李佳意, 任 梦, 董万鹏. 骨关节炎患者在不同步态角度下膝关节内部生物力学变化的有限元分析[J]. 中国组织工程研究, 2022, 26(9): 1357-1361. |
| [12] | 刘 峰, 冯 毅. 步态周期下不同克氏针张力带治疗髌骨横行骨折的有限元分析[J]. 中国组织工程研究, 2022, 26(9): 1367-1371. |
| [13] | 姚晓玲, 彭建城, 许岳荣, 杨志东, 张顺聪. 可变角度零切迹前路椎间融合内固定系统治疗脊髓型颈椎病:30个月随访[J]. 中国组织工程研究, 2022, 26(9): 1377-1382. |
| [14] | 姜欢畅, 张兆飞, 梁 德, 江晓兵, 杨晓东, 刘志祥. 单侧多方向弯曲与直行椎体成形治疗胸腰椎骨质疏松性压缩骨折优势的比较[J]. 中国组织工程研究, 2022, 26(9): 1407-1411. |
| [15] | 遇呈祥, 刘乐洪, 李文博, 陈金石, 冉春雷, 王忠平. 脊柱和骨盆矢状位参数与椎体成形治疗胸腰椎骨质疏松性椎体压缩骨折预后的相关性[J]. 中国组织工程研究, 2022, 26(9): 1412-1417. |
骨髓间充质干细胞来源于中胚层,具有多向分化潜能,可以分化为骨、软骨、脂肪、肌腱、韧带、肌肉、神经等组织,具有来源丰富、易于获取、培养简单、免疫原性低和外源基因容易转染并长期表达的特点,并且成骨分化能力优良,被广泛应用于骨组织工程[2-4]。理想的生物支架材料应具备以下条件:①无毒性及无致畸性:对人体无毒性,并且不能导致细胞变性,不能引起炎症反应及免疫排斥反应;②良好的生物相容性和生物可降解性;③足够的机械强度和可塑性:具有一定的柔韧性的同时有足够的机械强度,可承受一定的外力;④具有高孔隙率:高孔隙率有利于代谢废物的排出以及细胞的增殖生长[5-6]。近年来,骨组织工程集中于种子细胞在各种支架材料的增殖以及成骨分化的研究,以制作成拥有优良成骨分化能力的生物支架材料。该文就骨髓间充质干细胞在不同类型生物支架材料的增殖及成骨分化的研究热点做一综述。 中国组织工程研究杂志出版内容重点:生物材料;骨生物材料; 口腔生物材料; 纳米材料; 缓释材料; 材料相容性;组织工程
1.2 纳入与排除标准
纳入标准:①与生物支架材料改造有关的文献;②生物支架材料促进骨髓间充质干细胞成骨分化的相关文献。
排除标准:重复研究与只研究支架作用而未涉及骨髓间充质干细胞的文章。
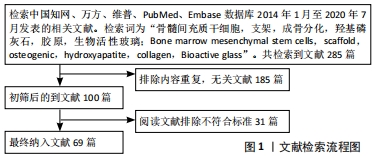
1.3 数据提取 共检索到文献285篇, 其中中文文献95篇、英文文献190篇,排除与研究目的相关性差及内容陈旧、重复的文献,纳入69篇符合标准的文献进行综述,见图1。

1.4 质量评价 符合纳入标准的69篇文献中,文献[1]探讨了骨组织工程发展,文献[2-6]探讨了骨髓间充质干细胞的优点及骨组织工程对支架材料的条件,文献[7-32]探讨了无机材料及其改性促进骨髓间充质干细胞成骨分化的研究进展,文献[34-50]探讨了天然高分子材料及其改性促进骨髓间充质干细胞的研究进展,文献[51-58]探讨了改性合成高分子材料对促进骨髓间充质干细胞成骨分化的研究进展,文献[58-65]探讨了钛金属材料改性促进骨髓间充质干细胞成骨分化研究进展,文献[66-69]描写了支架特性对骨髓间充质干细胞成骨分化的影响。

文题释义:
生物支架材料:目前单一支架材料难以满足骨组织工程的成骨需要,生物支架材料研究将集中于通过不同的制造技术将生物支架材料进行复合,并添加生长因子及具有趋化作用的多肽,将骨组织工程3要素集成一体,制成具有最优良的成骨作用的生物支架。
骨髓间充质干细胞:是一种中胚层来源的多能干细胞,具有易获取、易培养、低免疫原性和易于外源基因转染并长期表达等特点,并具有优良的成骨分化能力,是目前骨组织工程应用最广泛的干细胞。
文章对于近年来生物支架材料改性后促进骨髓间充质干细胞成骨分化研究热点进行归纳综述,指出不同的类型的支架材料在材料特性、制作方式、空间结构、表面涂层、复合材料、生长因子等方面改性后使材料特性、成骨性、生物相容性、抗压强度和弹性模量以及降解率等不断改进,在更优良的促进骨髓间充质干细胞成骨分化的同时,满足骨组织工程飞速发展对生物支架材料的需求,并小结了当前生物支架材料的研究热点以及未来复合支架材料的研究方向。
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||