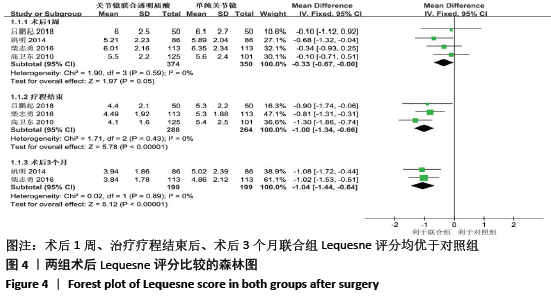
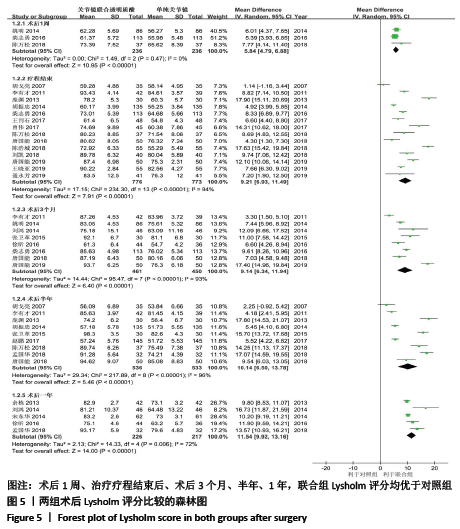
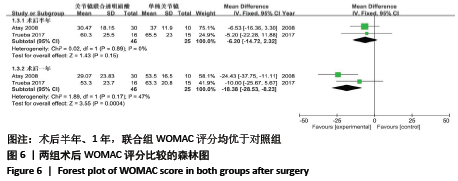
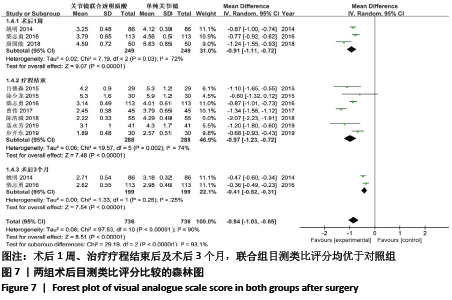
[1] BANNURU RR, OSANI MC, VAYSBROT EE, et al. OARSI guidelines for the non-surgical management of knee, hip, and polyarticular osteoarthritis. Osteoarthritis Cartilage. 2019;27(11):1578-1589.
[2] ZHANG W, MOSKOWITZ RW, NUKI G, et al. OARSI recommendations for the management of hip and knee osteoarthritis, part I: critical appraisal of existing treatment guidelines and systematic review of current research evidence. Osteoarthritis Cartilage. 2007;15(9):981-1000.
[3] SARDANA V, BURZYNSKI J, SCUDERI GR. The influence of the irrigating solution on articular cartilage in arthroscopic surgery: a systematic review. J Orthop. 2019;16(2):158-165.
[4] RYDELL N, BALAZS EA. Effect of intra-articular injection of hyaluronic acid on the clinical symptoms of osteoarthritis and on granulation tissue formation. Clin Orthop Relat Res. 1971;80:25-32.
[5] SHEN D, CHEN M, CHEN K, et al. Efficacy of hyaluronic acid after knee arthroscopy: A systematic review and meta-analysis. J Rehabil Med. 2018;50(10):860-865.
[6] 蒋勰,占美,李棋,等.关节镜下清理术联合关节内透明质酸注射治疗膝关节骨关节炎有效性的系统评价[J].中国循证医学杂志,2012,12(11):1361-1366.
[7] KOLASINSKI SL, NEOGI T, HOCHBERG MC, et al. 2019 American College of Rheumatology/Arthritis Foundation Guideline for the Management of Osteoarthritis of the Hand, Hip, and Knee. Arthritis Rheumatol. 2020; 72(2):220-233.
[8] 中华医学会骨科学分会关节外科学组.骨关节炎诊疗指南(2018年版)[J].中华骨科杂志,2018,38(12):705-715.
[9] ATAY T, ASLAN A, BAYDAR ML, et al. The efficacy of low- and high-molecular-weight hyaluronic acid applications after arthroscopic debridement in patients with osteoarthritis of the knee. Acta Orthopaedica Et Traumatologica Turcica. 2008;42(4):228-233.
[10] TRUEBA VASAVILBASO C, ROSAS BELLO CD, MEDINA LÓPEZ E, et al. Benefits of different postoperative treatments in patients undergoing knee arthroscopic debridement. Open Access Rheumatol. 2017;9:171-179.
[11] 胡戈亮.关节镜清理术结合透明质酸钠注射治疗膝关节骨性关节炎的临床疗效评价[D].武汉:湖北中医学院,2007.
[12] 高卫东.关节镜清理术与关节镜清理术联合玻璃酸钠治疗膝骨关节炎的疗效对比[J].中国中医药现代远程教育,2010, 8(21):143-144.
[13] 李有才,刘晋平,李正南,等.关节镜术后加玻璃酸钠治疗膝骨性关节炎疗效研究[J].中国医师进修杂志,2011,34(8):36-38.
[14] 庞渊,赵光宇,赵之颢.关节镜清理术配合透明质酸钠在膝关节骨性关节炎中的应用效果[J].临床合理用药杂志, 2013, 6(12):104-106.
[15] 余栋.膝关节镜联合玻璃酸钠治疗膝关节骨性关节炎的疗效观察[J].中外医疗, 2013,32(18):134-135.
[16] 姚明,应弋阳,汪满洋.玻璃酸钠联合关节镜清理治疗膝关节炎疗效观察[J].中国药师,2014,17(10):1716-1718.
[17] 胡振忠.关节镜下清理术联合透明质酸钠注射治疗老年膝骨关节炎疗效观察.山东医药,2014,54(48):60-62.
[18] 刘鸿,罗勇,梁轶,等.膝关节镜清理术联合透明质酸钠治疗骨性关节炎的疗效观察[J].医学理论与实践,2014,17(22): 2957-2958, 2971.
[19] 宋东华.膝关节镜下清理术联合玻璃酸钠治疗膝关节骨性关节炎的临床分析[J].中国医药指南,2014,12(30):102-102, 103.
[20] 吕德森.关节镜清理术联合透明质酸钠注射治疗膝骨关节炎疗效观察[J].临床心身疾病杂志,2015,21(z1):61.
[21] 涂少龙.关节镜清理术联合药物注射治疗膝关节骨性关节炎的疗效分析[J].骨科,2015,6(1):28-31.
[22] 张卫革,周运勇,唐刚健.关节镜技术配合玻璃酸钠治疗膝骨性关节炎[J].当代医学,2015,21(12):43-44.
[23] 徐昕,董耘,徐华,等.关节镜清理术联合透明质酸钠腔内注射治疗80例高龄膝关节骨性关节炎患者临床分析[J].中华全科医学,2016,14(9):1463-1465.
[24] 柴志勇,李宝军,吴克,等.综合治疗膝骨关节炎216例的临床分析[J].湖南师范大学学报(医学版),2016,13(6):131-133.
[25] 曾伟.关节镜清理术联合透明质酸钠注射液治疗膝关节骨性关节炎的临床疗效观察[J].医学理论与实践,2017,30(2):234-235.
[26] 王刊石,周超,赵磊.关节镜手术联合透明质酸钠对老年膝骨关节炎患者的临床疗效及对关节液内IL-6、IL-1、TNF-α水平的影响[J].中国老年学杂志, 2017, 37(13):3290-3291.
[27] 赵鹏.关节镜下清理术联合透明质酸钠注射治疗膝骨关节炎的效果分析[J].中国医药指南,2017,15(17):105-106.
[28] 吕鹏起.关节镜下关节清理术联合腔内注射SH治疗膝关节骨性关节炎的临床疗效观察[J].健康研究,2018,38(4):452-453,456.
[29] 刘凯.关节镜清理术结合玻璃酸钠注射治疗膝关节骨性关节炎患者的价值[J].医疗装备,2018,31(9):127-128.
[30] 陈万松.关节镜清理术联合玻璃酸钠治疗膝关节骨性关节炎的临床效果[J].甘肃医药,2018,37(9):818-819.
[31] 陈浩城.关节镜下关节清理术联合腔内注射玻璃酸钠治疗膝关节骨性关节炎临床效果及膝关节功能评价[J].陕西医学杂志,2018,47(3):344-346.
[32] 唐国能,黄粹业,蒋永益.关节镜下有限性清理术联合透明质酸钠注射液治疗膝骨性关节炎患者近期疗效分析[J].陕西医学杂志,2018,47(7):896-898.
[33] 孟国华.膝关节镜下清理术联合玻璃酸钠治疗膝关节骨性关节炎的临床价值[J].河南外科学杂志,2018,24(5):141-142.
[34] 步开东,范顺武,翁科迪.关节镜微创手术联合玻璃酸钠治疗对老年膝关节骨性关节炎患者生活质量及血清IL-6、IL-10的影响[J].中国老年学杂志, 2019,39(7): 1637-1639.
[35] 林伟,林任,邱俊钦.关节镜下清理术联合透明质酸钠注射对膝骨性关节炎炎症细胞因子的影响[J].福建医药杂志, 2019, 41(3):82-85.
[36] 贺婧,谭丽,冉彩霞,等.关节镜选择性清理术联合玻璃酸钠注射治疗膝骨性关节炎的疗效观察[J].中国地方病防治杂志, 2019,(4):430-432.
[37] 聂永芳,周晓琼.玻璃酸钠治疗膝骨关节炎的临床疗效[J].临床合理用药杂志, 2019,12(33):71-72.
[38] 王晓亚,任猛,王浩,等.关节镜手术联合透明质酸钠在老年膝骨关节炎治疗的效果及炎性因子的影响[J].河北医药, 2019,41(8):1235-1237.
[39] 唐国能,黄粹业,蒋永益.关节镜下有限性清理术联合透明质酸钠注射液治疗膝骨性关节炎疗效及对患者生活质量的影响[J].陕西医学杂志,2019,48(2):201-204.
[40] MAH, ET, LEE WK, SOUTHWOOD RT, et al. Effects of irrigation fluid on human menisci: an experimental comparison of water, normal saline, and glycine. Arthroscopy. 1991;7(1):24-32.
[41] TEEPLE E, KARAMCHEDU NP, LARSON KM, et al. Arthroscopic irrigation of the bovine stifle joint increases cartilage surface friction and decreases superficial zone lubricin. J Biomech. 2016;49(13):3106-3110.
[42] ALTMAN RD, MANJOO A, FIERLINGER A, et al. The mechanism of action for hyaluronic acid treatment in the osteoarthritic knee: a systematic review. BMC Musculoskelet Disord. 2015;16:321.
[43] GORMELI G, KARAKAPLAN M, GORMELI CA, et al. Clinical effects of platelet-rich plasma and hyaluronic acid as an additional therapy for talar osteochondral lesions treated with microfracture surgery: a prospective randomized clinical trial. Foot Ankle Int. 2015;36(8):891-900.
[44] 宋磊,王腾飞.透明质酸的研究现状综述.山东轻工业学院学报(自然科学版), 2012,26(2):15-18.
[45] BALAZS EA. The physical properties of synovial fluid and the special role of hyaluronic acid. Disorders Knee. 1974;2:61-74.
[46] MORELAND LW. Intra-articular hyaluronan (hyaluronic acid) and hylans for the treatment of osteoarthritis: mechanisms of action. Arthritis Res Ther. 2003;5(2):54-67.
[47] DAY RP. BROOKS P, CONAGHAN G, et al. A double blind, randomized, multicenter, parallel group study of the effectiveness and tolerance of intraarticular hyaluronan in osteoarthritis of the knee. J Rheumatol. 2004;31(4):775-782.
[48] POZO MA, BALAZS EA, BELMONTE C. Reduction of sensory responses to passive movements of inflamed knee joints by hylan, a hyaluronan derivative. Exp Brain Res. 1997;116(1):3-9.
[49] MOORE AR, WILLOUGHBY DA. Hyaluronan as a drug delivery system for diclofenac: a hypothesis for mode of action. Int J Tissue React. 1995;17(4):153-156.
|