中国组织工程研究 ›› 2021, Vol. 25 ›› Issue (10): 1577-1584.doi: 10.3969/j.issn.2095-4344.3024
• 生物材料综述 biomaterial review • 上一篇 下一篇
基于细胞外基质仿生工程心肌构建的研究进展
郭昊宇,李伟权,刘开源,肖瑞芬,孙登龙,席姣娅
- 华中科技大学同济医学院基础医学院生理学系,湖北省武汉市 430030
-
收稿日期:2020-05-13修回日期:2020-05-16接受日期:2020-06-12出版日期:2021-04-08发布日期:2020-12-18 -
通讯作者:席姣娅,博士,副教授,华中科技大学同济医学院基础医学院生理学系,湖北省武汉市 430030 -
作者简介:李伟权,男,1999年生,湖北省武汉市人,汉族,华中科技大学同济医学院在读博士,主要从事心肌组织工程研究。 刘开源,男,1999年生,湖北省仙桃市人,汉族,华中科技大学同济医学院在读博士,主要从事心肌组织工程研究。 -
基金资助:国家自然科学基金项目(31100828);湖北省自然科学基金(2018CFB460):华中科技大学自主创新基金(2017KFYXJJ058,2013TS145);省级大学生创新创业训练计划项目(S201910487157);华中科技大学校级大学生创新创业训练计划项目(2019A0211);华中科技大学校级大学生创新创业训练计划项目(2019A0212)
Recent research progress in construction of biomimetic engineered cardiac tissue based on extracellular matrix
Guo Haoyu, Li Weiquan, Liu Kaiyuan, Xiao Ruifen, Sun Denglong, Xi Jiaoya
- Department of Physiology, School of Basic Medicine, Tongji Medical College, Huazhong University of Science and Technology, Wuhan 430030, Hubei Province, China
-
Received:2020-05-13Revised:2020-05-16Accepted:2020-06-12Online:2021-04-08Published:2020-12-18 -
Contact:Xi Jiaoya, PhD, Associate professor, Department of Physiology, School of Basic Medicine, Tongji Medical College, Huazhong University of Science and Technology, Wuhan 430030, Hubei Province, China -
About author:Li Weiquan, Doctoral candidate, Department of Physiology, School of Basic Medicine, Tongji Medical College, Huazhong University of Science and Technology, Wuhan 430030, Hubei Province, China Liu Kaiyuan, Doctoral candidate, Department of Physiology, School of Basic Medicine, Tongji Medical College, Huazhong University of Science and Technology, Wuhan 430030, Hubei Province, China Guo Haoyu, Li Weiquan and Liu Kaiyuan contributed equally to this paper. -
Supported by:the National Natural Science Foundations of China, No. 31100828; the Natural Science Foundation of Hubei Province, China, No. 2018CFB460; the Fundamental Research Funds for the Central Universities (Huazhong University of Science and Technology), No. 2017KFYXJJ058 and No. 2013TS145; the Provincial Students’ Innovation and Entrepreneurship Training Program of China, No. S201910487157; and the Fundamental Research Funds for the Undergraduates (Huazhong University of Science and Technology), No. 2019A0211 and No. 2019A0212
摘要:
文题释义:
细胞外基质:细胞合成和分泌的大分子物质组成的复杂三维微环境,主要由胶原蛋白、糖胺聚糖、纤维蛋白、弹性蛋白、层粘蛋白和几种其他的糖蛋白组成,能为细胞提供物理支持与适宜微环境,从而诱导细胞黏附、存活、迁移、分化及细胞向特定的形态和功能发育。
工程心肌:将支架聚合物与合适的种子细胞结合起来,构建类似于天然心肌的组织工程,可植入心脏受损区域,替换坏死心肌组织以修复心功能。构建工程心肌的3大基石是合适的支架、合适的种子细胞和合适的构建方法。
背景:细胞外基质及其组成成分构成的贴片、粉末和水凝胶等材料已作为支架,与多种干细胞及其衍生细胞一起被用于构建仿生工程心肌组织。
目的:综述基于细胞外基质的仿生工程心肌构建的研究进展。
方法:应用计算机检索Web of Science Core Collection数据库、PubMed数据库中的相关文献,英文检索词为“the extracellular matrix;engineered cardiac tissue;cardiomyocyte;biomimetic;stem cells”,最终纳入64篇文献进行综述。
结果与结论:与传统的人工合成材料相比,细胞外基质具有良好的生物相容性与细胞亲和力,可为种子细胞提供最接近生物体内的环境,有利于种子细胞的生长、分化与成熟。大量研究证据表明,基于细胞外基质和干细胞的仿生工程心肌具有与天然心肌组织相似的兴奋性、收缩性和传导性等特点,能修复受损心肌、重塑微循环系统,有效改善心功能,具有治疗心肌梗死等心血管疾病的潜力。但基于细胞外基质构建的仿生工程心肌还存在脱细胞过程中结构破坏、种子细胞形态和功能发育相对迟缓等问题。
https://orcid.org/0000-0002-4370-7618 (郭昊宇)
中国组织工程研究杂志出版内容重点:生物材料;骨生物材料; 口腔生物材料; 纳米材料; 缓释材料; 材料相容性;组织工程
中图分类号:
引用本文
郭昊宇, 李伟权, 刘开源, 肖瑞芬, 孙登龙, 席姣娅. 基于细胞外基质仿生工程心肌构建的研究进展[J]. 中国组织工程研究, 2021, 25(10): 1577-1584.
Guo Haoyu, Li Weiquan, Liu Kaiyuan, Xiao Ruifen, Sun Denglong, Xi Jiaoya. Recent research progress in construction of biomimetic engineered cardiac tissue based on extracellular matrix[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(10): 1577-1584.
2.1.1 基于心肌组织来源dECM的仿生工程心肌组织 选用构建仿生工程心肌组织的最佳支架时,从提供最有利于心肌细胞生活的微环境这个角度考虑,心肌组织来源dECM无疑是最接近天然心肌组织微环境的支架材料。研究表明,啮齿类和哺乳类实验动物的心肌组织来源dECM由大量盘绕或排列整齐的胶原蛋白纤维束组成,呈现复杂的多孔网络结构[6,8]。
已有实验证据证实,心肌组织来源dECM支持种子细胞的存活、分化和成熟。LU等[16]报道心肌组织来源dECM能促进人源诱导多能干细胞来源的心血管祖细胞向心肌细胞、平滑肌细胞和内皮细胞分化。BLAZESKI等[9]报道了大鼠心肌组织来源dECM可以促进新生大鼠心室肌细胞呈长杆状有序生长和排列,促进细胞间形成电偶联,有利于构建可同步收缩的具有合胞体性质的工程心肌组织。AN等[8]将小鼠心房肌制备为心肌组织来源dECM,与从新生小鼠右心房分离出来的心房肌、窦房结、成纤维细胞等多种细胞按天然比例共培养,研究心肌组织来源dECM对不同细胞生存和生长的影响及可能机制。他们发现心肌组织来源dECM可促进心房肌细胞和窦房结细胞的增殖,抑制成纤维细胞的增殖,共培养2 d后,工程心肌组织中这两种细胞的比例明显增加,工程心肌组织的动作电位强度明显升高;心房组织来源dECM中存在外泌体,后者可以在氧化应激条件下释放miR-199a-3p,miR-199a-3p通过抑制HOPX蛋白的表达促进GATA-4乙酰化,从而促进心房肌细胞和窦房结细胞的增殖。
研究者们发现心肌组织来源dECM移植对心脏的结构和功能均有修复作用。YOSHIZUMI等[17]报道,将心肌组织来源dECM片移植至大鼠心肌梗死模型后可以显著减小左心室舒张末期和收缩末期面积,增加面积变化分数,明显增加左心室前壁厚度,显著提高左心室顺应性。2016年,SARIG等[18]进行了一项类似的研究,观察猪心肌组织来源dECM片对大鼠急性和慢性心肌梗死模型的疗效,在急性心肌梗死模型中,左前降支结扎后立即缝合心肌组织来源dECM;在慢性心肌梗死模型中,心肌组织来源dECM在心肌梗死后30 d即瘢痕组织形成后被缝合。治疗30 d后两种模型梗死面积显著减小,左心室内径显著减小,左心室射血分数增加;梗死区域病理评估显示,GATA4、C-Kit、MYLC和/或TrpI染色阳性的细胞数量呈时间依赖性增加,表明梗死区域微环境显著改善。POK等[19]研究了猪源心肌组织来源dECM对大鼠右心室流出道缺陷的修复作用,发现移植基于心肌组织来源dECM的混合支架4周后可整合入宿主心肌组织中,移植8周后可见心肌组织来源dECM片降解、变薄的同时呈现红、黄色外观,提示心肌组织来源dECM移植区有血管结构形成,更有利于组织再生;MRI结果提示,心肌组织来源dECM移植8周后左、右心室舒张末期容积显著增加,但并未观察到左、右心室射血分数明显改善;移植后心肌组织来源dECM导致M2/M1炎症巨噬细胞比例升高,可能参与介导前述现象的发生。
研究发现基于心肌组织来源dECM的工程心肌组织,在动物实验中对受损心脏结构与功能的修复作用较心肌组织来源dECM更为显著。WANG等[20]将整个大鼠心脏脱细胞化,然后切成心内膜和心外膜表面完整的薄片,在每张薄片的心内膜表面以104/mm2的密度接种含75%人源诱导多能干细胞来源的心肌细胞和25%人源诱导多能干细胞来源的非心肌细胞(CD90+细胞)的混合细胞。制作大鼠心肌梗死模型,结扎左前降支后立即将工程心肌组织贴于梗死区域,使种植细胞的一面紧贴心脏,2周后与心肌组织来源dECM处理组相比,工程心肌组织处理大鼠的左心室射血分数明显增加,缩短分数更高,收缩和舒张期左心室内径更小;4周后的组织学检查显示,与心肌组织来源dECM处理组相比,工程心肌组织处理心脏后梗死面积明显缩小,血管密度明显增高。
受伦理学限制,目前有关人源心肌组织来源dECM的研究极少。GUYETTE等[21]将捐自新英格兰器官库的、不能用于器官移植的人心脏制备成心肌组织来源dECM,再将其与人源诱导多能干细胞来源的心肌细胞共培养,发现共培养4-7 d内形成能自发收缩的工程心肌组织,共培养14 d后工程心肌组织能应答外源性电刺激发生兴奋和收缩,且其产生的场电位时程、收缩力和收缩速度均与成年心肌相似。尽管心肌组织来源dECM被认为是极富潜力的支架材料来源之一,但由于来源短缺限制了它的应用。此外,心肌组织来源dECM的抗伸展性和机械性能较差,这可能降低其构建工程心肌组织的机械性能,需要加入修饰材料进一步改进材料的特性。
2.1.2 基于ncECM固体支架的仿生工程心肌组织 目前报道的ncECM类型主要包括小肠黏膜下层组织细胞外基质、心包组织细胞外基质、膀胱细胞外基质、骨骼肌细胞外基质,这4种ncECM取材方便,更易实现患者自体取材,可避免异体或异种细胞外基质或者工程心肌组织移植带来的排斥反应。研究表明,移植ncECM或基于ncECM的工程心肌组织也可显著改善心功能,可作为替代心肌组织来源dECM的支架材料。
基于动物心肌梗死模型的研究证实,ncECM和基于ncECM的工程心肌组织可不同程度地修复受损心肌,改善心功能和梗死区域微环境。MEWHORT等[13]将小肠黏膜下层组织细胞外基质片直接缝合于猪冠状动脉缺血梗死区的心外膜,6周后观察到实验组心壁增厚至(28.6±14.0)%,明显高于假手术组的(4.2±13.5)%;相比假手术组,接受小肠黏膜下层组织细胞外基质片的梗死区微毛细血管和微动脉密度明显增加,同时心脏形变能力并没有降低,提示梗死区微环境明显改善。WANG等[14]将小鼠胚胎isl1+心脏祖细胞接种到小肠黏膜下层组织细胞外基质中构建工程心肌组织,体外培养7 d后再将工程心肌组织移植到小鼠心肌梗死模型中,移植4周后可见有活性的工程心肌组织紧贴宿主心肌表面,瘢痕面积显著减小;相比假手术组,左心室射血分数明显提高、左心室缩短率显著提高、左心室舒张末期内径和收缩末期内径明显减小,提示心功能显著改善。
心包是覆盖在心脏表面的膜性囊,内含丰富的基质蛋白成分。GáLVEZ-MONTóN等[22]用人源心包组织细胞外基质和猪脂肪祖细胞制成工程心肌组织植入猪心肌梗死模型的梗死区,发现移植1个月后左室射血分数明显提高,梗死面积和炎症发生率显著降低。
REMLINGER等[15]在大鼠RVOT defeat模型上对比研究了膀胱细胞外基质与心肌组织来源dECM移植对心脏结构和功能的影响,发现两种细胞外基质均能促进细胞浸润,降低病理性纤维包裹,显著修复心室壁结构;膀胱细胞外基质诱导宿主细胞迁移、浸润的能力更强,并促进移植区心肌细胞肌动蛋白表达,这将显著改善宿主心功能。
骨骼肌和心肌同属横纹肌,取材方便。作者所在课题组前期观察了骨骼肌细胞外基质对小鼠胚胎干细胞黏附、生存、增殖和心肌分化状态的影响,发现骨骼肌细胞外基质比心肌组织来源dECM更适合小鼠胚胎干细胞的黏附、存活、增殖,并支持小鼠胚胎干细胞向心肌组织的正常分化;在共培养14 d可获得能节律性兴奋和收缩的心肌样组织[6]。
2.1.3 基于细胞外基质水凝胶材料的仿生工程心肌组织 水凝胶作为经典的人工合成支架材料,由dECM经冻干、研磨、消化等处理后形成,可以被设计成特定的形状。由于水凝胶是由亲水聚合物组成的三维交联网络,吸收大量水后可以形成溶胀但不溶于水的交联基质,因此具有优良的组织相容性与扩散特性[23],可以包裹细胞成分和其他生物材料,可精准注射并长期固着于梗死区,有助于修复心功能。
现有研究表明,基于心肌组织来源dECM的水凝胶在改善微环境机械性能、提高材料生物相容性和促进血管形成等方面有明显作用。EFRAIM 等[7]用猪源心肌组织来源dECM、京尼平和壳聚糖制成水凝胶,并将人源间充质干细胞与水凝胶(每100 μL水凝胶内接种75 000个细胞)制成工程心肌组织,将其注入后大鼠心肌梗死区4周后左心室射血分数与对照组的42%相比增加了20%。STOPPEL等[24-25]用丝素蛋白和猪源心肌组织来源dECM制成具有可调力学性能的水凝胶,可促进心脏成纤维细胞的黏附、生长和迁移。此外,他们还将该水凝胶负载心脏成纤维细胞后注入心肌梗死模型的梗死区,发现其有助于局部血管化,改善梗死区域微环境。SEIF-NARAGHI等[26]也报道猪源心肌组织来源dECM水凝胶对大鼠心外膜细胞、人冠状动脉内皮细胞和大鼠主动脉平滑肌细胞均具有明显趋化作用,可促进血管形成。
由于基于心肌组织来源dECM水凝胶来源的短缺及临床应用的限制,有研究者也尝试用基于ncECM水凝胶构建工程心肌组织,并发现其能够明显改善受损心肌细胞微环境,促进血管生成。KIM等[27]发现可注射性小肠黏膜下层组织细胞外基质水凝胶可以促进大鼠肌源性干细胞的吸附和增殖,负载细胞后注射至大鼠皮下可明显诱导血管的新生和生长,并有效抑制巨噬细胞介导的炎症反应。SEIF-NARAGHI等[26]发现与心肌组织来源dECM水凝胶相比,猪源心包组织细胞外基质水凝胶对大鼠心外膜细胞、人冠状动脉内皮细胞和大鼠主动脉平滑肌细胞具有更强的趋化作用,提示其更有利于血管形成。
2.2 基于细胞外基质组分的仿生工程心肌组织 细胞外基质中富含胶原蛋白、纤连蛋白、糖胺聚糖等,构成了各向异性的复杂网络结构,在维持心室几何形状与传导性方面起着重要作用[10]。针对研究者的不同需求,可以选用特定的一种或几种组分构建工程心肌组织支架。根据构建工程心肌组织时所用的组分,可以将工程支架分为以下4类。
2.2.1 基于胶原蛋白的仿生工程心肌组织 心肌组织来源细胞外基质的主要成分是纤维胶原,故胶原蛋白常被用作工程心肌组织支架的生物材料[28],用于构建具有类似天然结构的功能性工程心肌组织。WANG等[29]用猪腱制备脱细胞胶原薄膜,将人源诱导多能干细胞来源心肌细胞接种在该胶原膜上,可形成有序的纤维状、能自发收缩的工程心肌组织;共培养4周后,异丙肾上腺素处理能增加工程心肌组织的跳动频率与收缩幅度增加。该结果提示基于胶原蛋白的工程心肌组织可用于药物筛选和药物毒性研究。
进一步研究发现,在合成支架时加入胶原蛋白有助于提高工程心肌组织的仿生性。ZHANG等[30]将胶原蛋白加入基质胶和聚二甲基硅氧烷中作为支架材料,接种人胚胎干细胞来源心肌细胞、人皮肤来源成纤维细胞和人骨髓来源间充质干细胞构建工程心肌组织,共培养2周后观察到人胚胎干细胞来源心肌细胞中出现了成熟的肌节结构,这将改善工程心肌组织的收缩能力。
综上所述,以胶原蛋白为原料构建的工程心肌组织,具有使心肌细胞的细胞内结构和细胞间排列趋向成熟的作用。
2.2.2 基于纤维蛋白的仿生工程心肌组织 纤维蛋白具有良好的组织相容性和能够大规模稳定生产的特性,方便制备结构稳定的支架材料,在现有研究中被广泛用于工程心肌组织的构建。
SIDOROV等[31]用纤维蛋白原凝胶、凝血酶与新生大鼠心肌细胞构建工程心肌组织,发现共培养10-12 d后的心肌细胞呈细长柱状,具有成熟的肌节结构,说明心肌细胞的结构趋向成熟。JACKMAN等[32]在纤维蛋白支架中注入大鼠心室肌细胞并动态培养2周,发现心肌细胞电生理功能与收缩功能相关基因(如L-型钙通道基因、肌球蛋白重链基因等)表达量均有提高。WANG等[33]以纤维蛋白装载新生大鼠心室肌细胞制成水凝胶,并通过生物打印技术构建出线状或片状结构,共培养3周后发现心肌细胞可以同步收缩,并在肾上腺素作用下搏动频率与收缩力显著增加,与天然心肌细胞反应类似。上述结果说明以纤维蛋白为支架材料的工程心肌组织可以促进心肌细胞的电生理特性与收缩功能明显改善,提高心肌细胞的仿生性。
除此之外,以纤维蛋白为原料构建的工程心肌组织能促进受损心脏的功能恢复。MENASCHé等[34]用纤维蛋白和人胚胎干细胞来源心肌祖细胞构建工程心肌组织,将其移植到心肌梗死大鼠心脏梗死区域,2周后观察到工程心肌组织移植组左心室射血分数相比假手术组明显升高,提示心肌梗死大鼠的心脏功能得到明显改善。
2.2.3 基于透明质酸的仿生工程心肌组织 透明质酸是细胞外基质中介导细胞信号传导、损伤修复和细胞骨架组装的重要成分,具有良好的生物相容性、生物降解性和非免疫原性特性[35]。以透明质酸为支架构建的工程心肌组织可以用于促进心肌细胞的成熟,延缓受损心肌中的病理性重构过程。GAETANI等[36]用来自于外科手术组织的人源心肌祖细胞为种子细胞、以明胶与透明质酸为基质构建工程心肌组织,植入心肌梗死模型小鼠的心室壁上,1个月后发现移植的心肌祖细胞开始出现进一步分化,并出现了肌节结构与缝隙连接结构,说明心肌祖细胞分化的心肌细胞的表型成熟;实验组小鼠植入工程心肌组织部位的室壁厚度明显增加,梗死区域纤维化的程度显著下降,标志心室重构的延缓与心功能的恢复。
2.2.4 基于多种细胞外基质成分和加入其他成分修饰的仿生工程心肌组织 除了上述成分,细胞外基质中还存在一些特殊的成分,如基底膜基质(基质胶)与聚集蛋白等,也可以起到促进心肌细胞结构与功能的成熟与修复创伤的作用。
基质胶内富含层粘连蛋白和胶原蛋白,可模拟体内细胞基底膜的结构、组成、物理特性和功能,有利于体外细胞的培养和分化。FEASTER等[37]将基质胶均匀排列成多条并行的胶垫,并接种人源诱导多能干细胞来源的心肌细胞,共培养5-7 d后几乎所有的人源诱导多能干细胞来源心肌细胞均可明显自发收缩并呈现出细胞伸长、圆形度降低与肌节长度的增加,标志着人源诱导多能干细胞来源心肌细胞结构的成熟;此外,加入肌丝钙敏化剂后工程心肌组织收缩力明显增强,说明该方法构建的心肌组织在药物实验和心脏毒性评估方面有潜在应用价值。
聚集蛋白可以使细胞分化程度降低,提高细胞增殖能力进而促进心脏修复。BASSAT等[38]发现,在心肌梗死小鼠心肌中注射聚集蛋白可以使心脏瘢痕面积与注射磷酸盐缓冲液的对照组相比显著减少。类似的结果在以3D培养的人源诱导多能干细胞来源心肌细胞为种子细胞的工程心肌组织组织中也有发现:与对照组相比,工程心肌组织中的心肌细胞成熟标志物表达降低、周期活性蛋白表达增强,提示心肌细胞的增殖能力的恢复,揭示了聚集蛋白在心脏修复过程中的重要作用。
虽然天然水凝胶可以促进心肌细胞的分化与成熟,但由于其机械性能和结构支撑能力较弱,研究人员常在天然细胞外基质组分中加入其他成分构成混合生物材料,既可保留天然支架固有的生物组分又能赋予支架材料优良的机械性能,能够有效促进心肌细胞结构与功能的成熟,形成具有稳定收缩能力的工程心肌组织。ROSHANBINFAR等[39]以聚乙二醇-纤维蛋白原为原料、人源诱导多能干细胞为种子细胞制成工程心肌组织水凝胶,分化第14天时观察到工程心肌组织基本均匀收缩,第24天时观察到人源诱导多能干细胞来源心肌细胞有明显的肌节与横小管结构形成,标志着心肌细胞的成熟。SUN等[40]用碳纳米管与胶原蛋白为原料制备了工程心肌组织复合水凝胶,并注入大鼠心室肌细胞,发现共培养7 d后的心室肌细胞具有更成熟的肌节结构,工程心肌组织的自发搏动频率相比于纯胶原蛋白的对照组显著增加。
除此以外,对天然生物材料进行化学修饰,可以使保留在移植区域内的细胞比例增加,促进心肌修复。 CHAN等[41]对透明质酸羧基端进行了化学修饰,将其与血清交联制成透明质酸-血清水凝胶后植入大鼠心球来源的心肌祖细胞、间充质干细胞与内皮细胞制成工程心肌组织水凝胶,发现在心肌中注射该水凝胶可增加干细胞在注射区域的增殖速率与保留率;在大鼠心肌梗死模型中,注射此透明质酸-血清水凝胶可使左心室射血分数增加,并促进血管的形成,改善梗死区域的功能。
2.3 基于人工合成材料的仿生工程心肌组织 天然细胞外基质来源受限,且性能不能完全满足仿生工程心肌组织构建的需求。以天然细胞外基质为基础加入其他修饰成分构建而成的人工合成支架材料,不仅保留了天然细胞外基质的结构和功能特点,而且机械性能优良、获得方便、可大量制备,被广泛应用于新一代工程心肌组织的构建中。
2.3.1 基于掺入修饰材料的复合水凝胶仿生工程心肌组织 水凝胶可以通过添加多种修饰成分来模拟天然组织理化特性,提高工程心肌组织各种生理特性与成熟心肌组织的相似度,有利于提高工程心肌组织受体心脏的心功能。WANG等[42]通过向透明质酸水凝胶中加入硫醇化基团并加入导电交联剂四苯胺-聚乙二醇二丙烯酸酯,原位加成得到了一种可导电的新型水凝胶材料,具有与天然心肌组织等同的传导性。将其与改造过的脂肪来源干细胞混合注射到SD大鼠心肌梗死区内后心脏整体mRNA表达谱中翻译内皮型一氧化氮合酶、收缩蛋白、促血管生长因子等与心功能相关的mRNA表达水平明显上升,且梗死面积缩小,QT间期延长等心律失常表现得到缓解,提示受体心功能恢复。此外,血清白蛋白[43]、壳聚糖-胸腺素等多种修饰成分也被报道用于工程心肌组织的构建中[44],通过改善材料的机械性能和与种子细胞的相互作用提高种子细胞的成熟度,提高对损伤心肌的修补能力。
碳纳米管、石墨烯、氧化石墨烯等新型纳米材料也可作为水凝胶构建时的修饰成分,促进种子细胞的存活、迁移和增殖及电信号的传导,进而改善心功能。ZHU等[45]将金纳米棒按实验测得的最佳浓度掺入明胶甲基丙烯酸酯水凝胶中,得到了弹性模量低于正常人心肌组织、表面比单纯明胶甲基丙烯酸酯更粗糙的水凝胶。作者推测较低的弹性模量有利于工程心肌组织内心肌细胞的整体收缩,进而促进水凝胶包裹心肌细胞,粗糙的表面还可以更好地黏附细胞,提高种子细胞的存活率,并通过凸出的金颗粒与细胞膜接触进行电传导,提高了工程心肌组织收缩的同步性。SHIN等[46-47]将新生大鼠心肌细胞分散在掺入了氧化石墨烯的明胶甲基丙烯酸酯水凝胶中,经紫外线照射交联制成工程心肌组织贴片,发现与掺入氧化石墨烯前相比,这种新型水凝胶不仅在弹性模量、电导率和生物相容性等方面更接近成熟心肌组织,并且由于纳米材料对基质蛋白质有很强的吸附力,明胶甲基丙烯酸酯本身的多孔性和可降解性也可以得到完整保留。活死细胞染色结果提示新材料促进了种子细胞的黏附、迁移和增殖,而且有利于提高细胞的存活率。ZHOU等[48]通过向大鼠心脏梗死区注射含有氧化石墨烯纳米颗粒的低聚聚乙二醇-富马酸酯水凝胶发现,氧化石墨烯增加了水凝胶的传导性,提高了细胞的黏附性,进而增强了心脏内正常心肌组织与瘢痕区心肌细胞之间的电偶联,使心脏射血分数上升,泵血功能改善。
修饰成分的引入还能够降低由水凝胶引起的组织炎症和免疫反应。由于水凝胶为网状交联结构的凝胶,在体内降解性差,长时间植入常引起慢性炎症细胞浸润和肉芽肿等免疫反应,与周围细胞相容性不佳。对此 WANG等[42]构建了由纳米药物强化的活性氧敏感可注射水凝胶,明显提高了水凝胶在体内的降解性和可吸收性,并通过纳米药物颗粒抑制了白细胞中炎症因子的表达,降低了炎症反应对组织的进一步破坏,抑制了梗死区域的扩大。
此外,在优化工程心肌组织各种细胞的比例结构、提高心肌细胞内收缩相关蛋白和缝隙连接蛋白等功能蛋白的表达量等方面,修饰成分也可以起到一定作用[45]。
2.3.2 基于3D打印细胞外基质立体支架的仿生工程心肌组织 上述的培养方式多为平面支架培养,相比之下立体支架培养通过模拟天然细胞外基质的三维结构,控制细胞的间距和排列方向,有助于促进组织和细胞结构功能成熟[2,49-51]。这些作用的机制表现在多个方面:①首先,细胞外基质的结构与细胞之间存在多种细胞-基质相互作用,进而介导和激活不同的细胞内信号通路。②此外,相比于传统的平面培养,3D支架材料能够从3个维度为细胞提供信号刺激,促进心肌细胞功能和结构的发育成熟。ZHANG等[52]发现,规则地接种在纤维蛋白制成的3D支架中的人胚胎干细胞来源心肌细胞动作电位传导速度可以达到(9.76±1.0)cm/s,高于对照组的 (5.17±0.7)cm/s;cTnT、MLC2v等收缩相关蛋白的表达水平更高,肌节长度等反映肌节发育程度的结构特性更接近成熟心肌;编码缝隙连接蛋白、钠钾通道蛋白、兴奋收缩耦联相关蛋白(肌浆网钙泵蛋白等)等兴奋和传导功能相关基因表达增加,表征分化程度低的Oct4、Nanog表达量下降,转录因子GATA4和ISL1等心肌特异性标志物表达上升。③第三,正常心脏中工作肌细胞、血管内皮细胞等各种组织细胞在排列上有各向异性,使心肌可以协同收缩,形成精细排列的微循环血管,持续供应工作细胞需要的营养,迅速移除代谢产物,有利于心脏高效完成泵血功能。
随着3D打印技术分辨率的大幅提高,研究者可以通过扫描天然细胞外基质的精细结构或者预先设计所需的立体支架结构图,通过3D打印方式生成所需支架材料,再植入种子细胞生成工程心肌组织;或者可以直接将种子细胞和支架材料水凝胶混匀后按设计结构3D打印成工程心肌组织,高精度地模仿心脏的天然三维结构,进而控制工作肌细胞间的排列方向和营养血管的走行,提高工程心肌组织的传导、收缩功能,改善细胞的局部微环境。ZHANG等[53]通过用3D打印机在单轴拉伸薄片上以35 μm的间距打孔并将多张薄片叠放成立体支架,制成了可以用于控制植入人源间充质干细胞方向性的仿细胞外基质结构支架。BEJLERI等[54]以明胶甲基丙烯酸酯、藻酸盐、光引发剂等为原料制成了“生物油墨”,并向其中混入了人脐静脉内皮细胞,3D打印制成微纤维支架,形成了按设计走行的管状的血管样组织。与之类似,MAIULLARI等[55]将人脐静脉内皮细胞和多能诱导干细胞源心肌细胞包封在含有藻酸盐和聚乙二醇-纤维蛋白原的水凝胶中并通过定制的微流体印刷头挤出,精确控制其3D空间沉积位置的方法,能够保证所构建3D心脏组织的高保真度和分辨率,并可以控制人脐静脉内皮细胞产生血管样结构的几何形状和方向。GAO等[56]以天然细胞外基质结构扫描图为模板,使用多光子激发的3D打印制作出了一种亚微米分辨率的仿生细胞外基质支架,并将人源诱导多能干细胞来源的心肌细胞、内皮细胞和平滑肌细胞按2∶1∶1的比例混入支架中制成心肌贴片,植入大鼠心肌梗死模型的梗死区内,发现支架可以使内皮细胞和平滑肌细胞在特定位置组装成微血管,并控制血管的走行方向和分布范围,改善了梗死周围区残存心肌细胞的微环境,也提高了注入人源诱导多能干细胞来源心肌细胞的存活率,同时未引起心律失常等移植常见问题。值得一提的是,2018年GAO等[57]继续优化了此研究的实验对象和适用范围,将上述3种细胞植入纤维蛋白支架材料中并制成了适用于临床规格大小(4 cm×2 cm×1.25 mm)的心肌贴片,应用于与人类心脏大小、同源性等更相近的猪心肌梗死模型中,取得了类似的结果,为3D打印支架在临床中的应用提供了研究基础。2019年,以色列科学家用3D打印按正常心脏内部的结构组成成功打印出了肌肉层、血管网等与正常心脏一致的完整的人工心脏,具有同步收缩的特性[49],其中用到的各种细胞均来源于患者的网膜组织细胞诱导成的人源诱导多能干细胞。这无疑是3D打印在工程心肌组织临床应用研究中的又一重大突破。
2.3.3 基于其他人工合成材料的仿生工程心肌组织 如何在工程心肌组织与受体心脏之间建立血管联系是近年来研究的热点之一,一些具有独特性质的新型材料和方法为解决此问题提供了新思路。SAKAGUCHI等[58]分别基于生物反应器或温度反应性培养体系构建出了新型工程心肌组织片,片与片之间用明胶水凝胶粘连,构成了一种能使受体的微血管长入其内部的工程心肌组织片,并可以通过添加不同量的聚合物、改变片与片之间的结构和厚度等方法来控制血管床的方向。
此外,由于心肌梗死后形成的瘢痕导电性差,使得相邻心肌细胞之间的电偶联被破坏,移植物与心肌细胞也难以建立稳定的电偶联结构是阻碍工程心肌组织应用的难题,人工合成材料的出现可以帮助工程心肌组织与受体之间达到兴奋收缩同步,使两者形成功能合胞体。SARAVANAN等[59]通过将氧化石墨烯-金纳米片掺入天然壳聚糖聚合物中合成出一种导电性良好、多孔隙、可降解的支架(不含外源细胞成分),可供受体自身的心肌细胞附着,与金颗粒接触,间接与工程心肌组织中的种子细胞接触,完成工程心肌组织与受体之间的电传导。此外,SHIN等[47]和ZHOU等[48]通过应用氧化石墨烯作为添加剂建立工程心肌组织与宿主心肌细胞之间的电偶联结构,也可以显着改善心肌的电活动,传导性和同步收缩性。

| [1] VALLS-MARGARIT M, IGLESIAS-GARCÍA O, DI GUGLIELMO C, et al. Engineered Macroscale Cardiac Constructs Elicit Human Myocardial Tissue-like Functionality. Stem Cell Reports. 2019;13(1): 207-220. [2] ALONZO M, ANILKUMAR S, ROMAN B, et al. 3D Bioprinting of cardiac tissue and cardiac stem cell therapy. Transl Res. 2019;211:64-83. [3] GOLDFRACHT I, PROTZE S, SHITI A, et al. Generating ring-shaped engineered heart tissues from ventricular and atrial human pluripotent stem cell-derived cardiomyocytes. Nat Commun. 2020;11(1):75. [4] THEOCHARIS AD, SKANDALIS SS, GIALELI C, et al. Extracellular matrix structure. Adv Drug Deliv Rev. 2016;97:4-27. [5] 姜煜东,李文思,尹盟盟,等.心肌ECM研究进展:心肌ECM的获取、评价、和改造[J].生理学研究,2013,1(1):1-6. [6] HONG X, YUAN Y, SUN X, et al. Skeletal Extracellular Matrix Supports Cardiac Differentiation of Embryonic Stem Cells: A Potential Scaffold for Engineered Cardiac Tissue. Cell Physiol Biochem. 2018;45(1): 319-331. [7] EFRAIM Y, SARIG H, COHEN ANAVY N, et al. Biohybrid cardiac ECM-based hydrogels improve long term cardiac function post myocardial infarction. Acta Biomater. 2017;50:220-233. [8] AN M, KWON K, PARK J, et al. Extracellular matrix-derived extracellular vesicles promote cardiomyocyte growth and electrical activity in engineered cardiac atria. Biomaterials. 2017;146:49-59. [9] BLAZESKI A, KOSTECKI GM, TUNG L. Engineered heart slices for electrophysiological and contractile studies. Biomaterials. 2015;55:119-128. [10] FRANGOGIANNIS NG. The extracellular matrix in myocardial injury, repair, and remodeling Find the latest version : The extracellular matrix in myocardial injury , repair, and remodeling. J Cllin Invest. 2017;127(5): 1600-1612. [11] GOLDFRACHT I, EFRAIM Y, SHINNAWI R, et al. Engineered heart tissue models from hiPSC-derived cardiomyocytes and cardiac ECM for disease modeling and drug testing applications. Acta Biomater. 2019;92(5):145-159. [12] TOEG HD, TIWARI-PANDEY R, SEYMOUR R, et al. Injectable small intestine submucosal extracellular matrix in an acute myocardial infarction model. Ann Thorac Surg. 2013;96(5): 1686-1694. [13] MEWHORT HEM, TURNBULL JD, SATRIANO A, et al. Epicardial infarct repair with bioinductive extracellular matrix promotes vasculogenesis and myocardial recovery. J Hear Lung Transplant. 2016;35(5): 661-670. [14] WANG L, MEIER EM, TIAN S, et al. Transplantation of Isl1+ cardiac progenitor cells in small intestinal submucosa improves infarcted heart function. Stem Cell Res Ther. 2017;8(1): 1-10. [15] REMLINGER NT, GILBERT TW, YOSHIDA M, et al. Urinary bladder matrix promotes site appropriate tissue formation following right ventricle outflow tract repair. Organogenesis. 2013;9(3): 215-226. [16] LU TY, LIN B, KIM J, et al. Repopulation of decellularized mouse heart with human induced pluripotent stem cell-derived cardiovascular progenitor cells. Nat Commun. 2013;4:2307. [17] YOSHIZUMI T, ZHU Y, JIANG H, et al. Timing effect of intramyocardial hydrogel injection for positively impacting left ventricular remodeling after myocardial infarction. Biomaterials. 2016;83:182-193. [18] SARIG U, SARIG H, DE-BERARDINIS E, et al. Natural myocardial ECM patch drives cardiac progenitor based restoration even after scarring. Acta Biomater. 2016;44:209-220. [19] POK S, STUPIN I V, TSAO C, et al. Full Thickness Heart Repair with an Engineered Multilayered Myocardial Patch in Rat Model. Adv Heal Mater. 2017;6(5): 1-12. [20] WANG Q, YANG H, BAI A, et al. Functional engineered human cardiac patches prepared from nature’s platform improve heart function after acute myocardial infarction. Biomaterials. 2016;105:52-65. [21] GUYETTE JP, CHAREST JM, MILLS RW, et al. Bioengineering Human Myocardium on Native Extracellular Matrix. Circ Res. 2016;118(1): 56-72. [22] GÁLVEZ-MONTÓN C, BRAGÓS R, SOLER-BOTIJA C, et al. Noninvasive Assessment of an Engineered Bioactive Graft in Myocardial Infarction: Impact on Cardiac Function and Scar Healing. Stem Cells Transl Med. 2017; 6(2): 647-655. [23] SALUDAS L, PASCUAL-GIL S, PRÓSPER F, et al. Hydrogel based approaches for cardiac tissue engineering. Int J Pharm. 2017;523(2): 454-475. [24] STOPPEL WL, HU D, DOMIAN IJ, et al. Anisotropic silk biomaterials containing cardiac extracellular matrix for cardiac tissue engineering. Biomed Mater. 2015;10(3):034105. [25] STOPPEL WL, GAO AE, GREANEY AM, et al. Elastic, silk-cardiac extracellular matrix hydrogels exhibit time- dependent stiffening that modulates cardiac fibroblast response. J Biomed Mater Res A. 2016;104(12): 3058-3072. [26] SEIF-NARAGHI SB, HORN D, SCHUP-MAGOFFIN P, et al. Patient-to-patient variability in autologous pericardial matrix scaffolds for cardiac repair. J Cardiovasc Transl Res. 2012;4(5): 545-556. [27] KIM K, KIM MS. An injectable hydrogel derived from small intestine submucosa as a stem cell carrier. J Biomed Mater Res B Appl Biomater. 2016;104(8):1544-1550. [28] HORN MA, TRAFFORD AW. Aging and the cardiac collagen matrix: Novel mediators of fibrotic remodelling.J Mol Cell Cardiol. 2016;93:175-185. [29] WANG L, ZHANG X, XU C, et al. Human induced pluripotent stem cell-derived cardiac tissue on a thin collagen membrane with natural microstructures. Biomater Sci. 2016;4(11): 1655-1662. [30] ZHANG W, KONG CW, TONG MH, et al. Maturation of human embryonic stem cell-derived cardiomyocytes (hESC-CMs) in 3D collagen matrix: Effects of niche cell supplementation and mechanical stimulation. Acta Biomater. 2017;49:204-217. [31] SIDOROV VY, SAMSON PC, SIDOROVA TN, et al. I-Wire Heart-on-a-Chip I: Three-dimensional cardiac tissue constructs for physiology and pharmacology. Acta Biomater. 2017;48: 68-78. [32] JACKMAN CP, CARLSON AL, BURSAC N. Dynamic culture yields engineered myocardium with near-adult functional output. Biomaterials. 2016;111: 66-79. [33] WANG Z, LEE SJ, CHENG H, et al. 3D Bioprinted Functional and Contractile Cardiac Tissue Constructs Wake Forest Institute for Regenerative Medicine Wake Forest School of Medicine. Acta Biomater. 2018;70:48-56. [34] MENASCHÉ P, VANNEAUX V, FABREGUETTES JR, et al. Towards a clinical use of human embryonic stem cell-derived cardiac progenitors: A translational experience. Eur Heart J. 2015;36(12):743-750. [35] GALLAGHER LB, DOLAN EB, O’SULLIVAN J, et al. Pre-culture of mesenchymal stem cells within RGD-modified hyaluronic acid hydrogel improves their resilience to ischaemic conditions. Acta Biomater. 2020;107:78-90. [36] GAETANI R, FEYEN DAM, VERHAGE V, et al. Epicardial application of cardiac progenitor cells in a 3D-printed gelatin/hyaluronic acid patch preserves cardiac function after myocardial infarction. Biomaterials. 2015;61:339-348. [37] FEASTER TK, CADAR AG, WANG L, et al. Matrigel Mattress: A Method for the Generation of Single Contracting Human-Induced Pluripotent Stem Cell-Derived Cardiomyocytes. Circ Res. 2015;117(12): 995-1000. [38] BASSAT E, MUTLAK YE, GENZELINAKH A, et al. The extracellular matrix protein agrin promotes heart regeneration in mice Elad. Nature. 2017; 547(7662): 179-184. [39] ROSHANBINFAR K, MOHAMMADI Z, SHEIKH-MAHDI MESGAR A, et al. Carbon nanotube doped pericardial matrix derived electroconductive biohybrid hydrogel for cardiac tissue engineering. Biomater Sci. 2019;7(9): 3906-3917. [40] SUN H, ZHOU J, HUANG Z, et al. Carbon Nanotube-Incorporated Collagen Hydrogels Improve Cell Alignment and the Performance of Cardiac Constructs. Int J Nanomedicine. 2017;12:3109-3120. [41] CHAN AT, KARAKAS MF, STYLIANI V, et al. Hyaluronic Acid-Serum Hydrogels Rapidly Restore Metabolism of Encapsulated Stem Cells and Promote Engraftment. Biomaterials.2015;73(24): 1-11. [42] WANG W, TAN B, CHEN J, et al. An injectable conductive hydrogel encapsulating plasmid DNA-eNOs and ADSCs for treating myocardial infarction. Biomaterials.2018;16:69-81. [43] THOMAS MR, SKAALURE SC, RICHARDSON RM, et al. Elastic serum-albumin based hydrogels: mechanism of formation and application in cardiac tissue engineering. J Mater Chem B. 2018;6(35): 5604-5612. [44] SHAGHIERA A, WIDIYANTI P, YUSUF H. Synthesis and Characterization of Injectable Hydrogels with Varying Collagen-Chitosan-Thymosin β4 Composition for Myocardial Infarction Therapy. J. Funct Biomater. 2018;9(2):33. [45] ZHU K, SHIN SR, Van KEMPEN T, et al. Gold Nanocomposite Bioink for Printing 3D Cardiac Constructs. Adv Funct Mater. 2017;27(12):1605352. [46] SHIN SR, JUNG SM, ZALABANY M, et al. Carbon-nanotube-embedded hydrogel sheets for engineering cardiac constructs and bioactuators. ACS Nano. 2013;7(3): 2369-2380. [47] SHIN SR, AGHAEI-GHAREH-BOLAGH B, DANG TT, et al. Cell-laden microengineered and mechanically tunable hybrid hydrogels of gelatin and graphene oxide. Adv Mater. 2013;25(44): 6385-6391. [48] ZHOU J, YANG X, LIU W, et al. Injectable OPF/graphene oxide hydrogels provide mechanical support and enhance cell electrical signaling after implantation into myocardial infarct. Theranostics. 2018;8(12): 3317-3330. [49] NOOR N, SHAPIRA A, EDRI R, et al. 3D Printing of Personalized Thick and Perfusable Cardiac Patches and Hearts. Adv Sci. 2019;6(11):1900344. [50] Fong AH, Romero-López M, Heylman CM, et al. Three-Dimensional Adult Cardiac Extracellular Matrix Promotes Maturation of Human Induced Pluripotent Stem Cell-Derived Cardiomyocytes. Tissue Eng Part A. 2016;22: 1016-1025. [51] SEO Y, JUNG Y, KIM SH. Decellularized heart ECM hydrogel using supercritical carbon dioxide for improved angiogenesis. Acta Biomater. 2018;67:270-281. [52] ZHANG D, SHADRIN IY, LAM J, et al. Tissue-engineered Cardiac Patch for Advanced Functional Maturation of Human ESC-derived Cardiomyocytes. Biomaterials. 2013;34(23): 5813-5820. [53] ZHANG W, WANG Z, XIE C, et al. Scaffold with Micro/Macro-Architecture for Myocardial Alignment Engineering into Complex 3D Cell Patterns. Adv Healthc Mater. 2019;8(22):e1901015. [54] BEJLERI D, STREETER BW, NACHLAS ALY, et al. A Bioprinted Cardiac Patch Composed of Cardiac-Specific Extracellular Matrix and Progenitor Cells for Heart Repair. Adv Healthc Mater. 2018;7(23):e1800672. [55] MAIULLARI F, COSTANTINI M, MILAN M, et al. A multi-cellular 3D bioprinting approach for vascularized heart tissue engineering based on HUVECs and iPSC-derived cardiomyocytes. Sci Rep. 2018;8(1): 1-15. [56] GAO L, KUPFER ME, JUNG JP, et al. Myocardial Tissue Engineering With Cells Derived from Human Induced-Pluripotent Stem Cells and a Native-Like, High- Resolution, 3-Dimensionally Printed Scaffold. Circ Res. 2017;120(8): 1318-1325. [57] GAO L, GREGORICH ZR, ZHU W, et al. Large Cardiac Muscle Patches Engineered From Human Induced-Pluripotent Stem Cell-Derived Cardiac Cells Improve Recovery From Myocardial Infarction in Swine. Circulation. 2018;137(3): 1712-1730. [58] SAKAGUCHI K, SHIMIZU T, OKANO T. Construction of three-dimensional vascularized cardiac tissue with cell sheet engineering. J Control Release. 2015;205:83-88. [59] SARAVANAN S, SAREEN N, ABU-EL-RUB E, et al. Graphene Oxide-Gold Nanosheets Containing Chitosan Scaffold Improves Ventricular Contractility and Function After Implantation into Infarcted Heart. Sci Rep. 2018;8(1): 15069. [60] KC P, SHAH M, LIAO J, et al. Prevascularization of Decellularized Porcine Myocardial Slice for Cardiac Tissue Engineering Pawan. Physiol Behav. 2017;176(12): 139-148. [61] KARBASSI E, FENIX A, MARCHIANO S, et al. Cardiomyocyte maturation: advances in knowledge and implications for regenerative medicine. Nat Rev Cardiol. 2020;17:341-359. [62] GARBERN JC, HELMAN A, SEREDA R, et al. Inhibition of mTOR Signaling Enhances Maturation of Cardiomyocytes Derived from Human Induced Pluripotent Stem Cells via p53-Induced Quiescence. Circulation. 2020; 141(4):285-300. [63] ROSHANBINFAR K, MOHAMMADI Z, SHEIKH-MAHDI MESGAR A, et al. Carbon nanotube doped pericardial matrix derived electroconductive biohybrid hydrogel for cardiac tissue engineering. Biomater. Sci. 2019;7(9): 3906-3917. [64] XU B, HAN X, HU Y, et al. A Remotely Controlled Transformable Soft Robot Based on Engineered Cardiac Tissue Construct. Small.2019;15(18):1-10. |
| [1] | 林清凡, 解一新, 陈婉清, 叶振忠, 陈幼芳. 人胎盘源间充质干细胞条件培养液可上调缺氧状态下BeWo细胞活力和紧密连接因子的表达[J]. 中国组织工程研究, 2021, 25(在线): 4970-4975. |
| [2] | 蒲 锐, 陈子扬, 袁凌燕. 不同细胞来源外泌体保护心脏的特点与效应[J]. 中国组织工程研究, 2021, 25(在线): 1-. |
| [3] | 张 超, 吕 欣. 髋臼骨折固定后的异位骨化:危险因素、预防及其治疗进展[J]. 中国组织工程研究, 2021, 25(9): 1434-1439. |
| [4] | 周继辉, 李新志, 周 游, 黄 卫, 陈文瑶. 髌骨骨折修复内植物选择的多重问题[J]. 中国组织工程研究, 2021, 25(9): 1440-1445. |
| [5] | 王德斌, 毕郑刚. 尺骨鹰嘴骨折-脱位解剖力学、损伤特点、固定修复及3D技术应用的相关问题[J]. 中国组织工程研究, 2021, 25(9): 1446-1451. |
| [6] | 姬志祥, 蓝常贡. 尿酸盐转运蛋白在痛风中的多态性和治疗相关性[J]. 中国组织工程研究, 2021, 25(8): 1290-1298. |
| [7] | 袁 美, 张新新, 郭祎莎, 毕 霞. 循环microRNA在血管性认知障碍诊断中的应用[J]. 中国组织工程研究, 2021, 25(8): 1299-1304. |
| [8] | 蒋红英, 朱 亮, 余 曦, 黄 靖, 向小娜, 兰正燕, 何红晨. 富血小板血浆干预脊髓损伤患者压力性损伤的作用[J]. 中国组织工程研究, 2021, 25(8): 1149-1153. |
| [9] | 张秀梅, 翟运开, 赵 杰, 赵 萌. 类器官模型国内外数据库近10年文献研究热点分析[J]. 中国组织工程研究, 2021, 25(8): 1249-1255. |
| [10] | 侯婧瑛, 于萌蕾, 郭天柱, 龙会宝, 吴 浩. 缺氧预处理激活HIF-1α/MALAT1/VEGFA通路促进骨髓间充质干细胞生存和血管再生[J]. 中国组织工程研究, 2021, 25(7): 985-990. |
| [11] | 史洋洋, 秦英飞, 吴福玲, 何 潇, 张雪静. 胎盘间充质干细胞预处理预防小鼠毛细支气管炎[J]. 中国组织工程研究, 2021, 25(7): 991-995. |
| [12] | 梁学奇, 郭黎姣, 陈贺捷, 武 杰, 孙雅琪, 邢稚坤, 邹海亮, 陈雪玲, 吴向未. 泡状棘球绦虫原头蚴抑制骨髓间充质干细胞向成纤维细胞的分化[J]. 中国组织工程研究, 2021, 25(7): 996-1001. |
| [13] | 樊全宝, 罗惠娜, 王丙云, 陈胜锋, 崔连旭, 江文康, 赵明明, 王静静, 罗冬章, 陈志胜, 白银山, 刘璨颖, 张 晖. 低氧培养犬脂肪间充质干细胞的生物学特性[J]. 中国组织工程研究, 2021, 25(7): 1002-1007. |
| [14] | 耿 瑶, 尹志良, 李兴平, 肖东琴, 侯伟光. hsa-miRNA-223-3p调控人骨髓间充质干细胞成骨分化的作用[J]. 中国组织工程研究, 2021, 25(7): 1008-1013. |
| [15] | 伦志刚, 金 晶, 王添艳, 李爱民. 过氧化物还原酶6干预骨髓间充质干细胞增殖及体外向神经谱系诱导分化[J]. 中国组织工程研究, 2021, 25(7): 1014-1018. |
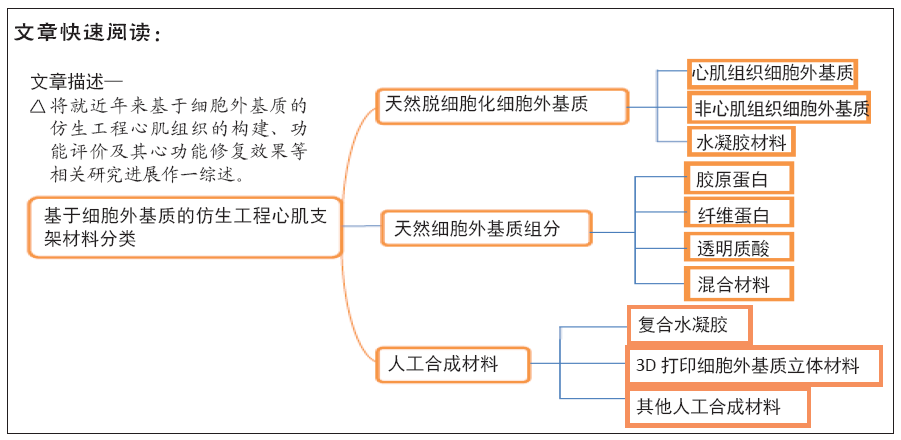
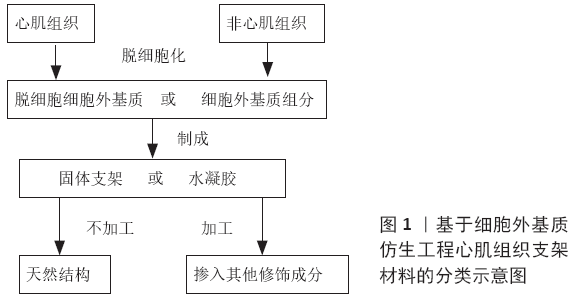
细胞外基质是由细胞合成和分泌的大分子物质组成的复杂三维微环境,主要由胶原蛋白、糖胺聚糖、纤维蛋白、弹性蛋白、层粘蛋白和几种其他糖蛋白组成[4]。研究表明,细胞外基质能为种子细胞提供物理支持与适宜微环境,在诱导种子细胞黏附、存活、迁移、分化及工程心肌组织形态和功能发育等方面具有明显的优势[5-6]。细胞外基质及其衍生材料被认为是理想支架,已被广泛用于构建仿生工程心肌组织的研究中。在基于细胞外基质的仿生工程心肌组织研究中,按细胞外基质组织来源可分为基于心肌组织细胞外基质和基于非心肌组织细胞外基质(non-cardiac extracellular matrix,ncECM)两类研究;按细胞外基质制备方法大致上可分为基于组织脱细胞细胞外基质(decellular extracellular matrix,dECM)和基于单一细胞外基质组分两类研究;按支架物理性质可分为基于固体材料和基于可注射水凝胶材料两类研究。文章将按照上述分类(图1),对近年来基于细胞外基质的仿生工程心肌组织构建、功能评价及其心功能修复效果等相关研究进展作一综述。
 中国组织工程研究杂志出版内容重点:生物材料;骨生物材料; 口腔生物材料; 纳米材料; 缓释材料; 材料相容性;组织工程
中国组织工程研究杂志出版内容重点:生物材料;骨生物材料; 口腔生物材料; 纳米材料; 缓释材料; 材料相容性;组织工程
1.2 入选标准
纳入标准:文献所述内容与构建基于dECM或细胞外基质成分的仿生工程心肌组织主题密切相关的文献。
排除标准:重复性研究,以及研究内容与该综述内容无关的文献。
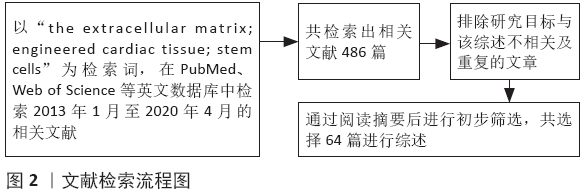
1.3 质量评估 阅读检索出文献的标题、摘要、结论进行初步筛选,最终保留64篇文献作进一步分析,见图2。
未来,工程心肌组织的研究应继续与材料科学[63]、智能机器人等学科的发展相结合[64],改良和研制更多基于细胞外基质和其组分品质优良、临床应用价值更高的支架材料,并探究其与种子细胞的相互作用及分子机制,为心脏再生的临床治疗等提供解决方案。
中国组织工程研究杂志出版内容重点:生物材料;骨生物材料; 口腔生物材料; 纳米材料; 缓释材料; 材料相容性;组织工程

文题释义:#br# 细胞外基质:细胞合成和分泌的大分子物质组成的复杂三维微环境,主要由胶原蛋白、糖胺聚糖、纤维蛋白、弹性蛋白、层粘蛋白和几种其他的糖蛋白组成,能为细胞提供物理支持与适宜微环境,从而诱导细胞黏附、存活、迁移、分化及细胞向特定的形态和功能发育。#br# 工程心肌:将支架聚合物与合适的种子细胞结合起来,构建类似于天然心肌的组织工程,可植入心脏受损区域,替换坏死心肌组织以修复心功能。构建工程心肌的3大基石是合适的支架、合适的种子细胞和合适的构建方法。
构建仿生的3大基石是合适的支架、合适的种子细胞和合适的构建方法。细胞外基质能为种子细胞提供物理支持与适宜微环境,在诱导种子细胞成熟及工程心肌组织形态和功能发育等方面具有明显的优势,因此被广泛用于构建仿生工程心肌组织的研究中。文章将对近年来基于细胞外基质的仿生工程心肌组织的构建等相关研究进展作一综述,为仿生工程心肌组织的临床应用提供进一步的理论依据。#br#
中国组织工程研究杂志出版内容重点:生物材料;骨生物材料; 口腔生物材料; 纳米材料; 缓释材料; 材料相容性;组织工程#br#
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||