| [1] Chang JH, Gabison EE, Kato T, et al. Corneal neovascularization. Curr Opin Ophthalmol. 2001;12(4): 242-249.[2] Peyman GA, Kivilcim M, Morales AM, et al. Inhibition of corneal angiogenesis by ascorbic acid in the rat model. Graefes Arch Clin Exp Ophthalmol. 2007;245:1461-1467.[3] Miller JW. Vascular endothelial growth factor and ocular neovascularization. Am J Pathol. 1997;151(1):13-23.[4] Dawson DW, Volpert OV, Gillis P, et al. Pigment epithelium-derived factor: a potent inhibitor of angiogenesis. Science. 1999;285(5425):245-248.[5] Kvanta A. Ocular angiogenesis: the role of growth factors. Acta Ophthalmol Scand. 2006;84:282-288.[6] Dorrell M, Usitalo-Jarvinen H, Aguilar E, et al. Ocular neovascularization: basic mechanisms and therapeutic advances. Surv Ophthalmol. 2007;52(Suppl):S3-S19.[7] Jimenez B, Volpert OV. Mechanistic insights on the inhibition of tumor angiogenesis. J Mol Med. 2001;78: 663-672.[8] Ambati BK, Nozaki M, Singh N, et al. Corneal avascularity is due to soluble VEGF receptor-1. Nature. 2006;443:993-997.[9] Spranger J, Osterhoff M, Reimann M, et al. Loss of the antiangiogenic PEDF in patients with angiogenic eye disease. Diabetes. 2001;50:2641-2645.[10] Gao G, Li Y, Zhang D, et al. Unbalanced expression of VEGF and PEDF in ischemia-induced retinal neovascularization. FEBS Lett. 2001;489(2-3):270-276.[11] Gao G, Ma J. Tipping the balance for angiogenic disorders. Drug Discov Today. 2002;7(3):171-172.[12] Amano S, Rohan R, Kuroki M, et al. Requirement for vascular endothelial growth factor in wound- and inflammation-related corneal neovascularization. Invest Ophthalmol Vis Sci. 1998; 39(1):18-22.[13] Tombran-Tink J, Johnson LV. Collagen-induced alterations in intercellular adhesion and antigen expression in retinoblastoma cells. Exp Eye Res. 1989;48(4):549-559.[14] Elahy M, Baindur-Hudson S, Dass CR. The emerging role of PEDF in stem cell biology. J Biomed Biotechnol. 2012;2012: 239091.[15] Yabe T, Sanagi T, Yamada H. The neuroprotective role of PEDF: implication for the therapy of neurological disorders. Curr Mol Med. 2010;10(3):259-266.[16] Tombran-Tink J. PEDF in angiogenic eye diseases. Curr Mol Med. 2010;10(3):267-278.[17] Kawaguchi T, Yamagishi SI, Sata M. Structure-function relationships of PEDF. Curr Mol Med. 2010;10(3):302-311.[18] Broadhead ML, Dass CR, Choong PF. In vitro and in vivo biological activity of PEDF against a range of tumors. Expert Opin Ther Targets. 2009;13(12):1429-1438.[19] Filleur S, Nelius T, de Riese W, et al. Characterization of PEDF: a multi-functional serpin family protein. J Cell Biochem. 2009;106(5):769-775.[20] Zhang SX, Ma JX. Ocular neovascularization: Implication of endogenous angiogenic inhibitors and potential therapy. Prog Retin Eye Res. 2007;26(1):1-37.[21] Duh EJ, Yang HS, Suzuma I, et al. Pigment epithelium-derived factor suppresses ischemia-induced retinal neovascularization and VEGF-induced migration and growth. Invest Ophthalmol Vis Sci. 2002;43(3):821-829.[22] Ueda S, Yamagishi SI, Okuda S. Anti-vasopermeability effects of PEDF in retinal-renal disorders. Curr Mol Med. 2010;10(3):279-283.[23] Jin J, Ma JX, Guan M, et al. Inhibition of chemical cautery-induced corneal neovascularization by topical pigment epithelium-derived factor eyedrops. Cornea. 2010; 29(9):1055-1061.[24] Stellmach V, Crawford SE, Zhou W, et al. Prevention of ischemia-induced retinopathy by the natural ocular antiangiogenic agent pigment epithelium-derived factor. Proc Natl Acad Sci USA. 2001;98(5):2593-2597.[25] Zhang SX, Wang JJ, Gao G, et al. Pigment epithelium-derived factor (PEDF) is an endogenous antiinflammatory factor. FASEB J. 2006;20(2):323-325.[26] Shi H, Yu HJ, Wang HY, et al. Topical administration of peroxiredoxin-6 on the cornea suppresses inflammation and neovascularization induced by ultraviolet radiation. nvest Ophthalmol Vis Sci. 2012;53(13):8016-8028.[27] Shin YJ, Nam WH, Park SE, et al. Aqueous humor concentrations of vascular endothelial growth factor and pigment epithelium-derived factor in high myopic patients. Mol Vis. 2012;18:2265-2270.[28] Chen HC, Yeh LK, Tsai YJ, et al. Expression of angiogenesis-related factors in human corneas after cultivated oral mucosal epithelial transplantation. Invest Ophthalmol Vis Sci. 2012;53(9):5615-5623. [29] Han Y, Shao Y, Lin Z, et al. Netrin-1 simultaneously suppresses corneal inflammation and neovascularization. Invest Ophthalmol Vis Sci. 2012;53(3):1285-1295.[30] Zhou Q, Yang L, Qu M, et al. Role of senescent fibroblasts on alkali-induced corneal neovascularization. J Cell Physiol. 2012; 227(3):1148-1156. [31] Jia C, Zhu W, Ren S, et al. Comparison of genome-wide gene expression in suture- and alkali burn-induced murine corneal neovascularization. Mol Vis. 2011;17:2386-2399. [32] Jin J, Ma JX, Guan M, et al. Inhibition of chemical cautery-induced corneal neovascularization by topical pigment epithelium-derived factor eyedrops. Cornea. 2010; 29(9):1055-1061.[33] Kuo CN, Yang LC, Yang CT, et al. Inhibition of corneal neovascularization with plasmid pigment epithelium-derived factor (p-PEDF) delivered by synthetic amphiphile INTeraction-18 (SAINT-18) vector in an experimental model of rat corneal angiogenesis. Exp Eye Res. 2009;89(5):678-685. [34] Feher J, Kovacs I, Pacella E, et al. Pigment epithelium-derived factor (PEDF) attenuated capsaicin-induced neurotrophic keratouveitis. Invest Ophthalmol Vis Sci. 2009;50(11):5173-5180.[35] Abdiu O, Van Setten G. Antiangiogenic activity in tears: presence of pigment-epithelium-derived factor. New insights and preliminary results. Ophthalmic Res. 2008;40(1):16-18.[36] Bock F, König Y, Kruse F, et al. Bevacizumab (Avastin) eye drops inhibit corneal neovascularization. Graefes Arch Clin Exp Ophthalmol. 2008;246:281-284.[37] Brown LF, Detmar M, Claffey K, et al. Vascular permeability factor/vascular endothelial growth factor: a multifunctional angiogenic cytokine. EXS. 1997;79:233-269.[38] Ferrara N, Gerber HP, LeCouter J. The biology of VEGF and its receptors. Nat Med. 2003;9:669-676.[39] Takahashi T, Ueno H, Shibuya M. VEGF activates protein kinase C-dependent, but Ras-independent Raf-MEK-MAP kinase pathway for DNA synthesis in primary endothelial cells. Oncogene. 1999;18:2221-2223.[40] Zwick E, Bange J, Ullrich A. Receptor tyrosine kinase signalling as a target for cancer intervention strategies. Endocr Relat Cancer. 2001;8:161-173.[41] Middleton J, Americh L, Gayon R, et al. A comparative study of endothelial cell markers expressed in chronically inflamed human tissues:MECA-79, Duffy antigen receptor for chemokines, von Willebrand factor,CD31, CD34, CD105 and CD146. J Pathol. 2005;206:260-268.[42] Apte RS, Barreiro RA, Duh E, et al. Stimulation of neovascularization by the anti-angiogenic factor PEDF. Invest Ophthalmol Vis Sci. 2004;45(12):4491-4497.[43] Takenaka K, Yamagishi S, Jinnouchi Y, et al. Pigment epithelium-derived factor (PEDF)-induced apoptosis and inhibition of vascular endothelial growth factor (VEGF) expression in MG63 human osteosarcoma cells. Life Sci. 2005;77(25):3231-3241.[44] Noel A, Jost M, Lambert V, et al. Anti-angiogenic therapy of exudative age-related macular degeneration: current progress and emerging concepts. Trends Mol Med. 2007; 13(8):345-352. [45] Zhang J, Huang C, Feng Y, et al. Comparison of beneficial factors for corneal wound-healing of rat mesenchymal stem cells and corneal limbal stem cells on the xenogeneic acellular corneal matrix in vitro. Mol Vis. 2012;18:161-173.[46] Venturi G, Gandini A, Monti E, et al. Lack of expression of SERPINF1, the gene coding for pigment epithelium-derived factor, causes progressively deforming osteogenesis imperfecta with normal type I collagen. J Bone Miner Res. 2012;27(3):723-728. |
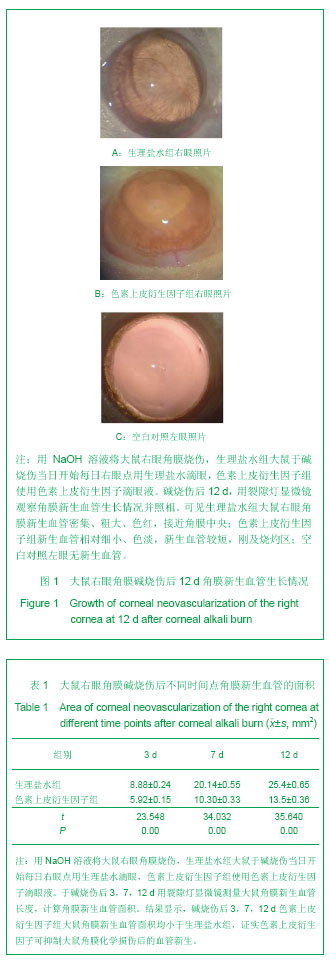
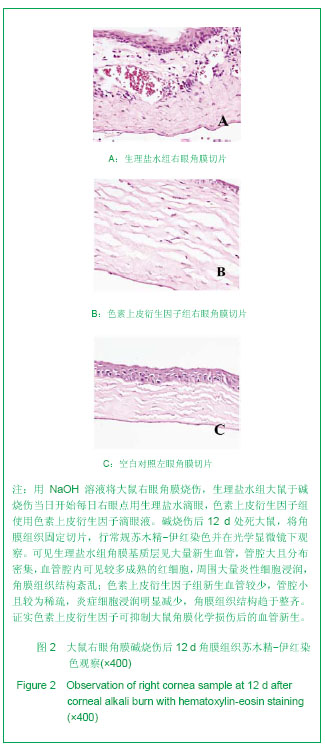
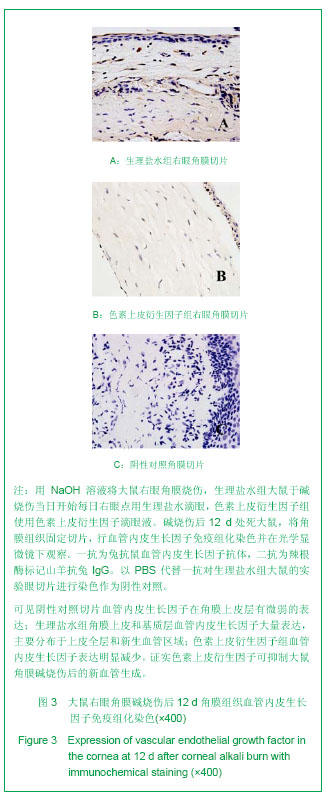
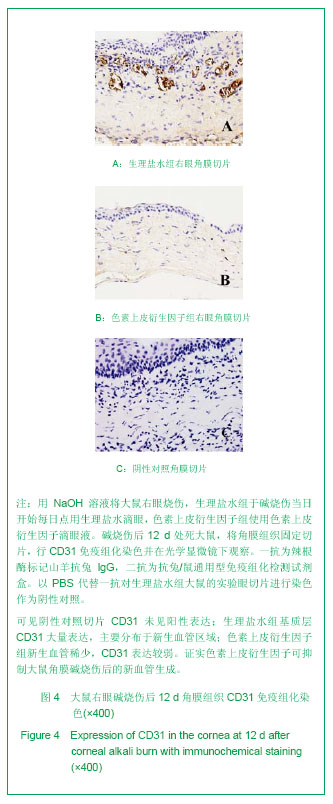
.jpg)
.jpg)