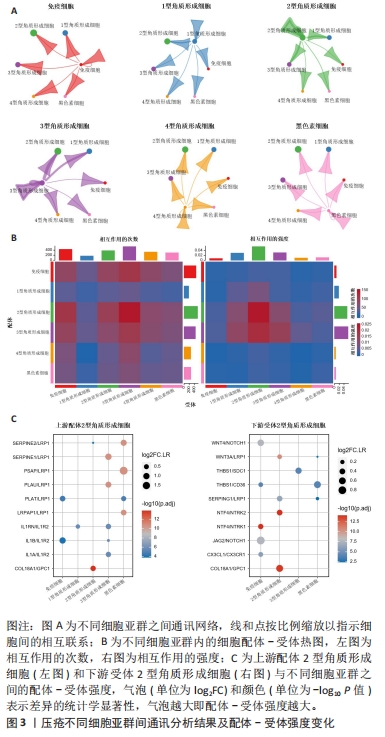
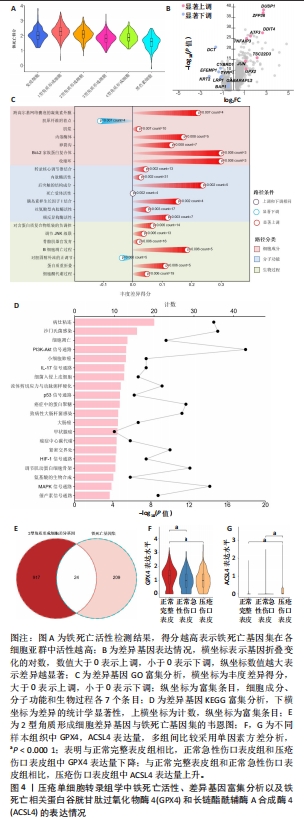
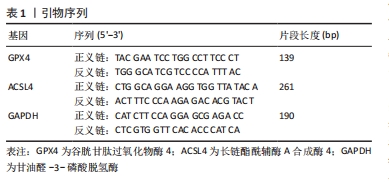
[1] MERVIS JS, PHILLIPS TJ. Pressure ulcers: pathophysiology, epidemiology, risk factors, and presentation. J Am Acad Dermatol. 2019;81(4):881-890.
[2] MAKITA K, OTSUKA N, TOMARU U, et al. NKG2D ligand expression induced by oxidative stress mitigates cutaneous ischemia-reperfusion injury. J Histochem Cytochem. 2023;71(2):61-72.
[3] KIM E, HAM S, JUNG BK, et al. Effect of baicalin on wound healing in a mouse model of pressure ulcers. Int J Mol Sci. 2022;24(1):329.
[4] BINIAZAN F, RAJAEI F, DARABI S, et al. Effects of placenta-derived human amniotic epithelial cells on the wound healing process and TGF-β induced scar formation in murine ischemic-reperfusion injury model. Stem Cell Rev Rep. 2022;18(6):2045-2058.
[5] INOUE Y, UCHIYAMA A, AMALIA SN, et al. Keratinocyte-specific SOX2 overexpression suppressed pressure ulcer formation after cutaneous ischemia-reperfusion injury via enhancement of amphiregulin production. J Invest Dermatol. 2024; 144(1):142-151.e5.
[6] WANG YX, LI B, LIU GT, et al. Corilagin attenuates intestinal ischemia/reperfusion injury in mice by inhibiting ferritinophagy-mediated ferroptosis through disrupting NCOA4-ferritin interaction. Life Sci. 2023;334:122176.
[7] LI J, CAO F, YIN HL, et al. Ferroptosis: past, present and future. Cell Death Dis. 2020; 11(2):88.
[8] WANG ZR, YAO MR, JIANG LY, et al. Dexmedetomidine attenuates myocardial ischemia/reperfusion-induced ferroptosis via AMPK/GSK-3β/Nrf2 axis. Biomed Pharmacother. 2022;154:113572.
[9] CHEN X, KANG R, KROEMER G, et al. Broadening horizons: the role of ferroptosis in cancer. Nat Rev Clin Oncol. 2021;18(5):280-296.
[10] FENG JW, WANG JL, WANG YQ, et al. Oxidative stress and lipid peroxidation: prospective associations between ferroptosis and delayed wound healing in diabetic ulcers. Front Cell Dev Biol. 2022;10:898657.
[11] YAN HF, TUO QZ, YIN QZ, et al. The pathological role of ferroptosis in ischemia/reperfusion-related injury. Zool Res. 2020;41(3):220-230.
[12] 原凌燕,贺云,汤云燕,等.表没食子儿茶素没食子酸酯对早期压疮大鼠模型缺血再灌注损伤的保护作用及NLRP3炎症小体相关机制研究[J].中药药理与临床,2019,35(1):43-47.
[13] 韩凤玉,闫凤华,张俊飞,等.枸杞多糖促进压疮大鼠皮肤创面愈合的作用机制研究[J].宁夏医学杂志,2023,45(1):5-7.
[14] 王智槟,邹晓玲,邹译娴,等.基于Nrf2/HO-1/GPX4信号轴探讨参芪地黄汤抑制高糖诱导人肾小管上皮细胞铁死亡的作用机制[J].中国中药杂志,2023, 48(19):5337-5344.
[15] 范志能,周厚清.黄柏酮通过调控铁死亡途径对心肌缺血/再灌注大鼠心肌损伤的保护作用研究[J].中国医院药学杂志,2023,43(17):1932-1938.
[16] 李丽琴,张鼎,袁莉,等.温阳复元方联合miR-137模拟剂调控线粒体铁死亡对脑缺血再灌注损伤大鼠的作用机制[J].陕西中医,2023,44(10):1354-1359.
[17] ZHANG M, YANG H, WAN LF, et al. Single-cell transcriptomic architecture and intercellular crosstalk of human intrahepatic cholangiocarcinoma. J Hepatol. 2020; 73(5):1118-1130.
[18] LI DQ, CHENG SL, PEI Y, et al. Single-cell analysis reveals major histocompatibility complex II‒expressing keratinocytes in pressure ulcers with worse healing outcomes. J Invest Dermatol. 2022;142(3 Pt A):705-716.
[19] JIN SQ, GUERRERO-JUAREZ CF, ZHANG LH, et al. Inference and analysis of cell-cell communication using CellChat. Nat Commun. 2021;12(1):1088.
[20] Wu TZ, Hu EQ, Xu SB, et al. ClusterProfiler 4.0: a universal enrichment tool for interpreting omics data. Innovation (Camb). 2021;2(3):100141.
[21] KOTTNER J, CUDDIGAN J, CARVILLE K, et al. Prevention and treatment of pressure ulcers/injuries: the protocol for the second update of the international clinical practice guideline 2019. J Tissue Viability. 2019;28(2):51-58.
[22] QUIŃOZ GALLARDO MD, BARRIENTOS-TRIGO S, PORCEL- GÁLVEZ AM. Effectiveness of the best practice spotlight organizations program to reduce the prevalence of pressure injuries in acute care settings for hospitalized patients in Spain: a quasi-experimental study. Worldviews Evid Based Nurs. 2023;20(4):306-314.
[23] QIANG L, YANG SW, CUI YH, et al. Keratinocyte autophagy enables the activation of keratinocytes and fibroblastsand facilitates wound healing. Autophagy. 2021; 17(9):2128-2143.
[24] PIIPPONNE M, LI D, LANDÉN NX. The immune functions of keratinocytes in skin wound healing. Int J Mol Sci. 2020;21(22):8790.
[25] TAKEO M, LEE W, ITO M. Wound healing and skin regeneration. Cold Spring Harb Perspect Med. 2015;5(1):a023267.
[26] SHEDOEVA A, LEAVESLEY D, UPTON Z, et al. Wound healing and the use of medicinal plants. Evid Based Complement Alternat Med. 2019;2019:2684108.
[27] ARRIBAS-LÓPEZ E, ZAND N, OJO O, et al. The effect of amino acids on wound healing: a systematic review and meta-analysis on arginine and glutamine. Nutrients. 2021;13(8):2498.
[28] CHU AS, DELMORE B. Arginine: what you need to know for pressure injury healing. Adv Skin Wound Care. 2021;34(12):630-636.
[29] SPEECKAERT R, DUGARDIN J, LAMBERT J, et al. Critical appraisal of the oxidative stress pathway in vitiligo: a systematic review and meta-analysis. J Eur Acad Dermatol Venereol. 2018;32(7):1089-1098.
[30] 张喆,王琪,陈佳希,等.氧化应激下角质形成细胞中YTHDC1升高促进IL-1β表达[J].现代生物医学进展,2022,22(10):1811-1816.
[31] GALLUZZI L, VITALE I, AARONSON SA, et al. Molecular mechanisms of cell death: recommendations of the nomenclature committee on cell death 2018. Cell Death Differ. 2018;25(3):486-541.
[32] 王莹,代彦丽,朴金龙,等.炎症因子、生长因子以及凋亡因子在压疮慢性难愈合性创面中的表达及作用[J].中国应用生理学杂志,2017,33(2):181-184,188.
[33] HE SX, LI R, PENG YM, et al. ACSL4 contributes to ferroptosis-mediated rhabdomyolysis in exertional heat stroke. J Cachexia Sarcopenia Muscle. 2022;13(3):1717-1730.
[34] BERSUKER K, HENDRICKS JM, LI Z, et al. The CoQ oxidoreductase FSP1 acts parallel to GPX4 to inhibit ferroptosis. Nature. 2019;575(7784):688-692.
[35] FORCINA GC, DIXON SJ. GPX4 at the crossroads of lipid homeostasis and ferroptosis. Proteomics. 2019;19(18):e1800311.
[36] YUAN H, LI XM, ZHANG XY, et al. Identification of ACSL4 as a biomarker and contributor of ferroptosis. Biochem Biophys Res Commun. 2016;478(3):1338-1343.
[37] DOLL S, PRONETH B, TYURINA YY, et al. ACSL4 dictates ferroptosis sensitivity by shaping cellular lipid composition. Nat Chem Biol. 2017;13(1):91-98.
[38] QIU CW, CHEN B, ZHU HF, et al. Gastrodin alleviates cisplatin nephrotoxicity by inhibiting ferroptosis via the SIRT1/FOXO3A/GPX4 signaling pathway. J Ethnopharmacol. 2024;319(Pt 3):117282.
[39] TANG LJ, LUO XJ, TU H, et al. Ferroptosis occurs in phase of reperfusion but not ischemia in rat heart following ischemia or ischemia/reperfusion. Naunyn Schmiedebergs Arch Pharmacol. 2021;394(2):401-410.
|