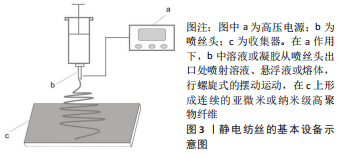
[1] PIGEOT S, KLEIN T, GULLOTTA F, et al. Manufacturing of human tissues as off-the-shelf grafts programmed to induce regeneration. Adv Mater. 2021;33(43):e2103737.
[2] MAIA FR, BASTOS AR, OLIVEIRA JM, et al. Recent approaches towards bone tissue engineering. Bone. 2022;154:116256.
[3] ATALA A. Bioengineered tissues for urogenital repair in children. Pediatr Res. 2008;63(5):569-575.
[4] ELGHBLAWI E. Platelet-rich plasma, the ultimate secret for youthful skin elixir and hair growth triggering. J Cosmet Dermatol. 2018;17(3):423-430.
[5] SARKAR R, GUPTA M. Platelet-rich plasma in melasma-a systematic review. Dermatol Surg. 2022;48(1):131-134.
[6] WU J, PIAO Y, LIU Q, et al. Platelet-rich plasma-derived extracellular vesicles: a superior alternative in regenerative medicine? Cell Prolif. 2021;54(12):e13123.
[7] BELK JW, KRAEUTLER MJ, HOUCK DA, et al. Platelet-rich plasma versus hyaluronic acid for knee osteoarthritis: a systematic review and meta-analysis of randomized controlled trials. Am J Sports Med. 2021;49(1):249-260.
[8] KONWARH R, KARAK N, MISRA M. Electrospun cellulose acetate nanofibers: the present status and gamut of biotechnological applications. Biotechnol Adv. 2013;31(4):421-437.
[9] FOSTER TE, PUSKAS BL, MANDELBAUM BR, et al. Platelet-rich plasma: from basic science to clinical applications. Am J Sports Med. 2009;37(11):2259-2272.
[10] ZHANG X, WANG J, REN M, et al. A novel collagen/platelet-rich plasma (COL/PRP) scaffold: preparation and growth factor release analysis. Cell Tissue Bank. 2016;17(2):327-334.
[11] OUDELAAR BW, PEERBOOMS JC, HUIS IN’T VELD R, et al. Concentrations of blood components in commercial platelet-rich plasma separation systems: a review of the literature. Am J Sports Med. 2019;47(2):479-487.
[12] KIM JI, BAE HC, PARK HJ, et al. Effect of Storage conditions and activation on growth factor concentration in platelet-rich plasma. J Orthop Res. 2020;38(4):777-784.
[13] SHAHRIAR SMS, MONDAL J, HASAN MN, et al. Electrospinning nanofibers for therapeutics delivery. Nanomaterials (Basel). 2019;9(4):532.
[14] CHAHAL S, KUMAR A, HUSSIAN FSJ. Development of biomimetic electrospun polymeric biomaterials for bone tissue engineering: a review. J Biomater Sci Polym Ed. 2019;30(14):1308-1355.
[15] BHATTARAI DP, AGUILAR LE, PARK CH, et al. A review on properties of natural and synthetic based electrospun fibrous materials for bone tissue engineering. Membranes (Basel). 2018;8(3):62.
[16] ZHANG CL, YU SH. Nanoparticles meet electrospinning: recent advances and future prospects. Chem Soc Rev. 2014;43(13):4423-4448.
[17] ASTI A, GIOGLIO L. Natural and synthetic biodegradable polymers: different scaffolds for cell expansion and tissue formation. Int J Artif Organs. 2014;37(3):187-205.
[18] LI WJ, COOPER JA JR, MAUCK RL, et al. Fabrication and characterization of six electrospun poly(alpha-hydroxy ester)-based fibrous scaffolds for tissue engineering applications. Acta Biomater. 2006;2(4):377-385.
[19] YILDIRIMER L, THANH NT, SEIFALIAN AM. Skin regeneration scaffolds: a multimodal bottom-up approach. Trends Biotechnol. 2012;30(12):638-648.
[20] ASKARZADEH N, NAZARPAK MH, MANSOORI K, et al. Bilayer cylindrical conduit consisting of electrospun polycaprolactone nanofibers and DSC cross-linked sodium alginate hydrogel to bridge peripheral nerve gaps. Macromol Biosci. 2020;20(9):e2000149.
[21] XI-XUN Y, FEI L, YUAN-TING X, et al. In vitro study in the endothelial cell compatibility and endothelialization of genipin-crosslinked biological tissues for tissue-engineered vascular scaffolds. J Mater Sci Mater Med. 2010;21(2):777-785.
[22] SONG JY, RYU HI, LEE JM, et al. Conformal fabrication of an electrospun nanofiber mat on a 3D ear cartilage-shaped hydrogel collector based on hydrogel-assisted electrospinning. Nanoscale Res Lett. 2021;16(1):116.
[23] 高婷婷,常丹,刘凤岐,等.有机复合水凝胶的研究进展[J].功能材料,2016, 47(S1):72-77.
[24] LIU X, ZU E, CHANG X, et al. Bi-phasic effect of gelatin in myogenesis and skeletal muscle regeneration. Dis Model Mech. 2021;14(12):dmm049290.
[25] 卢伟鹏,张兵,郭燕川.明胶静电纺丝的研究进展[J].明胶科学与技术,2013, 33(1):8-14.
[26] BARDONOVA L, KOTZIANOVA A, SKUHROVCOVA K, et al. Effects of emulsion, dispersion, and blend electrospinning on hyaluronic acid nanofibers with incorporated antiseptics. Int J Biol Macromol. 2022;194:726-735.
[27] CASTRO KC, CAMPOS MGN, MEI LHI. Hyaluronic acid electrospinning: challenges, applications in wound dressings and new perspectives. Int J Biol Macromol. 2021;173:251-266.
[28] NIU Y, STADLER FJ, FANG J, et al. Hyaluronic acid-functionalized poly-lactic acid (PLA) microfibers regulate vascular endothelial cell proliferation and phenotypic shape expression. Colloids Surf B Biointerfaces. 2021;206:111970.
[29] SNETKOV P, MOROZKINA S, OLEKHNOVICH R, et al. Curcumin/usnic acid-loaded electrospun nanofibers based on hyaluronic acid. Materials (Basel). 2020;13(16):3476.
[30] KERSANI D, MOUGIN J, LOPEZ M, et al. Stent coating by electrospinning with chitosan/poly-cyclodextrin based nanofibers loaded with simvastatin for restenosis prevention. Eur J Pharm Biopharm. 2020;150:156-167.
[31] PINA S, CANADAS RF, JIMENEZ G, et al. Biofunctional ionic-doped calcium phosphates: silk fibroin composites for bone tissue engineering scaffolding. Cells Tissues Organs. 2017;204(3-4):150-163.
[32] TSAI SW, YU WX, HWANG PA, et al. Fabrication and characteristics of pcl membranes containing strontium-substituted hydroxyapatite nanofibers for guided bone regeneration. Polymers (Basel). 2019;11(11):1761.
[33] DAELEMANS L, STEYAERT I, SCHOOLAERT E, et al. Nanostructured hydrogels by blend electrospinning of polycaprolactone/gelatin nanofibers. Nanomaterials (Basel). 2018;8(7):551.
[34] QIAN Y, CHEN H, XU Y, et al. The preosteoblast response of electrospinning PLGA/PCL nanofibers:effects of biomimetic architecture and collagen I. Int J Nanomedicine. 2016;11:4157-4171.
[35] EOM J, KWAK Y, NAM C. Electrospinning fabrication of magnetic nanoparticles-embedded polycaprolactone (PCL) sorbent with enhanced sorption capacity and recovery speed for spilled oil removal. Chemosphere. 2022;303(Pt 3):135063.
[36] YOSHIKAWA H, TAMAI N, MURASE T, et al. Interconnected porous hydroxyapatite ceramics for bone tissue engineering. J R Soc Interface. 2009;6 Suppl 3:S341-S348.
[37] KALIMULDINA G, TURDAKYN N, ABAY I, et al. A review of piezoelectric pvdf film by electrospinning and its applications. Sensors (Basel). 2020;20(18):5214.
[38] WU JY, WANG CY, CHEN KH, et al. Electrospinning of quaternized chitosan-poly(vinyl alcohol) composite nanofiber membrane: processing optimization and antibacterial efficacy. Membranes (Basel). 2022;12(3):332.
[39] DOS SANTOS VI, MERLINI C, ARAGONES Á, et al. In vitro evaluation of bilayer membranes of PLGA/hydroxyapatite/β-tricalcium phosphate for guided bone regeneration. Mater Sci Eng C Mater Biol Appl. 2020;112:110849.
[40] MIJIRITSKY E, ASSAF HD, PELEG O, et al. Use of PRP, PRF and CGF in periodontal regeneration and facial rejuvenation-a narrative review. Biology (Basel). 2021;10(4):317.
[41] CHENG G, MA X, LI J, et al. Incorporating platelet-rich plasma into coaxial electrospun nanofibers for bone tissue engineering. Int J Pharm. 2018;547(1-2):656-666.
[42] VOCETKOVA K, SOVKOVA V, BUZGO M, et al. A simple drug delivery system for platelet-derived bioactive molecules, to improve melanocyte stimulation in vitiligo treatment. Nanomaterials (Basel). 2020;10(9):1801.
[43] LANA JFSD, DA FONSECA LF, MACEDO RDR, et al. Platelet-rich plasma vs bone marrow aspirate concentrate:An overview of mechanisms of action and orthobiologic synergistic effects. World J Stem Cells. 2021;13(2):155-167.
[44] GHAFFARINOVIN Z, SOLTANINIA O, MORTAZAVI Y, et al. Repair of rat cranial bone defect by using amniotic fluid-derived mesenchymal stem cells in polycaprolactone fibrous scaffolds and platelet-rich plasma. Bioimpacts. 2021;11(3):209-217.
[45] PRABHAKARAN MP, VENUGOPAL JR, RAMAKRISHNA S. Mesenchymal stem cell differentiation to neuronal cells on electrospun nanofibrous substrates for nerve tissue engineering. Biomaterials. 2009;30(28):4996-5003.
[46] YIN A, BOWLIN GL, LUO R, et al. Electrospun silk fibroin/poly (L-lactide-ε-caplacton) graft with platelet-rich growth factor for inducing smooth muscle cell growth and infiltration. Regen Biomater. 2016;3(4):239-245.
[47] FESHARAKI M, RAZAVI S, GHASEMI-MOBARAKEH L, et al. Differentiation of human scalp adipose-derived mesenchymal stem cells into mature neural cells on electrospun nanofibrous scaffolds for nerve tissue engineering applications. Cell J. 2018;20(2):168-176.
[48] BHUMIRATANA S, BERNHARD JC, ALFI DM, et al. Tissue-engineered autologous grafts for facial bone reconstruction. Sci Transl Med. 2016;8(343):343ra83.
[49] LEE JW, HAN HS, HAN KJ, et al. Long-term clinical study and multiscale analysis of in vivo biodegradation mechanism of Mg alloy. Proc Natl Acad Sci U S A. 2016; 113(3):716-721.
[50] Koç S, Çakmak S, Gümüşderelioğlu M, et al. Three dimensional nanofibrous and compressible poly(L-lactic acid) bone grafts loaded with platelet-rich plasma. Biomed Mater. 2021;16(4):045012.
[51] ZHAO C, TAN A, PASTORIN G, et al. Nanomaterial scaffolds for stem cell proliferation and differentiation in tissue engineering. Biotechnol Adv. 2013; 31(5):654-668.
[52] LI Z, ZHANG X, YUAN T, et al. Addition of platelet-rich plasma to silk fibroin hydrogel bioprinting for cartilage regeneration. Tissue Eng Part A. 2020;26(15-16):886-895.
[53] KASHEF-SABERI MS, HAYATI RN, PARIVAR K, et al. Enhanced osteogenic differentiation of mesenchymal stem cells on electrospun polyethersulfone/poly (vinyl) alcohol/platelet rich plasma nanofibrous scaffolds. ASAIO J. 2018;64(5):e115-e122.
[54] ABAZARI MF, NEJATI F, NASIRI N, et al. Platelet-rich plasma incorporated electrospun PVA-chitosan-HA nanofibers accelerates osteogenic differentiation and bone reconstruction. Gene. 2019;720:144096.
[55] ABAZARI MF, SOLEIMANIFAR F, AMINI F, et al. Improved osteogenic differentiation of human induced pluripotent stem cells cultured on polyvinylidene fluoride/collagen/platelet-rich plasma composite nanofibers. J Cell Physiol. 2020;235(2):1155-1164.
[56] SAJESH KM, KIRAN K, NAIR SV, et al. Sequential layer-by-layer electrospinning of nano SrCO3/PRP loaded PHBV fibrous scaffold for bone tissue engineering. Compos B Eng. 2016;99:445-452.
[57] LIU J, NIE H, XU Z, et al. Construction of PRP-containing nanofibrous scaffolds for controlled release and their application to cartilage regeneration. J Mater Chem B. 2015;3(4):581-591.
[58] BARLIAN A, JUDAWISASTRA H, ALFARAFISA NM, et al. Chondrogenic differentiation of adipose-derived mesenchymal stem cells induced by L-ascorbic acid and platelet rich plasma on silk fibroin scaffold. Sci Rep. 2020;10(1):19449.
[59] QIU M, CHEN D, SHEN C, et al. Platelet-rich plasma-loaded poly (d,l-lactide)-poly (ethylene glycol)-poly (d, l-lactide) hydrogel dressing promotes full-thickness skin wound healing in a rodent model. Int J Mol Sci. 2016;17(7):1001.
[60] MIROSHNICHENKO S, TIMOFEEVA V, PERMYKOVA E, et al. Plasma-coated polycaprolactone nanofibers with covalently bonded platelet-rich plasma enhance adhesion and growth of human fibroblasts. Nanomaterials (Basel). 2019;9(4):637.
[61] SAMADIAN H, EHTERAMI A, SARRAFZADEH A, et al. Sophisticated polycaprolactone/gelatin nanofibrous nerve guided conduit containing platelet-rich plasma and citicoline for peripheral nerve regeneration:In vitro and in vivo study. Int J Biol Macromol. 2020;150:380-388.
[62] WU D, LIU J, PANG X, et al. Palmitic acid exerts pro-inflammatory effects on vascular smooth muscle cells by inducing the expression of C-reactive protein, inducible nitric oxide synthase and tumor necrosis factor-α. Int J Mol Med. 2014;34(6):1706-1712.
[63] WANG K, LIU L, XIE J, et al. Facile strategy to generate aligned polymer nanofibers:effects on cell adhesion. ACS Appl Mater Interfaces. 2018;10(2):1566-1574.
[64] JIN G, HE R, SHA B, et al. Electrospun three-dimensional aligned nanofibrous scaffolds for tissue engineering. Mater Sci Eng C Mater Biol Appl. 2018;92:995-1005. |