[1] 杨娜.即刻种植牙的临床研究进展[J].医疗装备,2019,32(12):189-190.
[2] 于婉琦,周延民,赵静辉.口腔种植体新材料的研究现状[J].国际口腔医学杂志,2019,46(4):488-496.
[3] 张晨秋,王柏翔,王慧明.种植体表面抗菌技术的分类与研究进展[J].口腔医学,2020,40(3):258-261.
[4] RASOULI R, BARHOUM A, ULUDAG H. A review of nanostructured surfaces and materials for dental implants: surface coating, patterning and functionalization for improved performance. Biomater Sci. 2018; 6(6):1312-1338.
[5] CASTELLANO A, GIL LF, BONFANTE EA, et al. Early Healing Evaluation of Commercially Pure Titanium and Ti-6Al-4V Presenting Similar Surface Texture: An In Vivo Study. Implant Dent. 2017;26(3):338-344.
[6] 马凯,赵宝红,邓春富,等.医用钛及钛合金牙种植体生物相容性及其相关抗菌性能研究进展[J].中国实用口腔科杂志,2016,9(7): 441-445.
[7] TALLARICO M, PARK CJ, LUMBAU AI, et al. Customized 3D-Printed Titanium Mesh Developed to Regenerate a Complex Bone Defect in the Aesthetic Zone: A Case Report Approached with a Fully Digital Workflow. Materials (Basel). 2020;13(17):3874.
[8] YANG BC, ZHOU XD, YU HY, et al. Advances in titanium dental implant surface modification. Hua Xi Kou Qiang Yi Xue Za Zhi. 2019;37(2):124-129.
[9] LIU X, LI S, MENG Y, et al. Osteoclast differentiation and formation induced by titanium implantation through complement C3a. Mater Sci Eng C Mater Biol Appl. 2021;122:111932.
[10] TRINDADE R, ALBREKTSSON T, GALLI S, et al. Osseointegration and foreign body reaction: Titanium implants activate the immune system and suppress bone resorption during the first 4 weeks after implantation. Clin Implant Dent Relat Res. 2018;20(1):82-91.
[11] CORDEIRO JM, BARÃO VAR. Is there scientific evidence favoring the substitution of commercially pure titanium with titanium alloys for the manufacture of dental implants? Mater Sci Eng C Mater Biol Appl. 2017;71:1201-1215.
[12] JIMAN PA, MOLDOVAN M, SAROSI C, et al. Surface characterization and cytotoxicity analysis of the titanium alloys for dentistry. Studia UBB Chemia. 2020;65:149-162.
[13] REVATHI A, BORRÁS AD, MUÑOZ AI, et al. Degradation mechanisms and future challenges of titanium and its alloys for dental implant applications in oral environment. Mater Sci Eng C Mater Biol Appl. 2017;76:1354-1368.
[14] YAN B, TAN J, WANG D, et al. Surface alloyed Ti–Zr layer constructed on titanium by Zr ion implantation for improving physicochemical and osteogenic properties. Progress in Natural Science: Materials International. 2020;30(5):635-641.
[15] ZHANG Y, SUN D, CHENG J, et al. Mechanical and biological properties of Ti-(0-25 wt%)Nb alloys for biomedical implants application. Regen Biomater. 2020;7(1):119-127.
[16] EL-HADAD S, SAFWAT EM, SHARAF NF. In-vitro and in-vivo, cytotoxicity evaluation of cast functionally graded biomaterials for dental implantology. Mater Sci Eng C Mater Biol Appl. 2018;93:987-995.
[17] KIM HJ, JEONG YH, CHOE HC, et al. Surface morphology of TiN-coated nanotubular Ti-25Ta-xZr alloys for dental implants prepared by RF sputtering. Thin Solid Films. 2013;549:131-134.
[18] HOPPE V, SZYMCZYK-ZIÓŁKOWSKA P, RUSIŃSKA M, et al. Assessment of Mechanical, Chemical, and Biological Properties of Ti-Nb-Zr Alloy for Medical Applications. Materials (Basel). 2020;14(1):126.
[19] FOWLER L, MASIA N, CORNISH LA, et al. Development of Antibacterial Ti-Cux Alloys for Dental Applications: Effects of Ageing for Alloys with Up to 10 wt% Cu. Materials (Basel). 2019;12(23):4017.
[20] PIGLIONICO S, BOUSQUET J, FATIMA N, et al. Porous Tantalum VS. Titanium Implants: Enhanced Mineralized Matrix Formation after Stem Cells Proliferation and Differentiation. J Clin Med. 2020;9(11):3657.
[21] USLU E, MIMIROGLU D, ERCAN B. Nanofeature size and morphology of Tantalum oxide surfaces control osteoblast functions. ACS Appl Bio Mater. 2021;4(1):780-794.
[22] SHARANRAJ V, RAMESHA CM, KAVYA K, et al. Zirconia: as a biocompatible biomaterial used in dental implants. Advances in Applied Ceramics. 2020;120(2):63-68.
[23] HAN J, ZHANG F, VAN MEERBEEK B, et al. Laser surface texturing of zirconia-based ceramics for dental applications: A review. Mater Sci Eng C Mater Biol Appl. 2021;123:112034.
[24] ROEHLING S, ASTASOV-FRAUENHOFFER M, HAUSER-GERSPACH I, et al. In Vitro Biofilm Formation on Titanium and Zirconia Implant Surfaces. J Periodontol. 2017;88(3):298-307.
[25] GANBOLD B, KIM SK, HEO SJ, et al. Osteoclastogenesis Behavior of Zirconia for Dental Implant. Materials (Basel). 2019;12(5):732.
[26] SAADALDIN SA, RIZKALLA AS. Synthesis and characterization of wollastonite glass-ceramics for dental implant applications. Dent Mater. 2014;30(3):364-371.
[27] SAADALDIN SA, DIXON SJ, COSTA DO, et al. Synthesis of bioactive and machinable miserite glass-ceramics for dental implant applications. Dent Mater. 2013;29(6):645-655.
[28] WU J, LIU Y, ZHANG H, et al. Silicon nitride as a potential candidate for dental implants: Osteogenic activities and antibacterial properties. J Mater Res. 2021;36:1866-1882.
[29] BADRAN Z, STRUILLOU X, HUGHES FJ, et al. Silicon Nitride (Si3N4) Implants: The Future of Dental Implantology? J Oral Implantol. 2017; 43(3):240-244.
[30] 王河军,曲弋,杨永栋,等.PEEK棒腰椎后路内固定的基础及临床应用进展[J].生物骨科材料与临床研究,2020,17(5):58-60.
[31] AL-RABAB’AH M, HAMADNEH W, ALSALEM I, et al. Use of High Performance Polymers as Dental Implant Abutments and Frameworks: A Case Series Report. J Prosthodont. 2019;28(4):365-372.
[32] MA Z, ZHAO X, ZHAO J, et al. Biologically Modified Polyether Ether Ketone as Dental Implant Material. Front Bioeng Biotechnol. 2020;8: 620537.
[33] WANG L, HE S, WU X, et al. Polyetheretherketone/nano-fluorohydroxyapatite composite with antimicrobial activity and osseointegration properties. Biomaterials. 2014;35(25):6758-6775.
[34] OUYANG L, CHEN M, WANG D, et al. Nano Textured PEEK Surface for Enhanced Osseointegration. ACS Biomater Sci Eng. 2019;5(3):1279-1289.
[35] XU D, SONG W, ZHANG J, et al. Osteogenic effect of polymethyl methacrylate bone cement with surface modification of lactoferrin. J Biosci Bioeng. 2021;132(2):132-139.
[36] 李小东,李新梅,孙晓晨,等.牙种植高分子材料聚甲基丙烯酸甲酯的生物相容性[J].中国组织工程研究,2015,19(47):7613-7618.
[37] WANG L, LUO Q, ZHANG X, et al. Co-implantation of magnesium and zinc ions into titanium regulates the behaviors of human gingival fibroblasts. Bioact Mater. 2020;6(1):64-74.
[38] ZHANG H, QIU J, LIU X. Enhanced antioxidant capability and osteogenic property of medical titanium by cerium plasma immersion ion implantation. Surfaces and Interfaces. 2021;26:101402.
[39] HUANG HH, SHIAU DK, CHEN CS, et al. Nitrogen plasma immersion ion implantation treatment to enhance corrosion resistance, bone cell growth, and antibacterial adhesion of Ti-6Al-4V alloy in dental applications. Surface and Coatings Technology. 2019;365:179-188.
[40] TANG X, HUANG K, DAI J, et al. Influences of surface treatments with abrasive paper and sand-blasting on surface morphology, hydrophilicity, mineralization and osteoblasts behaviors of n-CS/PK composite. Sci Rep. 2017;7(1):568.
[41] VELASCO-ORTEGA E, ORTIZ-GARCÍA I, JIMÉNEZ-GUERRA A, et al. Comparison between Sandblasted Acid-Etched and Oxidized Titanium Dental Implants: In Vivo Study. Int J Mol Sci. 2019;20(13):3267.
[42] CHIKARAKARA E, FITZPATRICK P, MOORE E, et al. In vitro fibroblast and pre-osteoblastic cellular responses on laser surface modified Ti-6Al-4V. Biomed Mater. 2014;10(1):015007.
[43] LIANG C, WANG H, YANG J, Et al. Femtosecond laser-induced micropattern and Ca/P deposition on Ti implant surface and its acceleration on early osseointegration. ACS Appl Mater Interfaces. 2013;5(16):8179-8186.
[44] SHARMA A, MCQUILLAN AJ, SHARMA LA, et al. Spark anodization of titanium-zirconium alloy: surface characterization and bioactivity assessment. J Mater Sci Mater Med. 2015;26(8):221.
[45] KAZEK-KĘSIK A, NOSOL A, PŁONKA J, et al. PLGA-amoxicillin-loaded layer formed on anodized Ti alloy as a hybrid material for dental implant applications. Mater Sci Eng C Mater Biol Appl. 2019;94:998-1008.
[46] BAI Y, ZHOU R, CAO J, et al. Microarc oxidation coating covered Ti implants with micro-scale gouges formed by a multi-step treatment for improving osseointegration. Mater Sci Eng C Mater Biol Appl. 2017; 76:908-917.
[47] LI G, CAO H, ZHANG W, et al. Enhanced Osseointegration of Hierarchical Micro/Nanotopographic Titanium Fabricated by Microarc Oxidation and Electrochemical Treatment. ACS Appl Mater Interfaces. 2016;8(6):3840-3852.
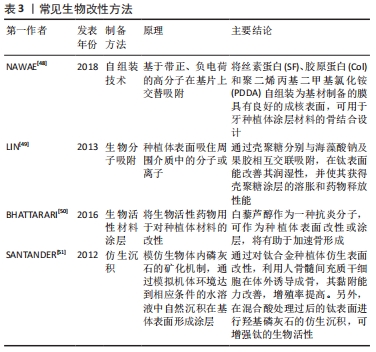
[48] NAWAE S, MEESANE J, MUENSIT N, et al. Layer-by-layer self-assembled films of silk fibroin/collagen/poly (diallyldimethylammonium chloride) as nucleating surface for osseointegration to design coated dental implant materials. Materials & Design. 2018;160:1158-1167.
[49] LIN HY, CHEN JH. Osteoblast differentiation and phenotype expressions on chitosan-coated Ti-6Al-4V. Carbohydr Polym. 2013;97(2):618-626.
[50] BHATTARAI G, POUDEL SB, KOOK SH, et al. Resveratrol prevents alveolar bone loss in an experimental rat model of periodontitis. Acta Biomater. 2016;29:398-408.
[51] SANTANDER S, ALCAINE C, LYAHYAI J, et al. In vitro osteoinduction of human mesenchymal stem cells in biomimetic surface modified titanium alloy implants. Dent Mater J. 2012;31(5):843-850.
[52] LIU MQ, GE K, JIANG L. Research progress on oral implant materials with antimicrobial properties. International Journal of Stomatology. 2018;45(5):516-521.
[53] GODOY-GALLARDO M, MANZANARES-CÉSPEDES MC, SEVILLA P, et al. Evaluation of bone loss in antibacterial coated dental implants: An experimental study in dogs. Mater Sci Eng C Mater Biol Appl. 2016;69: 538-545.
[54] LI D, LI Y, SHRESTHA A, et al. Effects of Programmed Local Delivery from a Micro/Nano-Hierarchical Surface on Titanium Implant on Infection Clearance and Osteogenic Induction in an Infected Bone Defect. Adv Healthc Mater. 2019;8(11):e1900002.
[55] FENBO M, XINGYU X, BIN T. Strontium chondroitin sulfate/silk fibroin blend membrane containing microporous structure modulates macrophage responses for guided bone regeneration. Carbohydr Polym. 2019;213:266-275.
[56] 邓雪阳,潘兰兰,胡婷,等.钛合金表面氧化石墨烯涂层的制备[J].国际口腔医学杂志,2018,45(5):539-545.
[57] LA WG, PARK S, YOON HH, et al. Delivery of a therapeutic protein for bone regeneration from a substrate coated with graphene oxide. Small. 2013;9(23):4051-4060.
[58] KIM JW, SHIN YC, LEE JJ, et al. The Effect of Reduced Graphene Oxide-Coated Biphasic Calcium Phosphate Bone Graft Material on Osteogenesis. Int J Mol Sci. 2017;18(8):1725.
[59] RAMS TE, DEGENER JE, VAN WINKELHOFF AJ. Antibiotic resistance in human peri-implantitis microbiota. Clin Oral Implants Res. 2014; 25(1):82-90.
[60] BAGHDAN E, RASCHPICHLER M, LUTFI W, et al. Nano spray dried antibacterial coatings for dental implants. Eur J Pharm Biopharm. 2019;139:59-67.
[61] 游滢滢,冯云枝.纳米含氟羟基磷灰石牙种植体的生物相容性[J].中国组织工程研究,2014,18(12):1901-1906.
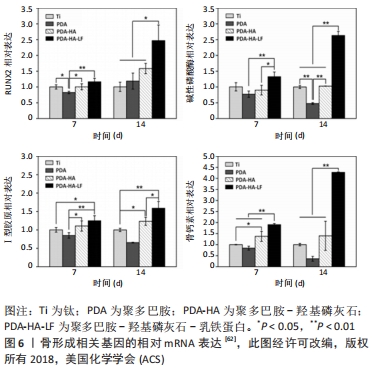
[62] SHEN T, YANG W, SHEN X, et al. Polydopamine-Assisted Hydroxyapatite and Lactoferrin Multilayer on Titanium for Regulating Bone Balance and Enhancing Antibacterial Property. ACS Biomater Sci Eng. 2018;4(9): 3211-3223.
[63] PALLA-RUBIO B, ARAÚJO-GOMES N, FERNÁNDEZ-GUTIÉRREZ M, et al. Synthesis and characterization of silica-chitosan hybrid materials as antibacterial coatings for titanium implants. Carbohydr Polym. 2019; 203:331-341.
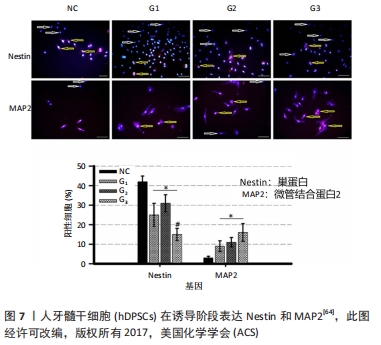
[64] GHASEMI HAMIDABADI H, REZVANI Z, NAZM BOJNORDI M, et al. Chitosan-Intercalated Montmorillonite/Poly(vinyl alcohol) Nanofibers as a Platform to Guide Neuronlike Differentiation of Human Dental Pulp Stem Cells. ACS Appl Mater Interfaces. 2017;9(13):11392-11404.
[65] 李伶俐,李潇.钛基种植体表面涂层的研究进展[J].中国临床新医学,2020,13(5):527-532.
[66] 孙丰权.钛种植体抗菌肽涂层的抗菌性及细胞相容性研究[D].佳木斯:佳木斯大学,2018.
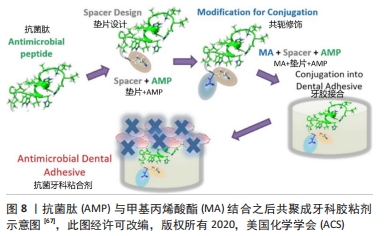
[67] XIE SX, SONG L, YUCA E, et al. Antimicrobial Peptide-Polymer Conjugates for Dentistry. ACS Appl Polym Mater. 2020;2(3):1134-1144.
|