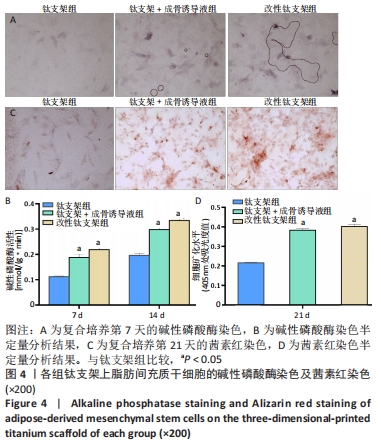
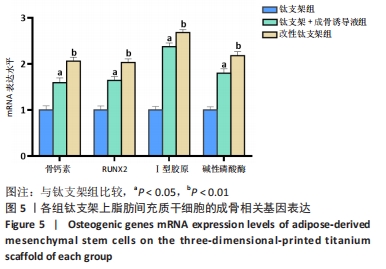
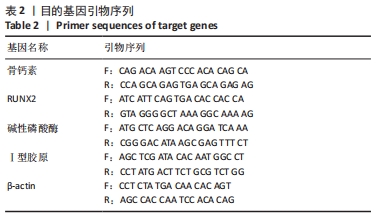
[1] WANG X, WU X, XING H, et al. Porous Nanohydroxyapatite/Collagen Scaffolds Loading Insulin PLGA Particles for Restoration of Critical Size Bone Defect. ACS Appl Mater Interfaces. 2017;9(13):11380-11391.
[2] 靳小雷,滕利,徐家杰,等.唇颊部洞穿性缺损的综合外科修复[J].中国美容医学杂志,2010,19(6):799-801.
[3] BOSE S, VAHABZADEH S, BANDYOPADHYAY A, et al. Bone tissue engineering using 3D printing. Mater Today. 2013;16(12):496-504.
[4] 付军,郭征,范宏斌,等.应用3D打印假体重建下肢肿瘤性长节段骨缺损[J].中华骨科杂志,2017,37(7):433-440.
[5] MARĘDZIAK M, MARYCZ K, LEWANDOWSKI D, et al. Static magnetic field enhance synthesis and secretion of membrane-derived microvesicles (MVs) rich in VEGF and BMP-2 in equine adipose-derived stromal cells (EqASCs)-A new approach in veterinary regenerative medicine. In Vitro Cell Dev Biol Anim. 2015;51(3):230-240.
[6] ULLAH I, SUBBARAO RB, RHO GJ, et al. Human mesenchymal stem cells-current trends and future prospective. Biosci Rep. 2015;35(2):e00191.
[7] FUKUNISHI T, BEST CA, ONG CS, et al. Role of Bone Marrow Mononuclear Cell Seeding for Nanofiber Vascular Grafts. Tissue Eng Part A. 2018;24(1-2):135-144.
[8] MITRA D, WHITEHEAD J, YASUI OW, et al. Bioreactor culture duration of engineered constructs influences bone formation by mesenchymal stem cells. Biomaterials. 2017;146:29-39.
[9] LIU C, DONG JY, YUE LL, et al. Rapamycin/sodium hyaluronate binding on nano-hydroxyapatite coated titanium surface improves MC3T3-E1 osteogenesis. Plos One. 2017;12(2):e0171693.
[10] TOOSI S, NADERI-MESHKIN H, KALALINIA F, et al. Bone defect healing is induced by collagen sponge/polyglycolic acid. J Mater Sci Mater Med. 2019;30(3):33.
[11] KO E, LEE JS, KIM H, et al. Electrospun Silk Fibroin Nanofibrous Scaffolds with Two-Stage Hydroxyapatite Functionalization for Enhancing the Osteogenic Differentiation of Human Adipose-Derived Mesenchymal Stem Cells. ACS Appl Mater Interfaces. 2018;10(9):7614-7625.
[12] LIAO HT, TSAI MJ, BRAHMAYYA M, et al. Bone Regeneration Using Adipose-Derived Stem Cells in Injectable Thermo-Gelling Hydrogel Scaffold Containing Platelet-Rich Plasma and Biphasic Calcium Phosphate. Int J Mol Sci. 2018;19(9):2537.
[13] ZHOU X, ZHANG D, WANG M, et al. Three-Dimensional Printed Titanium Scaffolds Enhance Osteogenic Differentiation and New Bone Formation by Cultured Adipose Tissue-Derived Stem Cells Through the IGF-1R/AKT/Mammalian Target of Rapamycin Complex 1 (mTORC1) Pathway. Med Sci Monit. 2019;25:8043-8054.
[14] QI X, WANG H, ZHANG Y, et al. Mesoporous bioactive glass-coated 3D printed borosilicate bioactive glass scaffolds for improving repair of bone defects. Int J Biol Sci. 2018;14(4):471-484.
[15] KIM SE, SHIM KM, JANG K, et al. Three-Dimensional Printing-based Reconstruction of a Maxillary Bone Defect in a Dog Following Tumor Removal. In Vivo. 2018;32(1):63-70.
[16] 党莹,李月,李瑞玉,等.骨组织工程支架材料在骨缺损修复及3D打印技术中的应用[J].中国组织工程研究,2017,21(14):2266-2273.
[17] SPETZGER U, FRASCA M, KÖNIG SA. Surgical planning, manufacturing and implantation of an individualized cervical fusion titanium cage using patient-specific data. Eur Spine J. 2016;25(7):2239-2246.
[18] BETTINGER CJ, LANGER R, BORENSTEIN JT, et al. Engineering substrate topography at the micro- and nanoscale to control cell function. Angew Chem Int Ed Engl. 2009;48(30):5406-5415.
[19] DUVVURU MK, HAN W, CHOWDHURY PR, et al. Bone marrow stromal cells interaction with titanium; Effects of composition and surface modification. PLoS One. 2019;14(5):e0216087.
[20] CARDAROPOLI F, ALFIERI V, CAIAZZO F, et al. Manufacturing of porous biomaterials for dental implant applications through selective laser melting. Adv Mater Res. 2012;6(535-537):1222-1229.
[21] WAN Y, WANG Y, LIU Z, et al. Adhesion and proliferation of OCT-1 osteoblast-like cells on micro- and nano-scale topography structured poly(L-lactide). Biomaterials. 2005;26(21):4453-4459.
[22] MA H, FENG C, CHANG J, et al. 3D-printed bioceramic scaffolds: From bone tissue engineering to tumor therapy. Acta Biomater. 2018;79:37-59.
[23] HUANG J, ZHANG X, YAN W, et al. Nanotubular topography enhances the bioactivity of titanium implants. Nanomedicine. 2017;13(6):1913-1923.
[24] ALVES SA, RIBEIRO AR, GEMINI-PIPERNI S, et al. TiO2 nanotubes enriched with calcium, phosphorous and zinc: promising bio-selective functional surfaces for osseointegrated titanium implants. RSC Advances. 2017;7(78):49720-49738.
[25] YU WQ, JIANG XQ, ZHANG FQ, et al. The effect of anatase TiO2 nanotube layers on MC3T3-E1 preosteoblast adhesion, proliferation, and differentiation. J Biomed Mater Res A. 2010;94(4):1012-1022.
[26] LV L, LIU Y, ZHANG P, et al. The nanoscale geometry of TiO2 nanotubes influences the osteogenic differentiation of human adipose-derived stem cells by modulating H3K4 trimethylation. Biomaterials. 2015;39:193-205.
[27] SHI Q, QIAN Z, LIU D, et al. Surface Modification of Dental Titanium Implant by Layer-by-Layer Electrostatic Self-Assembly. Front Physiol. 2017;8:574.
[28] CHEN S, GUO Y, LIU R, et al. Tuning surface properties of bone biomaterials to manipulate osteoblastic cell adhesion and the signaling pathways for the enhancement of early osseointegration. Colloids Surf B Biointerfaces. 2018;164:58-69.
[29] ZHANG J, LUO X, BARBIERI D, et al. The size of surface microstruc-tures as an osteogenic factor in calcium phosphate ceramics. Acta Biomater. 2014;10(7): 3254-3263.
[30] LI G, QIN S, LIU X, et al. Structure and properties of nano-hydroxyapatite / poly( butylene succinate) porous scaffold for bone tissue engineering prepared by using ethanol as porogen. J Biomater Appl. 2019;33(6):776-791.
[31] SADER MS, BALDUINO A, SOARES GDE A, et al. Effect of three distinct treatments of titanium surface on osteoblast attachment, proliferation, and differentiation. Clin Oral Implants Res. 2005;16(6):667-675.
[32] BRIE IC, SORITAU O, DIRZU N, et al. Comparative in vitro study regarding the biocompatibility of titanium-base composites infiltrated with hydroxyapatite or silicatitanate. J Biol Eng. 2014;8(1):1-19.
[33] 李庆帆,王佐林. ALP、Runx2及OCN在大鼠拔牙后牙槽骨来源BMSCs中的表达[J].口腔颌面外科杂志,2017,27(2):77-82.
[34] PAGANI F, FRANCUCCI CM, MORO L. Markers of bone turnover: biochemical and clinical perspectives. J Endocrinol Invest. 2005;28(10 Suppl):8-13.
[35] 史伟,甘洪全,王茜,等.不同程度低氧培养对多孔钽-人成骨细胞复合物细胞形态及COL-1、OCN蛋白表达的影响[J].中国矫形外科杂志,2017,25(8):729-736.
[36] 王茜,张辉,耿丽鑫,等.国产多孔钽复合MG63细胞培养Col-1、OCN和OPN蛋白表达及意义[J].中国矫形外科杂志,2015,23(5): 441-449.
[37] 张辉,李亮,王茜,等.骨形成蛋白-7对多孔钽-软骨细胞复合物分泌功能以及Col-II、AGG和Sox9基因表达的影响[J].北京大学学报(医学版),2015,47(1):216-222.
[38] MARELLI B, GHEZZI CE, BARRALET JE, et al. Three-dimensional mineralization of dense nanofibrillar collagen-bioglass hybrid scaffolds. Biomacromolecules. 2010;11(6):1470-1479.
[39] KOMORI T. Roles of Runx2 in Skeletal Development. Adv Exp Med Biol. 2017;962:83-93.
[40] 吴顺义,张晓蓉.Runx2在成骨细胞和软骨细胞分化中作用的研究进展[J].医学综述,2019,25(7):1302-1307.
[41] WILDMAN BJ, GODFREY TC, REHAN M, et al. MICROmanagement of Runx2 Function in Skeletal Cells. Curr Mol Biol Rep. 2019;5(1):55-64.
[42] LIN Z, HE H, WANG M, et al. MicroRNA-130a controls bone marrow mesenchymal stem cell differentiation towards the osteoblastic and adipogenic fate. Cell Prolif. 2019;52(6):e12688.
[43] GRIFFIN KS, DAVIS KM, MCKINLEY TO, et al. Evolution of Bone Grafting: Bone Grafts and Tissue Engineering Strategies for Vascularized Bone Regeneration. Clin Rev Bone Miner Metab. 2015;13(4):232-244.
[44] LI X, CHEN C, WEI L, et al. Exosomes derived from endothelial progenitor cells attenuate vascular repair and accelerate reendothelialization by enhancing endothelial function. Cytotherapy. 2016;18(2):253-262.
[45] WANG L, FAN H, ZHANG ZY, et al. Osteogenesis and angiogenesis of tissue-engineered bone constructed by prevascularized beta-tricalcium phosphate scaffold and mesenchymal stem cells. Biomaterials. 2010; 31(36):9452-9461.
[46] SOJO K, SAWAKI Y, HATTORI H, et al. Immunohistochemical study of vascular endothelial growth factor (VEGF) and bone morphogenetic protein-2, -4 (BMP-2, -4) on lengthened rat femurs. J Craniomaxillofac Surg. 2005;33(4):238-245.
|