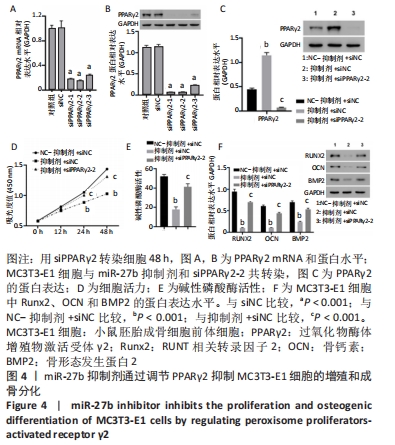
[1] FEEHAN J, AL SAEDI A, DUQUE G. Targeting fundamental aging mechanisms to treat osteoporosis. Expert Opin Ther Targets. 2019;23: 1031-1039.
[2] MENDOZA FA, LE ROUX M, AHMED I. Primary osteoporosis in men: an unmet medical need. Fertil Steril. 2019;112(5):791-798.
[3] SALARI N, DARVISHI N, BARTINA Y, et al. Global prevalence of osteoporosis among the world older adults: a comprehensive systematic review and meta-analysis. J Orthop Surg Res. 2021;16(1):669.
[4] SALARI N, GHASEMI H, MOHAMMADI L, et al. The global prevalence of osteoporosis in the world: a comprehensive systematic review and meta-analysis. J Orthop Surg Res. 2021;16(1):609.
[5] CHEN P, LI Z, HU Y. Prevalence of osteoporosis in China: a meta-analysis and systematic review. BMC Public Health. 2016;16(1):1039.
[6] CHENG X, ZHAO K, ZHA X, et al. Opportunistic Screening Using Low-Dose CT and the Prevalence of Osteoporosis in China: A Nationwide, Multicenter Study. J Bone Miner Res. 2021;36(3):427-435.
[7] CUI Z, MENG X, FENG H, et al. Estimation and projection about the standardized prevalence of osteoporosis in mainland China. Arch Osteoporos. 2019;15(1):2.
[8] WATANABE A, YONEYAMA S, NAKAJIMA M, et al. Osteosarcoma in Sprague-Dawley rats after long-term treatment with teriparatide (human parathyroid hormone (1-34)). J Toxicol Sci. 2012;37(3):617-629.
[9] MALLUCHE HH, CHEN J, LIMA F, et al. Bone Quality and Fractures in Women With Osteoporosis Treated With Bisphosphonates for 1 to 14 Years. JBMR Plus. 2021;5(11):e10549.
[10] LI J, CHEN X, LU L, et al. The relationship between bone marrow adipose tissue and bone metabolism in postmenopausal osteoporosis.Cytokine Growth Factor Rev. 2020;52:88-98.
[11] MURUGANANDAN S, IONESCU AM, SINAL CJ. At the Crossroads of the Adipocyte and Osteoclast Differentiation Programs: Future Therapeutic Perspectives. Int J Mol Sci. 2020;21(7):2277.
[12] MURUGANANDAN S, SINAL CJ. The impact of bone marrow adipocytes on osteoblast and osteoclast differentiation. IUBMB Life. 2014;66(3): 147-155.
[13] MURUGANANDAN S, GOVINDARAJAN R, SINAL CJ. Bone Marrow Adipose Tissue and Skeletal Health. Curr Osteoporos Rep. 2018;16(4): 434-442.
[14] ZHAO X, PATIL S, XU F, et al. Role of Biomolecules in Osteoclasts and Their Therapeutic Potential for Osteoporosis.Biomolecules. 2021; 11(5):747.
[15] YANG Y, YUJIAO W, FANG W, et al. The roles of miRNA, lncRNA and circRNA in the development of osteoporosis. Biol Res. 2020;53(1):40.
[16] ZHAO H, LU A, HE X. Roles of MicroRNAs in Bone Destruction of Rheumatoid Arthritis. Front Cell Dev Biol. 2020;8:600867.
[17] 彭建强,黄年盛,黄胜,等.H_2O_2下调miR-21对MC3T3-E1细胞成骨分化影响的研究[J].中国修复重建外科杂志,2018,32(3):276-284.
[18] 郑峰,张富财,许喆.miR-98-5p促进成骨细胞增殖和分化的可能及机制[J].中国组织工程研究,2021,25(26):4112-4117.
[19] 杨晓红,杨琨,廖立,等.微RNA-705对MC3T3-E1细胞成骨分化能力的影响[J].浙江大学学报(医学版),2016,45(6):575-580.
[20] 赵长铭,黄萌,王振宁,等.miR-129-5p调控MC3T3-E1细胞成骨分化的体外研究[J].解放军医学院学报,2021,42(5):565-570.
[21] HAN Z, ZHAN R, CHEN S, et al. miR-181b/Oncostatin m axis inhibits prostate cancer bone metastasis via modulating osteoclast differentiation. J Cell Biochem. 2020;121(2):1664-1674.
[22] KARBIENER M, FISCHER C, NOWITSCH S, et al. microRNA miR-27b impairs human adipocyte differentiation and targets PPARgamma.Biochem Biophys Res Commun. 2009;390(2):247-251.
[23] JACKSON SM, DEMER LL. Peroxisome proliferator-activated receptor activators modulate the osteoblastic maturation of MC3T3-E1 preosteoblasts. FEBS Lett. 2000;471(1):119-124.
[24] FAJAS L, AUBOEUF D, RASPÉ E, et al. The organization, promoter analysis, and expression of the human PPARgamma gene. J Biol Chem. 1997;272(30):18779-18789.
[25] 朱磊,路瑛丽,冯连世,等.低氧训练诱导miR-27/PPARγ调控肥胖大鼠腓肠肌脂肪酸代谢的研究[J].体育科学,2019,39(6):55-61.
[26] 郭鑫,宗欢欢,李杜达,等.PPARγ在肿瘤中的双重作用[J].中国细胞生物学学报,2021,43(2):460-468.
[27] WEI W, ZEVE D, WANG X, et al. Osteoclast progenitors reside in the peroxisome proliferator-activated receptor γ-expressing bone marrow cell population. Mol Cell Biol. 2011;31(23):4692-4705.
[28] MITTAL S, INAMDAR S, ACHARYA J, et al. miR-3666 inhibits development of hepatic steatosis by negatively regulating PPARγ.Biochim Biophys Acta Mol Cell Biol Lipids. 2020;1865(10):158777.
[29] WANG X, XU Y, ZHU YC, et al. LncRNA NEAT1 promotes extracellular matrix accumulation and epithelial-to-mesenchymal transition by targeting miR-27b-3p and ZEB1 in diabetic nephropathy. J Cell Physiol. 2019;234(8):12926-12933.
[30] WANG X, LU Y, ZHU L, et al. Inhibition of miR-27b Regulates Lipid Metabolism in Skeletal Muscle of Obese Rats During Hypoxic Exercise by Increasing PPARγ Expression. Front Physiol. 2020;11:1090.
[31] Xu J, Lv S, Hou Y, et al. miR-27b promotes type II collagen expression by targetting peroxisome proliferator-activated receptor-γ2 during rat articular chondrocyte differentiation.Biosci Rep. 2018;38(1): BSR20171109.
[32] 董莹莹,王猛,郭艳,等.低钙饲料联合地塞米松致大鼠骨质疏松模型的建立[J].中国骨质疏松杂志,2019,25(10):1393-1397+1404.
[33] YANG L, LIU S, MU S, et al. Paeoniflorin Attenuates Dexamethasone-Induced Apoptosis of Osteoblast Cells and Promotes Bone Formation via Regulating AKT/mTOR/Autophagy Signaling Pathway. Evid Based Complement Alternat Med. 2021;2021:6623464.
[34] PIGNOLO RJ, LAW SF, CHANDRA A. Bone Aging, Cellular Senescence, and Osteoporosis. JBMR Plus. 2021;5(4):e10488.
[35] PAIK J, SCOTT LJ. Romosozumab: A Review in Postmenopausal Osteoporosis. Drugs Aging. 2020;37(11):845-855.
[36] TASNIM N, DUTTA P, NAYEEM J, et al. Osteoporosis, an Inevitable Circumstance of Chronic Kidney Disease: A Systematic Review. Cureus. 2021;13(10):e18488.
[37] BABAN YN, EDICHERIA CM, JOSEPH J, et al. Osteoporosis Complications in Crohn’s Disease Patients: Factors, Pathogenesis, and Treatment Outlines. Cureus. 2021;13(12):e20564.
[38] DRAKE MT, MURAD MH, MAUCK KF, et al. Clinical review. Risk factors for low bone mass-related fractures in men: a systematic review and meta-analysis. J Clin Endocrinol Metab. 2012;97(6):1861-1870.
[39] BUCKLEY L, HUMPHREY MB. Glucocorticoid-Induced Osteoporosis.N Engl J Med. 2018;379(26):2547-2556.
[40] ZHANG L, LI G, WANG K, et al. MiR-30 family members inhibit osteoblast differentiation by suppressing Runx2 under unloading conditions in MC3T3-E1 cells. Biochem Biophys Res Commun. 2020; 522(1):164-170.
[41] 段克友,官建中.外泌体在骨质疏松症治疗中的研究进展[J].中国修复重建外科杂志,2021,35(12):1642-1649.
[42] KONG Y, NIE ZK, LI F, et al. MiR-320a was highly expressed in postmenopausal osteoporosis and acts as a negative regulator in MC3T3E1 cells by reducing MAP9 and inhibiting PI3K/AKT signaling pathway. Exp Mol Pathol. 2019;110:104282.
[43] FAN Q, LI Y, SUN Q, et al. miR-532-3p inhibits osteogenic differentiation in MC3T3-E1 cells by downregulating ETS1. Biochem Biophys Res Commun. 2020;525(2):498-504.
[44] 孙芬,刘名燕,刘铭,等.miR-132-3p过表达对MC3T3-E1细胞增殖分化的影响[J].中国组织工程研究,2020,24(1):59-64.
[45] 王丽娜,刘春梅,胡叶青,等.血清miR-27、PPAR-γ表达与妊娠期糖尿病胰岛素抵抗[J].中国计划生育学杂志,2021,29(5):1021-1024.
[46] LEE JJ, DRAKAKI A, ILIOPOULOS D, et al. MiR-27b targets PPARγ to inhibit growth, tumor progression and the inflammatory response in neuroblastoma cells. Oncogene. 2012;31(33):3818-3825.
[47] SEENPRACHAWONG K, TAWORNSAWUTRUK T, NANTASENAMAT C, et al. miR-130a and miR-27b Enhance Osteogenesis in Human Bone Marrow Mesenchymal Stem Cells via Specific Down-Regulation of Peroxisome Proliferator-Activated Receptor γ. Front Genet. 2018;9:543.
[48] WAN Y, CHONG LW, EVANS RM. PPAR-γ regulates osteoclastogenesis in mice.Nat Med. 2007;13(12):1496-1503.
[49] GU C, XU Y, ZHANG S, et al. miR-27a attenuates adipogenesis and promotes osteogenesis in steroid-induced rat BMSCs by targeting PPARγ and GREM1. Sci Rep. 2016;6:38491.
|