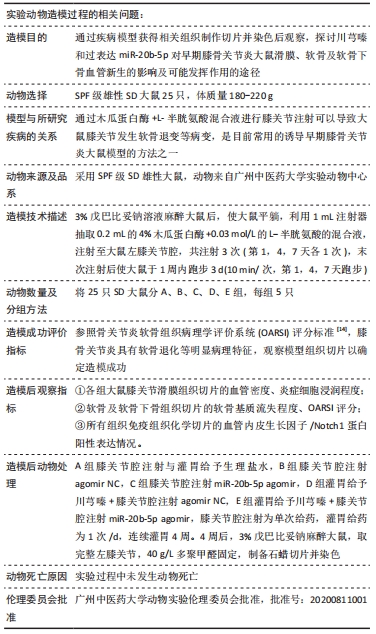
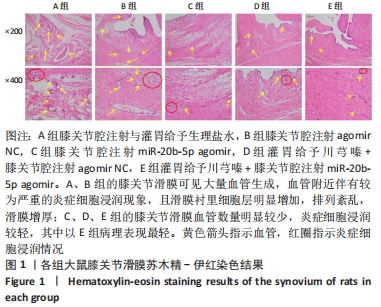
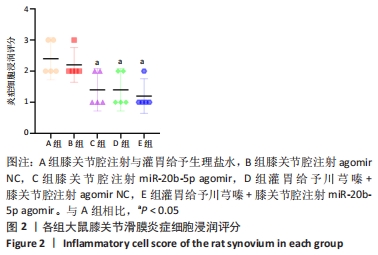
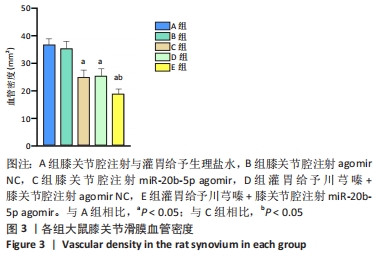
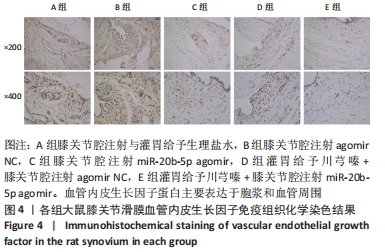
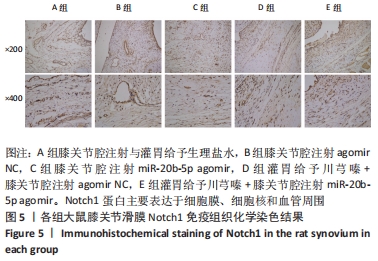
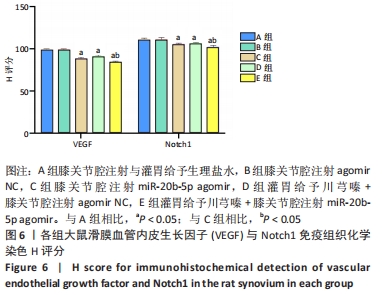
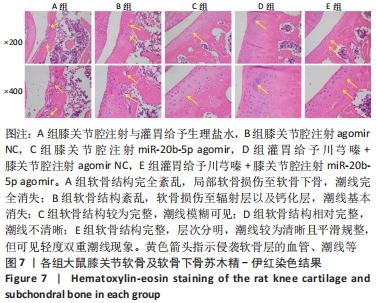
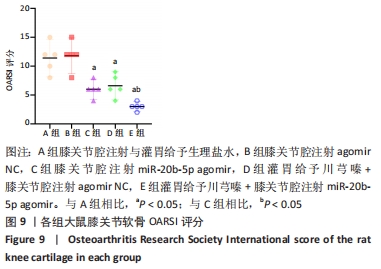
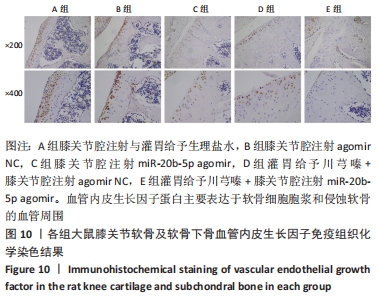
[1] LU KH, LU PW, LU EW, et al. The potential remedy of melatonin on osteoarthritis. J Pineal Res. 2021;71(3):e12762.
[2] WALSH DA, BONNET CS, TUMER EL, et al. Angiogenesis in the synovium and at the osteochondral junction in osteoarthritis. Osteoarthritis Cartilage. 2007;15(7):743-751.
[3] HENROTIN Y, PESESSE L, LAMBERT C. Targeting the synovial angiogenesis as a novel treatment approach to osteoarthritis. Ther Adv Musculoskelet Dis. 2014;6(1):20-34.
[4] PENG Y, WU S, LI Y, et al. Type H blood vessels in bone modeling and remodeling. Theranostics. 2020;10(1):426-436.
[5] BARRANCO C. Osteoarthritis: Animal data show VEGF blocker inhibits post-traumatic OA. Nat Rev Rheumatol. 2014;10(11):638.
[6] GORDON WR, ARNETT KL, BLACKLOW SC. The molecular logic of Notch signaling--a structural and biochemical perspective. J Cell Sci. 2008; 121(Pt 19):3109-3119.
[7] SAHARA M, HANSSON EM, WERNET O, et al. Manipulation of a VEGF-Notch signaling circuit drives formation of functional vascular endothelial progenitors from human pluripotent stem cells. Cell Res. 2014;24(7):820-841.
[8] 谢平金,余翔,柴生颋,等.川芎嗪干预早期膝骨关节炎大鼠软骨Ⅱ型胶原纤维α1基因与血管内皮生长因子mRNA及miR20b的表达[J].中国组织工程研究,2018,22(12):1846-1851.
[9] 李飞龙,谢平金,柴生颋,等.川芎嗪对膝骨性关节炎大鼠软骨VEGF表达的影响[J].中国骨质疏松杂志,2018,24(7):904-909.
[10] 梁桂洪,梁祖建,谢平金,等.川芎嗪对膝骨性关节炎大鼠软骨下骨中miR-20b/VEGF和BMP2/Smad1通路的影响[J].中国药房, 2019,30(4):448-453.
[11] MAISTO R, TROTTA MC, PETRILLO F, et al. Resolvin D1 Modulates the Intracellular VEGF-Related miRNAs of Retinal Photoreceptors Challenged With High Glucose. Front Pharmacol. 2020;11:235.
[12] LAZZARA F, TROTTA MC, PLATANIA CBM, et al. Stabilization of HIF-1α in Human Retinal Endothelial Cells Modulates Expression of miRNAs and Proangiogenic Growth Factors. Front Pharmacol. 2020;11:1063.
[13] 罗臻,李宏栩,卢启贵,等.红姜提取物保护早期膝骨关节炎模型大鼠的关节软骨[J].中国组织工程研究,2021,25(32):5155-5161.
[14] PRITZKER KP, GAY S, JIMENEZ SA, et al. Osteoarthritis cartilage histopathology: grading and staging. Osteoarthritis Cartilage. 2006; 14(1):13-29.
[15] MOULD AW, TONKS ID, CAHILL MM, et al. Vegfb gene knockout mice display reduced pathology and synovial angiogenesis in both antigen-induced and collagen-induced models of arthritis. Arthritis Rheum. 2003;48(9):2660-2669.
[16] 陈永,邱富娟,朱兴旺,等.血管翳并非类风湿关节炎的专利——膝骨关节炎血管翳病理形态观察[J].南方医科大学学报,2019,39(6): 747-750.
[17] VARGHESE F, BUKHARI AB, MALHOTRA R, et al. IHC Profiler: an open source plugin for the quantitative evaluation and automated scoring of immunohistochemistry images of human tissue samples. PLoS One. 2014;9(5):e96801.
[18] WALSH DA. Angiogenesis and arthritis. Rheumatology (Oxford). 1999; 38(2):103-112.
[19] SELLAM J, BERENBAUM F. The role of synovitis in pathophysiology and clinical symptoms of osteoarthritis. Nat Rev Rheumatol. 2010;6(11):625-635.
[20] BENITO MJ, VEALE DJ, FITZGERALD O, et al. Synovial tissue inflammation in early and late osteoarthritis. Ann Rheum Dis. 2005;64(9):1263-1267.
[21] WANG W, WANG L, GULKO PS, et al. Computational deconvolution of synovial tissue cellular composition: presence of adipocytes in synovial tissue decreased during arthritis pathogenesis and progression. Physiol Genomics. 2019;51(6):241-253.
[22] MIMPEN JY, BALDWIN MJ, CRIBBS AP, et al. Interleukin-17A Causes Osteoarthritis-Like Transcriptional Changes in Human Osteoarthritis-Derived Chondrocytes and Synovial Fibroblasts In Vitro. Front Immunol. 2021;12:676173.
[23] CHEN Y, JIANG W, YONG H, et al. Macrophages in osteoarthritis: pathophysiology and therapeutics. Am J Transl Res. 2020;12(1):261-268.
[24] FENG Y, HU S, LIU L, et al. HMGB1 contributes to osteoarthritis of temporomandibular joint by inducing synovial angiogenesis. J Oral Rehabil. 2021;48(5):551-559.
[25] SU W, LIU G, LIU X, et al. Angiogenesis stimulated by elevated PDGF-BB in subchondral bone contributes to osteoarthritis development. JCI Insight. 2020;5(8):e135446.
[26] MAPP PI, WALSH DA. Mechanisms and targets of angiogenesis and nerve growth in osteoarthritis. Nat Rev Rheumatol. 2012;8(7):390-398.
[27] PESESSE L, SANCHEZ C, HENROTIN Y. Osteochondral plate angiogenesis: A new treatment target in osteoarthritis. Joint Bone Spine. 2011;78(2):144-149.
[28] HU Y, CHEN X, WANG S, et al. Subchondral bone microenvironment in osteoarthritis and pain. Bone Res. 2021;9(1):20.
[29] YAJUN W, JIN C, ZHENGRONG G, et al. Betaine Attenuates Osteoarthritis by Inhibiting Osteoclastogenesis and Angiogenesis in Subchondral Bone. Front Pharmacol. 2021;12:723988.
[30] 梁桂洪,曾令烽,潘建科,等.川芎嗪干预骨性关节炎的机制研究进展[J].中华中医药杂志,2020,35(12):6228-6232.
[31] MAISTO R, TROTTA MC, PETRILLO F, et al. Resolvin D1 Modulates the Intracellular VEGF-Related miRNAs of Retinal Photoreceptors Challenged With High Glucose. Front Pharmacol. 2020;11:235.
[32] LUO Y, HE J, TAO X, et al. miR‑20b negatively regulates VEGF expression by targeting STAT3 in H22 hepatocellular carcinoma cells. Oncol Rep. 2018;40(5):2806-2813.
[33] CASCIO S, D’ANDREA A, FERLA R, et al. miR-20b modulates VEGF expression by targeting HIF-1 alpha and STAT3 in MCF-7 breast cancer cells. J Cell Physiol. 2010;224(1):242-249.
[34] 陶象男,汪忆梦,宋传旺.miR-20b直接靶向3’-UTR负性调节VEGF的表达[J].华中科技大学学报(医学版),2016,45(1):22-26.
[35] Borgonio Cuadra VM, Gonzalez-Huerta NC, Romero-Cordoba S, et al. Altered expression of circulating microRNA in plasma of patients with primary osteoarthritis and in silico analysis of their pathways. PLoS One. 2014;9(6):e97690.
[36] CHEN Y, ZHANG L, LI E, et al. Long-chain non-coding RNA HOTAIR promotes the progression of osteoarthritis via sponging miR-20b/PTEN axis. Life Sci. 2020;253:117685.
[37] SAETAN N, HONSAWEK S, TANAVALEE A, et al. Relationship of plasma and synovial fluid vascular endothelial growth factor with radiographic severity in primary knee osteoarthritis. Int Orthop.2014;38(5):1099.
[38] CARLEVARO MF, CERMELLI S, CANCEDDA R, et al. Vascular endothelial growth factor (VEGF) in cartilage neovascularization and chondrocyte differentiation: auto-paracrine role during endochondral bone formation. J Cell Sci. 2000;113(Pt 1):59.
[39] LU J, ZHANG H, CAI D, et al. Positive-Feedback Regulation of Subchondral H-Type Vessel Formation by Chondrocyte Promotes Osteoarthritis Development in Mice. J Bone Miner Res. 2018;33(5): 909-920.
[40] ROMEO SG, ALAWI KM, RODRIGUES J, et al. Endothelial proteolytic activity and interaction with non-resorbing osteoclasts mediate bone elongation. Nat Cell Biol. 2019;21(4):430-441.
[41] QIN H, ZHAO X, HU YJ, et al. Inhibition of SDF-1/CXCR4 Axis to Alleviate Abnormal Bone Formation and Angiogenesis Could Improve the Subchondral Bone Microenvironment in Osteoarthritis. Biomed Res Int. 2021;2021:8852574.
[42] TSAI CH, LIU SC, CHUNG WH, et al. Visfatin Increases VEGF-dependent Angiogenesis of Endothelial Progenitor Cells during Osteoarthritis Progression. Cells. 2020;9(5):1315.
[43] LI B, CHEN K, QIAN N, et al. Baicalein alleviates osteoarthritis by protecting subchondral bone, inhibiting angiogenesis and synovial proliferation. J Cell Mol Med. 2021;25(11):5283-5294.
[44] WANG YH, KUO SJ, LIU SC, et al. Apelin Affects the Progression of Osteoarthritis by Regulating VEGF-Dependent Angiogenesis and miR-150-5p Expression in Human Synovial Fibroblasts. Cells. 2020;9(3):594.
[45] LI W, LIN J, WANG Z, et al. Bevacizumab tested for treatment of knee osteoarthritis via inhibition of synovial vascular hyperplasia in rabbits. J Orthop Translat. 2019;19:38-46.
[46] PEREZ-FIDALGO JA, ORTEGA B, SIMON S, et al. NOTCH signalling in ovarian cancer angiogenesis. Ann Transl Med. 2020;8(24):1705.
[47] Sassi N, Laadhar L, Driss M, et al. The role of the Notch pathway in healthy and osteoarthritic articular cartilage: from experimental models to ex vivo studies. Arthritis Res Ther. 2011;13(2):208.
[48] CHIGURUPATI S, ARUMUGAM TV, SON TG, et al. Involvement of notch signaling in wound healing. PLoS One. 2007;2(11):e1167.
[49] EBRAHIM N, DESSOUKY AA, MOSTAFA O, et al. Adipose mesenchymal stem cells combined with platelet-rich plasma accelerate diabetic wound healing by modulating the Notch pathway. Stem Cell Res Ther. 2021;12(1):392.
[50] SUCHTING S, FREITAS C, LE NOBLE F, et al. The Notch ligand Delta-like 4 negatively regulates endothelial tip cell formation and vessel branching. Proc Natl Acad Sci U S A. 2007;104(9):3225-3230.
[51] LUO Z, SHANG X, ZHANG H, et al. Notch Signaling in Osteogenesis, Osteoclastogenesis, and Angiogenesis. Am J Pathol. 2019;189(8):1495-1500.
[52] AKIL A, GUTIÉRREZ-GARCÍA AK, GUENTER R, et al. Notch Signaling in Vascular Endothelial Cells, Angiogenesis, and Tumor Progression: An Update and Prospective. Front Cell Dev Biol. 2021;9:642352.
[53] 黄敏玲,卢赵琦,申震,等.骨碎补总黄酮干预Notch信号通路影响骨重建过程中成血管-成骨耦联[J].中国组织工程研究,2021, 25(32):5116-5122.
[54] GAO W, SWEENEY C, WALSH C, et al. Notch signalling pathways mediate synovial angiogenesis in response to vascular endothelial growth factor and angiopoietin 2. Ann Rheum Dis. 2013;72(6):1080-1088.
[55] LIAO J, WEI Q, ZOU Y, et al. Notch Signaling Augments BMP9-Induced Bone Formation by Promoting the Osteogenesis-Angiogenesis Coupling Process in Mesenchymal Stem Cells (MSCs). Cell Physiol Biochem. 2017;41(5):1905-1923.
[56] WANG H, HUANG X, ZHANG J, et al. The expression of VEGF and Dll4/Notch pathway molecules in ovarian cancer. Clin Chim Acta. 2014;436: 243-248.
|