中国组织工程研究 ›› 2024, Vol. 28 ›› Issue (18): 2819-2824.doi: 10.12307/2024.043
• 数字化骨科 digital orthopedics • 上一篇 下一篇
三维数字模型辅助微创穿针与钢板内固定治疗SandersⅡ、Ⅲ型跟骨骨折
刘文东,夏洪乐,刘 林,沈润斌,郭 巍,王旭洋,李国梁
- 河北省沧州中西医结合医院骨科,河北省沧州市 061000
Three-dimensional digital model-assisted minimally invasive needle penetration and steel plate internal fixation in treatment of Sanders types II and III calcaneal fractures
Liu Wendong, Xia Hongle, Liu Lin, Shen Runbin, Guo Wei, Wang Xuyang, Li Guoliang
- Department of Orthopedics, Cangzhou Integrated Traditional Chinese and Western Medicine Hospital, Cangzhou 061000, Hebei Province, China
摘要:
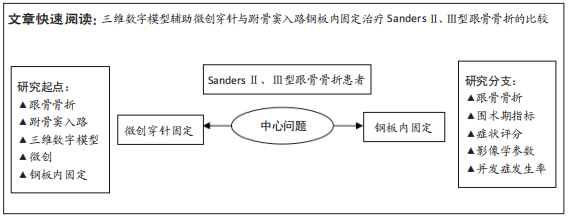
文题释义:
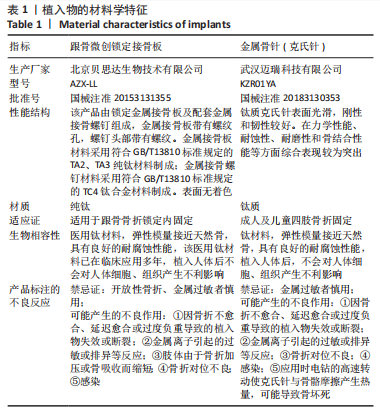
SandersⅡ、Ⅲ型跟骨骨折:跟骨骨折在跗骨骨折中最常见,根据严重程度,跟骨骨折Sanders分型为Ⅰ型、Ⅱ型、Ⅲ型、Ⅳ型这4种类型。Ⅱ型可见1条主要骨折线,有2块主要骨折块,跟骨后关节面为两部分骨折;Ⅲ型有3块主要关节骨折块,是三部分移位骨折,Ⅱ、Ⅲ型属于常见类型。微创穿针固定:一种应用闭合复位经皮穿针固定术式,用克氏针固定替代钢板,具有创伤小、保护足跟血运、加速骨折愈合的优势,可用于跟骨、桡骨、肱骨、锁骨等骨折手术中。
目的:比较三维数字模型辅助微创穿针与跗骨窦切口入路钢板内固定治疗SandersⅡ、Ⅲ型跟骨骨折的疗效。
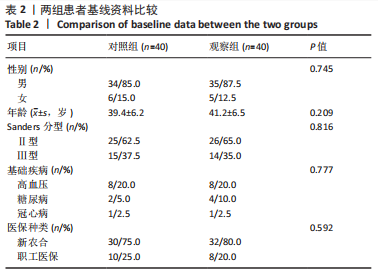
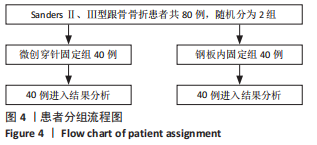
方法:将2021年1月至2022年10月在河北省沧州中西医结合医院骨科治疗的80例SandersⅡ、Ⅲ型跟骨骨折患者随机分为对照组40例和观察组40例。对照组给予传统跗骨窦入路手法复位钢板内固定治疗,观察组给予三维数字模型辅助微创交叉穿针固定治疗。记录两组患者手术时间、失血量、住院时间、骨折愈合时间,观察两组患者术前和术后12个月Maryland评分、AO-FAS评分、目测类比评分、生活质量评分(SF-36评分)、影像学参数(Böhler角、Gissane角,跟骨长度、宽度、高度)变化,并记录随访过程中并发症发生情况。
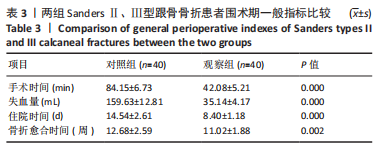
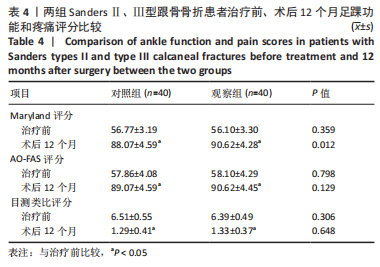
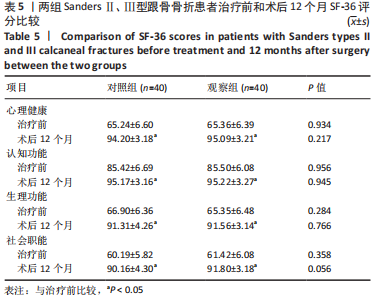
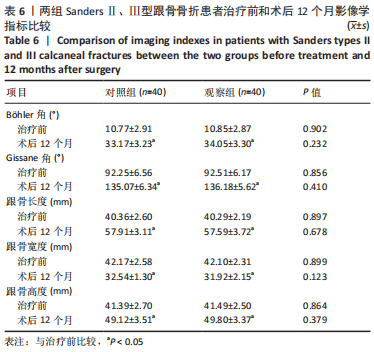
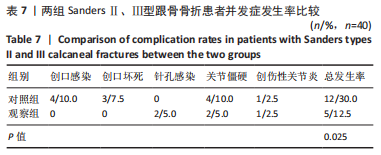
结果与结论:①观察组手术时间、失血量、住院时间、骨折愈合时间均少于对照组(P均 < 0.05);②两组患者治疗后Maryland评分、AO-FAS评分、SF-36评分和Böhler角、Gissane角、跟骨长度、跟骨高度明显高于治疗前(P均 < 0.05);目测类比评分、跟骨宽度明显低于治疗前(P均 < 0.05);③随访12个月,观察组并发症发生率均低于对照组(P均 < 0.05);④结果表明,应用三维数字模型辅助微创穿针固定疗法治疗SandersⅡ、Ⅲ型跟骨骨折可明显改善手术时间、出血量等多项围术期指标,并可减少多种并发症的发生,足踝功能恢复、疼痛症状缓解、提高生活质量方面与传统疗法相当。
https://orcid.org/0000-0002-4838-212X (刘文东)
中国组织工程研究杂志出版内容重点:人工关节;骨植入物;脊柱;骨折;内固定;数字化骨科;组织工程
中图分类号: