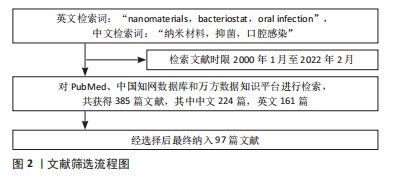
[1] 李洋洋,胡天琦,顾中一.纳米齿科学在抗菌方面的应用进展[J].口腔医学,2017,37(10):950-953.
[2] NORRBY SR, NORD CE, FINCH R, et al. Lack of development of new antimicrobial drugs: a potential serious threat to public health. Lancet Infect Dis. 2005;5(2):115-119.
[3] JAMES P, WORTHINGTON HV, PARNELL C, et al. Chlorhexidine mouthrinse as an adjunctive treatment for gingival health. Cochrane Database Syst Rev. 2017;3(3):CD008676.
[4] 强立,冯永海,刘磊.金基纳米结构光热抗菌研究进展[J].科学通报,2022,67(1):64-76.
[5] 缪婧,刘畅,王旭,等.纳米材料在口腔医学中的应用研究[J].医学信息,2019,32(12):34-36.
[6] 宋智勇,吴阳,韩鹤友.智能化纳米释药系统用于细菌感染治疗的研究进展[J].华中农业大学学报,2020,39(1):1-9.
[7] LE OUAY B, STELLACCI F. Antibacterial activity of silver nanoparticles: A surface science insight. Nano Today. 2015;10(3):339-354.
[8] AMRO NA, KOTRA LP, WADU-MESTHRIGE K, et al. High-Resolution Atomic Force Microscopy Studies of the Escherichiacoli Outer Membrane: Structural Basis for Permeability. Langmuir. 2000;16: 2789-2796.
[9] 谌礼佩,熊洁,江青松.纳米抗菌剂在口腔医学中的研究进展[J].口腔颌面修复学杂志,2019,20(6):351-356.
[10] WANG Y, YANG Y, SHI Y, et al. Antibiotic-Free Antibacterial Strategies Enabled by Nanomaterials: Progress and Perspectives. Adv Mater. 2020;32(18):e1904106.
[11] KUMAR R, UMAR A, KUMAR G, et al. Antimicrobial properties of ZnO nanomaterials: A review. Ceramics International. 2017;43(5):3940-3961.
[12] ECKHARDT S, BRUNETTO PS, GAGNON J, et al. Nanobio silver: its interactions with peptides and bacteria, and its uses in medicine. Chem Rev. 2013;113(7):4708-4754.
[13] ZHENG K, SETYAWATI MI, LEONG DT, et al. Antimicrobial silver nanomaterials. Coordination Chemistry Reviews. 2018;357:1-17.
[14] HOLT KB, BARD AJ. Interaction of silver(I) ions with the respiratory chain of Escherichia coli: an electrochemical and scanning electrochemical microscopy study of the antimicrobial mechanism of micromolar Ag+. Biochemistry. 2005;44(39):13214 -13223.
[15] KANG SJ, CHO YI, KIM KH, et al. Proteomic Analysis to Elucidate the Antibacterial Action of Silver Ions Against Bovine Mastitis Pathogens. Biol Trace Elem Res. 2016;171(1):101-106.
[16] 姚希燕,唐晓宁,王晓楠,等.无机抗菌材料抗菌机理研究进展[J].材料导报,2021,35(1):105-111.
[17] RAI M, YADAV A, GADE A. Silver nanoparticles as a new generation of antimicrobials. Biotechnol Adv. 2009;27(1):76-83.
[18] 马丽娜,米宏霏,薛云新,等.ROS在细菌耐药及抗生素杀菌中的作用机制[J].遗传,2016,38(10):902-909.
[19] 乔越.新型无机纳米生物材料在耐药菌感染慢性难愈合伤口和角膜炎的抗菌促愈功能研究[D].杭州:浙江大学,2020.
[20] JOE A, PARK SH, KIM DJ, et al. Antimicrobial activity of ZnO nanoplates and its Ag nanocomposites: Insight into an ROS-mediated antibacterial mechanism under UV light. Journal of Solid State Chemistry. 2018;267: 124-133.
[21] 赵芙蓉,周晓琴,洪樟连,等.二氧化钛基光催化抗菌材料的研究进展[J].材料导报,2005,19(11):35-38.
[22] 雷绍民,郝骞,熊毕华,等.蒙脱石矿物特性及开发利用前景[J].资源环境与工程,2006,20(5):565-569.
[23] NITHYA N, BHOOPATHI G, MAGESH G, et al. Neodymium doped TiO2 nanoparticles by sol-gel method for antibacterial and photocatalytic activity. Materials Science in Semiconductor Processing. 2018;83:70-82.
[24] QI K, CHENG B, YU J, et al. Review on the improvement of the photocatalytic and antibacterial activities of ZnO. Journal of Alloys and Compounds. 2017;727:792-820.
[25] CAI Y, STRMME M, WELCH K. Disinfection Kinetics and Contribution of Reactive Oxygen Species When Eliminating Bacteria with TiO2 Induced Photocatalysis. Journal of Biomaterials and Nanobiotechnology. 2014; 5:200-209.
[26] KASHEF N, HUANG YY, HAMBLIN MR. Advances in antimicrobial photodynamic inactivation at the nanoscale. Nanophotonics. 2017; 6(5):853-879.
[27] HAMBLIN MR, HASAN T. Photodynamic therapy: a new antimicrobial approach to infectious disease? Photochem Photobiol Sci. 2004;3(5): 436-450.
[28] LINK S, EL-SAYED MA. Shape and size dependence of radiative,non-radiative and photothermal properties of gold nanocrystals. Int Rev Phys Chem. 2000;19:409-453.
[29] 张旺全.新型噻吩--哌嗪类荧光分子的设计及其光热/成像性能的研究[D].青岛:青岛大学,2020.
[30] O’NEAL DP, HIRSCH LR, HALAS NJ, et al. Photo-thermal tumor ablation in mice using near infrared-absorbing nanoparticles. Cancer Lett. 2004; 209(2):171-176.
[31] LOO C, LOWERY A, HALAS N, et al. Immunotargeted nanoshells for integrated cancer imaging and therapy. Nano Lett. 2005;5(4):709-711.
[32] WU S, LI A, ZHAO X, et al. Silica-Coated Gold-Silver Nanocages as Photothermal Antibacterial Agents for Combined Anti-Infective Therapy. ACS Appl Mater Interfaces. 2019;11(19):17177-17183.
[33] LIU T, SHI S, LIANG C, et al. Iron oxide decorated MoS2 nanosheets with double PEGylation for chelator-free radiolabeling and multimodal imaging guided photothermal therapy. ACS Nano. 2015;9(1):950-960.
[34] ZHU X, JI X, KONG N, et al. Intracellular Mechanistic Understanding of 2D MoS2 Nanosheets for Anti-Exocytosis-Enhanced Synergistic Cancer Therapy. ACS Nano. 2018;12(3):2922-2938.
[35] YADAV V, ROY S, SINGH P, et al. 2D MoS2 -Based Nanomaterials for Therapeutic, Bioimaging, and Biosensing Applications. Small. 2019; 15(1):e1803706.
[36] YIN W, YU J, LV F, et al. Functionalized Nano-MoS2 with Peroxidase Catalytic and Near-Infrared Photothermal Activities for Safe and Synergetic Wound Antibacterial Applications. ACS Nano. 2016;10(12): 11000-11011.
[37] GAO Q, ZHANG X, YIN W, et al. Functionalized MoS2 Nanovehicle with Near-Infrared Laser-Mediated Nitric Oxide Release and Photothermal Activities for Advanced Bacteria-Infected Wound Therapy. Small. 2018; 14(45):e1802290.
[38] 杨莹莹,冯闪,马陇豫,等.光热纳米材料在抗菌领域的研究进展[J].河南大学学报(医学版),2021,40(2):147-151.
[39] ZHOU S, WANG Z, WANG Y, et al. Near-Infrared Light-Triggered Synergistic Phototherapy for Antimicrobial Therapy. ACS Appl Bio Mater. 2020;3(3):1730-1737.
[40] PANARIELLO BHD, DE ARAÚJO COSTA CAG, PAVARINA AC, et al. Advances and challenges in oral biofilm control.Curr Oral Health Rep. 2017;4(1):29-33.
[41] PITTS NB, ZERO DT, MARSH PD, et al. Dental caries. Nat Rev Dis Primers. 2017;3:17030.
[42] 莫祯妮,熊盈盈,邱树毅,等.群体感应抑制剂调控食源性微生物生物膜形成的研究进展[J].食品科学,2021,42(17):307-316.
[43] KANG M, KIM S, KIM H, et al. Calcium-Binding Polymer-Coated Poly(lactide-co-glycolide) Microparticles for Sustained Release of Quorum Sensing Inhibitors to Prevent Biofilm Formation on Hydroxyapatite Surfaces. ACS Appl Mater Interfaces. 2019;11(8):7686-7694.
[44] KOO H, HAYACIBARA MF, SCHOBEL BD, et al. Inhibition of Streptococcus mutans biofilm accumulation and polysaccharide production by apigenin and tt-farnesol. J Antimicrob Chemother. 2003;52(5):782-789.
[45] 赵霞,徐嘉昊,夏商.Farnesol纳米胶束的构建及对变形链球菌的抑菌作用研究[J].口腔医学研究,2020,36(9):875-878.
[46] HOREV B, KLEIN MI, HWANG G, et al. pH-activated nanoparticles for controlled topical delivery of farnesol to disrupt oral biofilm virulence. ACS Nano. 2015;9(3):2390-2404.
[47] 黄彦楠,程磊.纳米磷酸钙盐改性牙科材料防治牙体牙髓病研究进展[J].口腔疾病防治,2021,29(9):634-637.
[48] 石广立.甲苯胺蓝-碳纳米管复合光敏剂的合成及其表征[D].沈阳:沈阳理工大学,2015.
[49] 郗红,周惠,闫秀娟,等.纳米技术在龋病治疗中应用的研究进展[J].国际口腔医学杂志,2014,41(5):563-566.
[50] HAO Y, HUANG X, ZHOU X, et al. Influence of Dental Prosthesis and Restorative Materials Interface on Oral Biofilms. Int J Mol Sci. 2018; 19(10):3157.
[51] MANN J, BERNSTEIN Y, FINDLER M. Periodontal disease and its prevention, by traditional and new avenues. Exp Ther Med. 2020;19(2): 1504-1506.
[52] 王兴.第四次全国口腔健康流行病学调查报告[M].北京:人民卫生出版社,2018:25-34.
[53] KAVRIKOVA D, BORILOVA LINHARTOVA P, et al. Chemokine Receptor 2 (CXCR2) Gene Variants and Their Association with Periodontal Bacteria in Patients with Chronic Periodontitis. Mediators Inflamm. 2019;2019: 2061868.
[54] DO NASCIMENTO C, PAULO DF, PITA MS, et al. Microbial diversity of the supra- and subgingival biofilm of healthy individuals after brushing with chlorhexidine- or silver-coated toothbrush bristles. Can J Microbiol. 2015;61(2):112-123.
[55] 张新坚,张斌.纳米粒子递药系统在牙周炎局部药物治疗中应用的研究进展[J].口腔疾病防治,2022,30(1):73-76.
[56] 张灵玲.基于纳米材料的新型光热/药物协同抗菌体系的设计及应用[D].武汉:武汉大学,2019.
[57] 马旭东,王健平.纳米复合羟基磷灰石(nHA)根管充填材料的应用基础研究[J].西南军医,2009,11(3):485-487.
[58] 李平,肖丽英,李伟,等.新型纳米羟基磷灰石(n-HA)糊剂封闭根尖性能及其对病原菌抗菌活性的体外实验[J].牙体牙髓牙周病学杂志,2007,17(4):214-218.
[59] 游滢滢,冯云枝.纳米含氟羟基磷灰石牙种植体的生物相容性[J].中国组织工程研究,2014,18(12):1901-1906.
[60] WANG L, XIE X, LI C, et al. Novel bioactive root canal sealer to inhibit endodontic multispecies biofilms with remineralizing calcium phosphate ions. J Dent. 2017;60:25-35.
[61] 王建平,GEOGI GEORGE.纳米羟基磷灰石复合根充糊剂的抑菌性及微渗漏[J].中国组织工程研究,2014,18(21):3350-3354.
[62] 王昊阳,孟维艳.二氧化钛纳米管抗菌性能在口腔种植领域的研究进展[J].中华老年口腔医学杂志,2021,19(1):49-53.
[63] NILEBÄCK L, WIDHE M, SEIJSING J, et al. Bioactive Silk Coatings Reduce the Adhesion of Staphylococcus aureus while Supporting Growth of Osteoblast-like Cells. ACS Appl Mater Interfaces. 2019;11(28):24999-25007.
[64] PENG Z, NI J, ZHENG K, et al. Dual effects and mechanism of TiO2 nanotube arrays in reducing bacterial colonization and enhancing C3H10T1/2 cell adhesion. Int J Nanomedicine. 2013;8:3093-3105.
[65] 寇钢,白力静,龚振瑶,等.磁控溅射(TiO2 -ZnO) / TiO2梯度复合薄膜的制备及光致亲水性研究[J].人工晶体学报,2012,41(1):94-99.
[66] LIU W, SU P, CHEN S, et al. Antibacterial and osteogenic stem cell differentiation properties of photoinduced TiO₂ nanoparticle-decorated TiO₂ nanotubes. Nanomedicine (Lond). 2015;10(5):713-723.
[67] 马歆茹.多形貌氧化锌对变异链球菌的抑制作用研究[D].遵义:遵义医科大学,2021.
[68] 肖作慧.仿生肽引导纳米无定形磷酸钙再矿化脱矿牙釉质[D].天津:天津医科大学,2018.
[69] 李洁,李福军.复合纳米银托槽粘接剂在大鼠龋病模型上抗菌性的研究[J].口腔医学研究,2016,32(5):449-452.
[70] NI C, ZHOU J, KONG N, et al. Gold nanoparticles modulate the crosstalk between macrophages and periodontal ligament cells for periodontitis treatment. Biomaterials. 2019;206:115-132.
[71] HU F, ZHOU Z, XU Q, et al. A novel pH-responsive quaternary ammonium chitosan-liposome nanoparticles for periodontal treatment. Int J Biol Macromol. 2019;129:1113-1119.
[72] 邓咏梅,王辉,何松霖,等.盐酸米诺环素纳米脂质体治疗大鼠实验性牙周炎的疗效观察[J]. 实用口腔医学杂志,2018,34(6):753-757.
[73] 齐曼霖.近红外光激发的二氧化钛纳米粒子对牙周炎相关细菌的抗菌性能的研究[D].长春:吉林大学,2020.
[74] 刘奕,周荣静,吴红崑.4种纳米羟磷灰石复合材料对粪肠球菌抗菌性能的初步研究[J].华西口腔医学杂志,2015,32(3):301-305.
[75] 姚丽萍,张蕾,林玉红,等.纳米银溶液用于慢性根尖周炎根管内封药的实验动物研究[J].中华口腔医学研究杂志(电子版),2020, 14(2):95-100.
[76] IBRAHIM MS, ALQARNI FD, AL-DULAIJAN YA, et al. Tuning Nano-Amorphous Calcium Phosphate Content in Novel Rechargeable Antibacterial Dental Sealant. Materials (Basel). 2018;11(9):1544.
[77] DARABPOUR E, KASHEF N, MASHAYEKHAN S. Chitosan nanoparticles enhance the efficiency of methylene blue-mediated antimicrobial photodynamic inactivation of bacterial biofilms: An in vitro study. Photodiagnosis Photodyn Ther. 2016;14:211-217.
[78] POURHAJIBAGHER M, ROKN AR, ROSTAMI-RAD M, et al. Monitoring of virulence factors and metabolic activity in Aggregatibacter actinomycetemcomitans cells surviving antimicrobial photodynamic therapy via nano-chitosan encapsulated indocyanine green. Front Phys. 2018;6:124.
[79] SASAKI Y, HAYASHI JI, FUJIMURA T, et al. New Irradiation Method with Indocyanine Green-Loaded Nanospheres for Inactivating Periodontal Pathogens. Int J Mol Sci. 2017;18(1):154.
[80] GOLMOHAMADPOUR A, BAHRAMIAN B, KHOOBI M, et al. Antimicrobial photodynamic therapy assessment of three indocyanine green-loaded metal-organic frameworks against Enterococcus faecalis. Photodiagnosis Photodyn Ther. 2018;23:331-338.
[81] WU Z, XU H, XIE W, et al. Study on a novel antibacterial light-cured resin composite containing nano-MgO. Colloids Surf B Biointerfaces. 2020;188:110774.
[82] KO A, YEE M, SKUPIN-MRUGALSKA P, et al. Photodynamic therapy of Porphyromonas gingivalis via liposome-encapsulated sensitizers. J Calif Dent Assoc. 2013;41(11):827-830.
[83] 曹飞,惠敏,董西玲,等.载银纳米羟基磷灰石/聚己内酯复合纳米纤维支架的制备及成骨抗菌性能[J].中国组织工程研究,2022, 26(34):5461-5467.
[84] 王静,冀志江,水中和,等.纳米银溶胶与大肠杆菌作用及作用机理研究[J].材料导报,2013,27(24):4-8,21.
[85] 姬晓伟,刘娉婷,唐金成,等.二氧化钛纳米管阵列在大肠杆菌不同生长阶段的抗菌机理[J].中国有色金属学报(英文版),2021, 31(12):3821-3830.
[86] 程晓昆,张越,吕海军,等.多孔碳纳米材料构建抗肿瘤药物靶向传递系统的研究进展[J].无机材料学报,2021,36(1):9-24.
[87] 丁鑫,师红东,刘扬中.以人血清白蛋白为载体的Ru(Ⅲ)和全反式维甲酸共运输纳米药物的构建及抗肿瘤转移作用[J].高等学校化学学报,2021,42(10):3040-3046.
[88] 张颖,许霞青,何勐,等.富勒烯-苯丙氨酸多西他赛纳米脂质载体的制备及其体外抗肿瘤活性[J].医药导报,2022,41(4):506-513.
[89] 刘红梅,黄开勋,徐辉碧.纳米材料的生物安全性研究进展[J].化工进展,2006,25(9):1040-1044.
[90] 徐斐,姜昆,黎燕,等.食物基质和胃肠道对经口暴露纳米颗粒物理化学性质和生物效应的影响[J].食品与生物技术学报,2021,40(8): 17-26.
[91] HAN HY, YANG MJ, YOON C, et al. Toxicity of orally administered food-grade titanium dioxide nanoparticles. J Appl Toxicol. 2021;41(7):1127-1147.
[92] 王嘉,吴国锋,孙冠阳,等.经皮种植体表面纳米二氧化硅抗菌涂层的研究[J].实用口腔医学杂志,2017,33(1):5-9.
[93] WONG HL, CHATTOPADHYAY N, WU XY, et al. Nanotechnology applications for improved delivery of antiretroviral drugs to the brain. Adv Drug Deliv Rev. 2010;62(4-5):503-517.
[94] QIN W, HUANG G, CHEN Z, et al. Nanomaterials in Targeting Cancer Stem Cells for Cancer Therapy. Front Pharmacol. 2017;8:1.
[95] DEVADASU VR, BHARDWAJ V, KUMAR MN. Can controversial nanotechnology promise drug delivery? Chem Rev. 2013;113(3):1686-1735.
[96] KIM CS, DUNCAN B, CRERAN B, et al. Triggered Nanoparticles as Therapeutics. Nano Today. 2013;8(4):439-447.
[97] STUART MA, HUCK WT, GENZER J, et al. Emerging applications of stimuli-responsive polymer materials. Nat Mater. 2010;9(2):101-113. |