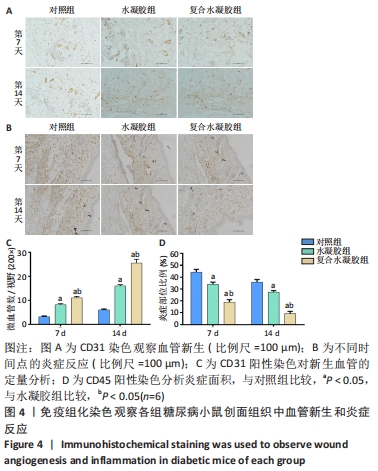
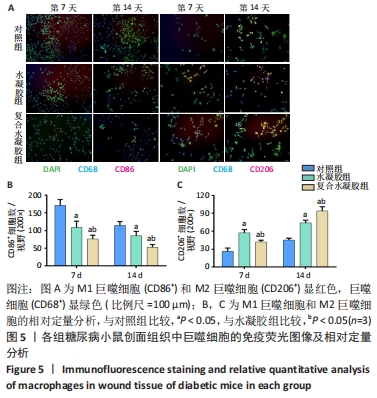
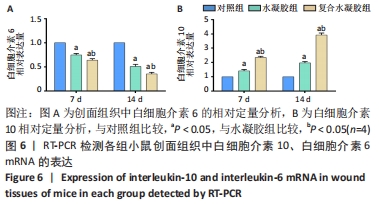
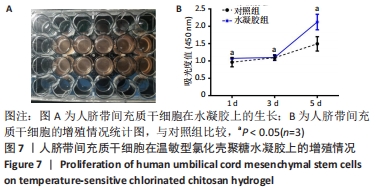
[1] DONG Y, RODRIGUES M, KWON SH, et al. Acceleration of Diabetic Wound Regeneration using an In Situ-Formed Stem-Cell-Based Skin Substitute. Adv Healthc Mater. 2018;7(17):e1800432.
[2] HYLDIG K, RIIS S, PENNISI CP, et al. Implications of Extracellular Matrix Production by Adipose Tissue-Derived Stem Cells for Development of Wound Healing Therapies. Int J Mol Sci. 2017;18(6):1167.
[3] MIYAGAWA I, NAKAYAMADA S, KONDO M, et al. Regulatory Mechanism of The Induction of Regulatory T Cells through Growth Factors Released by Human Mesenchymal Stem Cells. Crit Rev Immunol. 2018;38(6): 471-478.
[4] WANG F, TANG H, ZHU J, et al. Transplanting Mesenchymal Stem Cells for Treatment of Ischemic Stroke. Cell Transplant. 2018;27(12):1825-1834.
[5] LOPES L, SETIA O, AURSHINA A, et al. Stem cell therapy for diabetic foot ulcers: a review of preclinical and clinical research. Stem Cell Res Ther. 2018;9(1):188.
[6] ZHANG B, WU X, ZHANG X, et al. Human umbilical cord mesenchymal stem cell exosomes enhance angiogenesis through the Wnt4/β-catenin pathway. Stem Cells Transl Med. 2015;4(5):513-522.
[7] KANDHWAL M, BEHL T, KUMAR A, et al. Understanding the Potential Role and Delivery Approaches of Nitric Oxide in Chronic Wound Healing Management. Curr Pharm Des. 2021;27(17):1999-2014.
[8] LIU C, GE HM, LIU BH, et al. Targeting pericyte-endothelial cell crosstalk by circular RNA-cPWWP2A inhibition aggravates diabetes-induced microvascular dysfunction. Proc Natl Acad Sci U S A. 2019; 116(15):7455-7464.
[9] GAO W, JIN W, LI Y, et al. A highly bioactive bone extracellular matrix-biomimetic nanofibrous system with rapid angiogenesis promotes diabetic wound healing. J Mater Chem B. 2017;5(35):7285-7296.
[10] WANG C, WANG M, XU T, et al. Engineering Bioactive Self-Healing Antibacterial Exosomes Hydrogel for Promoting Chronic Diabetic Wound Healing and Complete Skin Regeneration. Theranostics. 2019; 9(1):65-76.
[11] ISHIHARA J, ISHIHARA A, STARKE RD, et al. The heparin binding domain of von Willebrand factor binds to growth factors and promotes angiogenesis in wound healing. Blood. 2019;133(24):2559-2569.
[12] QIAN Z, WANG H, BAI Y, et al. Improving Chronic Diabetic Wound Healing through an Injectable and Self-Healing Hydrogel with Platelet-Rich Plasma Release. ACS Appl Mater Interfaces. 2020;12(50):55659-55674.
[13] WANG T, LIAO Q, WU Y, et al. A composite hydrogel loading natural polysaccharides derived from Periplaneta americana herbal residue for diabetic wound healing. Int J Biol Macromol. 2020;164:3846-3857.
[14] XU Q, GUO L, A S, et al. Injectable hyperbranched poly(β-amino ester) hydrogels with on-demand degradation profiles to match wound healing processes. Chem Sci. 2018;9(8):2179-2187.
[15] SHI Q, QIAN Z, LIU D, et al. GMSC-Derived Exosomes Combined with a Chitosan/Silk Hydrogel Sponge Accelerates Wound Healing in a Diabetic Rat Skin Defect Model. Front Physiol. 2017;8:904.
[16] LIU X, YANG Y, LI Y, et al. Integration of stem cell-derived exosomes with in situ hydrogel glue as a promising tissue patch for articular cartilage regeneration. Nanoscale. 2017;9(13):4430-4438.
[17] ANNABI N, RANA D, SHIRZAEI SANI E, et al. Engineering a sprayable and elastic hydrogel adhesive with antimicrobial properties for wound healing. Biomaterials. 2017;139:229-243.
[18] SHADRIN IY, ALLEN BW, QIAN Y, et al. Cardiopatch platform enables maturation and scale-up of human pluripotent stem cell-derived engineered heart tissues. Nat Commun. 2017;8(1):1825.
[19] ACHARYA D, LOYAGA-RENDON RY, PAMBOUKIAN SV, et al. Ventricular Assist Device in Acute Myocardial Infarction. J Am Coll Cardiol. 2016; 67(16):1871-1880.
[20] YU Y, HU Z, LI B, et al. Ivabradine improved left ventricular function and pressure overload-induced cardiomyocyte apoptosis in a transverse aortic constriction mouse model. Mol Cell Biochem. 2019;450(1-2):25-34.
[21] PRABHAKAR PK, DOBLE M. Mechanism of action of natural products used in the treatment of diabetes mellitus. Chin J Integr Med. 2011; 17(8):563-574.
[22] SHARMA P, KUMAR A, DEY AD, et al. Stem cells and growth factors-based delivery approaches for chronic wound repair and regeneration: A promise to heal from within. Life Sci. 2021;268:6212-6225.
[23] HYLDIG K, RIIS S, PENNISI CP, et al. Implications of extracellular matrix production by adipose tissue-derived stem cells for development of wound healing therapies. Int J Mol Sci. 2017;18(6):1167-1177.
[24] EMING SA, MARTIN P, TOMIC-CANIC M. Wound repair and regeneration: mechanisms, signaling, and translation. Sci Transl Med. 2014;6(265):265-280.
[25] WANG T, LIAO Q, WU Y, et al. A composite hydrogel loading natural polysaccharides derived from Periplaneta americana herbal residue for diabetic wound healing. Int J Biol Macromol. 2020;164:3846-3857.
[26] ZHANG S, LIU Y, ZHANG X, et al. Prostaglandin E2 hydrogel improves cutaneous wound healing via M2 macrophages polarization. Theranostics. 2018;8(19):5348-5361.
[27] YANAGIBAYASHI S, KISHIMOTO S, ISHIHARA M, et al. Novel hydrocolloid-sheet as wound dressing to stimulate healing-impaired wound healing in diabetic db/db mice. Biomed Mater Eng. 2012;22(5):301-310.
[28] EL HOSARY R, EL-MANCY SMS, EL DEEB KS, et al. Efficient wound healing composite hydrogel using Egyptian Avena sativa L. polysaccharide containing β-glucan. Int J Biol Macromol. 2020;149:1331-1338.
[29] XIE H, CHEN X, SHEN X, et al. Preparation of chitosan-collagen-alginate composite dressing and its promoting effects on wound healing. Int J Biol Macromol. 2018;107(Pt A):93-104.
[30] GEORGE SM, TANDON S, KANDASUBRAMANIAN B. Advancements in Hydrogel-Functionalized immunosensing platforms. ACS Omega. 2020;5(5):2060-2068.
[31] CHEN H, CHENG R, ZHAO X, et al. An injectable self-healing coordinative hydrogel with antibacterial and angiogenic properties for diabetic skin wound repair. NPG Asia Mater.2019;11(3):18-29.
[32] KAISANG L, SIYU W, LIJUN F, et al. Adipose-derived stem cells seeded in Pluronic F-127 hydrogel promotes diabetic wound healing. J Surg Res. 2017;217:63-74.
[33] LI H, FENG Y, ZHENG X, et al. M2-type exosomes nanoparticles for rheumatoid arthritis therapy via macrophage re-polarization. J Control Release. 2021;341:16-30.
[34] KIM H, WANG SY, KWAK G, et al. Exosome-Guided Phenotypic Switch of M1 to M2 Macrophages for Cutaneous Wound Healing. Adv Sci (Weinh). 2019;6(20):1900513.
[35] WANG Y, MACK JA, MAYTIN EV. CD44 inhibits α-SMA gene expression via a novel G-actin/MRTF-mediated pathway that intersects with TGFβ R/p38MAPK signaling in murine skin fibroblasts. J Biol Chem. 2019; 294(34):12779-12794.
[36] ZHANG S, LIU Y, ZHANG X,et al. Prostaglandin E2 hydrogel improves cutaneous wound healing via M2 macrophages polarization. Theranostics. 2018;8(19):5348-5361.
|