[1] HOMASSEN A, WERNBERG M. Prevalence and prognostic significance of coma after cardiac arrest outside intensive care and coronary units. Acta Anaesthesiol Scand. 1979;23(2):143-148.
[2] LAVER S, FARROW C, TURNER D, et al. Mode of death after admission to an intensive care unit following cardiac arrest. Intensive Care Med. 2004;30(11):2126-2128.
[3] LEMIALE V, DUMAS F, MONGARDON N, et al.Intensive care unit mortality after cardiac arrest: the relative contribution of shock and brain injury in a large cohort. Intensive Care Med. 2013;39(11):1972-1980.
[4] DRAGANCEA I, WISE MP, AL-SUBAIE N, et al. TTM trial investigators. Protocol-driven neurological prognostication and withdrawal of life-sustaining therapy after cardiac arrest and targeted temperature management. Resuscitation. 2017;117:50-57.
[5] KRÄMER TJ, HACK N, BRÜHL TJ, et al. Depletion of regulatory T cells increases T cell brain infiltration, reactive astrogliosis, and interferon-γ gene expression in acute experimental traumatic brain injury. J Neuroinflammation. 2019;16(1):163.
[6] ASHTON NJ, HYE A, RAJKUMAR AP, et al. An update on blood-based biomarkers for non-Alzheimer neurodegenerative disorders. Nat Rev Neurol 2020;16:265-284.
[7] NOVAKOVA L, AXELSSON M, KHADEMI M, et al. Cerebrospinal fluid biomarkers as a measure of disease activity and treatment efficacy in relapsing-remitting multiple sclerosis. JNeurochem 2017;141:296-304.
[8] FUGATE JE, WIJDICKS EF, MANDREKAR J, et al. Predictors of neurologic outcome in hypothermia after cardiac arrest. Ann Neurol. 2010;68(6): 907-914.
[9] NIELSEN N, WETTERSLEV J, CRONBERG T, et al; TTM Trial Investigators.Targeted temperature management at 33°C versus 36°C after cardiac arrest. N Engl J Med. 2013;369(23):2197-2206.
[10] PFEIFER R, FRANZ M, FIGULLA HR. Hypothermia after cardiac arrest does not affect serum levels of neuron-specific enolase and protein S-100b. Acta Anaesthesiol Scand. 2014;58(9):1093-1100.
[11] HUNTGEBURTH M, ADLER C, ROSENKRANZ S, et al. Changes in neuronspecific enolase are more suitable than its absolute serum levels for the prediction of neurologic outcome in hypothermiatreated patients with outofhospital cardiac arrest. Neurocrit Care. 2014;20(3): 358-366.
[12] STORM C, NEE J, JÖRRES A, et al. Serial measurement of neuron specific enolase improves prognostication in cardiac arrest patients treated with hypothermia: a prospective study. Scand J Trauma Resusc Emerg Med. 2012;20:6.
[13] SANDRONI C, D’ARRIGO S, CACCIOLA S, et al.Prediction of poor neurological outcome in comatose survivors of cardiac arrest: a systematic review. Intensive Care Med. 2020;46(10):1803-1851.
[14] VONDRAKOVA D, KRUGER A, JANOTKA M, et al. Association of neuron-specific enolase values with outcomes in cardiac arrest survivors is dependent on the time of sample collection. Crit Care. 2017;21(1):172.
[15] NOLAN JP, CARIOU A. Post-resuscitation care: ERC–ESICM guidelines 2015. Intensive Care Med. 2015;41(12):2204-2206.
[16] RUNDGREN M, CRONBERG T, FRIBERG H, et al. Serum neuron specific enolase - impact of storage and measuring method. BMC Res Notes. 2014;7:726.
[17] MLYNASH M, BUCKWALTER MS, OKADA A, et al. Serum neuron-specific enolase levels from the same patients differ between laboratories:assessment of a prospective post-cardiac arrest cohort. Neurocrit Care. 2013;19(2):161-166.
[18] REZAEI O, PAKDAMAN H, GHAREHGOZLI K, et al. S100 B: A new concept in neurocritical care. Iran J Neurol. 2017;16(2):83-89.
[19] SORCI G, RIUZZI F, ARCURI C, et al. S100B protein in tissue development, repair and regeneration. World J Biol Chem. 2013;4(1):1-12.
[20] DUEZ CHV, GREJS AM, JEPPESEN AN, et al. Neuron-specific enolase and S-100b in prolonged targeted temperature management after cardiac arrest: A randomised study. Resuscitation. 2018;122:79-86.
[21] JANG JH, PARK WB, LIM YS, et al.Combination of S100B and procalcitonin improves prognostic performance compared to either alone in patients with cardiac arrest: A prospective observational study. Medicine (Baltimore). 2019;98(6):e14496.
[22] DEYE N, NGUYEN P, VODOVAR N, et al.. Protein S100B as a reliable tool for early prognostication after cardiac arrest. Resuscitation. 2020; 156:251-259.
[23] KANEKO T, KASAOKA S, MIYAUCHI T, et al. Serum glial fibrillary acidic protein as a predictive biomarker of neurological outcome after cardiac arrest. Resuscitation. 2009;80:790-794.
[24] LARSSON IM, WALLIN E, KRISTOFFERZON ML, et al. Post-cardiac arrest serum levels of glial fibrillary acidic protein for predicting neurological outcome. Resuscitation. 2014;85:1654-1661.
[25] HELWIG K, SEEGER F, HÖLSCHERMANN H, et al.Elevated Serum Glial Fibrillary Acidic Protein (GFAP) is Associated with Poor Functional Outcome After Cardiopulmonary Resuscitation. Neurocrit Care. 2017; 27(1):68-74.
[26] MO¨RTBERG E, ZETTERBERG H, NORDMARK J, et al. S-100B is superior to NSE, BDNF and GFAP in predicting outcome of resuscitation from cardiac arrest with hypothermia treatment. Resuscitation. 2011;82(1): 26-31.
[27] GUL SS, HUESGEN KW, WANG KK, et al.Prognostic utility of neuroinjury biomarkers in post out-of-hospital cardiac arrest (OHCA) patient management. Med Hypotheses. 2017;105:34-47.
[28] VENKATRAMANI A, PANDA D. Regulation of neuronal microtubule dynamics by tau: Implications for tauopathies. Int J Biol Macromol. 2019;133:473-483.
[29] SHARMA HS, MICLESCU A, WIKLUND L. Cardiac arrest-induced regional blood-brain barrier breakdown, edema formation and brain pathology: a light and electron microscopic study on a new model for neurodegeneration and neuroprotection in porcine brain. J Neural Transm (Vienna). 2011;118:87-114.
[30] MÖRTBERG E, ZETTERBERG H, NORDMARK J, et al. Plasma tau protein in comatose patients after cardiac arrest treated with therapeutic hypothermia. Acta Anaesthesiol. Scand. 2011;55(9):1132-1138.
[31] MATTSSON N, ZETTERBERG H, NIELSEN N, et al. Serum tau and neurological outcome in cardiac arrest. Ann Neurol. 2017;82(5):665-675.
[32] HASSLACHER J, RASS V, BEER R, Et al. Serum tau as a predictor for neurological outcome after cardiopulmonary resuscitation. Resuscitation. 2020;148:207-214.
[33] THELIN EP, ZEILER FA, ERCOLE A, et al. Serial Sampling of Serum Protein Biomarkers for Monitoring Human Traumatic Brain Injury Dynamics: A Systematic Review. Front Neurol. 2017;8:300.
[34] LIU H, POVYSHEVA N, ROSE ME, et al. Role of UCHL1 in axonal injury and functional recovery after cerebral ischemia. Proc Natl Acad Sci U S A. 2019;116(10):4643-4650.
[35] WANG KK, YANG Z, ZHU T, et al. An update on diagnostic and prognostic biomarkers for traumatic brain injury. Expert Rev Mol Diagn. 2018;18:165-180.
[36] EBNER F, MOSEBY-KNAPPE M, MATTSSON-CARLGREN N, et al.Serum GFAP and UCH-L1 for the prediction of neurological outcome in comatose cardiac arrest patients. Resuscitation. 2020;154:61-68.
[37] KHALIL M, TEUNISSEN CE, OTTO M, et al.Neurofilaments as biomarkers in neurological disorders. Nat Rev Neurol. 2018;14:577-589.
[38] KEIJZER HM, HOEDEMAEKERS CWE, MEIJER FJA, et al.Brain imaging in comatose survivors of cardiac arrest: Pathophysiological correlates and prognostic properties. Resuscitation. 2018;133:124-136.
[39] KIRSCHEN MP, YEHYA N, GRAHAM K, et al.Circulating Neurofilament Light Chain Is Associated With Survival After Pediatric Cardiac Arrest. Pediatr Crit Care Med. 2020;21(7):656-661.
[40] MOSEBY-KNAPPE M, MATTSSON N, NIELSEN N, et al.Serum Neurofilament Light Chain for Prognosis of Outcome After Cardiac Arrest. JAMA Neurol. 2019;76(1):64-71.
[41] IZZOTTI A, LONGOBARDI M, LA MAESTRA S, et al. Release of microRNAs into body fluids from ten organs of mice exposed to cigarette smoke. Theranostics. 2018;8:2147-2160.
[42] DE GONZALO-CALVO D, IGLESIAS-GUTIÉRREZ E, LLORENTE-CORTÉS V. Epigenetic biomarkers and cardiovascular disease: Circulating microRNAs. Rev Esp Cardiol(Engl. Ed.). 2017;70:763-769.
[43] KIM YK. Extracellular microRNAs as biomarkers in human disease. Chonnam Med J. 2015;51:51-57.
[44] YUAN Y, WANG JY, XU LY, et al. MicroRNA expression changes in the hippocampi of rats subjected to global ischemia. J Clin Neurosci. 2010;17(6):774-778 .
[45] OUYANG YB, STARY CM, YANG GY, et al. microRNAs: innovative targets for cerebral ischemia and stroke. Curr Drug T argets. 2013;14(1):90-101.
[46] STAMMET P, GORETTI E, VAUSORT M, et al. Circulating microRNAs after cardiac arrest. Crit Care Med. 2012;40(12):3209-3214 .
[47] DEVAUX Y, DANKIEWICZ J, SALGADO-SOMOZA A, et al. Association of circulating microrna-124-3p levels with outcomes after out-of-hospital cardiac arrest: A substudy of a randomized clinical trial. JAMA Cardiol. 2016;1:305-313.
[48] GILJE P, GIDLÖF O, RUNDGREN M, et al. The brain-enriched microRNA miR-124 in plasma predicts neurological outcome after cardiac arrest. Crit Care. 2014;18:R40.
[49] DEVAUX Y, SALGADO-SOMOZA A, DANKIEWICZ J, et al. TTM-trial investigators. Incremental Value of Circulating MiR-122-5p to Predict Outcome after Out of Hospital Cardiac Arrest. Theranostics. 2017;7(10):2555-2564.
[50] STEFANIZZI FM, NIELSEN N, ZHANG L, et al. Circulating Levels of Brain-Enriched MicroRNAs Correlate with Neuron Specific Enolase after Cardiac Arrest-A Substudy of the Target Temperature Management Trial. Int J Mol Sci. 2020;21(12):4353.
[51] SOHEL MH. Extracellular/circulating microRNAs: release mechanisms, functions and challenges. Achievem. Life Sci. 2016;10(2):175-186.
[52] WIHERSAARI L, ASHTON NJ, REINIKAINEN M, JAKKULA P, et al. Neurofilament light as an outcome predictor after cardiac arrest: a post hoc analysis of the COMACARE trial. Intensive Care Med. 2021;47(1):39-48.
[53] KUHLE J, BARRO C, ANDREASSON U, et al. Comparison of three analytical platforms for quantification of the neurofilament light chain in blood samples: ELISA, electrochemiluminescence immunoassay and Simoa. Clin Chem Lab Med. 2016;54:1655-1661.
[54] BAZARIAN JJ, BIBERTHALER P, WELCH RD, et al. Serum GFAP and UCH-L1 for prediction of absence of intracranial injuries on head CT (ALERT-TBI): a multicentre observational study. Lancet Neurol. 2018;17: 782-789. |
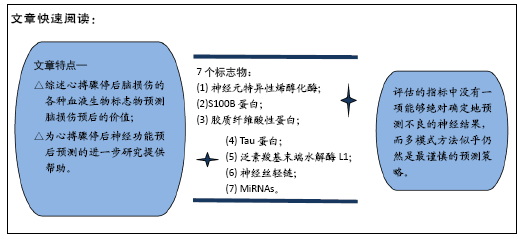

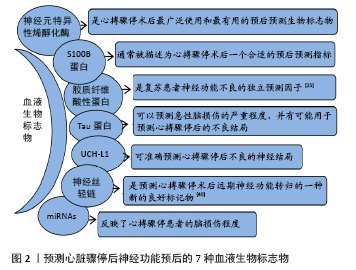 文章综述了几个用于预测神经功能结局的新指标的应用与进展,虽然对心搏骤停后神经功能结局的预测有一定的参考价值,但尚未获得有关学者及临床工作者的普遍认可,再加上心脏骤停后脑损伤机制及脑复苏后病理生理变化过程非常复杂,而用于评估心搏骤停后神经功能结局的指标、标准操作流程尚未达成共识,因此仍需要大样本多中心的临床研究来进一步证实上述指标对神经功能预后评估的有效性及准确性,对这些指标进行再优化、筛选,遴选出客观的评价指标,准确、全面地评估预测神经功能结局,为临床医师提供预测神经功能预后的合理策略及规范流程,指导临床医师对患者的治疗。
文章综述了几个用于预测神经功能结局的新指标的应用与进展,虽然对心搏骤停后神经功能结局的预测有一定的参考价值,但尚未获得有关学者及临床工作者的普遍认可,再加上心脏骤停后脑损伤机制及脑复苏后病理生理变化过程非常复杂,而用于评估心搏骤停后神经功能结局的指标、标准操作流程尚未达成共识,因此仍需要大样本多中心的临床研究来进一步证实上述指标对神经功能预后评估的有效性及准确性,对这些指标进行再优化、筛选,遴选出客观的评价指标,准确、全面地评估预测神经功能结局,为临床医师提供预测神经功能预后的合理策略及规范流程,指导临床医师对患者的治疗。