中国组织工程研究 ›› 2018, Vol. 22 ›› Issue (15): 2396-2406.doi: 10.3969/j.issn.2095-4344.0760
• 骨与关节综述 bone and joint review • 上一篇 下一篇
髋关节股骨侧翻修:原因、分型及不同修复技术的应用原则
冯 硕,查国春,郭开今,陈向阳
- 徐州医科大学附属医院骨科,江苏省徐州市 221000
-
出版日期:2018-05-28发布日期:2018-05-28 -
通讯作者:陈向阳,博士,主任医师,徐州医科大学附属医院骨科,江苏省徐州市 221000 -
作者简介:冯硕,男,1993年生,安徽省宿州市人,汉族,徐州医科大学在读硕士,目前从事骨关节及脊柱外科等方面的研究。 -
基金资助:江苏省青年医学人才项目(QNRC2016800);徐州市科技计划项目(KC16SL111);江苏省卫计委面上项目(H2017081);江苏省级社会发展重点项目(BE2015627)
Femoral revision of the hip: reason, type and different techniques
Feng Shuo, Zha Guo-chun, Guo Kai-jin, Chen Xiang-yang
- Department of Orthopedics, Affiliated Hospital of Xuzhou Medical University, Xuzhou 221000, Jiangsu Province, China
-
Online:2018-05-28Published:2018-05-28 -
Contact:Chen Xiang-yang, M.D., Chief physician, Department of Orthopedics, Affiliated Hospital of Xuzhou Medical University, Xuzhou 221000, Jiangsu Province, China -
About author:Feng Shuo, Master candidate, Department of Orthopedics, Affiliated Hospital of Xuzhou Medical University, Xuzhou 221000, Jiangsu Province, China -
Supported by:the Youth Medical Talent Project of Jiangsu Province, No. QNRC2016800; the Science and Technology Project of Xuzhou City, No. KC16SL111; the General Program of Health Planning Commission of Jiangsu Province, No. H2017081; the Key Project for Social Development in Jiangsu Province, No. BE2015627
摘要:
文章快速阅读:
.jpg)
中图分类号:
引用本文
冯 硕,查国春,郭开今,陈向阳. 髋关节股骨侧翻修:原因、分型及不同修复技术的应用原则[J]. 中国组织工程研究, 2018, 22(15): 2396-2406.
Feng Shuo, Zha Guo-chun, Guo Kai-jin, Chen Xiang-yang . Femoral revision of the hip: reason, type and different techniques[J]. Chinese Journal of Tissue Engineering Research, 2018, 22(15): 2396-2406.
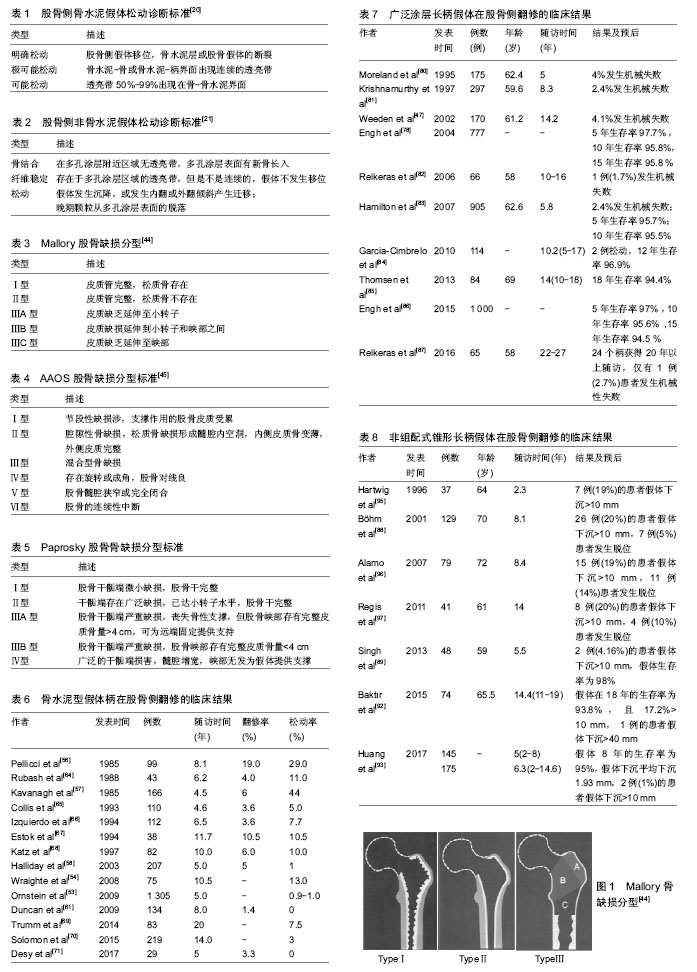
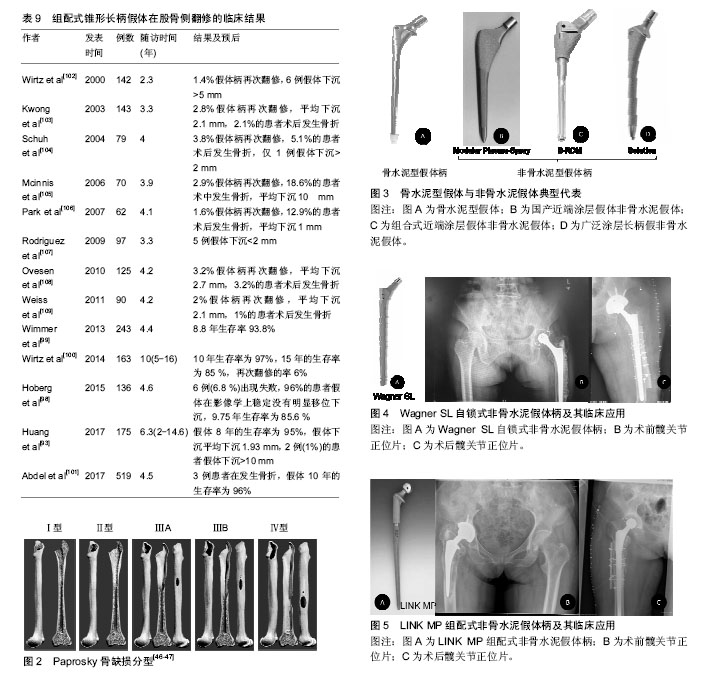
| [1] Callaghan JJ, Bracha P, Liu SS. Survivorship of a Charnley total hip arthroplasty. A concise follow-up, at a minimum of thirty-five years, of previous reports. J Bone Joint Surg Am.2009;91(11): 2617.[2] Parvizi J, Sullivan T, Duffy G, et al. Fifteen-year clinical survivorship of Harris-Galante total hip arthroplasty. J Arthroplasty. 2004;19(6): 672-677.[3] Kurtz SM, Ong KL, Schmier J, et al. Future clinical and economic impact of revision total hip and knee arthroplasty. J Bone Joint Surg Am.2007;89(Suppl 3): 144-151.[4] Kurtz S, Ong K, Lau E, et al. Projections of primary and revision hip and knee arthroplasty in the United States from. J Bone Joint Surg Am. 2005;87(7): 1487-1497.[5] Patel A, Pavlou G, Mújicamota RE, et al. The epidemiology of revision total knee and hip arthroplasty in England and Wales. Bone Joint J. 2015;97-B(8): 1076.[6] Sporer SM, Paprosky WG, O'Rourke MR. Managing bone loss in acetabular revision. J Bone Joint Surg Am.2005;55(7): 287-297.[7] Haddad FS, Rayan F. The role of impaction grafting: the when and how. Orthopedics. 2009;32(9). doi: 10.3928/01477447-20090728-19. [8] Bozic KJ, Durbhakula S, Berry DJ, et al. Differences in patient and procedure characteristics and hospital resource use in primary and revision total joint arthroplasty: a multicenter study. J Arthroplasty. 2005;20(7 Suppl 3): 17-25.[9] Prokopetz Julian JZ, Elena L, Bliss RL, et al. Risk factors for revision of primary total hip arthroplasty: a systematic review.BMC Musculoskelet Disord. 2012;13(1): 251.[10] Wright EA, Katz JN, Baron JA, et al. Risk factors for revision of primary total hip replacement: results from a national case-control study. Arthritis Care Res. 2012;64(12):1879-1885.[11] 王强,杨民,徐祝军.全髋置换影响应力遮挡效应的相关因素[J].中国组织工程研究与临床康复,2009,13(4):739-742.[12] Piao C, Wu D, Luo M, et al. Stress shielding effects of two prosthetic groups after total hip joint simulation replacement. J Orthop Surg Res. 2014;9(1): 1-8.[13] Gwam CU, Mistry JB, Mohamed NS, et al. Current epidemiology of revision total hip arthroplasty in the United States: National Inpatient Sample 2009 to 2013. J Arthroplasty. 2017.[14] 郝云甲.人工髋关节翻修术中股骨侧骨缺损的处理及假体的选择[D].吉林大学, 2014.[15] 简小飞.远端生物固定翻修柄在非感染性高龄患者髋关节股骨侧翻修中的应用[J].武汉大学, 2015.[16] Boyce BF, Li P, Yao Z, et al. TNF-alpha and pathologic bone resorption. Keio J Med. 2005;54(3): 127.[17] Münger P, Röder C, Ackermann-Liebrich U, et al. Patient-related risk factors leading to aseptic stem loosening in total hip arthroplasty: A case-control study of 5,035 patients. Acta Orthop. 2006;77(4): 567.[18] Hanna SA, Mccalden RW, Somerville L, et al. Morbid obesity is a significant risk of failure following revision total hip arthroplasty. J Arthroplasty. 2017.[19] Godoysantos AL, D'Elia CO, Teixeira WJ, et al. Aseptic loosening of total hip arthroplasty: preliminary genetic investigation. J Arthroplasty. 2009;24(2): 297.[20] Harris WH, Jr MCJ, O'Neill DA. Femoral component loosening using contemporary techniques of femoral cement fixation. J Bone Joint Surg Am. 1982;64(7): 1063.[21] Engh CA, Bobyn JD, Glassman AH. Porous-coated hip replacement. The factors governing bone ingrowth, stress shielding, and clinical results. J Bone Joint Surg Bm.1987;69(1): 45.[22] Hartman CW, Garvin KL. Femoral fixation in revision total hip arthroplasty. J Bone Joint Surg Am. 2011;93(24): 2311-2322.[23] Bozic KJ, Kurtz SM, Lau E, et al. The epidemiology of revision total hip arthroplasty in the United States. J Bone Joint Surg Am.2009; 91(1): 128-133.[24] Havelin LI, Fenstad AM, Salomonsson R, et al. The Nordic Arthroplasty Register Association. Acta Orthop. 2009;80(4): 393-401.[25] Ong KL, Kurtz SM, Lau E, et al. Prosthetic joint infection risk after total hip arthroplasty in the Medicare population. J Arthroplasty.2009;24 (6 Suppl):105.[26] Lee KJ, Goodman SB. Identification of periprosthetic joint infection after total hip arthroplasty. J Orthop Trans. 2015;3(1): 21-25.[27] Singh PK, Parsek MR, Greenberg EP, et al. A component of innate immunity prevents bacterial biofilm development. Nature. 2002; 417(6888): 552-555.[28] Tokarski AT, Novack TA, Parvizi J. Is tantalum protective against infection in revision total hip arthroplasty? Bone Joint J. 2015;97-B(1):45.[29] Pulido L, Ghanem E, Joshi A, et al. Periprosthetic joint infection: the incidence, timing, and predisposing factors. Clin Orthop Relat Res. 2008;466(7): 1710-1715.[30] Namba RS, Inacio MC, Paxton EW. Risk factors associated with deep surgical site infections after primary total knee arthroplasty: an analysis of 56,216 knees. J Bone Joint Surg Am. 2013;95(9): 775.[31] Fernández-Fairen M, Hernández-Vaquero D, Murcia-Mazón A, et al. Inestabilidad de la artroplastia total de cadera. Una aproximación desde los criterios de la evidencia científica. Revista Espaola De Cirugía Ortopédica Y Traumatología. 2011;55(6): 460-475.[32] Capóngarcía D, Lópezpardo A, Alvespérez MT. Causes for revision surgery in total hip replacement. A retrospective epidemiological analysis. Revista Española De Cirugía Ortopédica Y Traumatología. 2016;60(3):160-166.[33] Sanzreig J, Lizaurutrilla A, Mirallesmuñoz F. Risk factors for total hip arthroplasty dislocation and its functional outcomes. Revista Española De Cirugía Ortopédica Y Traumatología. 2015;59(1): 19-25.[34] Amlie E, Høvik Ø, Reikerås O. Dislocation after total hip arthroplasty with 28 and 32-mm femoral head. J Orthop Traumatol. 2010;11(2): 111-115.[35] Lewinnek GE, Lewis JL, Tarr R, et al. Dislocations after total hip-replacement arthroplasties. J Bone Joint Surg Am.1978;60(2): 217.[36] Maruyama M, Feinberg JR, Capello WN, et al. The Frank Stinchfield Award: Morphologic features of the acetabulum and femur: anteversion angle and implant positioning. Clin Orthop Relat Res. 2001;393(393): 52.[37] Dorr LD, Malik A, Dastane M, et al. Combined anteversion technique for total hip arthroplasty. Clin Orthop Relat Res. 2009;467(1): 119-127.[38] Mcgrory BJ, Morrey BF, Cahalan TD, et al. Effect of femoral offset on range of motion and abductor muscle strength after total hip arthroplasty. J Bone Joint Surg Am.1995;77(6):865-869.[39] G L, MH F, R P, et al. Femoral offset: anatomical concept, definition, assessment, implications for preoperative templating and hip arthroplasty. Orthop Traumatol Surg Res. 2009;95(3): 210.[40] Abdel MP, Cottino U, Mabry TM. Management of periprosthetic femoral fractures following total hip arthroplasty: a review. Int Orthop. 2015;39(10): 2005.[41] Lindahl H. Epidemiology of periprosthetic femur fracture around a total hip arthroplasty. Injury. 2007;38(6): 651-654.[42] Berry DJ. EPIDEMIOLOGY : Hip and Knee. Orthop Clin N Am.1999; 30(2):183-190.[43] Sidler-Maier CC, Waddell JP. Incidence and predisposing factors of periprosthetic proximal femoral fractures: a literature review. Int Orthop. 2015;39(9): 1673-1682.[44] Mallory TH. Preparation of the proximal femur in cementless total hip revision. Clin Orthop Relat Res. 1988;(235): 47.[45] D'Antonio J, Mccarthy JC, Bargar WL, et al. Classification of femoral abnormalities in total hip arthroplasty. Clin Orthop Relat Res. 1993; 296(296):133.[46] Weeden SH, Paprosky WG. Minimal 11-year follow-up of extensively porous-coated stems in femoral revision total hip arthroplasty. J Arthroplasty. 2002;17(4): 134-137.[47] Della Valle CJ, Paprosky WG. The femur in revision total hip arthroplasty evaluation and classification. Clin Orthop Relat Res. 2004;420(420): 55-62.[48] Saleh KJ, Holtzman J, Gafni A, et al. Reliability and intraoperative validity of preoperative assessment of standardized plain radiographs in predicting bone loss at revision hip surgery. J Bone Joint Surg Am. 2001;83(7): 1040-1046.[49] Meding JB, Ritter MA, Keating EM, et al. Impaction bone-grafting before insertion of a femoral stem with cement in revision total hip arthroplasty. A minimum two-year follow-up study. J Bone Joint Surg Am.1997;79(12): 1834-1841.[50] Eldridge JD, Smith EJ, Hubble MJ, et al. Massive early subsidence following femoral impaction grafting. J Arthroplasty. 1997;12(5): 535-540.[51] Ornstein E, Atroshi I, Franzén H, et al. Early complications after one hundred and forty-four consecutive hip revisions with impacted morselized allograft bone and cement. J Bone Joint Surg Am. 2002; 84-A(8): 1323.[52] Sierra RJ, Charity J, Tsiridis E, et al. The use of long cemented stems for femoral impaction grafting in revision total hip arthroplasty. J Bone Joint Surg Am. 2008;90(6): 1330-1336.[53] Ornstein E, Linder L, Ranstam J, et al. Femoral impaction bone grafting with the Exeter stem - the Swedish experience: survivorship analysis of 1305 revisions performed between 1989 and 2002. J Bone Joint Surg Br. 2009;91(4):441-446.[54] Wraighte PJ, Howard PW. Femoral impaction bone allografting with an Exeter cemented collarless, polished, tapered stem in revision hip replacement: a mean follow-up of 10.5 years. Bone Joint J.2008;90(8): 1000-1004.[55] Ghoz A, Broadhead ML, Morley J, et al. Outcomes of dual modular cementless femoral stems in revision hip arthroplasty. Orthop Rev (Pavia). 2014;6(1):5247. [56] Pellicci PM, Jr WP, Sledge CB, et al. Long-term results of revision total hip replacement. A follow-up report. J Bone Joint Surg Am.1985;67(4): 513-516.[57] Kavanagh BF, Ilstrup DM, Fitzgerald RH, Jr. Revision total hip arthroplasty. J Bone Joint Surg Am. 1985;67(4): 517-526.[58] Halliday BR, English HW, Timperley AJ, et al. Femoral impaction grafting with cement in revision total hip replacement. Evolution of the technique and results. J Bone Joint Surg Br. 2003;85(6): 809-817.[59] Iorio R, Healy WL, Presutti AH. A prospective outcomes analysis of femoral component fixation in revision total hip arthroplasty. J Arthroplasty. 2008;23(5): 662-669.[60] Weiss RJ, Stark A, Kärrholm J. A modular cementless stem vs. cemented long-stem prostheses in revision surgery of the hip: A population-based study from the Swedish Hip Arthroplasty Register. Acta Orthop. 2011;82(2): 136-142.[61] Duncan WW, Hubble MJ, Howell JR. Revision of the cemented femoral stem using a cement-in-cement technique: a five- to 15-year review. J Bone Joint Surg Br. 2009;91(5): 577-582.[62] Mounsey EJ, Williams DH, Howell JR, et al. Revision of hemiarthroplasty to total hip arthroplasty using the cement-in-cement technique. Bone Joint J. 2015;97-B(12): 1623-1627.[63] Cnudde PH, Kärrholm J, Rolfson O, et al. Cement-in-cement revision of the femoral stem: analysis of 1179 first-time revisions in the Swedish Hip Arthroplasty Register. Bone Joint J. 2017;99-B(4 Supple B): 27-32.[64] Rubash HE, Harris WH. Revision of nonseptic, loose, cemented femoral components using modern cementing techniques. J Arthroplasty. 1988;3(3): 241-248.[65] Collis DK. Revision total hip replacement with cement. Semin Arthroplasty. 1993;4(1): 38.[66] Izquierdo RJ, Northmoreball MD. Long-term results of revision hip arthroplasty. Survival analysis with special reference to the femoral component. J Bone Joint Surg Br.1994;76(1): 34-39.[67] Estok DM 2nd, Harris WH. Long-term results of cemented femoral revision surgery using second-generation techniques. An average 11.7-year follow-up evaluation. Clin Orthop Relat Res.1994;(299):190.[68] Katz RP, Callaghan JJ, Sullivan PM, et al. Long-term results of revision total hip arthroplasty with improved cementing technique. J Bone Joint Surg Br. 1997;79(2): 322-326.[69] Trumm BN, Callaghan JJ, George CA, et al. Minimum 20-year follow-up results of revision total hip arthroplasty with improved cementing technique. J Arthroplasty. 2014;29(1): 236-241.[70] Solomon LB, Costi K, Kosuge D, et al. Revision total hip arthroplasty using cemented collarless double-taper femoral components at a mean follow-up of 13 years (8 to 20): an update. Bone Joint J. 2015; 97-B(8): 1038.[71] Desy NM, Johnson JD, Sierra RJ. Satisfactory results of the exeter revision femoral stem used for primary total hip arthroplasty. J Arthroplasty. 2017;32(2): 494.[72] Berry DJ, Harmsen WS, Ilstrup D, et al. Survivorship of uncemented proximally porous-coated femoral components. Clin Orthop Relat Res. 1995;(319): 168.[73] Malkani AL, Lewallen DG, Cabanela ME, et al. Femoral component revision using an uncemented, proximally coated, long-stem prosthesis. J Arthroplasty. 1996;11(4): 411-418.[74] Cameron HU. The long-term success of modular proximal fixation stems in revision total hip arthroplasty. J Arthroplasty.2002;17(1): 138-141.[75] Mc Carthy JC, Lee JA. Complex revision total hip arthroplasty with modular stems at a mean of 14 years. Clin Orthop Relat Res. 2007; 465(465):166-169.[76] Bolognesi MP, Pietrobon R, Clifford PE, et al. Comparison of a hydroxyapatite-coated sleeve and a porous-coated sleeve with a modular revision hip stem. A prospective, randomized study. J Bone Joint Surg Am. 2004;86-A(12): 2720.[77] Adolphson PY, Salemyr MO, Sköldenberg OG, et al. Large femoral bone loss after hip revision using the uncemented proximally porous-coated Bi-Metric prosthesis. Acta Orthop. 2009;80(1): 14-19.[78] Jr EC, Jr HR, Sr EC. Distal ingrowth components. Clin Orthop Relat Res, 2004, 420(420): 135-141.[79] Sporer SM, Paprosky WG. Revision total hip arthroplasty: the limits of fully coated stems. Clin Orthop Relat Res. 2003;417(417): 203-209.[80] Moreland JR, Bernstein ML. Femoral revision hip arthroplasty with uncemented, porous-coated stems. Clin Orthop Relat Res. 1995; 319(319):141.[81] Krishnamurthy AB, Macdonald SJ, Paprosky WG. 5- to 13-year follow-up study on cementless femoral components in revision surgery. J Arthroplasty. 1997;12(8): 839-847.[82] Reikeras O, Gunderson RB. Excellent results with femoral revision surgery using an extensively hydroxyapatite-coated stem: 59 patients followed for 10–16 years. Acta Orthop. 2006; 77(1): 98-103.[83] Hamilton WG, Hopper RH, Cashen DV, et al. Extensively porous-coated stems for femoral revision: a choice for all seasons. J Arthroplasty. 2007;22(4 Suppl 1): 106.[84] Garcia-Cimbrelo E, Garcia-Rey E, Cruz-Pardos A, et al. Stress-shielding of the proximal femur using an extensively porous-coated femoral component without allograft in revision surgery: a 5- to 17-year follow-up study. J Bone Joint Surg Br. 2010;92(10): 1363-1369.[85] Thomsen PB, Jensen NJ, Kampmann J, et al. Revision hip arthroplasty with an extensively ?porous-coated stem - excellent long-term ?results also in severe femoral bone stock loss. Hip Int. 2013;23(4): 352-358.[86] Engh CA. Extensively porous coated femoral cylinders: thirty years onward. 2015.[87] Reikerås O. Femoral revision surgery using a fully hydroxyapatite- coated stem: a cohort study of twenty two to twenty seven years. Int Orthop. 2016;41(2):271-275.[88] Böhm P, Bischel O. Femoral revision with the Wagner SL revision stem : evaluation of one hundred and twenty-nine revisions followed for a mean of 4.8 years. J Bone Joint Surg Am. 2001;83-A(7):1023-1031.[89] Singh SP, Bhalodiya HP. Results of Wagner SL revision stem with impaction bone grafting in revision total hip arthroplasty. Indian J Orthop. 2013;47(4): 357-363.[90] Sandiford NA, Garbuz DS, Masri BA, et al. Nonmodular tapered fluted titanium stems osseointegrate reliably at short term in revision THAs. Clin Orthop Relat Res. 2016: 1-7.[91] Bischel OE, Böhm PM. The use of a femoral revision stem in the treatment of primary or secondary bone tumours of the proximal femur: a prospective study of 31 cases. J Bone Joint Surg Br. 2010;92(10): 1435-1441.[92] Bakt?r A, Karaaslan F, Gencer K, et al. Femoral revision using the Wagner SL revision stem: a aingle-aurgeon experience featuring 11–19 years of follow-up. J Arthroplasty. 2015;30(5): 827-834.[93] Huang Y, Zhou Y, Shao H, et al. What is the difference between modular and nonmodular tapered fluted titanium stems in revision total hip arthroplasty. J Arthroplasty. 2017.[94] Kolb A, Grübl A, Schneckener CD, et al. Cementless total hip arthroplasty with the rectangular titanium Zweymuller stem: a concise follow-up, at a minimum of twenty years, of previous reports. J Bone Joint Surg Am. 2012;94(18):1681.[95] Hartwig CH, Böhm P, Czech U, et al. The Wagner revision stem in alloarthroplasty of the hip. Arch Orthop Traum Su. 1996;115(1): 5.[96] Alamo JGD, Garcia-Cimbrelo E, Castellanos V, et al. Radiographic bone regeneration and clinical outcome with the Wagner SL revision stem: a 5-year to 12-year follow-up study. J Arthroplasty.2007;22(4): 515-524.[97] Regis D, Sandri A, Bonetti I, et al. Femoral revision with the Wagner tapered stem: a ten- to 15-year follow-up study. J Bone Joint Surg Br.2011;93(10):1320.[98] Hoberg M, Konrads C, Engelien J, et al. Outcome of a modular tapered uncemented titanium femoral stem in revision hip arthroplasty. Int Orthop. 2015;39(9):1709-1713.[99] Wimmer MD, Randau TM, Deml MC, et al. Impaction grafting in the femur in cementless modular revision total hip arthroplasty: a descriptive outcome analysis of 243 cases with the MRP-TITAN revision implant.BMC Musculoskelet Disord.2013;14(1):19.[100] Wirtz DC, Gravius S, Ascherl R, et al. Uncemented femoral revision arthroplasty using a modular tapered, fluted titanium stem: 5- to 16-year results of 163 cases. Acta Orthop. 2014;85(6): 562-569.[101] Abdel MP, Cottino U, Larson DR, et al. Modular fluted tapered stems in aseptic revision total hip arthroplasty. J Bone Joint Surg Am. 2017; 99(10): 873.[102] Wirtz DC, Heller KD, Holzwarth U, et al. A modular femoral implant for uncemented stem revision in THR. Int Orthop. 2000;24(3): 134-138.[103] Kwong LM, Miller AJ, Lubinus P. A modular distal fixation option for proximal bone loss in revision total hip arthroplasty: a 2- to 6-year follow-up study. J Arthroplasty. 2003;18(1):94-97.[104] Schuh A, Werber S, Holzwarth U, et al. Cementless modular hip revision arthroplasty using the MRP Titan Revision Stem: outcome of 79 hips after an average of 4 years’ follow-up. Arch Orthop Traum Su. 2004;124(5): 306-309.[105] Mcinnis DP, Horne G, Devane PA. Femoral revision with a fluted, tapered, modular stem seventy patients followed for a mean of 3.9 years. J Arthroplasty. 2006;21(3):372-380.[106] Park YS, Moon YW, Lim SJ. Revision total hip arthroplasty using a fluted and tapered modular distal fixation stem with and without extended trochanteric osteotomy. J Arthroplasty. 2007;22(7): 993.[107] Rodriguez JA, Fada R, Murphy SB, et al. Two-year to five-year follow-up of femoral defects in femoral revision treated with the link MP modular stem. J Arthroplasty. 2009;24(5): 751-758.[108] Ovesen O, Emmeluth C, Hofbauer C, et al. Revision total hip arthroplasty using a modular tapered stem with distal fixation: good short-term results in 125 revisions. J Arthroplasty. 2010;25(3): 348.[109] Weiss RJ, Beckman MO, Enocson A, et al. Minimum 5-year follow-up of a cementless, modular, tapered stem in hip revision arthroplasty. J Arthroplasty. 2011;26(1):16. |
| [1] | 韦 玮, 李 剑, 黄林海, 兰敏东, 卢显威, 黄绍东. 全膝或全髋关节置换后老年人首次活动时跌倒恐惧的影响因素[J]. 中国组织工程研究, 2021, 25(9): 1351-1355. |
| [2] | 肖国庆, 刘选泽, 严钰皓, 钟喜红. 后交叉韧带替代型假体全膝关节置换术后屈曲受限的影响因素[J]. 中国组织工程研究, 2021, 25(9): 1362-1367. |
| [3] | 张 冲, 刘志昂, 姚帅辉, 高军胜, 姜 岩, 张 陆. 局部应用氨甲环酸减少老年股骨颈骨折全髋关节置换后引流的安全和有效性[J]. 中国组织工程研究, 2021, 25(9): 1381-1386. |
| [4] | 袁家威, 张海涛, 揭 珂, 曹厚然, 曾意荣. 基于网络药理学研究桃红四物汤治疗假体周围感染的潜在靶点和机制[J]. 中国组织工程研究, 2021, 25(9): 1428-1433. |
| [5] | 张 超, 吕 欣. 髋臼骨折固定后的异位骨化:危险因素、预防及其治疗进展[J]. 中国组织工程研究, 2021, 25(9): 1434-1439. |
| [6] | 陈俊名, 岳 辰, 何沛霖, 张俊涛, 孙墨渊, 刘又文. 髋关节置换与股骨近端防旋髓内钉内固定修复高龄股骨转子间骨折效果的Meta分析[J]. 中国组织工程研究, 2021, 25(9): 1452-1457. |
| [7] | 刘立华, 孙 伟, 王云亭, 高福强, 程立明, 李子荣, 王江宁. 头颈部开窗减压治疗L1型激素性股骨头坏死:单中心前瞻性临床研究[J]. 中国组织工程研究, 2021, 25(6): 906-911. |
| [8] | 化昊天, 赵文宇, 张 磊, 白文博, 王新卫. 抗生素人工骨治疗慢性骨髓炎疗效和安全性的Meta分析[J]. 中国组织工程研究, 2021, 25(6): 970-976. |
| [9] | 许玉林, 沈 师, 卓乃强, 杨惠麟, 杨 超, 李 洋, 赵 恒, 赵 露. 髋臼后柱骨折3种不同钢板固定后站立及坐立位下的生物力学比较[J]. 中国组织工程研究, 2021, 25(6): 826-830. |
| [10] | 张 宾, 孙丽华, 张俊花, 刘玉三, 崔彩云. 改良翻瓣即刻种植有利于上颌前牙区的软硬组织重建[J]. 中国组织工程研究, 2021, 25(5): 707-712. |
| [11] | 李晨杰, 吕林蔚, 宋 阳, 刘静娜, 张春秋. 预紧力作用下钛合金人工假体界面骨小梁形态参数测量与统计分析[J]. 中国组织工程研究, 2021, 25(4): 516-520. |
| [12] | 李晓壮, 段 浩, 王伟舟, 唐志宏, 王旸昊, 何 飞. 骨组织工程材料治疗骨缺损疾病在体内实验中的应用[J]. 中国组织工程研究, 2021, 25(4): 626-631. |
| [13] | 凡一诺, 管芷莹, 李伟峰, 陈立新, 魏秋实, 何 伟, 陈镇秋. 股骨髋臼撞击综合征全球研究现状及发展趋势的文献计量与可视化分析[J]. 中国组织工程研究, 2021, 25(3): 414-419. |
| [14] | 贺 杰, 常 祺. 四肢恶性骨肿瘤骨切除后大段骨缺损的生物重建[J]. 中国组织工程研究, 2021, 25(3): 420-425. |
| [15] | 邢 浩, 张永红, 王 栋. 长骨大段骨缺损修复方法的优势与不足[J]. 中国组织工程研究, 2021, 25(3): 426-430. |
中国组织工程研究杂志出版内容重点:人工关节;骨植入物;脊柱;骨折;内固定;数字化骨科;组织工程
1.1 资料来源
1.2 入选标准
深层感染(subfascial extension of infection)是目前是翻修的第3个最常见的原因,其发生率在0.3%-2.2%,特别是假体周围感染对于关节科医生来说是一个非常严峻挑战。细菌侵入髋关节后,移行至假体表面,黏附增殖形成一种膜,被称细菌生物被膜,细菌生物被膜的形成,机体的炎症细胞无法对其吞噬清除,躲藏在多糖基质内的细菌会释放各种炎性因子及酶类,造成局部的组织坏死和骨溶解,导致假体松动。不幸的是生物被膜内的细菌会产生耐药,且耐药机制尚不清楚,如何有效治疗仍是一大难点。目前,除了使用抗生素以外,有学者也将目光转到改进制造假体的材料上。 中国组织工程研究杂志出版内容重点:人工关节;骨植入物;脊柱;骨折;内固定;数字化骨科;组织工程
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||
.jpg)