中国组织工程研究 ›› 2026, Vol. 30 ›› Issue (35): 9365-9374.doi: 10.12307/2026.268
• 组织工程相关大数据分析 Big data analysis in tissue engineering • 上一篇
代谢健康肥胖表型与慢性腰痛的流行病学关联:基于NHANES数据库横断面分析
叶仕成1,2,刘玉新1,2 ,曾 轩1,2 ,隋丽丽3,刘 姣2,陈雨婷2,曲崇正1,2
- 1广州中医药大学第三临床医学院,广东省广州市 510405;2广州中医药大学第三附属医院,广东省广州市 510378;3广州中医药大学第一临床医学院,广东省广州市 510405
-
收稿日期:2025-09-04修回日期:2025-12-10出版日期:2026-12-18发布日期:2026-04-30 -
通讯作者:曲崇正,博士,主任医师,广州中医药大学第三临床医学院,广东省广州市 510405;广州中医药大学第三附属医院,广东省广州市 510378 -
作者简介:叶仕成,男,1997年生,江西省乐平市人,汉族,主治中医师,硕士在读,主要从事针灸推拿防治中医筋伤疾病的研究。 -
基金资助:广州中医药大学第三附属医院科研创新基金项目(Sy2023007),项目负责人:刘姣
Epidemiological association between metabolic health obesity phenotype and chronic low back pain: a cross-sectional analysis based on the NHANES database
Ye Shicheng1, 2, Liu Yuxin1, 2, Zeng Xuan1, 2, Sui Lili3, Liu Jiao2, Chen Yuting2, Qu Chongzheng1, 2
- 1Third Clinical Medical College, Guangzhou University of Chinese Medicine, Guangzhou 510405, Guangdong Province, China; 2The Third Affiliated Hospital of Guangzhou University of Chinese Medicine, Guangzhou 510378, Guangdong Province, China; 3The First Clinical Medical College of Guangzhou University of Chinese Medicine, Guangzhou 510405, Guangdong Province, China
-
Received:2025-09-04Revised:2025-12-10Online:2026-12-18Published:2026-04-30 -
Contact:Qu Chongzheng, MD, PhD, Chief physician, Third Clinical Medical College, Guangzhou University of Chinese Medicine, Guangzhou 510405, Guangdong Province, China; The Third Affiliated Hospital of Guangzhou University of Chinese Medicine, Guangzhou 510378, Guangdong Province, China -
About author:Ye Shicheng, MS candidate, Attending physician, Third Clinical Medical College, Guangzhou University of Chinese Medicine, Guangzhou 510405, Guangdong Province, China; The Third Affiliated Hospital of Guangzhou University of Chinese Medicine, Guangzhou 510378, Guangdong Province, China -
Supported by:Scientific Research Innovation Fund Project of Third Affiliated Hospital of Guangzhou University of Chinese Medicine, No. Sy2023007 (to LJ)
摘要:
文题释义:
代谢健康肥胖表型:这类人群常具有3个主要临床特征:内脏脂肪和异位脂肪的积累减少、胰岛素敏感性保留以及与代谢不健康型肥胖个体相比全身和脂肪组织炎症程度较低。
慢性腰痛:腰痛是指肌肉骨骼起源的疼痛,从最低的肋骨延伸至臀褶,有时可因躯体性疼痛而延伸至大腿 (膝盖以上)。腰痛症状持续超过12周的为慢性腰痛。
背景:相较于代谢不健康肥胖人群,代谢健康肥胖表型个体是否以及如何影响慢性腰痛的风险和病理进程目前尚不清楚,亟需研究明确其关联性及潜在机制。
目的:探究代谢健康肥胖表型与慢性腰痛的流行病学关联。
方法:基于美国国家健康与营养检查调查(NHANES)1999-2004年及2009-2010年4个调查周期数据(n=4 956),采用回顾性横断面研究设计,按照世界卫生组织标准,通过体质指数和腰围界定肥胖状态,联合代谢综合征核心指标(空腹血糖、血脂谱、血压等)进行代谢表型分层,确立代谢健康型肥胖与代谢不健康型肥胖分类体系。通过构建多因素校正Logistic回归模型与限制性立方样条曲线,系统评估代谢健康肥胖表型与慢性腰痛风险的非线性剂量-反应关系,最终建立多变量校正模型分层解析慢性腰痛风险,采用亚组分析、阈值效应分析及多重敏感性分析框架验证模型的稳健性。
结果与结论:①代谢不健康型肥胖显著增加慢性腰痛风险[体质量指数标准:OR(95%CI)=1.44(1.11,1.85),P=0.007 0;腰围标准:OR(95%CI)=1.57(1.25,1.97),P=0.000 3],吸烟[OR(95%CI)=1.44(1.24,1.67),P < 0.000 1]、关节炎[OR(95%CI)=2.44(2.06,2.88),P < 0.000 1]等共病因素显著放大代谢健康型肥胖对慢性腰痛的风险效应。体质量指数≥39.73 kg/m²和腰围≥125 cm为代谢不健康人群的慢性腰痛风险阈值。低教育水平、低收入、丧偶/离异或分居状态加重患慢性腰痛风险。在总人群和代谢不健康参与者中,体质量指数和慢性腰痛之间存在线性关系(P < 0.05)。在代谢健康参与者中,体质量指数和慢性腰痛之间的剂量-反应关系存在近似线性关系(P > 0.05);在总人群、代谢健康和代谢不健康参与者中,慢性腰痛之间的剂量-反应关系存在近似线性关系(P > 0.05)。②基于NHANES数据的横断面分析显示,代谢不健康型肥胖与慢性腰痛存在显著的正向独立关联,代谢健康型肥胖与慢性腰痛的关联强度较弱且不具统计学差异,表明代谢健康状况是影响肥胖人群慢性腰痛发生的重要关联因素。通过国际研究构建的代谢健康肥胖与慢性腰痛关联模型,为中国人群探索同类疾病的种族异质性及本土化机制(如亚洲特异性代谢阈值)提供了关键理论参照, 结果警示中国需关注代谢健康肥胖群体的腰痛风险,推动临床分型干预策略优化(如避免过度减重)并前瞻性防控肥胖相关肌骨疾病的公共卫生负担。
https://orcid.org/0009-0003-7211-2116 (叶仕成)
中国组织工程研究杂志出版内容重点:干细胞;骨髓干细胞;造血干细胞;脂肪干细胞;肿瘤干细胞;胚胎干细胞;脐带脐血干细胞;干细胞诱导;干细胞分化;组织工程
中图分类号:
引用本文
叶仕成, 刘玉新, 曾 轩, 隋丽丽, 刘 姣, 陈雨婷, 曲崇正. 代谢健康肥胖表型与慢性腰痛的流行病学关联:基于NHANES数据库横断面分析[J]. 中国组织工程研究, 2026, 30(35): 9365-9374.
Ye Shicheng, Liu Yuxin, Zeng Xuan, Sui Lili, Liu Jiao, Chen Yuting, Qu Chongzheng. Epidemiological association between metabolic health obesity phenotype and chronic low back pain: a cross-sectional analysis based on the NHANES database[J]. Chinese Journal of Tissue Engineering Research, 2026, 30(35): 9365-9374.
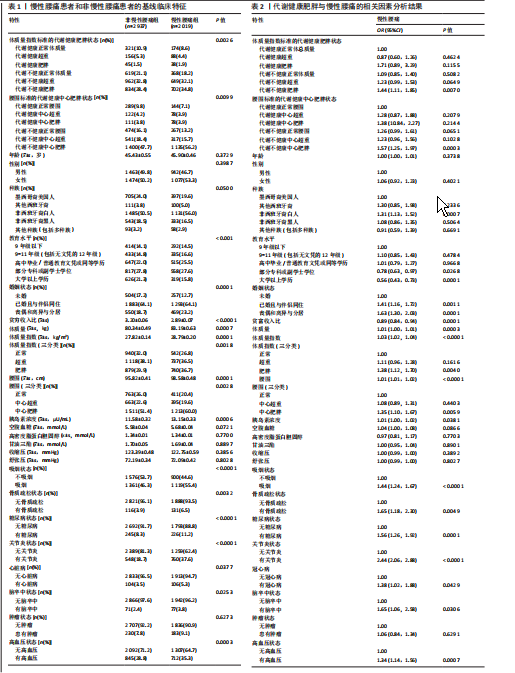
基于体质量指数/腰围双维度的表型分层分析显示:①代谢健康亚组中,正常体质量及超重组的慢性腰痛患病率显著低于代谢不健康组(体质指数标准:代谢健康正常体质量组8.6% vs.代谢不健康正常体质量组18.2%;代谢健康超重组4.4% vs.代谢不健康超重组32.1%;P=0.002 6;腰围标准:代谢健康正常体质量组7.1% vs.代谢不健康正常体质量组13.2%;代谢健康超重组3.9% vs. 代谢不健康超重组15.7%;P=0.009 9);②肥胖表型(代谢健康肥胖/代谢不健康肥胖)在慢性腰痛组呈显著聚集趋势(体质指数标准:代谢健康肥胖组1.9% vs. 代谢不健康肥胖组34.8%;腰围标准:代谢健康肥胖组3.9% vs. 代谢不健康肥胖组56.2%)。
多维度风险分析揭示,在社会梯度效应(低教育水平、低收入、吸烟状态)、婚姻解组效应(丧偶/离异或分居)、代谢负荷累积效应(胰岛素浓度)及心脑血管疾病(心脏病、脑卒中)中慢性腰痛风险显著(P < 0.05)。在临床共病中,糖尿病、关节炎、高血压展现出强关联(所有P < 0.001)。
组间均衡性检验表明,非慢性腰痛组与慢性腰痛组在基础人口学特征(年龄、性别、种族)、核心代谢参数(空腹血糖、高密度脂蛋白胆固醇、甘油三酯、收缩压/舒张压)及恶性肿瘤患病率方面比较差异均无显著性意义(P > 0.05),证实研究结果的独立性和稳健性。
2.2 代谢健康肥胖表型与慢性腰痛的相关性 根据Logistic回归分析的结果,在代谢不健康型肥胖群体中患有慢性腰痛的风险更大,体质指数标准:OR(95%CI)=1.44 (1.11,1.85),P=0.007 0;腰围标准:OR(95%CI)=1.57 (1.25,1.97),P=0.000 3。此外,在婚姻状态[OR(95%CI)=1.63 (1.30,2.03),P=0.000 1]、贫富收入比[OR(95%CI)=0.89 (0.84,0.94),P=0.000 1]、体质量[OR(95%CI)=1.01 (1.00,1.01),P=0.000 3]、体质量指数[OR(95%CI)=1.03 (1.02,1.04),P < 0.000 1]、胰岛素[OR(95%CI)=1.01(1.00,1.02),P=0.038 1]、吸烟[OR(95%CI)=1.44 (1.24,1.67),P < 0.000 1]、骨质疏松[OR(95%CI)=1.65 (1.18,2.30),P=0.004 9]、糖尿病[OR(95%CI)=1.56 (1.26,1.92),P=0.000 1]、关节炎[OR(95%CI)=2.44 (2.06,2.88),P < 0.000 1]、冠心病[OR(95%CI)=1.38 (1.02,1.88),P=0.042 9]、脑卒中[OR(95%CI)=1.65 (1.06,2.58),P=0.030 6]、高血压[OR(95%CI)=1.34 (1.14,1.56),P=0.000 7]等方面更能体现出与慢性腰痛的强关联性,见表2。
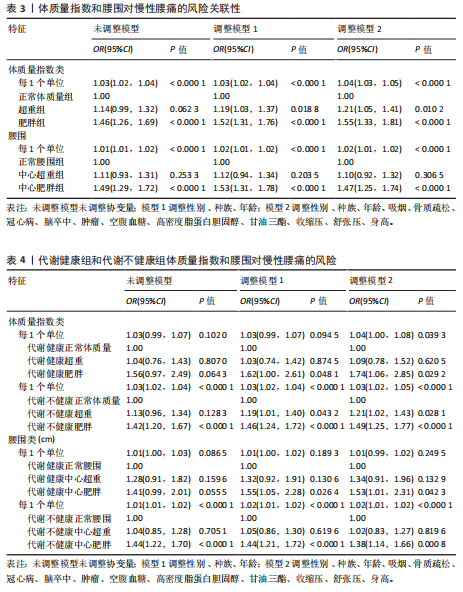
2.3 体质量指数和腰围与慢性腰痛的独立关联 建立了3个二元Logistic回归模型,以探讨体质量指数和腰围对慢性腰痛的潜在影响,结果表明,体质量指数和腰围与未调整模型、模型1、模型2中的慢性腰痛呈正相关,与受控协变量关系不大,见表3。在未调整模型中,体质量指数或腰围增加一个单位,患有慢性腰痛的概率增加[体质量指数:OR(95%CI)=1.03(1.02,1.04),P < 0.000 1;腰围:OR(95%CI)=1.01(1.01,1.02),P < 0.000 1]。体质量指数或腰围每增加一个单位,模型1中[体质量指数:OR(95%CI)=
1.03(1.02,1.04),P < 0.000 1;腰围:OR(95%CI)=1.02(1.01,1.02),P < 0.000 1]和模型2[体质量指数:OR(95%CI)=1.04(1.03,1.05),P < 0.000 1;腰围:OR(95%CI)=1.02(1.01,1.02),P < 0.000 1]中患有慢性腰痛的概率也增加。将体质量指数和腰围转换为分类变量(体质量指数分为3组:“正常”“超重”和“肥胖”;腰围也分为3组:“正常”“中心性超重”和“中心性肥胖”)。校正模型2的协变量后,根据体质量指数标准的肥胖与发生慢性腰痛的可能性增加相关[OR(95%CI)=1.55(1.33,1.81),P < 0.000 1],根据腰围标准的中心性肥胖也与发生慢性腰痛的概率增加相关[OR(95%CI)=1.47(1.25,1.74),P < 0.000 1]。
2.4 代谢健康肥胖表型与慢性腰痛的关系 按代谢健康和肥胖(体质量指数类别和腰围类别)交叉分类的慢性腰痛风险,见表4。在调整模型2协变量后,代谢健康型肥胖患者发生慢性腰痛的概率相对高于代谢健康型正常体质量患者[体质量指数标准:OR(95%CI)=1.74 (1.06,2.85),P=0.0292;腰围标准:OR(95%CI)=1.53 (1.01,2.31),P=0.0423]。此外,代谢不健康型肥胖参与者发生慢性腰痛的可能性显著高于代谢不健康型正常体质量个体[体质指数标准:OR(95%CI)=1.49(1.25,1.77),P < 0.000 1;腰围标准:OR(95%CI)=1.38(1.14,1.66),P=0.000 8]。
在代谢健康和不健康的参与者中,体质量指数每增加一个单位都会增加发生慢性腰痛的概率[代谢健康:OR(95%CI)=1.04(1.00,1.08),P=0.039 3;代谢不健康:OR(95%CI)=1.03 (1.02,1.05),P < 0.000 1]。在代谢不健康的参与者中,腰围每增加一个单位发生慢性腰痛的概率也增加[OR(95%CI)=1.02(1.01,1.02),P < 0.000 1]。而在代谢健康参与者中腰围和发生慢性腰痛的概率关系不显著(P=0.249 5)。
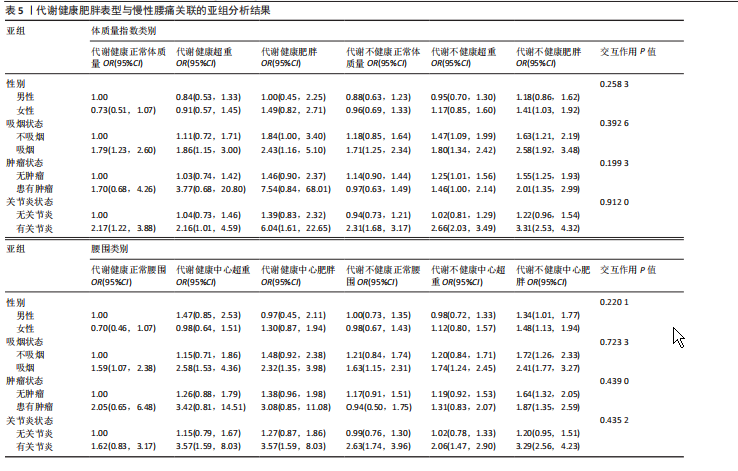
2.5 亚组分析结果 亚组分析结果见表5。未检测到代谢健康肥胖表型在性别、吸烟状况、肿瘤状态和关节炎状态方面发生慢性腰痛概率的显著交互作用(P > 0.05)。
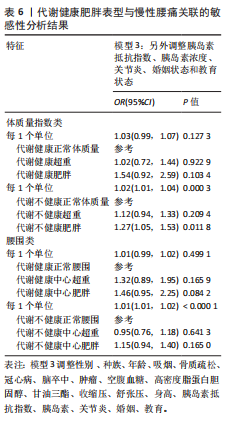
2.6 敏感性分析结果 在敏感性分析中,当在模型2的基础上额外调整婚姻状态、教育水平、关节炎状态、胰岛素浓度和胰岛素抵抗指数时,代谢健康肥胖表型和慢性腰痛之间的关联基本不变,见表6。
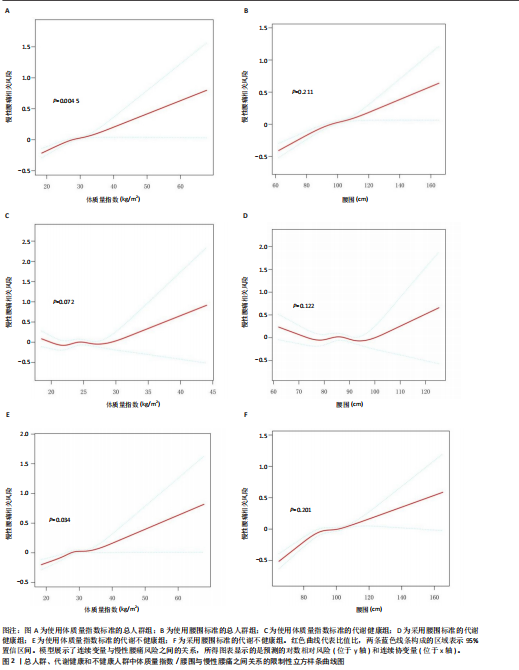
2.7 限制性立方样条图 此次研究利用限制性立方样条来模拟和建模总人群、代谢健康和代谢不健康参与者中体质量指数/腰围与慢性腰痛的关系,见图2所示。在总人群和代谢不健康参与者中,体质量指数和慢性腰痛之间的剂量-反应关系存在线性关系(P < 0.05),表明体质量指数和慢性腰痛之间存在正相关。在代谢健康参与者中,体质量指数和慢性腰痛之间的剂量-反应关系存在近似线性关系(P > 0.05);在总人群、代谢健康和代谢不健康参与者中,腰围和慢性腰痛之间的剂量-反应关系存在近似线性关系(P > 0.05)。
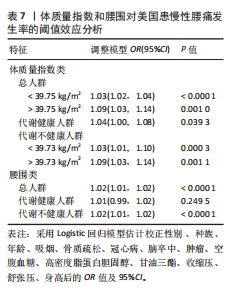
2.8 阈值效应分析结果 根据体质量指数标准类别,在总人群参与者中,当体质量指数< 39.75 kg/m2时,每增加1单位发生慢性腰痛的概率增加3%[OR(95%CI)=1.03(1.02,1.04),P < 0.000 1];当体质量指数≥39.75 kg/m2时,每增加1单位发生慢性腰痛的概率升至9%[OR(95%CI)=1.09(1.03,1.14),P=0.001]。在代谢健康参与者中,体质量指数与慢性腰痛的整体关联较弱[OR(95%CI)=1.04(1.00,1.08),P=0.039 3]。在代谢不健康参与者中,与总人群结果几乎保持一致,当体质量指数≥39.73 kg/m2时发生慢性腰痛的概率显著增加9%(OR=1.09,P=0.001 1),见表7。
根据腰围标准类别,在总人群参与者和代谢不健康人群中,腰围每增加1 cm发生慢性腰痛概率均增加2%[OR(95%CI)=1.02(1.01,1.02),P < 0.000 1],而在代谢健康人群中二者无显著关联(OR=1.01,P=0.249 5)。如表7所示。
| [1] GBD 2021 Low Back Pain Collaborators. Global, regional, and national burden of low back pain, 1990-2020, its attributable risk factors, and projections to 2050: a systematic analysis of the Global Burden of Disease Study 2021. Lancet Rheumatol. 2023;5(6):e316-e329. [2] VAN DER GAAG WH, ROELOFS PD, ENTHOVEN WT, et al. Non-steroidal anti-inflammatory drugs for acute low back pain. Cochrane Database Syst Rev. 202;4(4):D13581. [3] TAGLIAFERRI SD, MILLER CT, OWEN PJ, et al. Domains of Chronic Low Back Pain and Assessing Treatment Effectiveness: A Clinical Perspective. Pain Pract. 2020;20(2):211-225. [4] ABRAHAM S, JOHNSON CL. Prevalence of severe obesity in adults in the United States. Am J Clin Nutr. 1980;33(2 Suppl):364-369. [5] HARTVIGSEN J, HANCOCK MJ, KONGSTED A, et al. What low back pain is and why we need to pay attention. Lancet. 2018;391(10137):2356-2367. [6] SHIRI R, KARPPINEN J, LEINO-ARJAS P, et al. The association between obesity and low back pain: a meta-analysis. Am J Epidemiol. 2010;171(2):135-154. [7] LI Y, SCHOUFOUR J, WANG DD, et al. Healthy lifestyle and life expectancy free of cancer, cardiovascular disease, and type 2 diabetes: prospective cohort study. BMJ. 2020;368:l6669. [8] HIGGINS DM, BUTA E, HEAPY AA, et al. The Relationship Between Body Mass Index and Pain Intensity Among Veterans with Musculoskeletal Disorders: Findings from the MSD Cohort Study. Pain Med. 2020;21(10):2563-2572. [9] HERZOG W. Reflections on obesity, exercise, and musculoskeletal health. J Sport Health Sci. 2020;9(2):108-109. [10] WALSH TP, ARNOLD JB, EVANS AM, et al. The association between body fat and musculoskeletal pain: a systematic review and meta-analysis. BMC Musculoskelet Disord. 2018;19(1):233. [11] MENDONCA CR, NOLL M, DE CARVALHO SANTOS ASEA, et al. High prevalence of musculoskeletal pain in individuals with severe obesity: sites, intensity, and associated factors. Korean J Pain. 2020;33(3):245-257. [12] BLUHER M. Metabolically Healthy Obesity. Endocr Rev. 2020;41(3):bnaa004. [13] WU A, MARCH L, ZHENG X, et al. Global low back pain prevalence and years lived with disability from 1990 to 2017: estimates from the Global Burden of Disease Study 2017. Ann Transl Med. 2020;8(6):299. [14] SMITH GI, MITTENDORFER B, KLEIN S. Metabolically healthy obesity: facts and fantasies. J Clin Invest. 2019;129(10):3978-3989. [15] KRAMER CK, ZINMAN B, RETNAKARAN R. Are metabolically healthy overweight and obesity benign conditions?: A systematic review and meta-analysis. Ann Intern Med. 2013;159(11):758-769. [16] CAO Z, ZHENG X, YANG H, et al. Association of obesity status and metabolic syndrome with site-specific cancers: a population-based cohort study. Br J Cancer. 2020;123(8):1336-1344. [17] STEFAN N, HARING H, HU FB, et al. Metabolically healthy obesity: epidemiology, mechanisms, and clinical implications. Lancet Diabetes Endocrinol. 2013;1(2):152-162. [18] GÓMEZ-AMBROSI J, SILVA C, GALOFRÉ JC, et al. Body mass index classification misses subjects with increased cardiometabolic risk factors related to elevated adiposity. Int J Obes (Lond). 2012;36(2):286-294. [19] LEMIEUX S, PRUD’HOMME D, BOUCHARD C, et al. A single threshold value of waist girth identifies normal-weight and overweight subjects with excess visceral adipose tissue. Am J Clin Nutr. 1996;64(5):685-693. [20] LEAN ME, HAN TS, MORRISON CE. Waist circumference as a measure for indicating need for weight management. BMJ. 1995; 311(6998):158-161. [21] ALBERTI KGMM, ECKEL RH, GRUNDY SM, et al. Harmonizing the metabolic syndrome: a joint interim statement of the International Diabetes Federation Task Force on Epidemiology and Prevention; National Heart, Lung, and Blood Institute; American Heart Association; World Heart Federation; International Atherosclerosis Society; and International Association for the Study of Obesity. Circulation. 2009;120(16):1640-1645. [22] MATTHEWS DR, HOSKER JP, RUDENSKI AS, et al. Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia. 1985;28(7):412-419. [23] Obesity: preventing and managing the global epidemic. Report of a WHO consultation. World Health Organ Tech Rep Ser. 2000;894:1-253. [24] MAN S, GAO Y, LV J, et al. Metabolically healthy obesity was significantly associated with increased risk of gallstones. Eur J Endocrinol. 2022;186(2):275-283. [25] PENISTON JH. A review of pharmacotherapy for chronic low back pain with considerations for sports medicine. Phys Sportsmed. 2012;40(4):21-32. [26] HEUCH I, HEUCH I, HAGEN K, et al. A Comparison of Anthropometric Measures for Assessing the Association between Body Size and Risk of Chronic Low Back Pain: The HUNT Study. PLoS One. 2015;10(10):e141268. [27] KAWI J. Predictors of self-management for chronic low back pain. Appl Nurs Res. 2014;27(4):206-212. [28] MORELHÃO PK, TUFIK S, ANDERSEN ML. What Are the Effects of Physical Activity on Sleep Quality and Low Back Pain in Older Adults? J Clin Sleep Med. 2019;15(7):1067-1068. [29] DU T, NARITA I, YANAI T. Three-Dimensional Torso Motion in Tethered Front Crawl Stroke and its Implications on Low Back Pain. J Appl Biomech. 2016;32(1):50-58. [30] ANDRADE FCD, CHEN XS. A biopsychosocial examination of chronic back pain, limitations on usual activities, and treatment in Brazil, 2019. PLoS One. 2022;17(6):e269627. [31] RISBUD MV, SHAPIRO IM. Role of cytokines in intervertebral disc degeneration: pain and disc content. Nat Rev Rheumatol. 2014;10(1):44-56. [32] MOSKOWITZ RW, ZIV I, DENKO CW, et al. Spondylosis in sand rats: a model of intervertebral disc degeneration and hyperostosis. J Orthop Res. 1990;8(3):401-411. [33] ZHANG Y, SI M, LI C, et al. Effect of hyperlipidaemia to accelerate intervertebral disc degeneration in the injured rat caudal disc model. J Orthop Sci. 2019;24(1):42-49. [34] WANG F, CAI F, SHI R, et al. Aging and age related stresses: a senescence mechanism of intervertebral disc degeneration. Osteoarthritis Cartilage. 2016;24(3):398-408. [35] SEGAR AH, FAIRBANK JCT, Urban J. Leptin and the intervertebral disc: a biochemical link exists between obesity, intervertebral disc degeneration and low back pain-an in vitro study in a bovine model. Eur Spine J. 2019;28(2):214-223. [36] CURIC G. Intervertebral Disc and Adipokine Leptin-Loves Me, Loves Me Not. Int J Mol Sci. 2020; 22(1):375. [37] HUA K, LI L, YU H, et al. Leptin Induces MMP-1 Expression Through the RhoA/ERK1/2/NF-κB Axis in Human Intervertebral Disc Cartilage Endplate-Derived Stem Cells. J Inflamm Res. 2023;16:5235-5248. [38] LI Z, SHEN J, WU W KK, et al. The role of leptin on the organization and expression of cytoskeleton elements in nucleus pulposus cells. J Orthop Res. 2013;31(6):847-857. [39] AZIM S, NICHOLSON J, REBECCHI MJ, et al. Interleukin-6 and leptin levels are associated with preoperative pain severity in patients with osteoarthritis but not with acute pain after total knee arthroplasty. Knee. 2018;25(1):25-33. [40] NIEMANTSVERDRIET E, VAN DEN AKKER EB, BOETERS DM, et al. Gene expression identifies patients who develop inflammatory arthritis in a clinically suspect arthralgia cohort. Arthritis Res Ther. 2020;22(1):266. [41] KOSE R, SARGIN G, SENTURK T, et al. The association between clinically suspect arthralgia and adipokines in obese patients. Acta Reumatol Port. 2018;43(4):284-290. [42] WANG T, HE C. Pro-inflammatory cytokines: The link between obesity and osteoarthritis. Cytokine Growth Factor Rev. 2018;44:38-50. [43] ZHAO C, LIU D, LI H, et al. Expression of leptin and its functional receptor on disc cells: contribution to cell proliferation. Spine (Phila Pa 1976). 2008; 33(23):E858-E864. [44] GO O, FREEMAN RH, REAMS GP, et al. Obesity hypertension: pathophysiological role of leptin in neuroendocrine dysregulation. Am J Med Sci. 2014;347(6):485-489. [45] WEBER KT, ALIPUI DO, SISON CP, et al. Serum levels of the proinflammatory cytokine interleukin-6 vary based on diagnoses in individuals with lumbar intervertebral disc diseases. Arthritis Res Ther. 2016;18:3. [46] 孟祥杰,王文军,张超飞,等.身高、质量及腰靠凸起对驾驶员腰部载荷的影响[J].西安交通大学学报,2015,49(9):114-119. [47] RIHN JA, KURD M, HILIBRAND AS, et al. The influence of obesity on the outcome of treatment of lumbar disc herniation: analysis of the Spine Patient Outcomes Research Trial (SPORT). J Bone Joint Surg Am. 2013;95(1):1-8. [48] GAYE A, DOUMATEY AP, DAVIS SK, et al. Whole-genome transcriptomic insights into protective molecular mechanisms in metabolically healthy obese African Americans. NPJ Genom Med. 2018;3:4. [49] PERSEGHIN G. Is a nutritional therapeutic approach unsuitable for metabolically healthy but obese women? Diabetologia. 2008;51(9):1567-1569. [50] 唐雨菲,周敬凯,莫烨云,等.地菍总黄酮对高脂饮食诱导非酒精性脂肪肝大鼠脂代谢的影响[J].中国畜牧兽医,2023,50(8):3438-3447. [51] 季晓琪,刘澳,孙永兵,等.基于定量CT对内脏脂肪面积与肝功能相关指标的相关性分析[J].临床放射学杂志,2025,44(6):1107-1111. [52] OHNISHI H, ZHANG Z, YURUBE T, et al. Anti-Inflammatory Effects of Adiponectin Receptor Agonist AdipoRon against Intervertebral Disc Degeneration. Int J Mol Sci. 2023;24(10):8566. [53] RUIZ-FERNÁNDEZ C, FRANCISCO V, PINO J, et al. Molecular Relationships among Obesity, Inflammation and Intervertebral Disc Degeneration: Are Adipokines the Common Link? Int J Mol Sci. 2019;20(8):2030. [54] HAMER M, BELL JA, SABIA S, et al. Stability of metabolically healthy obesity over 8 years: the English Longitudinal Study of Ageing. Eur J Endocrinol. 2015;173(5):703-708. [55] SEO MH, RHEE EJ. Metabolic and cardiovascular implications of a metabolically healthy obesity phenotype. Endocrinol Metab (Seoul). 2014; 29(4):427-434. [56] CITKO A, GÓRSKI S, MARCINOWICZ L, et al. Sedentary Lifestyle and Nonspecific Low Back Pain in Medical Personnel in North-East Poland. Biomed Res Int. 2018;2018:1965807. [57] LI Y, CHEN L, GAO Y, et al. Oxidative Stress and Intervertebral Disc Degeneration: Pathophysiology, Signaling Pathway, and Therapy. Oxid Med Cell Longev. 2022;2022:1984742. [58] WANG D, ZHENG H, ZHOU W, et al. Mitochondrial Dysfunction in Oxidative Stress-Mediated Intervertebral Disc Degeneration. Orthop Surg. 2022;14(8):1569-1582. [59] WANG Y, CHENG H, WANG T, et al. Oxidative stress in intervertebral disc degeneration: Molecular mechanisms, pathogenesis and treatment. Cell Prolif. 2023;56(9):e13448. [60] SAWA AGU, LEHRMAN JN, CRAWFORD NR, et al. Variations Among Human Lumbar Spine Segments and Their Relationships to In Vitro Biomechanics: A Retrospective Analysis of 281 Motion Segments From 85 Cadaveric Spines. Int J Spine Surg. 2020; 14(2):140-150. [61] ZAWOJSKA K, WNUK-SCARDACCIONE A, BILSKI J, et al. Correlation of Body Mass Index with Pelvis and Lumbar Spine Alignment in Sagittal Plane in Hemophilia Patients. Medicina (Kaunas). 2019;55(10):627. [62] HUSSAIN SM, URQUHART DM, WANG Y, et al. Fat mass and fat distribution are associated with low back pain intensity and disability: results from a cohort study. Arthritis Res Ther. 2017;19(1):26. [63] XU T, JIN F, YU Y, et al. Association between waist circumference and chronic pain: insights from observational study and two-sample Mendelian randomization. Front Nutr. 2024;11:1415208. [64] 周永慧,龚海宁,陶再晓,等.肥胖与疼痛[J].中国疼痛医学杂志,2016,22(4):298-300. [65] 中华医学会内分泌学分会.肥胖患者的长期体重管理及药物临床应用指南(2024版)[J].中华内分泌代谢杂志,2024,40(7):545-564. [66] 中国营养学会.中国高龄老年人体质指数适宜范围与体重管理指南(T/CNSS 021—2023)[J].中华流行病学杂志,2023,44(9):1335-1337. [67] 刘家顺,谢鸿儒,孙云凯,等.腰椎间盘退变与椎旁肌改变的相关性及机制[J].中国组织工程研究,2025,29(27):5897-5906. [68] GHASEMI M, ARJMAND N. Spinal segment ranges of motion, movement coordination, and three-dimensional kinematics during occupational activities in normal-weight and obese individuals. J Biomech. 2021;123:110539. [69] HASHIMOTO Y, MATSUDAIRA K, SAWADA SS, et al. Obesity and low back pain: a retrospective cohort study of Japanese males. J Phys Ther Sci. 2017;29(6):978-983. [70] FAY M, BLACK M. Risk factors for low back pain amongst adults in Nigeria and South Africa: a systematic review. BMC Musculoskelet Disord. 2024;25(1):968. [71] AMINDE JA, AMINDE LN, BIJA MD, et al. Health-related quality of life and its determinants in patients with chronic low back pain at a tertiary hospital in Cameroon: a cross-sectional study. BMJ Open. 2020;10(10):e35445. [72] 孙文江,余波,吕君,等.非特异性颈腰痛与心理压力和社会支持相关性的问卷调查[J].中国康复医学杂志,2020,35(6):723-726. [73] 汪敏,吴建贤.腰痛与心理社会因素的相关研究现状[J].中国康复医学杂志,2009,24(5):473-475. [74] CITKO A, GÓRSKI S, MARCINOWICZ L, et al. Sedentary Lifestyle and Nonspecific Low Back Pain in Medical Personnel in North-East Poland. Biomed Res Int. 2018;2018:1965807. [75] KALITA J, SONKAR KK, MISRA UK, et al. Does Metabolic Syndrome Determine Severity and Disability of Chronic Low Backache? J Neurosci Rural Pract. 2018;9(2):208-213. [76] GROßSCHÄDL F, STOLZ E, MAYERL H, et al. Educational inequality as a predictor of rising back pain prevalence in Austria-sex differences. Eur J Public Health. 2016;26(2):248-253. [77] ADLER NE, STEWART J. Health disparities across the lifespan: meaning, methods, and mechanisms. Ann N Y Acad Sci. 2010;1186:5-23. [78] MCEWEN BS, GIANAROS PJ. Central role of the brain in stress and adaptation: links to socioeconomic status, health, and disease. Ann N Y Acad Sci. 2010;1186:190-222. [79] STRINGHINI S, CARMELI C, JOKELA M, et al. Socioeconomic status and the 25 × 25 risk factors as determinants of premature mortality: a multicohort study and meta-analysis of 1·7 million men and women. Lancet. 2017;389(10075):1229-1237. [80] TAN M, MAMUN A, KITZMAN H, et al. Neighborhood Disadvantage and Allostatic Load in African American Women at Risk for Obesity-Related Diseases. Prev Chronic Dis. 2017;14:E119. [81] BURKERT NT, RÁSKY É, GROßSCHÄDL F, et al. The influence of socioeconomic factors on health parameters in overweight and obese adults. PLoS One. 2013;8(6):e65407. [82] 朱洪柳,王维.中国中老年人腰痛相关因素分析及列线图预测模型的构建[J].中国组织工程研究,2023,27(31):4937-4942. [83] 王大兴,解京明,邓虹,等.退变性慢性下腰痛与社会心理因素的相关性研究[J].中国全科医学, 2011,14(4):442-445. [84] HENEWEER H, AUFDEMKAMPE G, VAN TULDER MW, et al. Psychosocial variables in patients with (sub)acute low back pain: an inception cohort in primary care physical therapy in The Netherlands. Spine (Phila Pa 1976). 2007;32(5):586-592. [85] LUCHA-LÓPEZ MO, HIDALGO-GARCÍA C, MONTI-BALLANO S, et al. Body Mass Index and Its Influence on Chronic Low Back Pain in the Spanish Population: A Secondary Analysis from the European Health Survey (2020). Biomedicines. 2023;11(8):2175. [86] LIN Y, DE ARAUJO I, STANLEY G, et al. Chronic pain precedes disrupted eating behavior in low-back pain patients. PLoS One, 2022;17(2):e263527. [87] IKEDA T, SUGIYAMA K, AIDA J, et al. Socioeconomic inequalities in low back pain among older people: the JAGES cross-sectional study. Int J Equity Health. 2019;18(1):15. [88] MAGNI G, CALDIERON C, RIGATTI-LUCHINI S, et al. Chronic musculoskeletal pain and depressive symptoms in the general population. An analysis of the 1st National Health and Nutrition Examination Survey data. Pain. 1990;43(3):299-307. [89] HURWITZ EL, MORGENSTERN H, YU F. Cross-sectional and longitudinal associations of low-back pain and related disability with psychological distress among patients enrolled in the UCLA Low-Back Pain Study. J Clin Epidemiol. 2003;56(5):463-471. [90] MEI Q, LI C, YIN Y, et al. The relationship between the psychological stress of adolescents in school and the prevalence of chronic low back pain: a cross-sectional study in China. Child Adolesc Psychiatry Ment Health. 2019;13:24. [91] MAHARTY DC, HINES SC, BROWN RB. Chronic Low Back Pain in Adults: Evaluation and Management. Am Fam Physician. 2024;109(3):233-244. [92] MuÑOZ-GARACH A, CORNEJO-PAREJA I, TINAHONES FJ. Does Metabolically Healthy Obesity Exist? Nutrients. 2016;8(6):320. [93] PERREAULT M, ZULYNIAK MA, BADOUD F, et al. A distinct fatty acid profile underlies the reduced inflammatory state of metabolically healthy obese individuals. PLoS One. 2014;9(2):e88539. [94] JUNG CH, LEE WJ, SONG K. Metabolically healthy obesity: a friend or foe? Korean J Intern Med. 2017;32(4):611-621. [95] LEAN ME, HAN T S, SEIDELL JC. Impairment of health and quality of life in people with large waist circumference. Lancet. 1998;351(9106): 853-856. [96] STREICHER SA, LIM U, PARK SL, et al. Genome-wide association study of abdominal MRI-measured visceral fat: The multiethnic cohort adiposity phenotype study. PLoS One. 2023;18(1):e279932. [97] CARROLL JF, CHIAPA AL, RODRIQUEZ M, et al. Visceral fat, waist circumference, and BMI: impact of race/ethnicity. Obesity (Silver Spring). 2008;16(3):600-607. [98] STEFAN N, HÄRING H, SCHULZE MB. Metabolically healthy obesity: the low-hanging fruit in obesity treatment? Lancet Diabetes Endocrinol. 2018;6(3):249-258. [99] MATHIS BJ, TANAKA K, HIRAMATSU Y. Metabolically Healthy Obesity: Are Interventions Useful? Curr Obes Rep. 2023;12(1):36-60. [100] ALQHTANI RS, AHMED H, GHULAM HSH, et al. Efficacy of Core-Strengthening and Intensive Dynamic Back Exercises on Pain, Core Muscle Endurance, and Functional Disability in Patients with Chronic Non-Specific Low Back Pain: A Randomized Comparative Study. J Clin Med. 2024;13(2):475. [101] LIU C, WANG C, GUAN S, et al. The Prevalence of Metabolically Healthy and Unhealthy Obesity according to Different Criteria. Obes Facts. 2019;12(1):78-90. [102] LAN Y, MAI Z, ZHOU S, et al. Prevalence of metabolic syndrome in China: An up-dated cross-sectional study. PLoS One. 2018;13(4): e196012. |
| [1] | 孙志远, 徐 凯, 田雪文, 商庆慧. 代谢功能障碍相关脂肪性肝病:共性和异质性途径介导的病理机制[J]. 中国组织工程研究, 2026, 30(28): 7378-7387. |
| [2] | 余圣涵, 成贤锴, 郑 跃, 杨 颖, . 基于Transformer-卷积神经网络模型实现单节点腰部康复训练动作识别任务[J]. 中国组织工程研究, 2026, 30(16): 4125-4136. |
| [3] | 周子贵, 刘菁菁. 三酰甘油-葡萄糖-体质量指数与中国中老年高血压的发病风险[J]. 中国组织工程研究, 2026, 30(16): 4137-4145. |
| [4] | 要俪娟, 王印凤, 马震南, 陈乐琴. 运动诱导细胞外囊泡:在胰岛素抵抗发生发展中的作用与机制[J]. 中国组织工程研究, 2026, 30(13): 3412-3423. |
| [5] | 王 鹏, 陆 欢, 刘海凤, 李 峰. 穿心莲内酯干预妊娠糖尿病模型大鼠胰岛素抵抗的作用机制[J]. 中国组织工程研究, 2026, 30(12): 3058-3065. |
| [6] | 王世杰, 胡骁宇, 段卓然, 唐英峰, 王 维. 握力体质量比和新发心脑血管疾病的关联:中国健康与养老追踪调查大数据分析[J]. 中国组织工程研究, 2026, 30(12): 3190-3197. |
| [7] | 蔡之幸, 夏秋芳, 陈莉莉, 朱丹阳, 朱慧雯, 孙亚男, 梁文玉, 赵鹤倩. 柔肌顺膵饮改善2型糖尿病小鼠骨骼肌胰岛素抵抗的作用[J]. 中国组织工程研究, 2025, 29(35): 7537-7543. |
| [8] | 刘 璇, 丁雨晴, 夏若寒, 汪献旺, 胡淑娟. 运动防治胰岛素抵抗:Keap1/核因子E2相关因子2信号通路的作用与分子机制[J]. 中国组织工程研究, 2025, 29(35): 7578-7588. |
| [9] | 陈春兰, 叶美仪, 潘雨薇, 袁 佳, 周朋君. 脐带间充质干细胞对 2 型糖尿病的免疫调节作用[J]. 中国组织工程研究, 2025, 29(23): 5031-5040. |
| [10] | 朱 鹏, 李瑛玉, 卢小倩, 吴 琼. 类胰岛素生长因子1对自然衰老小鼠的抗肥胖作用[J]. 中国组织工程研究, 2025, 29(12): 2536-2543. |
| [11] | 魏 娟, 李 婷, 郇梦婷, 谢 颖, 谢舟煜, 韦庆波, 吴云川. 静力性训练改善2型糖尿病骨骼肌胰岛素抵抗的机制[J]. 中国组织工程研究, 2024, 28(8): 1271-1276. |
| [12] | 梁 飞. 不同强度累积和持续运动对胰岛素抵抗小鼠肠黏膜通透性的影响[J]. 中国组织工程研究, 2024, 28(27): 4332-4339. |
| [13] | 郭项英, 彭子富, 何亦敏, 房洪波, 姜 宁. MiRNA-122在运动改善非酒精性脂肪肝中的作用[J]. 中国组织工程研究, 2024, 28(2): 272-279. |
| [14] | 刘仁凡, 吕丽婷, 伍 怡, 王 璐. 不同强度训练方式对2型糖尿病超重或肥胖者体成分及糖代谢影响的Meta分析[J]. 中国组织工程研究, 2024, 28(14): 2274-2281. |
| [15] | 张 艳, 何瑞波, 王庆博, 皮亦华, 陆春敏, 徐传仪, 马 刚, 彭 朋. 不同负荷量有氧运动对肥胖大鼠骨骼肌炎症反应和胰岛素信号途径的影响及机制[J]. 中国组织工程研究, 2023, 27(8): 1237-1244. |
肥胖诊断维度存在显著方法学异质性。体质量指数作为国际通用形态学诊断标准(世界卫生组织分类体系)虽具有操作简便性优势,但无法表现出体脂分布的异质性[18]。近年研究强调中心性肥胖在慢性腰痛机械负荷机制中的特异性作用,腰围作为内脏脂肪沉积的替代指标,其诊断价值已获美国心脏协会(AHA)指南认可[19-20]。
因此,基于美国国家健康与营养检查调查(National Health and Nutrition Examination Survey,NHANES)的多周期数据,此次研究通过双维度肥胖诊断框架(整体性肥胖与中心性肥胖)系统解构代谢健康型肥胖/代谢不健康型肥胖与慢性腰痛的流行病学关联,并量化社会人口学调节因子的潜在调控效应,创新性整合体质量指数与腰围双重诊断维度,通过代谢表型分层及社会人口学多变量校正模型(年龄、性别、教育程度等),旨在揭示肥胖表型异质性对慢性腰痛风险的差异化影响模式。
中国组织工程研究杂志出版内容重点:干细胞;骨髓干细胞;造血干细胞;脂肪干细胞;肿瘤干细胞;胚胎干细胞;脐带脐血干细胞;干细胞诱导;干细胞分化;组织工程
1.1 资料来源 横断面研究。
1.2 时间及地点 研究于2025年5月在广州中医药大学第三临床医学院完成。
1.3 资料 研究数据来自1999-2004年及2009-2010年的NHANES数据,研究数据来自于美国国家健康与营养检查调查,由美国疾病控制和预防中心(CDC)管理和监督。
研究人群:NHANES(网站:https://wwwn.cdc.gov/nchs/nhanes/Default.aspx)是由美国疾病控制和预防中心(CDC)管理的2年一次的横断面调查,旨在评估美国人口的健康和营养状况。NHANES调查方案已获得美国国家卫生统计中心伦理审查委员会的批准,所有参与者均已提供书面知情同意书。此次研究中的统计分析是对来自美国的代表性非机构样本进行,采用复杂的分层和多阶段设计。研究参与者最初在住所接受采访,随后在移动检查中心(MEC)接受健康检查。
此次研究的数据来自4个周期的NHANES数据,1999-2004年及2009-2010年,共有
41 663名参与者参与。排除腰痛、腰围、收缩压/舒张压、血糖、高密度胆固醇、甘油三酯、胰岛素、空腹血糖、体质量指数、婚姻状态、教育状态、贫富收入比、高血压状态、吸烟状态、关节炎、心脏病、脑卒中状态、癌症、糖尿病、骨质疏松缺失数据以及体质量指数< 18.5 kg/m2后,最终4 956名参与者被纳入研究分析(图1)。该分析框架通过加权处理,确保样本对目标人群的统计推断有效性。
1.4.1 暴露和结局变量 慢性腰痛样本的确定通过问卷调查,询问参与者“是否有一次,{您}几乎每天都有腰痛、疼痛或僵硬,连续3个月或更长时间?”问题,回答“是”的参与者被认定为存在慢性腰痛。
使用标准化问卷收集了人口统计学特征、教育水平、婚姻状况、吸烟状况、高血压状态、关节炎状态、冠心病状态、脑卒中状态、癌症状态、糖尿病状态、骨质疏松状态数据。在移动检查中心访视期间,使用标准方案的校准仪器测量身高、体质量、腰围、收缩压和舒张压。在美国国家健康与营养研究中心总参与者的子样本中收集空腹静脉血样本,并提取空腹血糖、胰岛素、总胆固醇、甘油三酯、高密度脂蛋白胆固醇相关指标。
根据2009年代谢综合征和胰岛素抵抗稳态模型评估协调标准定义代谢健康[21-22]。代谢综合征的5个组成部分中无任何1个符合被认为是代谢健康:①收缩压≥130 mmHg或舒张压≥85 mmHg或自报高血压或服用降压药;②空腹血糖≥5.6 mmol/L或自报糖尿病或服用降糖药;③男性高密度脂蛋白胆固醇< 1.03 mmol/L,女性< 1.29 mmol/L或使用降脂药物;④甘油三酯≥1.7 mmol/L或使用降脂药物;⑤胰岛素抵抗指数≥2.5(以胰岛素×葡萄糖/22.5计算),有≥1种组分的受试者则被归类为代谢不健康。
为全面探讨肥胖与慢性腰痛的关系,进一步使用体质量指数标准和腰围标准将参与者分为不同组。体质量指数的计算为体质量(kg)除以身高(m)的平方,根据世界卫生组织建议的临界值将其分为正常体质量(体质量指数18.5-24.9 kg/m2)、超重(体质量指数25.0-29.9 kg/m2)和肥胖(体质量指数≥30.0 kg/m2)[23]。对于腰围标准,根据世界卫生组织的建议,参与者也被分为3个组,对于男性,102 cm>腰围≥94 cm为中心型超重,腰围≥102 cm为中心型肥胖;对于女性,88 cm>腰围≥80 cm为中心型超重,腰围≥88 cm为中心型肥胖[20]。
最终,根据体质量指数标准结合代谢情况,参与者被分为6种表型:代谢健康型正常体质量、代谢健康型超重、代谢健康型肥胖、代谢不健康型正常体质量、代谢不健康型超重和代谢不健康型肥胖。类似地,根据腰围标准和代谢情况,参与者也被分类为相同的6种表型:代谢健康型正常体质量、代谢健康型超重、代谢健康型肥胖、代谢不健康型正常体质量、代谢不健康型超重和代谢不健康型肥胖[24]。
1.4.2 协变量 询问参与者一生中消费100支香烟的情况,一生中至少消费了100支香烟者被归类为吸烟者,否则为未吸烟者。此外,医疗专业人员通过询问参与者以下问题来诊断各种疾病,“医生或健康专业人员是否曾告诉过您患有 __?”这些个体报告了几种合并症,即冠心病、糖尿病、脑卒中、骨质疏松、关节炎、癌症、高血压等。
研究中检查的协变量包括年龄、性别、种族、教育水平、体质指数和贫富收入比,以及参与者提供的是否存在冠心病、糖尿病、脑卒中、骨质疏松、关节炎、癌症、高血压等病史信息。
性别分类为男性或女性。年龄作为连续变量进行分析。人种和种族分类为墨西哥裔美国人、其他西班牙裔、非西班牙裔白人、非西班牙裔黑人、其他种族(包括多种族墨西哥裔美国人)。婚姻状况分为“未婚”“结婚或同居”“丧偶、离婚或分离(婚姻解组状态)”。教育程度分为9年级以下、9-11年级(包括无文凭的12年级)、高中毕业/普通教育文凭或同等学历、部分专科或副学士学位、大学以上学历。吸烟状态(根据至少100支香烟/年的标准划分为吸烟和不吸烟)。冠心病、糖尿病、脑卒中、骨质疏松、关节炎、癌症、高血压等从调查问卷上获得,分类为患有和不患有。
1.5 主要观察指标 代谢健康肥胖表型与慢性腰痛的流行病学关联。
1.6 统计学分析 此次研究整合了来自4个NHANES的周期数据:1999-2004年、2009-2010年,所有统计分析均按照移动检查中心指南进行。鉴于NHANES中收集的数据是通过分层、多阶段概率样本设计获得的,使用调查分析程序来解释研究中的样本权重。根据不同的代谢健康-肥胖表型描述样本量和特征。分类变量的数据表示为加权比例( Squeeze and Excitation,SE),连续变量的数据表示为加权平均值±SE。采用Logistic回归模型计算比值比(Odds Ratio,OR)和95%置信区间(Confidence Interval,CI)。在3个模型中,使用多元Logistic回归研究代谢健康肥胖表型与慢性腰痛之间的关系。
①未调整模型:没有调整协变量;②模型1调整了性别、年龄、种族;③模型2调整了性别、年龄、种族、吸烟、骨质疏松、冠心病、脑卒中、癌症、空腹血糖、高密度脂蛋白胆固醇、甘油三酯、收缩压、舒张压和身高;④模型3:调整性别、种族、年龄、吸烟、骨质疏松、冠心病、脑卒中、肿瘤、空腹血糖、高密度脂蛋白胆固醇、甘油三酯、收缩压、舒张压、身高、胰岛素抵抗指数、胰岛素、关节炎、婚姻、教育。使用性别(男性/女性)、种族(墨西哥裔美国人、其他西班牙裔、非西班牙裔白人、非西班牙裔黑人、其他种族)、教育水平(9年级以下、9-11年级(包括无文凭的12年级)、高中毕业/普通教育文凭或同等学历、部分专科或副学士学位以及大学以上学历)、婚姻状态(未婚/已婚、同居/离异、丧偶或分居)、体质量指数(正常/超重/肥胖)、吸烟(有/无)、糖尿病状态(存在/无)、骨质疏松状态(存在/无)、关节炎状态(存在/无)、癌症状态(存在/无)、高血压状态(存在/无)、冠心病(存在/无)和脑卒中(存在/无)等分层因素,在亚组中检查代谢健康肥胖表型与慢性腰痛患者之间的关系。为了研究代谢健康和不健康参与者体质量指数/腰围与慢性腰痛之间的剂量-反应关系,利用加权限制3次样条(限制性立方样条)及阈值效应分析。所有分析均使用R 4.3版和Empower软件4.2。双侧 P < 0.05为差异有显著性意义。该文统计学方法已经广州中医药大学陆丽明专家审核。
然而,代谢不健康型肥胖的致病机制可能涉及多因素交互作用:①代谢异常的中介效应:胰岛素抵抗、慢性炎症及血脂紊乱可能通过促进椎间盘退变、神经根炎症或肌肉骨骼系统代谢失衡,直接加剧腰痛。例如,高胰岛素血症可激活核因子κB通路,促进促炎因子(如白细胞介素6、肿瘤坏死因子α)释放,加速椎间盘基质的降解[31-34]。具有炎症性质的瘦素会导致椎间盘退行性变,从而导致腰痛[35-38]。有研究表明,在脂肪组织增加的肥胖人群中会产生与C-反应蛋白水平升高的其他重要炎性细胞因子以及肿瘤坏死因子α、白细胞介素6,而这些细胞因子会加剧关节炎症和肌肉骨骼疼痛[39-42]。②机械负荷与脂肪分布的协同作用:代谢不健康型肥胖患者常伴随内脏脂肪堆积,其分泌的脂肪因子(如瘦素、脂联素)失衡可能加重腰椎负荷并诱发局部炎症反应[43-44]。例如,肥胖也可能通过增加腰椎的机械负荷而导致非特异性腰痛[45-46],并可能通过增加多余脂肪组织中炎症递质的分泌干扰椎间盘的愈合,参与腰椎根性疼痛的发展[47]。
代谢健康肥胖表型与慢性腰痛的关联呈现显著异质性,在表4的调整模型2中,代谢健康型肥胖-体质量指数组与发生慢性腰痛可能性呈边缘性正相关[OR(95%CI)=1.74(1.06,2.85),P=0.029 2];而经加入胰岛素抵抗指数、胰岛素浓度、关节炎、婚姻状态和教育状态调整进行敏感性分析后,其效应值降低且统计学显著性消失[OR(95%CI)=1.54(0.92,2.59),P=0.103 4]。这一矛盾可能源于以下原因:①代谢代偿机制的短期保护作用:代谢健康型肥胖人群保留正常的胰岛素敏感性和脂代谢稳态,可能通过减少炎症因子释放和氧化应激部分抵消肥胖的机械负荷[48-49]。例如,脂联素水平较高的代谢健康型肥胖个体可能通过抑制白细胞介素1β和环氧合酶2表达减轻椎间盘退变[50-53]。②代谢健康肥胖表型的不稳定性:长期随访研究显示,30%-40%的代谢健康型肥胖个体在5-10年内转化为代谢不健康状态[15,54],提示当前的横断面数据可能低估其远期风险。此外,代谢健康型肥胖的定义缺乏统一标准(如是否纳入内脏脂肪指标),可能导致分类偏倚[55]。尽管如此,此次研究提示代谢健康型肥胖对慢性腰痛的直接影响有限,但仍需警惕其作为“代谢缓冲期”的潜在风险。
此次研究中腰围与慢性腰痛的强关联[OR(95%CI)=1.02(1.01,1.02),P < 0.000 1]进一步支持中心性肥胖的独立危害。值得注意的是,代谢健康型肥胖虽保留正常代谢稳态(空腹血糖、血压等核心指标),但其发生慢性腰痛的概率在特定亚组中显著升高。例如,在吸烟者中,代谢健康型肥胖-体质量指数组发生慢性腰痛的概率较非吸烟者相对增加(吸烟者与非吸烟者OR:2.43 vs. 1.84),而关节炎共病进一步放大代谢健康型肥胖的效应[OR(95%CI)= 6.04(1.61,22.65)],代谢健康型肥胖的代谢保护效应可能因炎症负荷或行为风险因素(如吸烟)而被部分抵消,同时吸烟和关节炎显著放大代谢不健康型肥胖效应(吸烟OR=2.58;关节炎OR=3.31),提示环境与共病因素可能通过氧化应激和关节退变加剧代谢异常与慢性腰痛的恶性循环[56-59]。然而,腰围的效应在代谢健康人群中未达显著性[OR(95%CI)=1.01(0.99,1.02),P=0.249 5],提示:①体质量指数的全局性影响:作为整体肥胖指标,体质量指数可能更综合反映全身脂肪堆积对腰椎生物力学的负面影响[60-61];②腰围的代谢特异性:腰围对慢性腰痛的预测价值在代谢不健康人群中更突出,可能与其反映内脏脂肪堆积和胰岛素抵抗程度密切相关[62-63]。
周永慧等[64]研究发现,体质量指数25.0-35.0 kg/m2人群患有腰痛的概率明显大于体质量指数18.5-24.9 kg/m2的人群,与此次研究发现体质量指数与发生慢性腰痛的概率呈显著正相关一致。此次研究发现,体质量指数≥39.73 kg/m²为代谢不健康人群的风险阈值,当体质量指数≥39.73kg/m²时发生慢性腰痛概率增幅显著升高[OR(95%CI)=1.09(1.03,1.14),P=0.001],提示超重管理应针对不同代谢状态分层干预[65-66]:①代谢不健康人群:需优先控制体质量指数< 40 kg/m²,并结合腰围监测(如男性< 102 cm,女性< 88 cm)以降低机械与代谢双重负荷。②代谢健康人群:尽管体质量指数关联较弱,仍需关注肥胖相关的生物力学改变(如椎间盘压力增高)[67-68]。限制性立方样曲线和阈值效应分析显示,体质量指数在总人群和代谢不健康人群中增大发生慢性腰痛的概率,代谢健康人群发生慢性腰痛的概率[OR(95%CI)=1.04(1.00,1.08)]显著低于代谢不健康(体质量指数≥39.73 kg/m²)人群[OR(95%CI)=1.09(1.03,1.14)],提示即使代谢健康状态下,重度肥胖仍可能通过机械负荷途径增加发生慢性腰痛可能,这与日本的一项关于体型较胖男性出现腰痛发作风险更高的前瞻性研究一致[69]。
此外,研究发现,社会决定因素在代谢健康肥胖表型-慢性腰痛关联中发挥重要调节作用[70-73]。低教育水平与低收入显著增强代谢健康肥胖表型的慢性腰痛可能[74-75],如一项欧洲的研究表明,教育不平等导致女性背部疼痛患病率上升[76] ,而婚姻解组状态(丧偶/离异或分居)的效应值(OR=1.63)高于已婚人群(OR=1.41),这一发现与“社会代谢复合暴露”理论一致,即社会经济劣势可能通过慢性应激和健康行为差异加剧肥胖相关的生物力学损伤[77-81],正如此次研究所发现的低教育水平、低收入及丧偶/离异或分居状态增加慢性腰痛可能一致[82-84]。另外,低收入群体由于经济限制往往肥胖相关疼痛的未治疗率较高,可能加重慢性腰痛[85-87]。研究表明,尽管抑郁和焦虑尚未被确定为背痛的特定原因,但大量数据显示,与一般人群相比,患有慢性腰痛个体的抑郁和焦虑发生率更高[88-90]。这些发现提示慢性腰痛的防控需整合社会支持政策(如社区健康促进项目)与个体化医学干预,尤其需关注弱势群体的多维健康需求[91]。
需要强调的是,此次研究为横断面设计,无法确立代谢健康状态与慢性腰痛之间的因果关系,反向因果关系(即慢性腰痛导致活动受限,进而诱发或加重代谢紊乱)的可能性不能被排除。由于此次研究采用胰岛素抵抗指数≥2.5和代谢综合征组分定义代谢状态,但未纳入内脏脂肪或脂肪因子(如瘦素/脂联素比值),可能影响分类准确性,尽管采用美国心脏协会标准定义代谢健康,但代谢健康肥胖表型中仍存在未被完全捕获的亚临床炎症或脂肪分布异质性[92-94]。例如,敏感性分析中腰围定义的代谢健康型肥胖(腰围-代谢健康肥胖表型)较体质量指数-代谢健康肥胖表型显示更强的发生慢性腰痛可能趋势(OR=1.46 vs. 1.54),这提示中心性脂肪沉积可能独立于代谢指标影响慢性腰痛病理进程[95]。在数据缺失与测量偏倚中,NHANES依赖自我报告确定慢性腰痛,可能存在回忆偏倚;此外,尽管研究通过双维度肥胖分类(体质量指数/腰围)系统解析代谢健康肥胖表型-慢性腰痛关联,为代谢肥胖表型异质性提供了流行病学证据,然而横断面设计限制因果推断,加上此次研究缺乏椎间盘退变、椎体终板改变、椎旁肌肉脂肪浸润或肌肉质量/力量等直接的影像学或生物力学数据,这一缺失限制了人们深入探讨肥胖(无论是代谢健康与否)导致慢性腰痛的具体病理生理机制,特别是无法区分和量化机械性负荷(如椎间盘压力增加、关节突关节应力增大)与系统性代谢因素(如炎症、脂肪因子)各自的作用以及它们如何相互作用最终导致组织损伤(如椎间盘退变加速、肌肉功能下降)和疼痛感知。 未来研究结合影像学、生物标志物和详细的疼痛评估将有助于阐明这些复杂的机制。
未来应当考虑纵向队列与机制研究,设计前瞻性研究进一步验证代谢/肥胖与慢性腰痛的因果关系,并结合生物标志物(如炎症因子、脂肪分布影像)阐明代谢-机械交互机制。通过临床干预试验,探索针对代谢不健康型肥胖人群的综合干预策略(如减重手术联合抗炎治疗)对慢性腰痛的预防效果以及借助社会医学整合,开发基于社区的多维度干预模式,将代谢管理、疼痛康复与社会支持相结合,尤其针对低教育/低收入群体。
此次研究证实代谢不健康肥胖是慢性腰痛的强独立危险因素,而代谢健康肥胖的短期风险较低,但仍需警惕其远期转化的风险。临床实践中应做到:①优先筛查代谢不健康型肥胖人群:对体质量指数≥30 kg/m²且合并代谢异常者,建议定期疼痛评估与早期干预。②个性化体质量管理:针对代谢状态制定差异化管理目标,如代谢不健康型肥胖人群以体质量指数< 40 kg/m²为短期目标,对于代谢健康型肥胖人群,应以维持当前代谢健康状态和预防向代谢不健康型肥胖转化为重点的个性化体重管理策略,可能有助于降低其未来发生慢性腰痛的风险。③整合社会支持:通过政策倾斜与健康教育改善弱势群体的健康行为,减少慢性腰痛的社会决定因素。未来研究需结合多组学技术与真实世界数据,进一步揭示肥胖、代谢异常与慢性腰痛的复杂网络,为精准防控提供依据。
采用国际数据库、美国群体分析对中国生物医学具有以下几点借鉴意义: ①此次研究提供跨种族比较的理论框架,欧美人群研究中建立的代谢健康肥胖表型与慢性腰痛关联模型(如炎症通路、代谢-骨骼肌交互机制),可为探索中国人群同类疾病的异质性提供假设基础。通过对比种族间效应量差异(如亚洲人群更低的内脏脂肪阈值)有助于揭示遗传与环境因素的调控作用[96-97]。②有助于推动精准分型的临床实践,国际研究证实代谢健康型肥胖是肥胖管理中需区别对待的亚型,这提示中国临床工作者需警惕‘一刀切’减重策略[98-99]。对代谢健康但超重/肥胖的慢性腰痛患者,应优先强化核心肌群康复而非单纯减重,避免过度医疗化干预[100]。③能验证表型定义的普适性,欧美采用的代谢健康肥胖表型标准(如胰岛素抵抗指数< 2.5、无代谢综合征)在中国人群中的预测效度尚存争议[101]。此次研究提示的腰痛风险关联,可推动建立适合中国代谢特征的代谢健康肥胖表型诊断阈值(如纳入尿酸、肝酶等东亚敏感指标),促进精准分型本土化。④还能警示潜在公共卫生负担,例如:中国正经历肥胖率激增但代谢异常率低于欧美的“代谢健康窗口期”[102]。该研究发现代谢健康型肥胖群体仍存在显著腰痛风险,提示中国需提前防控肥胖相关肌骨疾病,避免重蹈欧美“先肥胖后并发症”的医疗负担覆辙。
中国组织工程研究杂志出版内容重点:干细胞;骨髓干细胞;造血干细胞;脂肪干细胞;肿瘤干细胞;胚胎干细胞;脐带脐血干细胞;干细胞诱导;干细胞分化;组织工程
此次研究基于美国国家健康与营养调查(NHANES)具有全国代表性的大样本数据,深入探讨了不同代谢健康-肥胖表型(特别是代谢健康型肥胖和代谢不健康型肥胖)与慢性腰痛的流行病学关联,为代谢健康肥胖与腰痛的复杂关系提供了新的分层证据。此次研究的主要亮点包括:①聚焦前沿表型,揭示分层风险: 突破传统体质指数分类局限,结合代谢状态(健康/不健康)与肥胖程度(正常/超重/肥胖)定义六种精细表型(代谢健康正常体质量,代谢健康超重,代谢健康肥胖,代谢不健康正常体质量,代谢不健康超重和代谢不健康肥胖),首次系统评估了代谢健康型肥胖这一特殊人群的慢性腰痛风险,明确了代谢不健康肥胖与慢性腰痛存在最显著的正向独立关联,其风险显著高于代谢健康型正常体重人群,这提示代谢健康状态可能部分缓冲肥胖对慢性腰痛的不利影响。②大样本强证据,控制广泛混杂: 利用NHANES数据库优势,纳入4956名成人参与者,确保了结果的代表性和统计效力。通过多变量Logistic回归严格调整了人口学(年龄、性别、种族)、社会经济(教育、收入)、行为(吸烟、饮酒)及多种共病(糖尿病、关节炎等)等潜在混杂因素,增强了关联结果的稳健性和独立性。③引发机制探讨,指明未来方向: 研究结果强烈提示代谢因素(而不仅是机械负荷)在肥胖相关慢性腰痛中的核心作用,并支持代谢健康型肥胖可能存在内源性保护机制(如脂肪因子谱差异)的假说。这为未来研究探索脂联素等生物标志物、椎间盘退变影像学改变及机械-代谢交互作用等具体病理机制指明了方向。
中国组织工程研究杂志出版内容重点:干细胞;骨髓干细胞;造血干细胞;脂肪干细胞;肿瘤干细胞;胚胎干细胞;脐带脐血干细胞;干细胞诱导;干细胞分化;组织工程
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||