[1] HU Y, XU R, CHEN C, et al. Extracellular vesicles from human umbilical cord blood ameliorate bone loss in senile osteoporotic mice. Metabolism. 2019;95:93-101.
[2] HEGEWALD AB, BREITWIESER K, OTTINGER SM, et al. Extracellular miR-574-5p Induces Osteoclast Differentiation via TLR 7/8 in Rheumatoid Arthritis. Front Immunol. 2020;11:585282.
[3] MI B, CHEN L, XIONG Y, et al. Osteoblast/Osteoclast and Immune Cocktail Therapy of an Exosome/Drug Delivery Multifunctional Hydrogel Accelerates Fracture Repair. ACS Nano. 2022;16(1):771-782.
[4] PAVONE V, CHISARI E, VESCIO A, et al. Aetiology of Legg-Calvé-Perthes disease: A systematic review. World J Orthop. 2019;10(3):145-165.
[5] MA Q, LIANG M, WU Y, et al. Small extracellular vesicles deliver osteolytic effectors and mediate cancer-induced osteolysis in bone metastatic niche. J Extracell Vesicles. 2021;10(4):e12068.
[6] SOBACCHI C, SCHULZ A, COXON FP, et al. Osteopetrosis: genetics, treatment and new insights into osteoclast function. Nat Rev Endocrinol. 2013;9(9): 522-536.
[7] LU B, JIAO Y, WANG Y, et al. A FKBP5 mutation is associated with Paget’s disease of bone and enhances osteoclastogenesis. Exp Mol Med. 2017; 49(5):e336.
[8] LIU M, SUN Y, ZHANG Q. Emerging Role of Extracellular Vesicles in Bone Remodeling. J Dent Res. 2018;97(8):859-868.
[9] 陈逸青,章秋,代芳.外泌体在骨重建以及骨质疏松中的研究进展[J].中国骨质疏松杂志,2020,26(1):129-134.
[10] LI Q, LI C, ZHANG W, et al. Potential Effects of Exosomes and their MicroRNA Carrier on Osteoporosis. 2022;28(11):899-909.
[11] FENG Q, ZHENG S, ZHENG J. The emerging role of microRNAs in bone remodeling and its therapeutic implications for osteoporosis. Biosci Rep. 2018; 38(3):BSR20180453.
[12] KO NY, CHEN LR, CHEN KH. The Role of Micro RNA and Long-Non-Coding RNA in Osteoporosis. Int J Mol Sci. 2020;21(14):4886.
[13] PONTING CP, OLIVER PL, REIK W. Evolution and functions of long noncoding RNAs. Cell. 2009;136(4):629-641.
[14] GOODALL GJ, WICKRAMASINGHE VO. RNA in cancer. Nat Rev Cancer. 2021; 21(1): 22-36.
[15] SHI X, SUN M, LIU H, et al. Long non-coding RNAs: a new frontier in the study of human diseases. Cancer Lett. 2013;339(2):159-166.
[16] WILUSZ JE, SUNWOO H, SPECTOR DL. Long noncoding RNAs: functional surprises from the RNA world. Genes Dev. 2009;23(13):1494-1504.
[17] GAO M, ZHANG Z, SUN J, et al. The roles of circRNA-miRNA-mRNA networks in the development and treatment of osteoporosis. Front Endocrinol (Lausanne). 2022;13:945310.
[18] OTON-GONZALEZ L, MAZZIOTTA C, IAQUINTA MR, et al. Genetics and Epigenetics of Bone Remodeling and Metabolic Bone Diseases. Int J Mol Sci. 2022;23(3):1500.
[19] LI D, LIU J, GUO B, et al. Osteoclast-derived exosomal miR-214-3p inhibits osteoblastic bone formation. Nat Commun. 2016;7:10872.
[20] HOLLIDAY LS, MCHUGH KP, ZUO J, et al. Exosomes: novel regulators of bone remodelling and potential therapeutic agents for orthodontics. Orthod Craniofac Res. 2017;20 Suppl 1(Suppl 1):95-99.
[21] HUANG X, XIONG X, LIU J, et al. MicroRNAs-containing extracellular vesicles in bone remodeling: An emerging frontier. Life Sci. 2020;254:117809.
[22] SADU L, KRISHNAN RH, AKSHAYA RL, et al. Exosomes in bone remodeling and breast cancer bone metastasis. Prog Biophys Mol Biol. 2022;175:120-130.
[23] PEPE J, ROSSI M, BATTAFARANO G, et al. Characterization of Extracellular Vesicles in Osteoporotic Patients Compared to Osteopenic and Healthy Controls. J Bone Miner Res. 2022;37(11):2186-2200.
[24] XU R, SHEN X, XIE H, et al. Identification of the canonical and noncanonical role of miR-143/145 in estrogen-deficient bone loss. Theranostics. 2021; 11(11): 5491-510.
[25] LI Y, JIN D, XIE W, et al. Mesenchymal Stem Cells-Derived Exosomes: A Possible Therapeutic Strategy for Osteoporosis. Curr Stem Cell Res Ther. 2018;13(5):362-368.
[26] XIE Y, CHEN Y, ZHANG L, et al. The roles of bone-derived exosomes and exosomal microRNAs in regulating bone remodelling. J Cell Mol Med. 2017; 21(5):1033-1041.
[27] LUO ZW, LI FX, LIU YW, et al. Aptamer-functionalized exosomes from bone marrow stromal cells target bone to promote bone regeneration. Nanoscale. 2019;11(43):20884-20892.
[28] LAI G, ZHAO R, ZHUANG W, et al. BMSC-derived exosomal miR-27a-3p and miR-196b-5p regulate bone remodeling in ovariectomized rats. PeerJ. 2022;10:e13744.
[29] XU R, SHEN X, SI Y, et al. MicroRNA-31a-5p from aging BMSCs links bone formation and resorption in the aged bone marrow microenvironment. Aging Cell. 2018;17(4):e12794.
[30] FOESSL I, KOTZBECK P, OBERMAYER-PIETSCH B. miRNAs as novel biomarkers for bone related diseases. J Lab Precis Med. 2019;4:2-13.
[31] WU P, JIAO F, HUANG H, et al. Morinda officinalis polysaccharide enable suppression of osteoclastic differentiation by exosomes derived from rat mesenchymal stem cells. Pharm Biol. 2022;60(1):1303-1316.
[32] WANG Y, ZHOU X, WANG D. Mesenchymal Stem Cell-Derived Extracellular Vesicles Inhibit Osteoporosis via MicroRNA-27a-Induced Inhibition of DKK2-Mediated Wnt/β-Catenin Pathway. Inflammation. 2022;45(2):780-799.
[33] MINAMIZAKI T, NAKAO Y, IRIE Y, et al. The matrix vesicle cargo miR-125b accumulates in the bone matrix, inhibiting bone resorption in mice. Commun Biol. 2020;3(1):30.
[34] MURACA M, CAPPARIELLO A. The Role of Extracellular Vesicles (EVs) in the Epigenetic Regulation of Bone Metabolism and Osteoporosis. Int J Mol Sci. 2020;21(22):8682.
[35] ZHAO J, HUANG M, ZHANG X, et al. MiR-146a Deletion Protects From Bone Loss in OVX Mice by Suppressing RANKL/OPG and M-CSF in Bone Microenvironment. J Bone Miner Res. 2019;34(11):2149-2161.
[36] LEE KS, LEE J, KIM HK, et al. Extracellular vesicles from adipose tissue-derived stem cells alleviate osteoporosis through osteoprotegerin and miR-21-5p. J Extracell Vesicles. 2021;10(12):e12152.
[37] HE Y, WUERTZ-KOZAK K, KUEHL L, et al. Extracellular Vesicles: Potential Mediators of Psychosocial Stress Contribution to Osteoporosis? Int J Mol Sci. 2021;22(11):5846.
[38] SONG H, LI X, ZHAO Z, et al. Reversal of Osteoporotic Activity by Endothelial Cell-Secreted Bone Targeting and Biocompatible Exosomes. Nano Lett. 2019;19(5):3040-3048.
[39] GUO L, ZHU Y, LI L, et al. Breast cancer cell-derived exosomal miR-20a-5p promotes the proliferation and differentiation of osteoclasts by targeting SRCIN1. Cancer Med. 2019;8(12):5687-5701.
[40] WU K, FENG J, LYU F, et al. Exosomal miR-19a and IBSP cooperate to induce osteolytic bone metastasis of estrogen receptor-positive breast cancer. Nat Commun. 2021;12(1):5196.
[41] LI Q, HUANG Q, WANG Y, et al. Extracellular vesicle-mediated bone metabolism in the bone microenvironment. J Bone Miner Metab. 2018;36(1):1-11.
[42] KAGIYA T. MicroRNAs: Potential Biomarkers and Therapeutic Targets for Alveolar Bone Loss in Periodontal Disease. Int J Mol Sci. 2016;17(8):1317.
[43] YU L, SUI B, FAN W, et al. Exosomes derived from osteogenic tumor activate osteoclast differentiation and concurrently inhibit osteogenesis by transferring COL1A1-targeting miRNA-92a-1-5p. J Extracell Vesicles. 2021;10(3):e12056.
[44] YUAN X, QIAN N, LING S, et al. Breast cancer exosomes contribute to pre-metastatic niche formation and promote bone metastasis of tumor cells. Theranostics. 2021;11(3):1429-1445.
[45] XU Z, LIU X, WANG H, et al. Lung adenocarcinoma cell-derived exosomal miR-21 facilitates osteoclastogenesis. Gene. 2018;666:116-122.
[46] KAGIYA T. MicroRNAs and Osteolytic Bone Metastasis: The Roles of MicroRNAs in Tumor-Induced Osteoclast Differentiation. J Clin Med. 2015; 4(9):1741-1752.
[47] LUO T, ZHOU X, JIANG E, et al. Osteosarcoma Cell-Derived Small Extracellular Vesicles Enhance Osteoclastogenesis and Bone Resorption Through Transferring MicroRNA-19a-3p. Front Oncol. 2021;11:618662.
[48] LIN L, WANG H, GUO W, et al. Osteosarcoma-derived exosomal miR-501-3p promotes osteoclastogenesis and aggravates bone loss. Cell Signal. 2021; 82:109935.
[49] LI S. The basic characteristics of extracellular vesicles and their potential application in bone sarcomas. J Nanobiotechnology. 2021;19(1):277.
[50] GUO S, GU J, MA J, et al. GATA4-driven miR-206-3p signatures control orofacial bone development by regulating osteogenic and osteoclastic activity. Theranostics. 2021;11(17):8379-8395.
[51] NAKAO Y, FUKUDA T, ZHANG Q, et al. Exosomes from TNF-α-treated human gingiva-derived MSCs enhance M2 macrophage polarization and inhibit periodontal bone loss. Acta Biomater. 2021;122:306-324.
[52] TIAN J, CHEN W, XIONG Y, et al. Small extracellular vesicles derived from hypoxic preconditioned dental pulp stem cells ameliorate inflammatory osteolysis by modulating macrophage polarization and osteoclastogenesis. Bioact Mater. 2022;22:326-342.
[53] XU C, ZHANG Z, LIU N, et al. Small extracellular vesicle-mediated miR-320e transmission promotes osteogenesis in OPLL by targeting TAK1. Nat Commun. 2022;13(1):2467.
[54] HUANG Q, LI B, LIN C, et al. MicroRNA sequence analysis of plasma exosomes in early Legg-Calvé-Perthes disease. Cell Signal. 2022;91:110184.
[55] DONATE PB, ALVES DE LIMA K, PERES RS, et al. Cigarette smoke induces miR-132 in Th17 cells that enhance osteoclastogenesis in inflammatory arthritis. Proc Natl Acad Sci U S A. 2021;118(1):e2017120118.
[56] TAKAMURA Y, AOKI W, SATOMURA A, et al. Small RNAs detected in exosomes derived from the MH7A synovial fibroblast cell line with TNF-α stimulation. PloS one. 2018;13(8):e0201851.
[57] CHANG C, XU L, ZHANG R, et al. MicroRNA-Mediated Epigenetic Regulation of Rheumatoid Arthritis Susceptibility and Pathogenesis. Front Immunol. 2022;13:838884.
[58] FENG W, JIN Q, MING-YU Y, et al. MiR-6924-5p-rich exosomes derived from genetically modified Scleraxis-overexpressing PDGFRα(+) BMMSCs as novel nanotherapeutics for treating osteolysis during tendon-bone healing and improving healing strength. Biomaterials. 2021;279:121242.
[59] SINGLETON Q, VAIBHAV K, BRAUN M, et al. Bone Marrow Derived Extracellular Vesicles Activate Osteoclast Differentiation in Traumatic Brain Injury Induced Bone Loss. Cells. 2019;8(1):63.
[60] HU CH, SUI B D, LIU J, et al. Sympathetic Neurostress Drives Osteoblastic Exosomal MiR-21 Transfer to Disrupt Bone Homeostasis and Promote Osteopenia. Small Methods. 2022;6(3):e2100763.
[61] GONG N, ZHU W, XU R, et al. Keratinocytes-derived exosomal miRNA regulates osteoclast differentiation in middle ear cholesteatoma. Biochem Biophys Res Commun. 2020;525(2):341-347.
[62] MEI B, WANG Y, YE W, et al. LncRNA ZBTB40-IT1 modulated by osteoporosis GWAS risk SNPs suppresses osteogenesis. Hum Genet. 2019;138(2):151-166.
[63] LIU C, CAO Z, BAI Y, et al. LncRNA AK077216 promotes RANKL-induced osteoclastogenesis and bone resorption via NFATc1 by inhibition of NIP45. J Cell Physiol. 2019;234(2):1606-1617.
[64] YANG Z, LIU X, ZHAO F, et al. Bioactive glass nanoparticles inhibit osteoclast differentiation and osteoporotic bone loss by activating lncRNA NRON expression in the extracellular vesicles derived from bone marrow mesenchymal stem cells. Biomaterials. 2022;283:121438.
[65] LI C, WANG S, XING Z, et al. A ROR1-HER3-lncRNA signalling axis modulates the Hippo-YAP pathway to regulate bone metastasis. Nat Cell Biol. 2017; 19(2):106-119.
[66] NI J, ZHANG X, LI J, et al. Tumour-derived exosomal lncRNA-SOX2OT promotes bone metastasis of non-small cell lung cancer by targeting the miRNA-194-5p/RAC1 signalling axis in osteoclasts. Cell Death Dis. 2021;12(7):662.
[67] SONG J, KIM D, HAN J, et al. PBMC and exosome-derived Hotair is a critical regulator and potent marker for rheumatoid arthritis. Clin Exp Med. 2015; 15(1):121-126.
[68] DOU C, CAO Z, YANG B, et al. Changing expression profiles of lncRNAs, mRNAs, circRNAs and miRNAs during osteoclastogenesis. Sci Rep. 2016;6: 21499.
[69] WANG W, QIAO S, WU X, et al. Circ_0008542 in osteoblast exosomes promotes osteoclast-induced bone resorption through m6A methylation. Cell Death Dis. 2021;12(7):628.
[70] PUPPO M, JAAFAR M, DIAZ JJ, et al. MiRNAs and snoRNAs in Bone Metastasis: Functional Roles and Clinical Potential. Cancers (Basel). 2022;15(1):242.
[71] RAI AK, RAJAN KS, BISSERIER M, et al. Spaceflight-Associated Changes of snoRNAs in Peripheral Blood Mononuclear Cells and Plasma Exosomes-A Pilot Study. Front Cardiovasc Med. 2022;9:886689. |

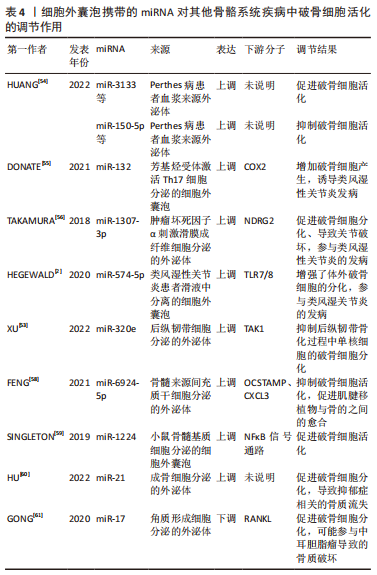
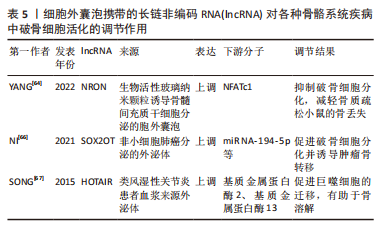

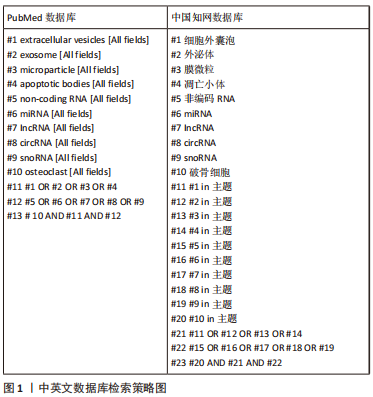
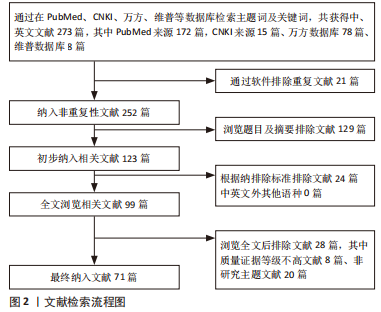
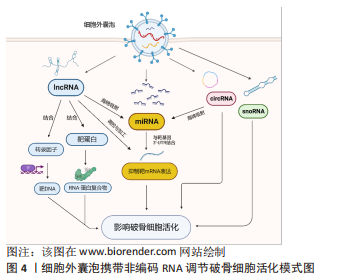 目前对细胞外囊泡携带的非编码RNA在破骨细胞活化中的作用机制研究进展很少报道,此文对明确非编码RNA介导的破骨细胞活化如何参与疾病进展提供了新思路,但同时也存在局限:①细胞外囊泡携带的miRNA、IncRNA和circRNA参与破骨细胞活化相关的骨稳态失衡过程的具体机制复杂多样,以往的细胞外囊泡携带非编码RNA对破骨细胞活化的调节的研究基本集中于miRNA,且部分研究尚未进一步阐明调控机制。②细胞外囊泡中的其他非编码RNA如snoRNA、scRNA等是否参与破骨细胞活化尚未有研究证实,而lncRNA和circRNA的调节机制的研究仍处于体外实验的阶段,尚缺乏体内实验及临床试验进一步研究。③细胞外囊泡是否可携带多种非编码RNA协同介导破骨细胞活化从而影响骨稳态尚不清楚。
目前对细胞外囊泡携带的非编码RNA在破骨细胞活化中的作用机制研究进展很少报道,此文对明确非编码RNA介导的破骨细胞活化如何参与疾病进展提供了新思路,但同时也存在局限:①细胞外囊泡携带的miRNA、IncRNA和circRNA参与破骨细胞活化相关的骨稳态失衡过程的具体机制复杂多样,以往的细胞外囊泡携带非编码RNA对破骨细胞活化的调节的研究基本集中于miRNA,且部分研究尚未进一步阐明调控机制。②细胞外囊泡中的其他非编码RNA如snoRNA、scRNA等是否参与破骨细胞活化尚未有研究证实,而lncRNA和circRNA的调节机制的研究仍处于体外实验的阶段,尚缺乏体内实验及临床试验进一步研究。③细胞外囊泡是否可携带多种非编码RNA协同介导破骨细胞活化从而影响骨稳态尚不清楚。