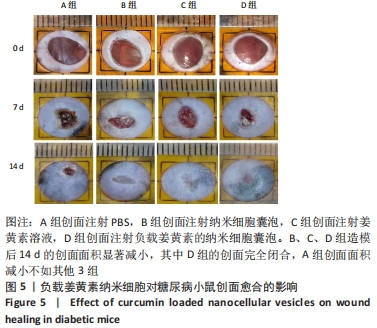
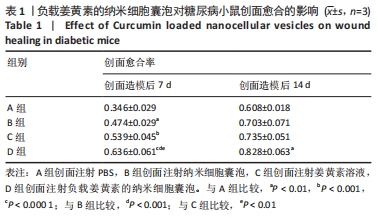
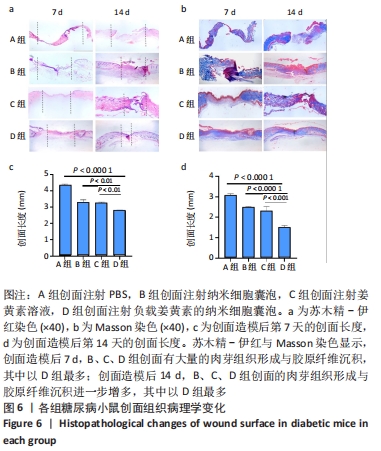
[1] LI Y, XU TZ, TU ZL, et al. Bioactive antibacterial silica-based nanocomposites hydrogel scaffolds with high angiogenesis for promoting diabetic wound healing and skin repair. Theranostics. 2020; 10(11):4929-4943.
[2] International Diabetes Federation. IDF Diabetes Atlas-10th Edition. DiabetesAtlas http://www.diabetesatlas.org/ (2021).
[3] PATEL S, SRIVASTAVA S, SINGH MR, et al, Mechanistic insight into diabetic wounds: Pathogenesis, molecular targets and treatment strategies to pace wound healing. Biomed Pharmacother. 2019;112: 108615.
[4] Bakker K, Apelqvist J, Lipsky BA, et al. The 2015 IWGDF guidance documents on prevention and management of foot problems in diabetes: development of an evidence-based global consensus. Diabetes Metab Res Rev. 2016;32 Suppl 1:2-6.
[5] Chan YW, So C, Yau KL, et al. Adipose-derived stem cells and cancer cells fuse to generate cancer stem cell-like cells with increased tumorigenicity. J Cell Physiol. 2020;235(10):6794-6807.
[6] Riedl J, Popp C, Eide C, et al. Mesenchymal stromal cells in wound healing applications: role of the secretome, targeted delivery and impact on recessive dystrophic epidermolysis bullosa treatment. Cytotherapy. 2021;23(11):961-973.
[7] Choi YJ, Yi HG, Kim SW, et al. 3Dcell printedtissue analogues:anew platformfor theranostics. Theranostics. 2017;7(12):3118.
[8] Yang JY, Chen ZY, Pan DY, et al. Umbilical Cord-Derived Mesenchymal Stem Cell-Derived Exosomes Combined Pluronic F127 Hydrogel Promote Chronic Diabetic Wound Healing and Complete Skin Regeneration. Int J Nanomedicine. 2020;15:5911-5926.
[9] Xunian Z ,Kalluri R. The Biology and Therapeutic Potential of Mesenchymal Stem Cells derived Exosomes. Cancer Sci. 2020;111(9): 3100-3110.
[10] Ferguson SW, Nguyen J. Exosomes as therapeutics: The implications of molecular composition and exosomal heterogeneity. J Control Release. 2016;228:179-190.
[11] Hu YQ, Wu B, Xiong Y, et al. Cryogenic 3D Printed Hydrogel Scaffolds Loading Exosomes Accelerate Diabetic Wound Healing. Chem Eng J. 2021;(9):130634.
[12] Huang JH, Yu M , Yin WJ, et al. Development of a novel RNAi therapy: Engineered miR-31 exosomes promoted the healing of diabetic wounds. Bioact Mater. 2021;6(9):2841-2853.
[13] Guo SC, Tao SC, Yin WJ, et al. Exosomes derived from platelet-rich plasma promote the re-epithelization of chronic cutaneous wounds via activation of YAP in a diabetic rat model. Theranostics. 2017;7(1):81-96.
[14] Jang SC, Kim OY, Yoon CM, et al. Bioinspired exosome-mimetic nanovesicles for targeted delivery of chemotherapeutics to malignant tumors. ACS Nano. 2013;7(9):7698-7710.
[15] AlQahtani SA, Harisa GI, Badran MM, et al. Nano-erythrocyte membrane-chaperoned 5-fluorouracil liposomes as biomimetic delivery platforms to target hepatocellular carcinoma cell lines. Artif Cells Nanomed Biotechnol. 2019;47(1):989-996.
[16] Fereydouni N, Darroudi M, Movaffagh J, et al. Curcumin nanofibers for the purpose of wound healing. J Cell Physiol. 2019; 234(5):5537-5554.
[17] Mokhtari M, Razzaghi R, Mansooreh MH. The effects of Curcumin intake on wound healing and metabolic status in patients with diabetic foot ulcer: A randomized, double-blind, placebo-controlled trial. Phytother Res. 2021;35(4):2099-2107.
[18] Mohanty C, Pradhan J. A human epidermal growth factor-Curcumin bandage bioconjugate loaded with mesenchymal stem cell for in vivo diabetic wound healing. Mater Sci Eng C Mater Biol Appl. 2020;111:110751.
[19] Li F, Shi YJ, Liang J, et al. Curcumin-loaded chitosan nanoparticles promote diabetic wound healing via attenuating inflammation in a diabetic rat model. J Biomater Appl. 2019;34(4):476-486.
[20] Feng T, Wei YM, Lee RJ, et al. Liposomal Curcumin and its application in cancer. Int J Nanomedicine. 2017;12:6027-6044.
[21] Ghufran H, Mehmood A, Azam M, et al. Curcumin preconditioned human adipose derived stem cells co-transplanted with platelet rich plasma improve wound healing in diabetic rats. Life Sci. 2020;257: 118091.
[22] Liu YF, Li Z, Li JJ, et al. Stiffness-mediated mesenchymal stem cell fate decision in 3D-bioprinted hydrogels. Burns Trauma. 2020;8:tkaa029.
[23] Fan JB, Lee CS, Kim S, et al. Generation of Small RNA-Modulated Exosome Mimetics for Bone Regeneration. ACS Nano. 2020;14(9): 11973-11984.
[24] Wang QR, Ye CQ, Sun SK, et al. Curcumin attenuates collagen-induced rat arthritis via anti-inflammatoryand apoptotic effects. Int Immunopharmaco. 2019;72:292-300.
[25] Wang CG, Wang M, Xu TZ, et al. Engineering Bioactive Self-Healing Antibacterial Exosomes Hydrogel for Promoting Chronic Diabetic Wound Healing and Complete Skin Regeneration. Theranostics. 2019; 9(1):65-76.
[26] Ahmadi H, Amini A, Fathabady FF, et al.Transplantation of photobiomodulation-preconditioned diabetic stem cells accelerates ischemic wound healing in diabetic rats. Stem Cell Res Ther. 2020; 11(1):494.
[27] Alamdari NM, Mehraneroodi B, Gholizadeh B, et al. The efficacy of negative pressure wound therapy compared with conventional dressing in treating infected diabetic foot ulcers: a randomized controlled trial. Int J Diabetes Dev C. 2021(9).doi:10.1007/s13410-021-00941-9
[28] Abolgheit S, Abdelkader S, Aboushelib M, et al. Bone marrow-derived mesenchymal stem cells and extracellular vesicles enriched collagen chitosan scaffold in skin wound healing (a rat model). J Biomater Appl. 2021;36(1):128-139.
[29] Nikfarjam S, Rezaie J , Zolbanin NM, et al. Mesenchymal Stem Cell Derived-Exosomes: A Modern Approach in Translational Medicine. J Transl Med. 2020;18(1):449.
[30] Adalberto EJ, Argenta DF, Bazzo GC, et al. Development of Curcumin-loaded chitosan/pluronic membranes for wound healing applications. Int J Biol Macromol. 2020;163:167-179.
[31] Walter MNM, Wright KT, Fuller HR, et al. Mesenchymal stem cell-conditioned medium accelerates skin wound healing: an in vitro study of fibroblast and keratinocyte scratch assays. Exp Cell Res. 2010; 316(7):1271-1281.
[32] Rong XL, Chu WH, Zhang HY, et al. Antler stem cell-conditioned medium stimulates regenerative wound healing in rats. Stem Cell Res Ther. 2019;10(1):326.
[33] Huang YZ, Gou M, Da LC, et al. Mesenchymal Stem Cells for Chronic Wound Healing: Current Status of Preclinical and Clinical Studies. Tissue Eng Part B Rev. 2020;26(6):555-570.
[34] PELIZZO G, AVANZINI MA, ICARO CORNAGLIA A, et al. Mesenchymal stromal cells for cutaneous wound healing in a rabbit model: pre-clinical study applicable in the pediatric surgical setting. J Transl Med. 2015;13(1):1-14.
[35] MURPHY KC, WHITEHEAD J, FALAHEE PC, et al. MμLtifactorial experimental design to optimize the anti-inflammatory and proangiogenic potential of mesenchymal stem cell spheroids. Stem Cells. 2017;35(6):1493-1504.
[36] CAPPUZZELLO C, DONI A, DANDER E, et al. Mesenchymal stromal cell-derived PTX3 promotes wound healing via fibrin remodeling. J Invest Dermatol. 2016; 136(1):293-300.
[37] WANG C, WANG M, XU T, et al. Engineering bioactive self-healing antibacterial exosomes hydrogel for promoting chronic diabetic wound healing and complete skin regeneration. Theranostics. 2019;9(1):65.
[38] Zhang W, Bai XZ, Zhao B, et al. Cell-free therapy based on adipose tissue stem cell-derived exosomes promotes wound healing via the PI3K/Akt signaling pathway. Exp Cell Res. 2018;370(2):333-342.
[39] Liu HM, Deng SC, Han L, et al. Mesenchymal stem cells, exosomes and exosome-mimics as smart drug carriers for targeted cancer therapy. Colloids Surf B Biointerfaces. 2021;209(Pt 1):112163.
[40] van der Meel R, Fens MHAM, Vader P, et al. Extracellular vesicles as drug delivery systems: Lessons from the liposome field J Control Release. 2014;195:72-85.
[41] Li F, Shi YJ, Liang J, et al. Curcumin-loaded chitosan nanoparticles promote diabetic wound healing via attenuating inflammation in a diabetic rat model. J Biomater Appl. 2019;34(4):476-486.
[42] Panchatcharam M, Miriyala S, Gayathri VS, et al. Curcumin improves wound healing by modulating collagen and decreasing reactive oxygen species. Mol Cell Biochem. 2006;290(1-2):87-96.
[43] Aggarwal BB, Sung B. Pharmacological basis for the role of curcumin in chronic diseases: an age-old spice with modern targets. Trends Pharmacol Sci. 2009;30(2):85-94.
[44] Lakhal S, Wood MJA. Exosome nanotechnology: An emerging paradigm shift in drug delivery : Exploitation of exosome nanovesicles for systemic in vivo delivery of RNAi heralds new horizons for drug delivery across biological barriers. Bioessays. 2011;33(10):737-741.
|