[1] 赵鹏,冯连世.新的低氧训练模式研究及应用进展[J].体育科学, 2005,25(6):71-75,79.
[2] WANG GL, SEMENZA GL. Purification and characterization of hypoxia-inducible factor 1. J Biol Chem. 1995;270(3):1230-1237.
[3] SEMENZA GL. Regulation of physiological responses to continuous and intermittent hypoxia by hypoxia-inducible factor 1. Exp Physiol. 2006;91(5):803-806.
[4] SCHOFIELD CJ, RATCLIFFE PJ. Oxygen sensing by HIF hydroxylases. Nat Rev Mol Cell Biol. 2004;5(5):343-354.
[5] BERRA E, BENIZRI E, GINOUVÈS A, et al. HIF prolyl-hydroxylase 2 is the key oxygen sensor setting low steady-state levels of HIF-1alpha in normoxia. EMBO J. 2003;22(16):4082-4090.
[6] HAMPTON-SMITH RJ, DAVENPORT BA, NAGARAJAN Y, et al. The conservation and functionality of the oxygen-sensing enzyme Factor Inhibiting HIF (FIH) in non-vertebrates. PLoS One. 2019;14(4):e0216134.
[7] DESPLANCHES D, HOPPELER H, LINOSSIER MT, et al. Effects of training in normoxia and normobaric hypoxia on human muscle ultrastructure. Pflugers Arch. 1993;425(3-4):263-267.
[8] SUNDBERG CJ. Exercise and training during graded leg ischaemia in healthy man with special reference to effects on skeletal muscle. Acta Physiol Scand Suppl. 1994;615:1-50.
[9] GÖRGENS SW, BENNINGHOFF T, ECKARDT K, et al. Hypoxia in Combination With Muscle Contraction Improves Insulin Action and Glucose Metabolism in Human Skeletal Muscle via the HIF-1α Pathway. Diabetes. 2017;66(11):2800-2807.
[10] SEMENZA GL. Oxygen sensing, homeostasis, and disease. N Engl J Med. 2011;365(6):537-547.
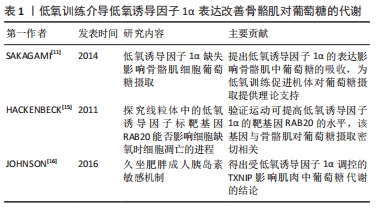
[11] SAKAGAMI H, MAKINO Y, MIZUMOTO K, et al. Loss of HIF-1α impairs GLUT4 translocation and glucose uptake by the skeletal muscle cells. Am J Physiol Endocrinol Metab. 2014;306(9):E1065-1076.
[12] MACKENZIE R, MAXWELL N, CASTLE P, et al. Acute hypoxia and exercise improve insulin sensitivity (S(I) (2*)) in individuals with type 2 diabetes. Diabetes Metab Res Rev. 2011;27(1):94-101.
[13] MASON SD, HOWLETT RA, KIM MJ, et al. Loss of skeletal muscle HIF-1alpha results in altered exercise endurance. PLoS Biol. 2004;2(10): e288.
[14] RICHARDSON RS, WAGNER H, MUDALIAR SR, et al. Exercise adaptation attenuates VEGF gene expression in human skeletal muscle. Am J Physiol Heart Circ Physiol. 2000;279(2):H772-778.
[15] HACKENBECK T, HUBER R, SCHIETKE R, et al. The GTPase RAB20 is a HIF target with mitochondrial localization mediating apoptosis in hypoxia. Biochim Biophys Acta. 2011;1813(1):1-13.
[16] JOHNSON ML, DISTELMAIER K, LANZA IR, et al. Mechanism by Which Caloric Restriction Improves Insulin Sensitivity in Sedentary Obese Adults. Diabetes. 2016;65(1):74-84.
[17] EGAN B, ZIERATH JR. Exercise metabolism and the molecular regulation of skeletal muscle adaptation. Cell Metab. 2013;17(2):162-184.
[18] VOGT M, PUNTSCHART A, GEISER J, et al. Molecular adaptations in human skeletal muscle to endurance training under simulated hypoxic conditions. J Appl Physiol (1985). 2001;91(1):173-182.
[19] BURGOMASTER KA, HUGHES SC, HEIGENHAUSER GJ, et al. Six sessions of sprint interval training increases muscle oxidative potential and cycle endurance capacity in humans. J Appl Physiol (1985). 2005;98(6):1985-1990.
[20] MELISSA L, MACDOUGALL JD, TARNOPOLSKY MA, et al. Skeletal muscle adaptations to training under normobaric hypoxic versus normoxic conditions. Med Sci Sports Exerc. 1997;29(2):238-243.
[21] TERRADOS N, JANSSON E, SYLVÉN C, et al. Is hypoxia a stimulus for synthesis of oxidative enzymes and myoglobin? J Appl Physiol (1985). 1990;68(6):2369-2372.
[22] GREEN HJ, SUTTON JR, CYMERMAN A, et al. Operation Everest II: adaptations in human skeletal muscle. J Appl Physiol (1985). 1989; 66(5):2454-2461.
[23] MACDOUGALL JD, GREEN HJ, SUTTON JR, et al. Operation Everest II: structural adaptations in skeletal muscle in response to extreme simulated altitude. Acta Physiol Scand. 1991;142(3):421-427.
[24] MIZUNO M, SAVARD GK, ARESKOG NH, et al. Skeletal muscle adaptations to prolonged exposure to extreme altitude: a role of physical activity? High Alt Med Biol. 2008;9(4):311-317.
[25] MAXWELL PH, WIESENER MS, CHANG GW, et al. The tumour suppressor protein VHL targets hypoxia-inducible factors for oxygen-dependent proteolysis. Nature. 1999;399(6733):271-275.
[26] TAYLOR CT. Mitochondria and cellular oxygen sensing in the HIF pathway. Biochem J. 2008;409(1):19-26.
[27] MAHONEY DJ, PARISE G, MELOV S, et al. Analysis of global mRNA expression in human skeletal muscle during recovery from endurance exercise. FASEB J. 2005;19(11):1498-1500.
[28] SCHMUTZ S, DÄPP C, WITTWER M, et al. Endurance training modulates the muscular transcriptome response to acute exercise. Pflugers Arch. 2006;451(5):678-687.
[29] AMARAL SL, LINDERMAN JR, MORSE MM, et al. Angiogenesis induced by electrical stimulation is mediated by angiotensin II and VEGF. Microcirculation. 2001;8(1):57-67.
[30] BREEN EC, JOHNSON EC, WAGNER H, et al. Angiogenic growth factor mRNA responses in muscle to a single bout of exercise. J Appl Physiol (1985). 1996;81(1):355-361.
[31] GUSTAFSSON T, PUNTSCHART A, KAIJSER L, et al. Exercise-induced expression of angiogenesis-related transcription and growth factors in human skeletal muscle. Am J Physiol. 1999;276(2):H679-685.
[32] LLOYD PG, PRIOR BM, YANG HT, et al. Angiogenic growth factor expression in rat skeletal muscle in response to exercise training. Am J Physiol Heart Circ Physiol. 2003;284(5):H1668-1678.
[33] FORSYTHE JA, JIANG BH, IYER NV, et al. Activation of vascular endothelial growth factor gene transcription by hypoxia-inducible factor 1. Mol Cell Biol. 1996;16(9):4604-4613.
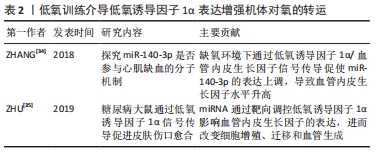
[34] ZHANG L, LUO X, CHEN F, et al. LncRNA SNHG1 regulates cerebrovascular pathologies as a competing endogenous RNA through HIF-1α/VEGF signaling in ischemic stroke. J Cell Biochem. 2018;119(7): 5460-5472.
[35] ZHU Y, WANG Y, JIA Y, et al. Roxadustat promotes angiogenesis through HIF-1α/VEGF/VEGFR2 signaling and accelerates cutaneous wound healing in diabetic rats. Wound Repair Regen. 2019;27(4):324-334.
[36] HOFER T, WENGER H, GASSMANN M. Oxygen sensing, HIF-1alpha stabilization and potential therapeutic strategies. Pflugers Arch. 2002; 443(4):503-507.
[37] THOMAS LW, ASHCROFT M. Exploring the molecular interface between hypoxia-inducible factor signalling and mitochondria. Cell Mol Life Sci. 2019;76(9):1759-1777.
[38] SEMENZA GL, JIANG BH, LEUNG SW, et al. Hypoxia response elements in the aldolase A, enolase 1, and lactate dehydrogenase A gene promoters contain essential binding sites for hypoxia-inducible factor 1. J Biol Chem. 1996;271(51):32529-32537.
[39] WENGER RH. Cellular adaptation to hypoxia: O2-sensing protein hydroxylases, hypoxia-inducible transcription factors, and O2-regulated gene expression. FASEB J. 2002;16(10):1151-1162.
[40] ZIMNA A, KURPISZ M. Hypoxia-Inducible Factor-1 in Physiological and Pathophysiological Angiogenesis: Applications and Therapies. Biomed Res Int. 2015;2015:549412.
[41] KIERANS SJ, TAYLOR CT. Regulation of glycolysis by the hypoxia-inducible factor (HIF): implications for cellular physiology. J Physiol. 2021;599(1):23-37.
[42] CARROLL VA, ASHCROFT M. Role of hypoxia-inducible factor (HIF)-1alpha versus HIF-2alpha in the regulation of HIF target genes in response to hypoxia, insulin-like growth factor-I, or loss of von Hippel-Lindau function: implications for targeting the HIF pathway. Cancer Res. 2006;66(12):6264-6270.
[43] GREIJER AE, VAN DER GROEP P, KEMMING D, et al. Up-regulation of gene expression by hypoxia is mediated predominantly by hypoxia-inducible factor 1 (HIF-1). J Pathol. 2005;206(3):291-304.
[44] CERADINI DJ, KULKARNI AR, CALLAGHAN MJ, et al. Progenitor cell trafficking is regulated by hypoxic gradients through HIF-1 induction of SDF-1. Nat Med. 2004;10(8):858-864.
[45] MANALO DJ, ROWAN A, LAVOIE T, et al. Transcriptional regulation of vascular endothelial cell responses to hypoxia by HIF-1. Blood. 2005; 105(2):659-669.
[46] KELLY BD, HACKETT SF, HIROTA K, et al. Cell type-specific regulation of angiogenic growth factor gene expression and induction of angiogenesis in nonischemic tissue by a constitutively active form of hypoxia-inducible factor 1. Circ Res. 2003;93(11):1074-1081.
[47] LEE P, CHANDEL NS, SIMON MC. Cellular adaptation to hypoxia through hypoxia inducible factors and beyond. Nat Rev Mol Cell Biol. 2020; 21(5):268-283.
[48] CHEN L, ENDLER A, SHIBASAKI F. Hypoxia and angiogenesis: regulation of hypoxia-inducible factors via novel binding factors. Exp Mol Med. 2009;41(12):849-857.
[49] AMELN H, GUSTAFSSON T, SUNDBERG CJ, et al. Physiological activation of hypoxia inducible factor-1 in human skeletal muscle. FASEB J. 2005; 19(8):1009-1011.
[50] NAGAHISA H, MUKAI K, OHMURA H, et al. Effect of High-Intensity Training in Normobaric Hypoxia on Thoroughbred Skeletal Muscle. Oxid Med Cell Longev. 2016;2016:1535367.
|