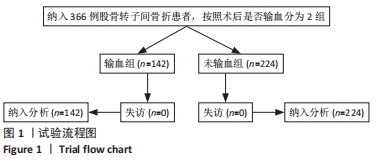
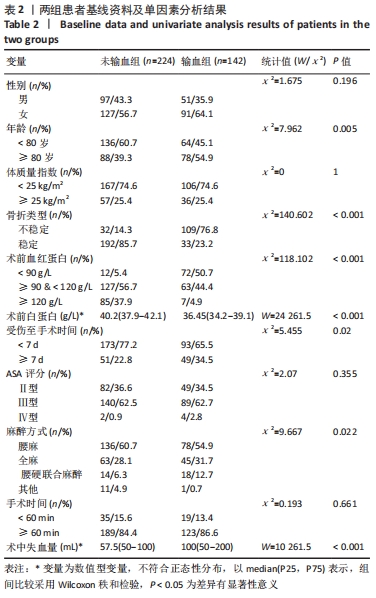
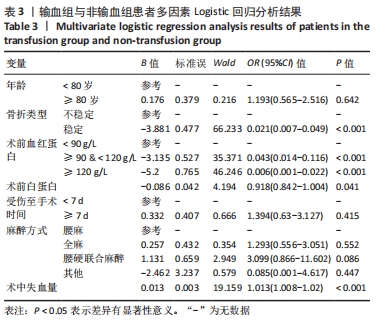
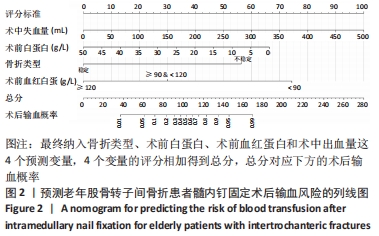
[1] DAI CQ, WANG LH, ZHU YQ, et al. Risk factors of perioperative blood transfusion in elderly patients with femoral intertrochanteric fracture. Medicine (Baltimore). 2020;99(15):e19726.
[2] KANNUS P, LEIPONEN P, PARKKARI J, et al. A sideways fall and hip fracture. Bone. 2006;39(2):383-384.
[3] 孙海波,张英泽,彭阿钦,等.PFNA治疗老年股骨转子间骨折围手术期隐性失血量分析[J].中国骨与关节外科,2014,7(6):494-497.
[4] LUO X, HE S, LI Z, et al. Quantification and influencing factors of perioperative hidden blood loss during intramedullary fixation for intertrochanteric fractures in the elderly. Arch Orthop Trauma Surg. 2020;140(10):1339-1348.
[5] 李志强,宫济武.溶血性输血反应与细菌性输血反应处置流程[J].中国输血杂志,2012,25(9):824-825.
[6] HOU G, ZHOU F, TIAN Y, et al. Predicting the need for blood transfusions in elderly patients with pertrochanteric femoral fractures. Injury. 2014;45(12): 1932-1937.
[7] SMITH GH, TSANG J, MOLYNEUX SG, et al. The hidden blood loss after hip fracture. Injury. 2011;42(2):133-135.
[8] BERGSTRÖM U, JONSSON H, GUSTAFSON Y, et al. The hip fracture incidence curve is shifting to the right. Acta Orthop. 2009;80(5):520-524.
[9] 梁昌详,郑晓青,昌耘冰,等.精确定位防旋髓内钉置入治疗股骨转子间骨折[J].研究,2014,18(17):2685-2690.
[10] YU W, ZHANG X, WU R, et al. The visible and hidden blood loss of Asia proximal femoral nail anti-rotation and dynamic hip screw in the treatment of intertrochanteric fractures of elderly high- risk patients: a retrospective comparative study with a minimum 3 years of follow-up. BMC Musculoskelet Disord. 2016;17:269.
[11] TANG P, HU F, SHEN J, et al. Proximal femoral nail antirotation versus hemiarthroplasty: a study for the treatment of intertrochanteric fractures. Injury. 2012;43(6):876-881.
[12] ESPINOSA KA, GÉLVEZ AG, TORRES LP, et al. Pre-operative factors associated with increased mortality in elderly patients with a hip fracture: A cohort study in a developing country. Injury. 2018;49(6):1162-1168.
[13] VOCHTELOO AJ, BORGER VAN DER BURG BL, MERTENS B, et al. Outcome in hip fracture patients related to anemia at admission and allogeneic blood transfusion: an analysis of 1262 surgically treated patients. BMC Musculoskelet Disord. 2011;12:262.
[14] WANG JQ, CHEN LY, JIANG BJ, et al. Development of a Nomogram for Predicting Blood Transfusion Risk After Hemiarthroplasty for Femoral Neck Fractures in Elderly Patients. Med Sci Monit. 2020;26:e920255.
[15] ALDEBEYAN S, NOOH A, AOUDE A, et al. Hypoalbuminaemia-a marker of malnutrition and predictor of postoperative complications and mortality after hip fractures. Injury. 2017;48(2):436-440.
[16] HUANG R, GREENKY M, KERR GJ, et al. The effect of malnutrition on patients undergoing elective joint arthroplasty. J Arthroplasty. 2013;28(8 Suppl):21-24.
[17] NELSON CL, ELKASSABANY NM, KAMATH AF,et al. Low Albumin Levels, More Than Morbid Obesity, Are Associated With Complications After TKA. Clin Orthop Relat Res. 2015;473(10):3163-3172.
[18] LIM S, KIM BD, KIM JY, et al. Preoperative Albumin Alone is Not a Predictor of 30-Day Outcomes in Pressure Ulcer Patients: A Matched Propensity-Score Analysis of the 2006-2011 NSQIP Datasets. Ann Plast Surg. 2015;75(4):439-447.
[19] ADUNSKY A, LICHTENSTEIN A, MIZRAHI E, et al. Blood transfusion requirements in elderly hip fracture patients. Arch Gerontol Geriatr. 2003;36(1):75-81.
[20] KUMAR D, MBAKO AN, RIDDICK A, et al. On admission haemoglobin in patients with hip fracture. Injury. 2011;42(2):167-170.
[21] SUH YS, NHO JH, SEO J, et al. Hip Fracture Surgery without Transfusion in Patients with Hemoglobin Less Than 10 g/dL. Clin Orthop Surg. 2021;13(1): 30-36.
[22] 张立超,苏鹏,云才.老年股骨转子间骨折围术期输血的相关因素[J].中国矫形外科杂志,2021,29(6):499-502.
[23] SEHAT KR, EVANS RL, NEWMAN JH. Hidden blood loss following hip and knee arthroplasty. Correct management of blood loss should take hidden loss into account. J Bone Joint Surg Br. 2004;86(4):561-565.
[24] FOSS NB, KEHLET H. Hidden blood loss after surgery for hip fracture. J Bone Joint Surg Br. 2006;88(8):1053-1059.
[25] RYAN DJ, YOSHIHARA H, YONEOKA D, et al. Delay in Hip Fracture Surgery: An Analysis of Patient-Specific and Hospital-Specific Risk Factors. J Orthop Trauma. 2015;29(8):343-348.
[26] LAWLESS AM, NARULA S, D’ALESSANDRO P, et al. Time to surgery and transfer-associated mortality for hip fractures in Western Australia. ANZ J Surg. 2020;90(9):1750-1753.
[27] KRISTAN A, OMAHEN S, CIMERMAN M. Causes for Delay to Surgery in Hip Fractures and How It Impacts on Mortality: a Single Level 1 Trauma Center Experience. Acta Chir Orthop Traumatol Cech. 2021;88(1):28-34.
[28] VERBEEK DO, PONSEN KJ, GOSLINGS JC, et al. Effect of surgical delay on outcome in hip fracture patients: a retrospective multivariate analysis of 192 patients. Int Orthop. 2008;32(1):13-18.
[29] OROSZ GM, MAGAZINER J, HANNAN EL, et al. Association of timing of surgery for hip fracture and patient outcomes. JAMA. 2004;291(14):1738-1743.
[30] 张华,陶立元,赵一鸣.开展病历回顾性研究的注意事项[J].中华儿科杂志,2018,56(1):47.
|