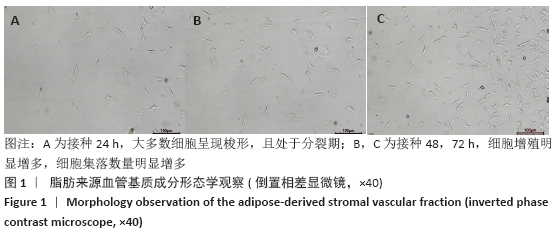
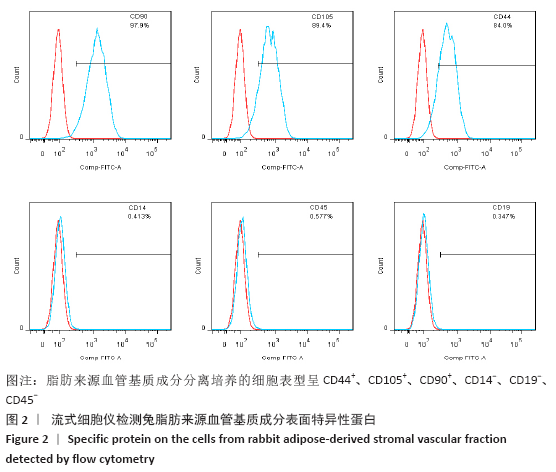
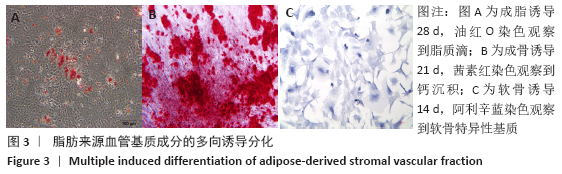
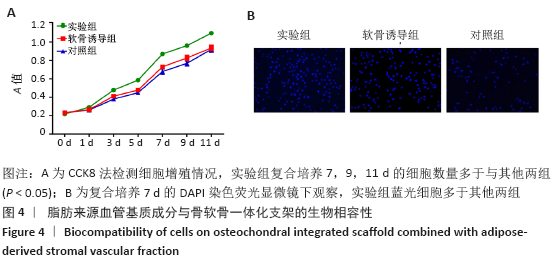
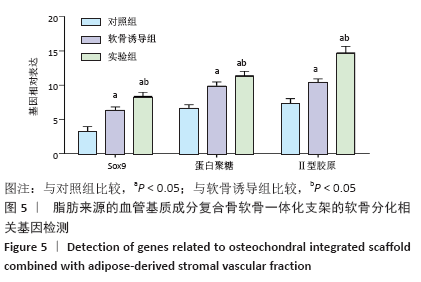
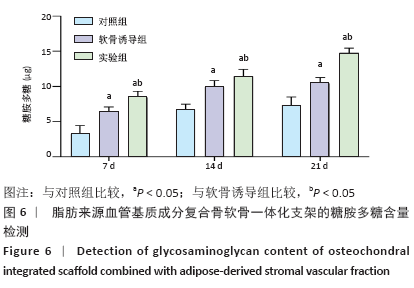
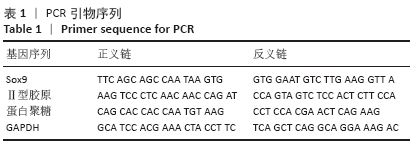
[1] HUEY DJ, HU JC, ATHANASIOU KA. Unlike bone, cartilage regeneration remains elusive. Science. 2012;338(6109):917-927.
[2] GUGJOO MB, SHARMA GT, AITHAL HP, et al. Cartilage tissue engineering: Role of mesenchymal stem cells along with growth factors & scaffolds. Indian J Med Res. 2016;144(3):339-347.
[3] ALBRIGHT JC, DAOUD AK. Microfracture and Microfracture Plus. Clin Sports Med. 2017;36(3):501-507.
[4] KRAEUTLER MJ, HOUCK DA, MCQUEEN MB, et al. A Cost-Effectiveness Analysis of Surgical Treatment Modalities for Chondral Lesions of the Knee: Microfracture, Osteochondral Autograft Transplantation, and Autologous Chondrocyte Implantation. Orthop J Sports Med. 2017; 5(5):1-8.
[5] GOMOLL AH, MADRY H, KNUTSEN G, et al. The subchondral bone in articular cartilage repair: current problems in the surgical management. Knee Surg Sports Traumatol Arthrosc. 2010;18(4):434-447.
[6] ASIK M, CIFTCI F, SEN C, et al. The microfracture technique for the treatment of full-thickness articular cartilage lesions of the knee: midterm results. Arthroscopy. 2008;24(11):1214-1220.
[7] ARMIENTO AR, STODDART MJ, ALINI M, et al. Biomaterials for articular cartilage tissue engineering: Learning from biology. Acta Biomater. 2018;65:1-20.
[8] PATEL JM, WISE BC, BONNEVIE ED, et al. A Systematic Review and Guide to Mechanical Testing for Articular Cartilage Tissue Engineering. Tissue Eng Part C Methods. 2019;25(10):593-608.
[9] WALTER SG, OSSENDORFF R, SCHILDBERG FA, et al. Articular cartilage regeneration and tissue engineering models: a systematic review. Arch Orthop Trauma Surg. 2019;139(3):305-316.
[10] KWON H, BROWN WE, LEE CA, et al. Surgical and tissue engineering strategies for articular cartilage and meniscus repair. Nat Rev Rheumatol. 2019;15(9):550-570.
[11] MEHRANFAR S, ABDI RAD I, MOSTAFAV E, et al. The use of stromal vascular fraction (SVF), platelet-rich plasma (PRP) and stem cells in the treatment of osteoarthritis: an overview of clinical trials. Artif Cells Nanomed Biotechnol. 2019;47(1):882-890.
[12] BANSAL H, COMELLA K, LEON J, et al. Intra-articular injection in the knee of adipose derived stromal cells (stromal vascular fraction) and platelet rich plasma for osteoarthritis. J Transl Med. 2017; 15(1):141.
[13] 郑蕊,杰永生,陈磊,等.脱细胞真皮基质/生物矿化胶原一体化骨软骨支架的制备及其生物相容性的研究[J].中国医药生物技术, 2019,14(2):121-126.
[14] 舒雄,杰永生,郑蕊,等.激活的富血小板血浆促进Pellet 培养的脂肪间充质干细胞成软骨样分化[J].中国医药生物技术,2018, 13(4):328-333.
[15] ZHOU W, LIN J, ZHAO K, et al. Single-Cell Profiles and Clinically Useful Properties of Human Mesenchymal Stem Cells of Adipose and Bone Marrow Origin. Am J Sports Med. 2019;47(7):1722-1733.
[16] ZHAO Z, FAN C, CHEN F, et al. Progress in Articular Cartilage Tissue Engineering: A Review on Therapeutic Cells and Macromolecular Scaffolds. Macromol Biosci. 2020;20(2):e1900278.
[17] BAKHSHAYESH A, BABAIE S, NASRABADI HT, et al. An overview of various treatment strategies, especially tissue engineering for damaged articular cartilage. Artif Cells Nanomed Biotechnol. 2020;48(1):1089-1104.
[18] CIPOLLARO L, CIARDULLI MC, PORTA GD, et al. Biomechanical issues of tissue-engineered constructs for articular cartilage regeneration: in vitro and in vivo approaches. Br Med Bull. 2019;132(1):53-80.
[19] LEMOINE M, CASEY SM, O’BYRNE JM, et al. The development of natural polymer scaffold-based therapeutics for osteochondral repair. Biochem Soc Trans. 2020;48(4):1433-1445.
[20] Dan X, Wei L, Li JJ, et al. Engineering 3D functional tissue constructs using self-assembling cell-laden microniches. Acta Biomater. 2020; 114:170-182.
[21] BAPTISTA LS. Adipose stromal/stem cells in regenerative medicine: Potentials and limitations. World J Stem Cells. 2020;12(1):1-7.
[22] WEN YT, DAI NT, HSU SH. Biodegradable water-based polyurethane scaffolds with a sequential release function for cell-free cartilage tissue engineering. Acta Biomater. 2019;88:301-313.
[23] CARVALHO MS, SILVA JC, UDANGAWA RN, et al. Co-culture cell-derived extracellular matrix loaded electrospun microfibrous scaffolds for bone tissue engineering. Mater Sci Eng C Mater Biol Appl. 2019;99:479-490.
[24] TAKAHASHI H, OKANO T. Thermally-triggered fabrication of cell sheets for tissue engineering and regenerative medicine. Adv Drug Deliv Rev. 2019;138:276-292.
[25] NEO PY, TEH TK, TAY AS, et al. Stem cell-derived cell-sheets for connective tissue engineering. Connect Tissue Res. 2016;57(6): 428-442.
[26] CHOI JS, CHAE DS, RYU HA, et al. Transplantation of human adipose tissue derived-SVF enhance liver function through high anti-inflammatory property. Biochim Biophys Acta Mol Cell Biol Lipids. 2019;1864(12):158526.
[27] KILINC MO, SANTIDRIAN A, MINEV I, et al. The ratio of ADSCs to HSC-progenitors in adipose tissue derived SVF may provide the key to predict the outcome of stem-cell therapy. Clin Transl Med. 2018;7(1):5.
[28] SOLODEEV I, ORGIL M, COHEN M, et al. Cryopreservation of Stromal Vascular Fraction Cells Reduces Their Counts but Not Their Stem Cell Potency. Plast Reconstr Surg Glob Open. 201;7(7):e2321.
[29] MORANDI EM, PLONER C, WOLFRAM D, et al. Risk factors and complications after body-contouring surgery and the amount of stromal vascular fraction cells found in subcutaneous tissue. Int Wound J. 2019;16(6):1545-1552.
[30] ZANATA F, BOWLES A, FRAZIER T, et al. Effect of Cryopreservation on Human Adipose Tissue and Isolated Stromal Vascular Fraction Cells: In Vitro and In Vivo Analyses. Plast Reconstr Surg. 2018;141(2): 232e-243e.
[31] MEHRANFAR S, RAD IA, MOSTAFAV E, et al. The use of stromal vascular fraction (SVF), platelet-rich plasma (PRP) and stem cells in the treatment of osteoarthritis: an overview of clinical trials. Artif Cells Nanomed Biotechnol. 2019;47(1):882-890.
[32] YOKOTA N, HATTORI M, OHTSURU T, et al. Comparative Clinical Outcomes After Intra-articular Injection With Adipose-Derived Cultured Stem Cells or Noncultured Stromal Vascular Fraction for the Treatment of Knee Osteoarthritis. Am J Sports Med. 2019;47(11):2577-2583.
[33] FRANKLIN SP, STOKER AM, BOZYNSKI CC, et al. Comparison of Platelet-Rich Plasma, Stromal Vascular Fraction (SVF), or SVF with an Injectable PLGA Nanofiber Scaffold for the Treatment of Osteochondral Injury in Dogs. J Knee Surg. 2018;31(7):686-697.
[34] DONGEN JA, HARMSEN MC, STEVENS HP, et al. Isolation of Stromal Vascular Fraction by Fractionation of Adipose Tissue. Methods Mol Biol. 2019;1993:91-103.
[35] YAO Y, DONG Z, LIAO Y, et al. Adipose Extracellular Matrix/Stromal Vascular Fraction Gel: A Novel Adipose Tissue-Derived Injectable for Stem Cell Therapy. Plast Reconstr Surg. 2017;139(4):867-879.
[36] SCHNEIDER MC, CHU S, RANDOLPH MA, et al. An in vitro and in vivo comparison of cartilage growth in chondrocyte-laden matrix metalloproteinase-sensitive poly(ethylene glycol) hydrogels with localized transforming growth factor β3. Acta Biomater. 2019;93: 97-110.
[37] JIA ZF, WANG SJ, LIANG YJ, et al. Combination of kartogenin and transforming growth factor-β3 supports synovial fluid-derived mesenchymal stem cell-based cartilage regeneration. Am J Transl Res. 2019;11(4):2056-2069.
[38] QU D, ZHU JP, CHILDS HR, et al. Nanofiber-based transforming growth factor-β3 release induces fibrochondrogenic differentiation of stem cells. Acta Biomater. 2019;93:111-122.
[39] CHEN YR, ZHOU ZX, ZHANG JY, et al. Low-Molecular-Weight Heparin-Functionalized Chitosan-Chondroitin Sulfate Hydrogels for Controlled Release of TGF-β3 and in vitro Neocartilage Formation. Front Chem. 2019;7:745.
[40] NAKAGAWA Y, FORTIER LA, MAO JJ, et al. Long-term Evaluation of Meniscal Tissue Formation in 3-dimensional-Printed Scaffolds With Sequential Release of Connective Tissue Growth Factor and TGF-β3 in an Ovine Model. Am J Sports Med. 2019;47(11):2596-2607.
|