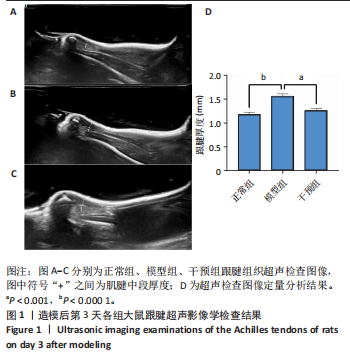
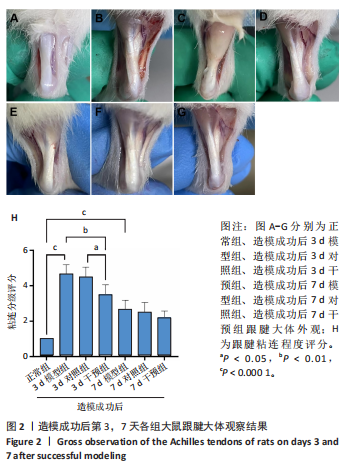
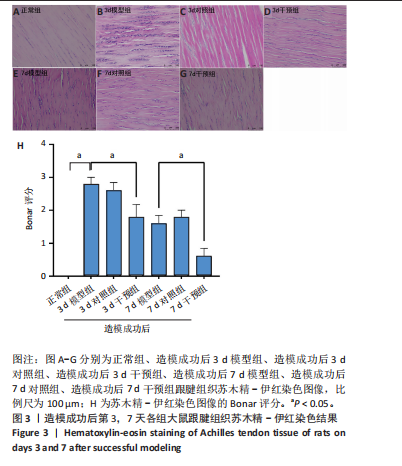
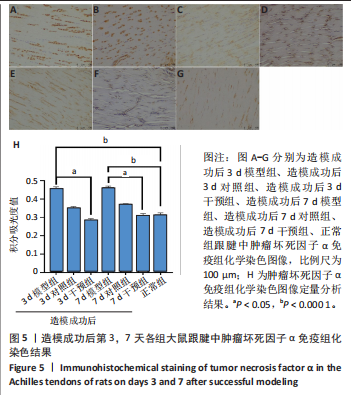
[1] LYU K, LIU X, LIU T, et al. miRNAs contributing to the repair of tendon injury. Cell Tissue Res. 2023;393(2):201-215.
[2] JIANG L, LU J, CHEN Y, et al. Mesenchymal stem cells: An efficient cell therapy for tendon repair (Review). Int J Mol Med. 2023;52(2):70.
[3] ZHANG L, ZHANG Q, CUI L, et al. Kartogenin Combined Platelet-Rich Plasma (PRP) Promoted Tendon-Bone Healing for Anterior Cruciate Ligament (ACL) Reconstruction by Suppressing Inflammatory Response Via targeting AKT/PI3K/NF-κB. Appl Biochem Biotechnol. 2023;195(2):1284-1296.
[4] KAMEL SI, ROSAS HG, GORBACHOVA T. Local and Systemic Side Effects of Corticosteroid Injections for Musculoskeletal Indications. AJR Am J Roentgenol. 2024;222(3):e2330458.
[5] SHAMROCK AG, DREYER MA, VARACALLO MA. Achilles Tendon Rupture. StatPearls. Treasure Island (FL): StatPearls Publishing, Copyright © 2025, StatPearls Publishing LLC.; 2025.
[6] DAMBUZA IM, HE C, CHOI JK, et al. IL-12p35 induces expansion of IL-10 and IL-35-expressing regulatory B cells and ameliorates autoimmune disease. Nat Commun. 2017;8(1):719.
[7] SHI J, SHI S, XIE W, et al. IL-10 alleviates lipopolysaccharide-induced skin scarring via IL-10R/STAT3 axis regulating TLR4/NF-κB pathway in dermal fibroblasts. J Cell Mol Med. 2021;25(3):1554-1567.
[8] KIERAN I, KNOCK A, BUSH J, et al. Interleukin-10 reduces scar formation in both animal and human cutaneous wounds: results of two preclinical and phase II randomized control studies. Wound Repair Regen. 2013;21(3):428-436.
[9] NAKAGOME K, DOHI M, OKUNISHI K, et al. In vivo IL-10 gene delivery attenuates bleomycin induced pulmonary fibrosis by inhibiting the production and activation of TGF-beta in the lung. Thorax. 2006;61(10):886-894.
[10] SHORT WD, STEEN E, KAUL A, et al. IL-10 promotes endothelial progenitor cell infiltration and wound healing via STAT3. FASEB J. 2022;36(7):e22298.
[11] FEARON A, DAHLSTROM JE, TWIN J, et al. The Bonar score revisited: region of evaluation significantly influences the standardized assessment of tendon degeneration. J Sci Med Sport. 2014;17(4):346-350.
[12] STEINMANN S, PFEIFER CG, BROCHHAUSEN C, et al. Spectrum of Tendon Pathologies: Triggers, Trails and End-State. Int J Mol Sci. 2020;21(3):844.
[13] ATTIA AK, MAHMOUD K, D’HOOGHE P, et al. Outcomes and Complications of Open Versus Minimally Invasive Repair of Acute Achilles Tendon Ruptures: A Systematic Review and Meta-analysis of Randomized Controlled Trials. Am J Sports Med. 2023;51(3):825-836.
[14] ZHANG J, BROWN R, HOGAN MV, et al. Mitigating Scar Tissue Formation in Tendon Injuries: Targeting HMGB1, AMPK Activation, and Myofibroblast Migration All at Once. Pharmaceuticals (Basel). 2023;16(12):1739.
[15] TRAWEGER A, SCOTT A, KJAER M, et al. Achilles tendinopathy. Nat Rev Dis Primers. 2025;11(1):20.
[16] DARRIEUTORT-LAFFITE C, BLANCHARD F, SOSLOWSKY LJ, et al. Biology and physiology of tendon healing. Joint Bone Spine. 2024;91(5):105696.
[17] JIANG F, ZHAO H, ZHANG P, et al. Challenges in tendon-bone healing: emphasizing inflammatory modulation mechanisms and treatment. Front Endocrinol (Lausanne). 2024;15:1485876.
[18] DAKIN SG, DUDHIA J, SMITH RK. Resolving an inflammatory concept: the importance of inflammation and resolution in tendinopathy. Vet Immunol Immunopathol. 2014;158(3-4):121-127.
[19] CHEN R, AI L, ZHANG J, et al. Dendritic Cell-Derived Exosomes Promote Tendon Healing and Regulate Macrophage Polarization in Preventing Tendinopathy. Int J Nanomedicine. 2024;19:11701-11718.
[20] THOMOPOULOS S, HATTERSLEY G, ROSEN V, et al. The localized expression of extracellular matrix components in healing tendon insertion sites: an in situ hybridization study. J Orthop Res. 2002;20(3):454-463.
[21] NAJAFI Z, RAHMANIAN-DEVIN P, BARADARAN RAHIMI V, et al. Challenges and opportunities of medicines for treating tendon inflammation and fibrosis: A comprehensive and mechanistic review. Fundam Clin Pharmacol. 2024;38(5): 802-841.
[22] CHEN J, SHENG R, MO Q, et al. Controlled TPCA-1 delivery engineers a pro-tenogenic niche to initiate tendon regeneration by targeting IKKβ/NF-κB signaling. Bioact Mater. 2025;44:319-338.
[23] LANE RA, MIGOTSKY N, HAVLIOGLU N, et al. The effects of NF-κB suppression on the early healing response following intrasynovial tendon repair in a canine model. J Orthop Res. 2023;41(10):2295-2304.
[24] LI H, LI Y, LUO S, et al. The roles and mechanisms of the NF-κB signaling pathway in tendon disorders. Front Vet Sci. 2024;11:1382239.
[25] ZHANG P, HU J, LIU X, et al. Antiadhesion Biomaterials in Tendon Repair: Application Status and Future Prospect. Tissue Eng Part B Rev. 2025;31(1):20-30.
[26] SHARMA P , MAFFULLI N. Biology of tendon injury: healing, modeling and remodeling. J Musculoskelet Neuronal Interact. 2006;6(2):181-190.
[27] HAST MW, ZUSKOV A, SOSLOWSKY LJ. The role of animal models in tendon research. Bone Joint Res. 2014;3(6):193-202.
[28] LAKE SP, ANSORGE HL, SOSLOWSKY LJ. Animal models of tendinopathy. Disabil Rehabil. 2008;30(20-22):1530-1541.
[29] VIDAL L, LOPEZ-GARZON M, VENEGAS V, et al. A Novel Tendon Injury Model, Induced by Collagenase Administration Combined with a Thermo-Responsive Hydrogel in Rats, Reproduces the Pathogenesis of Human Degenerative Tendinopathy. Int J Mol Sci. 2024;25(3):1868.
[30] DUNICAN AL, LEUENROTH SJ, GRUTKOSKI P, et al. TNFalpha-induced suppression of PMN apoptosis is mediated through interleukin-8 production. Shock. 2000;14(3):284-288; discussion 288-289.
[31] GARBACKI N, TITS M, ANGENOT L, et al. Inhibitory effects of proanthocyanidins from Ribes nigrum leaves on carrageenin acute inflammatory reactions induced in rats. BMC Pharmacol. 2004;4:25.
[32] JIANG L, LIU T, LYU K, et al. Inflammation-related signaling pathways in tendinopathy. Open Life Sci. 2023;18(1):20220729.
[33] DE SOUZA S, ROSARIO CLAUDIO J, SIM J, et al. Interleukin-10 signaling in somatosensory neurons controls CCL2 release and inflammatory response. Brain Behav Immun. 2024;116:193-202.
[34] WANG S, YAO Z, CHEN L, et al. Preclinical assessment of IL-1β primed human umbilical cord mesenchymal stem cells for tendon functional repair through TGF-β/IL-10 signaling. Heliyon. 2023;9(11):e21411.
|