Chinese Journal of Tissue Engineering Research ›› 2024, Vol. 28 ›› Issue (4): 651-656.doi: 10.12307/2024.240
Rehabilitative efficacy of kinesio taping following anterior cruciate ligament reconstruction: a Meta-analysis
Wang Juan1, Wang Ling1, Zuo Huiwu1, Zheng Cheng2, Wang Guanglan1, Chen Peng1
- 1School of Sports Medicine, Wuhan Sports University, Wuhan 430079, Hubei Province, China; 2Department of Sports Medicine, Affiliated Hospital of Wuhan Sports University, Wuhan 430079, Hubei Province, China
-
Received:2023-02-16Accepted:2023-03-18Online:2024-02-08Published:2023-07-14 -
Contact:Wang Guanglan, Master, Professor, School of Sports Medicine, Wuhan Sports University, Wuhan 430079, Hubei Province, China Chen Peng, School of Sports Medicine, Wuhan Sports University, Wuhan 430079, Hubei Province, China -
About author:Wang Juan, Master, School of Sports Medicine, Wuhan Sports University, Wuhan 430079, Hubei Province, China Wang Ling, Master candidate, School of Sports Medicine, Wuhan Sports University, Wuhan 430079, Hubei Province, China -
Supported by:Teaching and Research Project of Hubei Province Department of Education, No. 2021407 (to WJ); Donghu Scholar Program of Wuhan Sports University and Research Fund for Young Teachers of Wuhan Sports University, No. 20Z01 (to ZC)
CLC Number:
Cite this article
Wang Juan, Wang Ling, Zuo Huiwu, Zheng Cheng, Wang Guanglan, Chen Peng. Rehabilitative efficacy of kinesio taping following anterior cruciate ligament reconstruction: a Meta-analysis[J]. Chinese Journal of Tissue Engineering Research, 2024, 28(4): 651-656.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
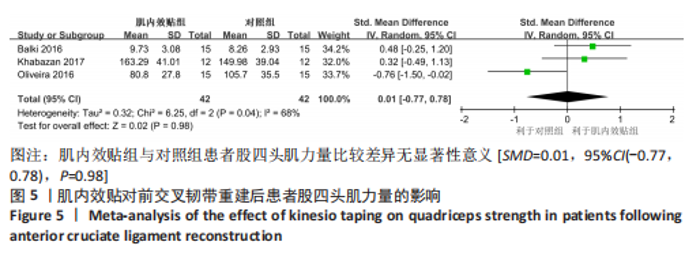
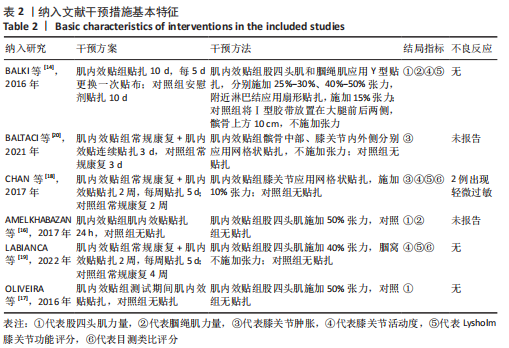
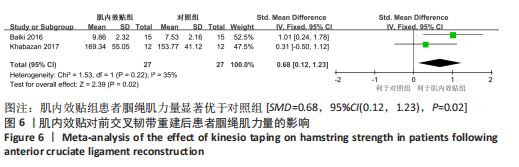
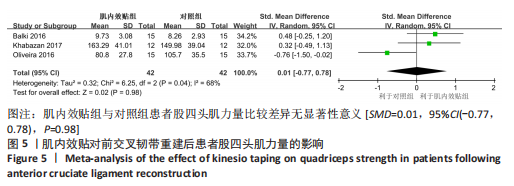
2.4 Meta分析结果 2.4.1 股四头肌力量 有3篇文献报告了股四头肌力量的结果[14,16-17],各文献之间异质性较大(I2=68%, P=0.04),采用随机效应模型进行分析,由于文献间测量方式不同,故采用SMD进行合并。Meta分析结果显示,与对照组相比,肌内效贴并不能显著提升前交叉韧带重建后患者股四头肌力量[SMD=0.01,95%CI(-0.77,0.78),P=0.98],详见图5。敏感性分析显示1项研究具有高度敏感性[17],将其剔除后对剩余文献进行Meta分析,研究间异质性减小(I2=0%,P=0.78),且合并结果稳定[SMD=0.41,95%CI(-0.13,0.95),P=0.14]。"
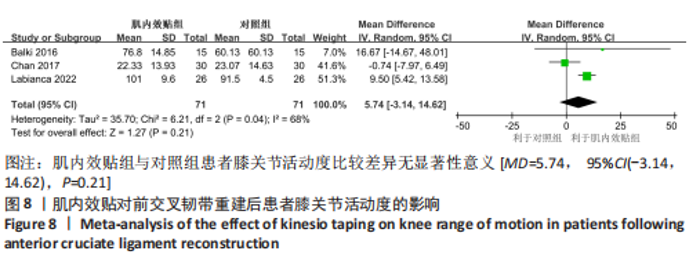
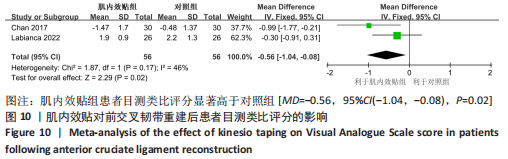
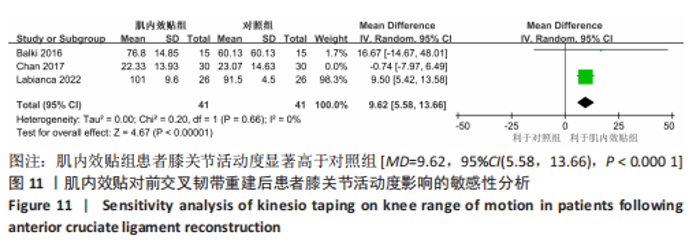
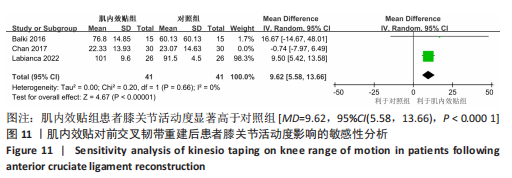
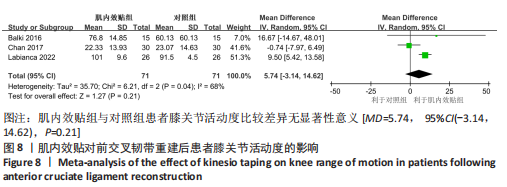
2.4.4 膝关节活动度 有3篇文献报告了膝关节活动度的结果[14,18-19],各文献之间异质性较大(I2=68%, P=0.04),采用随机效应模型进行分析,由于文献间测量方式相同,故采用MD进行合并。Meta分析结果显示,与对照组相比,肌内效贴并不能显著改善前交叉韧带重建术患者膝关节活动度[MD=5.74, 95%CI(-3.14,14.62),P=0.21],详见图8。敏感性分析显示1 项研究具有高度敏感性[18],将其剔除后对剩余文献进行Meta分析,研究间异质性减小(I2=0%,P=0.66),合并结果提示肌内效贴有利于提高患者膝关节活动度[MD=9.62,95%CI(5.58,13.66),P < 0.000 01]。"
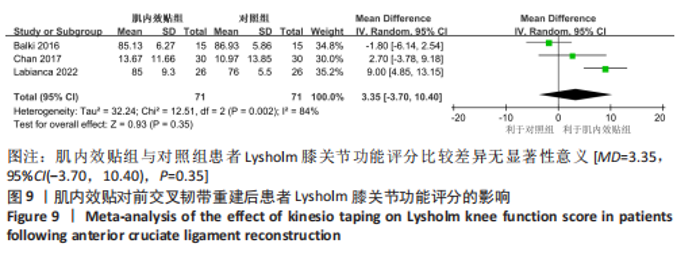
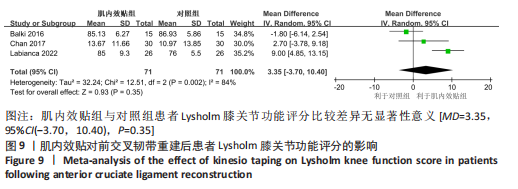
2.4.5 Lysholm膝关节功能评分 有3篇文献报告了Lysholm膝关节功能评分的结果[14,18-19],各文献之间异质性较大(I2=84%,P=0.002),采用随机效应模型进行分析,由于文献间测量方式相同,故采用MD进行合并。Meta分析结果显示,与对照组相比,肌内效贴并不能显著改善前交叉韧带重建后患者膝关节活动度[MD=3.35,95%CI(-3.70,10.40),P=0.35],详见图9。敏感性分析显示1 项研究具有高度敏感性[19],将其剔除后对剩余文献进行Meta分析,研究间异质性减小(I2=22%,P=0.26),且合并结果稳定[MD=-0.22, 95%CI(-4.43,3.99),P=0.31]。"
| [1] RIVERA-BROWN AM, FRONTERA WR, FONTáNEZ R, et al. Evidence for isokinetic and functional testing in return to sport decisions following ACL surgery. PM R. 2022;14(5):678-690. [2] LV ZT, ZHANG JM, PANG ZY, et al. The efficacy of platelet rich plasma on anterior cruciate ligament reconstruction: a systematic review and meta-analysis. Platelets. 2022;33(2):229-241. [3] PASCHOS NK, HOWELL SM. Anterior cruciate ligament reconstruction: principles of treatment. EFORT Open Rev. 2016;1(11):398-408. [4] KIAPOUR AM, MURRAY MM. Basic science of anterior cruciate ligament injury and repair. Bone Joint Res. 2014;3(2):20-31. [5] ARDERN CL, TAYLOR NF, FELLER JA, et al. Fifty-five per cent return to competitive sport following anterior cruciate ligament reconstruction surgery: an updated systematic review and meta-analysis including aspects of physical functioning and contextual factors. Br J Sports Med. 2014; 48(21):1543-1552. [6] WIGGINS AJ, GRANDHI RK, SCHNEIDER DK, et al. Risk of Secondary Injury in Younger Athletes After Anterior Cruciate Ligament Reconstruction: A Systematic Review and Meta-analysis. Am J Sports Med. 2016;44(7):1861-1876. [7] SMEETS A, WILLEMS M, GILSON L, et al. Neuromuscular and biomechanical landing alterations persist in athletes returning to sport after anterior cruciate ligament reconstruction. Knee. 2021;33(11):305-317. [8] NAGELLI CV, WORDEMAN SC, DI STASI S, et al. Neuromuscular Training Improves Biomechanical Deficits at the Knee in Anterior Cruciate Ligament-Reconstructed Athletes. Clin J Sport Med. 2021; 31(2):113-119. [9] TOTH MJ, TOURVILLE TW, VOIGT TB, et al. Utility of Neuromuscular Electrical Stimulation to Preserve Quadriceps Muscle Fiber Size and Contractility After Anterior Cruciate Ligament Injuries and Reconstruction: A Randomized, Sham-Controlled, Blinded Trial. Am J Sports Med. 2020;48(10): 2429-2437. [10] FU CL, YUNG SH, LAW KY, et al. The effect of early whole-body vibration therapy on neuromuscular control after anterior cruciate ligament reconstruction: a randomized controlled trial. Am J Sports Med. 2013;41(4):804-814. [11] WENGLE L, MIGLIORINI F, LEROUX T, et al. The Effects of Blood Flow Restriction in Patients Undergoing Knee Surgery: A Systematic Review and Meta-analysis. Am J Sports Med. 2022;50(10): 2824-2833. [12] YAM ML, YANG Z, ZEE BC, et al. Effects of Kinesio tape on lower limb muscle strength, hop test, and vertical jump performances: a meta-analysis. BMC Musculoskelet Disord. 2019;20(1):212-233. [13] KIM HH, KIM KH. Effects of Kinesio Taping with Squat Exercise on the Muscle Activity, Muscle Strength, Muscle Tension, and Dynamic Stability of Softball Players in the Lower Extremities: A Randomized Controlled Study. Int J Environ Res Public Health. 2021;19(1):276-286. [14] BALKI S, GÖKTAŞ HE, ÖZTEMUR Z. Kinesio taping as a treatment method in the acute phase of ACL reconstruction: A double-blind, placebo-controlled study. Acta Orthop Traumatol Turc. 2016;50(6):628-634. [15] LIMROONGREUNGRAT W, BOONKERD C. Immediate effect of ACL kinesio taping technique on knee joint biomechanics during a drop vertical jump: a randomized crossover controlled trial. BMC Sports Sci Med Rehabil. 2019;11(11):32-38. [16] AMEL KHABAZAN M, SOLTANI H. The mid – term effect of kinesio taping on peak power of quadriceps and hamstring muscles after anterior cruciate ligament reconstruction. Physical education of students. 2017;21(1):27-32. [17] OLIVEIRA AK, BORGES DT, LINS CA, et al. Immediate effects of Kinesio Taping(®) on neuromuscular performance of quadriceps and balance in individuals submitted to anterior cruciate ligament reconstruction: A randomized clinical trial. J Sci Med Sport. 2016;19(1):2-6. [18] CHAN MC, WEE JW, LIM MH. Does Kinesiology Taping Improve the Early Postoperative Outcomes in Anterior Cruciate Ligament Reconstruction? A Randomized Controlled Study. Clin J Sport Med. 2017;27(3):260-265. [19] LABIANCA L, ANDREOZZI V, PRINCI G, et al. The effectiveness of Kinesio Taping in improving pain and edema during early rehabilitation after Anterior Cruciate Ligament Reconstruction: A Prospective, Randomized, Control Study. Acta Biomed. 2022;92(6):e2021336. [20] BALTACI G, OZUNLU PEKYAVAS N, ATAY OA. Short-time Effect of Sterile Kinesio Tape applied during Anterior Cruciate Ligament Reconstruction on Edema, Pain and Range of Motion. Res Sports Med. 2021:2(12):1-12. [21] AGHAPOUR E, KAMALI F, SINAEI E. Effects of Kinesio Taping(®) on knee function and pain in athletes with patellofemoral pain syndrome. J Bodyw Mov Ther. 2017;21(4):835-839. [22] AYTAR A, OZUNLU N, SURENKOK O, et al. Initial effects of kinesio® taping in patients with patellofemoral pain syndrome: A randomized, double-blind study. Isokinetics and Exercise Science. 2011;19(2):135-142. [23] BALKI S, GöKTAS HE. Short-Term Effects of the Kinesio Taping® on Early Postoperative Hip Muscle Weakness in Male Patients With Hamstring Autograft or Allograft Anterior Cruciate Ligament Reconstruction. J Sport Rehabil. 2019;28(4):311-317. [24] LIETZ-KIJAK D, KIJAK E, KRAJCZY M, et al. The Impact of the Use of Kinesio Taping Method on the Reduction of Swelling in Patients After Orthognathic Surgery: A Pilot Study. Med Sci Monit. 2018;24(6):3736-3743. [25] BOGUSZEWSKI D, TOMASZEWSKA I, ADAMCZYK JG, et al. Evaluation of effectiveness of kinesiology taping as an adjunct to rehabilitation following anterior cruciate ligament reconstruction. Preliminary report. Ortop Traumatol Rehabil. 2013;15(5):469-478. [26] BIAŁOSZEWSKI D, WOŹNIAK W, ZAREK S. Clinical efficacy of kinesiology taping in reducing edema of the lower limbs in patients treated with the ilizarov method--preliminary report. Ortop Traumatol Rehabil. 2009;11(1):46-54. [27] DONEC V, KRIŠČIŪNAS A. The effectiveness of Kinesio Taping® after total knee replacement in early postoperative rehabilitation period. A randomized controlled trial. Eur J Phys Rehabil Med. 2014;50(4):363-371. [28] PELLETIER A, SANZO P, KIVI D, et al. The effect of patellar taping on lower extremity running kinematics in individuals with patellofemoral pain syndrome. Physiother Theory Pract. 2019; 35(8):764-772. [29] YOSHIDA A, KAHANOV L. The effect of kinesio taping on lower trunk range of motions. Res Sports Med. 2007;15(2):103-112. [30] LU Z, LI X, CHEN R, et al. Kinesio taping improves pain and function in patients with knee osteoarthritis: A meta-analysis of randomized controlled trials. Int J Surg. 2018;59(11):27-35. [31] MONTALVO AM, CARA EL, MYER GD. Effect of kinesiology taping on pain in individuals with musculoskeletal injuries: systematic review and meta-analysis. Phys Sportsmed. 2014;42(2):48-57. [32] PIVA SR, FITZGERALD GK, WISNIEWSKI S, et al. Predictors of pain and function outcome after rehabilitation in patients with patellofemoral pain syndrome. J Rehabil Med. 2009;41(8):604-612. [33] GóMEZ-SORIANO J, ABIáN-VICéN J, APARICIO-GARCíA C, et al. The effects of Kinesio taping on muscle tone in healthy subjects: a double-blind, placebo-controlled crossover trial. Man Ther. 2014;19(2):131-136. [34] CSAPO R, ALEGRE LM. Effects of Kinesio(®) taping on skeletal muscle strength-A meta-analysis of current evidence. J Sci Med Sport. 2015;18(4): 450-456. [35] LIU K, QIAN J, GAO Q, et al. Effects of Kinesio taping of the knee on proprioception, balance, and functional performance in patients with anterior cruciate ligament rupture: A retrospective case series. Medicine (Baltimore). 2019;98(48):e17956. [36] BELL DR, KULOW SM, STIFFLER MR, et al. Squatting mechanics in people with and without anterior cruciate ligament reconstruction: the influence of graft type. Am J Sports Med. 2014;42(12):2979-2987. [37] TAN SHS, LAU BPH, KRISHNA L. Outcomes of Anterior Cruciate Ligament Reconstruction in Females Using Patellar-Tendon-Bone versus Hamstring Autografts: A Systematic Review and Meta-Analysis. J Knee Surg. 2019;32(8):770-787. [38] HEWETT TE, MYER GD, FORD KR. Anterior cruciate ligament injuries in female athletes: Part 1, mechanisms and risk factors. Am J Sports Med. 2006;34(2):299-311. |
| [1] | Zhang Zeyi, Yang Yimin, Li Wenyan, Zhang Meizhen. Effect of foot progression angle on lower extremity kinetics of knee osteoarthritis patients of different ages: a systematic review and meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 968-975. |
| [2] | Hu Zhixing, Li Qun, Yang Chao, Wang Xiaoxiao, Fang Luochangting, Hou Wuqiong, Lin Na, Chen Weiheng, Liu Chunfang, Lin Ya. Network meta-analysis of the modeling effects of different factors on rabbit models of steroid-induced osteonecrosis of femoral head [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 976-984. |
| [3] | Abuduwupuer·Haibier, Alimujiang·Yusufu, Maihemuti·Yakufu, Maimaitimin·Abulimiti, Tuerhongjiang·Abudurexiti. Meta-analysis of efficacy and safety of terlipatide and bisphosphate in the treatment of postmenopausal osteoporosis fractures [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(4): 639-645. |
| [4] | Bai Xiaotian, Chen Zhaoying, Song Yiling, Wang Ye, Liu Jingmin. Effect of minimalist shoes on foot muscle morphology: systematic evaluation and Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(4): 646-650. |
| [5] | Dai Jiansong, Xin Dongling, Chen Gangrui. Effects of fascia gun versus stretching on exercise-induced muscle fatigue [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(2): 242-246. |
| [6] | Lyu Moran, Xu Wenxin, Wang Di, Li Ming. New trends and developments of functional training research in the field of health care [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(2): 302-307. |
| [7] | Chang Wanpeng, Zhang Zhongwen, Yang Yulin, Zi Yang, Yang Mengqi, Du Bingyu, Wang Nan, Yu Shaohong. Efficacy of rehabilitation exoskeleton robots on post-stroke lower limb motor dysfunction: a Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(2): 321-328. |
| [8] | Zhang Lichuang, Gao Huali, Wang Jingchao, Lin Huijun, Wu Chonggui, Ma Yinghui, Huang Yunfei, Fang Xue, Zhai Weitao. Effect of tendon manipulation with equal emphasis on muscles and bones on accelerating the functional rehabilitation of quadriceps femoris after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1383-1389. |
| [9] | Wang Yanjin, Zhou Yingjie, Chai Xubin, Zhuo Hanjie. Meta-analysis of the efficacy and safety of 3D printed porous titanium alloy fusion cage in anterior cervical discectomy and fusion [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1434-1440. |
| [10] | Jiang Xiaocheng, Shi Lu, Wang Yinbin, Li Qiujiang, Xi Chuangzhen, Ma Zefeng, Cai Lijun. Systematical evaluation of bone fusion rate after interbody fusion in patients with osteoporosis and lumbar degenerative disease treated with teriparatide [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1427-1433. |
| [11] | Li Wenjie, You Aijia, Zhou Junli, Fang Sujuan, Li Chun. Effects of different dressings in the treatment of burn wounds: a network meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1141-1148. |
| [12] | Chen Guanting, Zhang Linqi, Li Qingru. Meta-analysis of the value of exosomal miRNA for the diagnosis of chronic kidney disease [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 970-976. |
| [13] | Yan Le, Zhang Huiping, Dai Lintong. Mesenchymal stem cells for allergic rhinitis: a meta-analysis based on animal experiments [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 977-984. |
| [14] | Feng Liang, Gong Shuhui, Huo Hongfeng. Effect of short-foot training on foot and ankle function in patients with flat feet: Meta-analysis and systematic review [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(5): 799-804. |
| [15] | Pan Weimin, Wang Bing, Han Yabing, Li Ting, Song Jiaqi, Qin Huasheng, Liu Yang. Effects of blood flow restriction training on muscle strength, muscle mass and physical performance in older adults: a Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(5): 805-812. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||