Chinese Journal of Tissue Engineering Research ›› 2024, Vol. 28 ›› Issue (2): 321-328.doi: 10.12307/2023.868
Efficacy of rehabilitation exoskeleton robots on post-stroke lower limb motor dysfunction: a Meta-analysis
Chang Wanpeng1, Zhang Zhongwen2, Yang Yulin1, Zi Yang3, Yang Mengqi1, Du Bingyu1, Wang Nan1, Yu Shaohong3, 4
- 1College of Rehabilitation Medicine, Shandong University of Traditional Chinese Medicine, Jinan 250355, Shandong Province, China; 2The First Affiliated Hospital of Shandong First Medical University & Shandong Provincial Qianfoshan Hospital, Jinan 250014, Shandong Province, China; 3The Second Affiliated Hospital of Shandong University of Traditional Chinese Medicine, Jinan 250001, Shandong Province, China; 4College of Medicine, Shandong University of Traditional Chinese Medicine, Jinan 250355, Shandong Province, China
-
Received:2022-12-03Accepted:2023-01-10Online:2024-01-18Published:2023-06-30 -
Contact:Yu Shaohong, Associate professor, The Second Affiliated Hospital of Shandong University of Traditional Chinese Medicine, Jinan 250001, Shandong Province, China; College of Medicine, Shandong University of Traditional Chinese Medicine, Jinan 250355, Shandong Province, China -
About author:Chang Wanpeng, Master candidate, College of Rehabilitation Medicine, Shandong University of Traditional Chinese Medicine, Jinan 250355, Shandong Province, China -
Supported by:the National Natural Science Foundation of China (Youth Program), No. 82000788 (to ZZW); Cross-cutting project: HX-2020-13, No. SDAM202009003 (to YSH)
CLC Number:
Cite this article
Chang Wanpeng, Zhang Zhongwen, Yang Yulin, Zi Yang, Yang Mengqi, Du Bingyu, Wang Nan, Yu Shaohong. Efficacy of rehabilitation exoskeleton robots on post-stroke lower limb motor dysfunction: a Meta-analysis[J]. Chinese Journal of Tissue Engineering Research, 2024, 28(2): 321-328.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
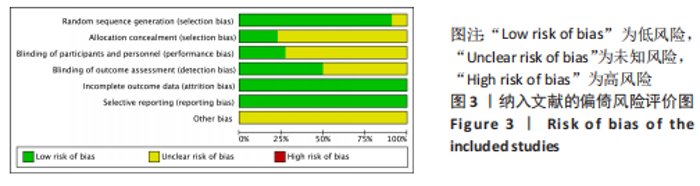
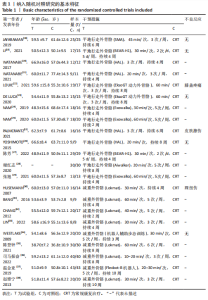
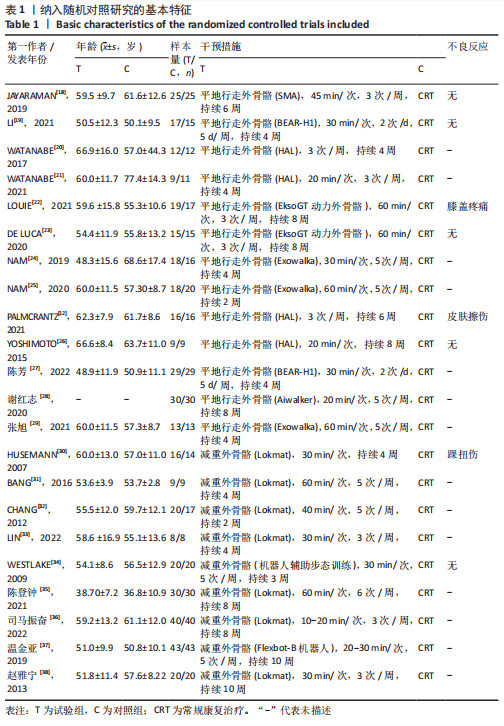
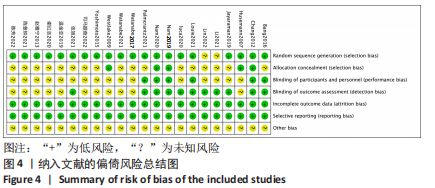
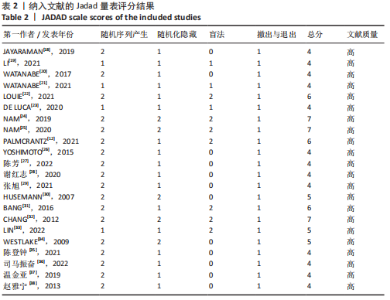
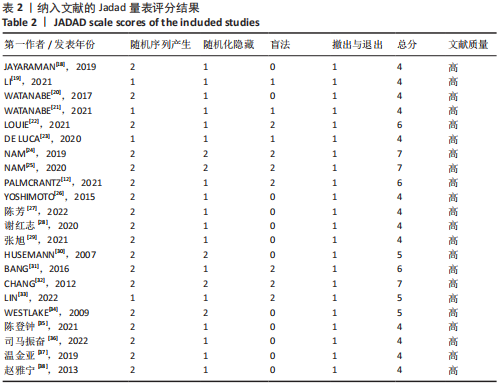
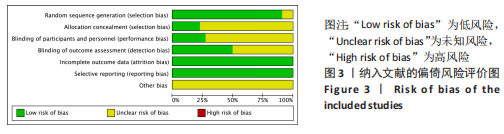
2.2 纳入文献的质量评价结果 纳入的22篇文献均提及随机分组[12,18-38],其中19篇文献提及具体随机方法(低风险)[12,18,20-22,24-32,34-38];5篇文献对研究进行分配隐藏(低风险) [24-25,30,32,34];6篇文献对纳入对象或干预者施盲(低风险) [12,22,24-25,31-32],10篇文献对结果测评者施盲(低风险) [12,18-19,22,24-25,29,31-33];所有文献数据结果完整(低风险)[12,18-38];所有文献无选择性报道(低风险) [12,18-38];所有文献其他偏倚风险情况均不清楚[12,18-38]。 各项研究具体评估结果见图3,4。根据修订版Jadad量表进行质量评价,所有文献均为高质量[12,18-38],平均4.82分,详情见表2。"
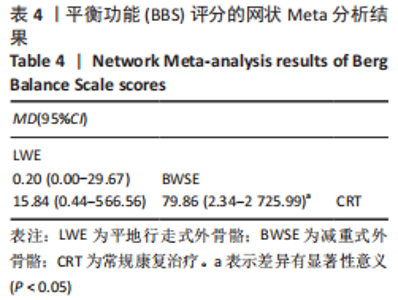
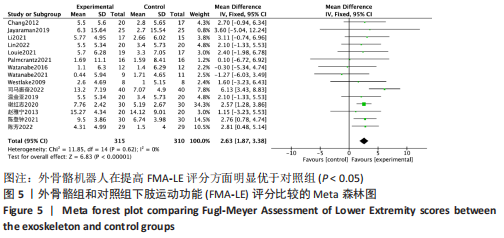
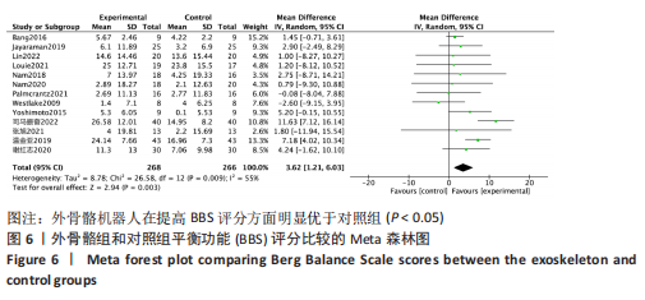
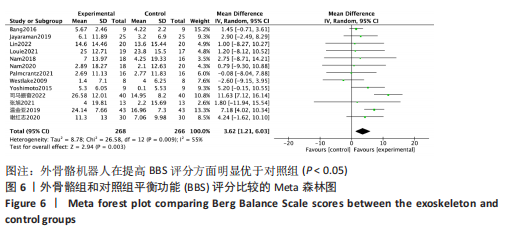
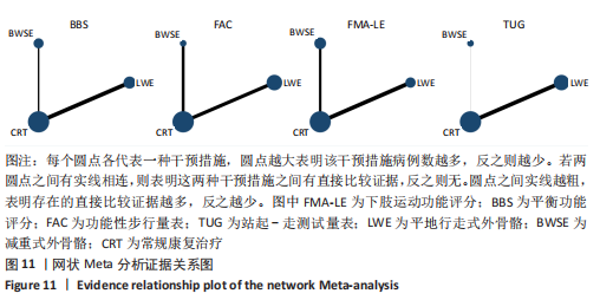
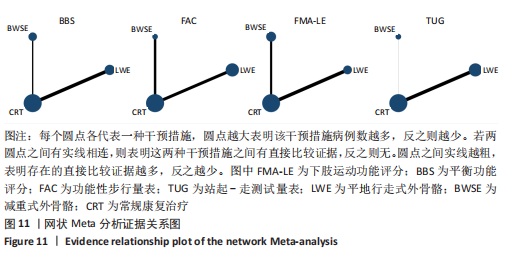
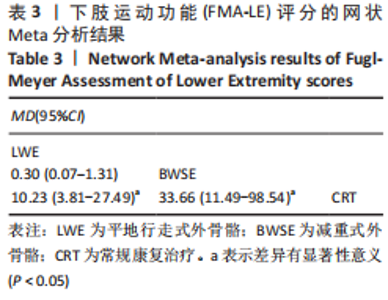
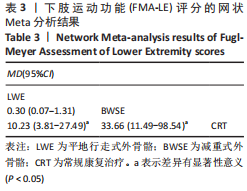
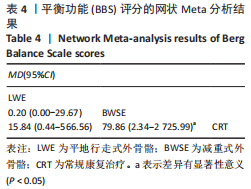
2.4.2 BBS评分分析结果 (1)纳入研究证据关系:有13项研究的结局指标涉及到BBS评分[12,18,22,24-26,28-29,31,33-34,36-37],网状Meta分析共涉及到平地行走式外骨骼、减重式外骨骼和常规康复治疗3种训练方法。进行不同训练后BBS评分的网状关系见图11。 (2)BBS评分的异质性检测结果:所纳入结局指标均为双臂研究,故进性异质性分析,见图6。结果显示,研究间总体I2=55%,提示各研究间有异质性,采用随机效应模型。 (3)BBS评分的网状Meta分析结果:减重式外骨骼与常规康复治疗相比(MD=79.86,95%CI:2.34-2 725.99)能显著改善BBS评分(P < 0.05),其他各干预措施无显著性差异(P > 0.05),见表4。"
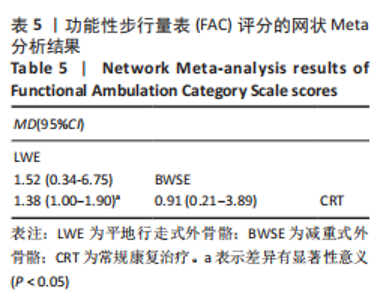
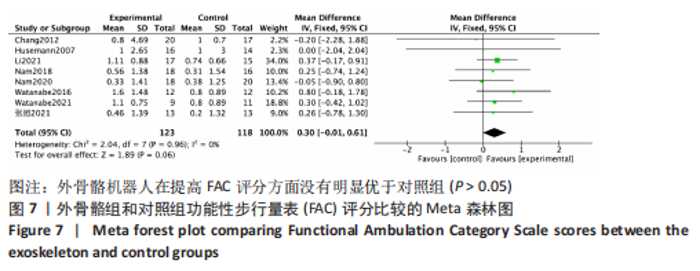
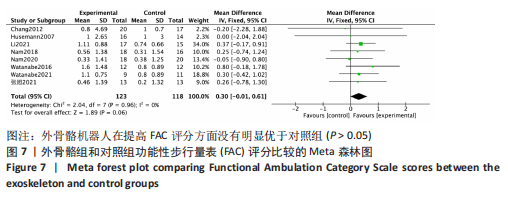
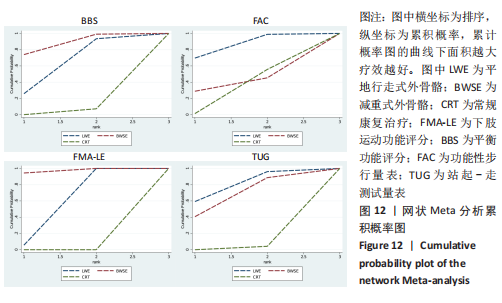
(4)BBS评分的网状Meta排序结果:各训练方法的排序结果见图12,BBS评分排序为减重式外骨骼>平地行走式外骨骼>常规康复治疗。 2.4.3 FAC评分分析结果 (1)纳入研究证据关系:有8项研究的结局指标涉及到FAC评分[19-21,24-25,29-30,32],网状Meta分析共涉及到平地行走式外骨骼、减重式外骨骼和常规康复治疗3种训练方法。进行不同训练后FAC评分的网状关系见图11。 (2)FAC的异质性检测结果:所纳入结局指标均为双臂研究,故进性异质性分析,见图7。结果显示,研究间总体I2=0%,提示各研究间无异质性,采用固定效应模型。 (3)FAC评分的网状Meta分析结果:平地行走式外骨骼与常规康复治疗相比(MD=1.38,95%CI:1.00-1.90)能显著改善FAC评分(P < 0.05),其他各干预措施无显著性差异(P > 0.05),见表5。"
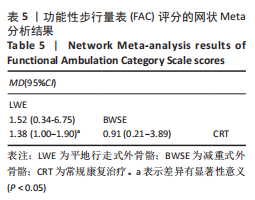
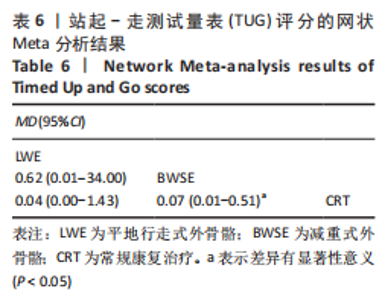
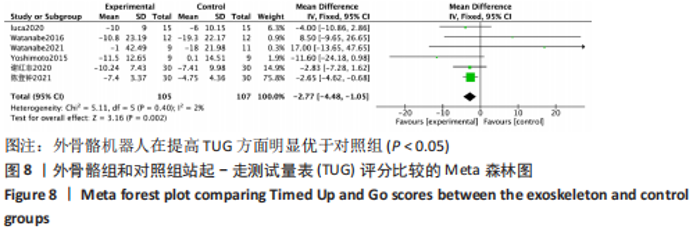
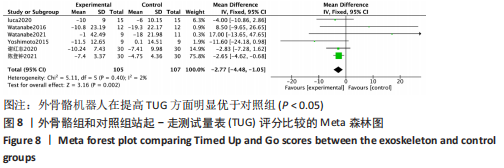
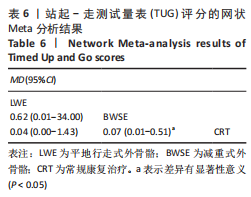
(4)FAC评分的网状Meta排序结果:各训练方法的排序结果见图12,FAC评分排序为平地行走式外骨骼>减重式外骨骼>常规康复治疗。 2.4.4 TUG评分分析结果 (1)纳入研究证据关系:有6项研究的结局指标涉及到TUG评分[20-21,23,26,28,35],网状Meta分析共涉及到平地行走式外骨骼、减重式外骨骼和常规康复治疗3种训练方法。进行不同训练后TUG评分的网状关系见图11。 (2)TUG评分的异质性检测结果:所纳入结局指标均为双臂研究,故进性异质性分析,见图8。结果显示,研究间总体I2=2%,提示各研究间异质性小,采用固定效应模型。 (3)TUG评分的网状Meta分析结果:减重式外骨骼与常规康复治疗相比(MD=0.07,95%CI:0.01-0.51)能显著改善TUG评分(P < 0.05),其余各干预措施无显著性差异(P > 0.05),见表6。"
| [1] FEIGIN VL, KRISHNAMURTHI RV, PARMAR P, et al. Update on the Global Burden of Ischemic and Hemorrhagic Stroke in 1990-2013: The GBD 2013 Study. Neuroepidemiology. 2015;45(3):161-176. [2] MUKHERJEE D, PATIL CG. Epidemiology and the global burden of stroke. World Neurosurg. 2011;76(6 Suppl):S85-S90. [3] JøRGENSEN HS, NAKAYAMA H, RAASCHOU HO, et al. Recovery of walking function in stroke patients: the Copenhagen Stroke Study. Arch Phys Med Rehabil. 1995;76(1):27-32. [4] KOLLEN B, KWAKKEL G, LINDEMAN E. Longitudinal robustness of variables predicting independent gait following severe middle cerebral artery stroke: a prospective cohort study. Clin Rehabil. 2006; 20(3):262-268. [5] YEN CL, WANG RY, LIAO KK, et al. Gait training induced change in corticomotor excitability in patients with chronic stroke. Neurorehabil Neural Repair. 2008;22(1):22-30. [6] MIYAI I, YAGURA H, HATAKENAKA M, et al. Longitudinal optical imaging study for locomotor recovery after stroke. Stroke. 2003;34(12):2866-2870. [7] PORTELLI R, LOWE D, IRWIN P, et al. Institutionalization after stroke. Clin Rehabil. 2005; 19(1):97-108. [8] SCRIVENER K, SHERRINGTON C, SCHURR K. Exercise dose and mobility outcome in a comprehensive stroke unit: description and prediction from a prospective cohort study. J Rehabil Med. 2012; 44(10):824-829. [9] FRENCH B, THOMAS L, LEATHLEY M, et al. Does repetitive task training improve functional activity after stroke? A Cochrane systematic review and meta-analysis. J Rehabil Med. 2010;42(1):9-14. [10] MORONE G, PAOLUCCI S, CHERUBINI A, et al. Robot-assisted gait training for stroke patients: current state of the art and perspectives of robotics. Neuropsychiatr Dis Treat. 2017;13(13):3-11. [11] BIERNASKIE J, CHERNENKO G, CORBETT D. Efficacy of rehabilitative experience declines with time after focal ischemic brain injury. J Neurosci. 2004; 24(5):1245-1254. [12] PALMCRANTZ S, WALL A, VREEDE KS, et al. Impact of intensive gait training with and without electromechanical assistance in the chronic phase after stroke-a multi-arm randomized controlled trial with a 6 and 12 months follow up. Front Neurosci. 2021;15:660726. [13] MEHRHOLZ J, THOMAS S, WERNER C, et al. Electromechanical-assisted training for walking after stroke. Cochrane Database Syst Rev. 2017; 5(5):Cd006185. [14] MOUCHEBOEUF G, GRIFFIER R, GASQ D, et al. Effects of robotic gait training after stroke: a meta-analysis. Ann Phys Rehabil Med. 2020;63(6):518-534. [15] MEHRHOLZ J, POHL M, KUGLER J, et al. The Improvement of Walking Ability Following Stroke. Dtsch Arztebl Int. 2018;115(39):639-645. [16] 杨旭,马秋平.下肢康复机器人辅助训练改善脑卒中病人下肢功能效果的Meta分析[J].循证护理,2018,4(8):673-679. [17] 各类脑血管疾病诊断要点[J].中华神经科杂志, 1996(6):60-61. [18] JAYARAMAN A, O’BRIEN MK, MADHAVAN S, et al. Stride management assist exoskeleton vs functional gait training in stroke: a randomized trial. Neurology. 2019;92(3):e263-e273. [19] LI DX, ZHA FB, LONG JJ, et al. Effect of robot assisted gait training on motor and walking function in patients with subacute stroke: a random controlled study. J Stroke Cerebrovasc Dis. 2021;30(7):105807. [20] WATANABE H, GOTO R, TANAKA N, et al. Effects of gait training using the Hybrid Assistive Limb® in recovery-phase stroke patients: a 2-month follow-up, randomized, controlled study. NeuroRehabilitation. 2017;40(3):363-367. [21] WATANABE H, TSURUSHIMA H, YANAGI H. Effect of hybrid assistive limb treatment on maximal walking speed and six-minute walking distance during stroke rehabilitation: a pilot study. J Phys Ther Sci. 2021;33(2):168-174. [22] LOUIE DR, MORTENSON WB, DUROCHER M, et al. Efficacy of an exoskeleton-based physical therapy program for non-ambulatory patients during subacute stroke rehabilitation: a randomized controlled trial. J Neuroeng Rehabil. 2021;18(1):149. [23] DE LUCA R, MARESCA G, BALLETTA T, et al. Does overground robotic gait training improve non-motor outcomes in patients with chronic stroke? Findings from a pilot study. J Clin Neurosci. 2020;81:240-245. [24] NAM YG, LEE JW, PARK JW, et al. Effects of electromechanical exoskeleton-assisted gait training on walking ability of stroke patients: a randomized controlled trial. Arch Phys Med Rehabil. 2019;100(1):26-31. [25] NAM YG, PARK JW, LEE HJ, et al. Further effects of electromechanically assisted gait trainer (Exowalk®) in patients with chronic stroke: a randomized controlled trial. J Rehabil Med. 2020; 52(9):jrm00097. [26] YOSHIMOTO T, SHIMIZU I, HIROI Y, et al. Feasibility and efficacy of high-speed gait training with a voluntary driven exoskeleton robot for gait and balance dysfunction in patients with chronic stroke: nonrandomized pilot study with concurrent control. Int J Rehabil Res. 2015;38(4):338-343. [27] 陈芳,季晶,苏彬,等.平地行走式下肢外骨骼机器人对脑卒中患者步行功能的影响[J].中华物理医学与康复杂志,2022,44(6):497-502. [28] 谢红志,董继革,王战斌,等.下肢外骨骼助行机器人对脑卒中患者运动功能和步行能力恢复的影响[J].中国老年保健医学,2020,18(6):68-72. [29] 张旭,邱模炎,权范善,等.步行机器人训练对慢性期脑卒中偏瘫患者步行能力的影响[J].中华物理医学与康复杂志,2021,43(1):30-33. [30] HUSEMANN B, MüLLER F, KREWER C, et al. Effects of locomotion training with assistance of a robot-driven gait orthosis in hemiparetic patients after stroke: a randomized controlled pilot study. Stroke. 2007;38(2):349-354. [31] BANG DH, SHIN WS. Effects of robot-assisted gait training on spatiotemporal gait parameters and balance in patients with chronic stroke: a randomized controlled pilot trial. NeuroRehabilitation. 2016;38(4):343-349. [32] CHANG WH, KIM MS, HUH JP, et al. Effects of robot-assisted gait training on cardiopulmonary fitness in subacute stroke patients: a randomized controlled study. Neurorehabil Neural Repair. 2012;26(4): 318-324. [33] LIN YN, HUANG SW, KUAN YC, et al. Hybrid robot-assisted gait training for motor function in subacute stroke: a single-blind randomized controlled trial. J Neuroeng Rehabil. 2022;19(1):99. [34] WESTLAKE KP, PATTEN C. Pilot study of Lokomat versus manual-assisted treadmill training for locomotor recovery post-stroke. J Neuroeng Rehabil. 2009;6:18. [35] 陈登钟,苏小燕,黄祖成.下肢机器人步态训练对脑卒中足下垂患者的疗效观察[J].按摩与康复医学,2021,12(3):7-9, 16. [36] 司马振奋,龚剑秋,吴月峰.Lokomat训练对脑卒中后下肢痉挛患者步行能力的影响[J].中华物理医学与康复杂志,2022,44(3):209-213. [37] 温金亚.下肢康复机器人结合康复训练对脑卒中偏瘫患者下肢肌力及平衡功能的影响[J].中国疗养医学,2019,28(11):1163-1165. [38] 赵雅宁,郝正玮,李建民.Lokomat对脑梗死后偏瘫患者关节活动度及下肢运动功能的影响[J].中华物理医学与康复杂志,2013,35(8):626-629. [39] VIRANI SS, ALONSO A, BENJAMIN EJ, et al. Heart disease and stroke statistics-2020 update: a report from the american heart association. Circulation. 2020;141(9):e139-e596. [40] GRAU-PELLICER M, CHAMARRO-LUSAR A, MEDINA-CASANOVAS J, et al. Walking speed as a predictor of community mobility and quality of life after stroke. Top Stroke Rehabil. 2019;26(5):349-358. [41] MINET LR, PETERSON E, VON KOCH L, et al. Occurrence and predictors of falls in people with stroke: six-year prospective study. Stroke. 2015;46(9):2688-2690. [42] KLEIM JA, JONES TA. Principles of experience-dependent neural plasticity: implications for rehabilitation after brain damage. J Speech Lang Hear Res. 2008;51(1):S225-S239. [43] SALE P, FRANCESCHINI M, WALDNER A, et al. Use of the robot assisted gait therapy in rehabilitation of patients with stroke and spinal cord injury. Eur J Phys Rehabil Med. 2012;48(1):111-121. [44] CALABRò RS, CACCIOLA A, BERTè F, et al. Robotic gait rehabilitation and substitution devices in neurological disorders: where are we now? Neurol Sci. 2016;37(4):503-514. [45] CHRISTENSEN LO, JOHANNSEN P, SINKJAER T, et al. Cerebral activation during bicycle movements in man. Exp Brain Res. 2000;135(1):66-72. [46] FLANSBJER UB, BLOM J, BROGåRDH C. The reproducibility of Berg Balance Scale and the Single-leg Stance in chronic stroke and the relationship between the two tests. PM R. 2012; 4(3):165-170. [47] BORTOLE M, VENKATAKRISHNAN A, ZHU F, et al. The H2 robotic exoskeleton for gait rehabilitation after stroke: early findings from a clinical study. J Neuroeng Rehabil. 2015;12:54. [48] BUESING C, FISCH G, O’DONNELL M, et al. Effects of a wearable exoskeleton stride management assist system (SMA®) on spatiotemporal gait characteristics in individuals after stroke: a randomized controlled trial. J Neuroeng Rehabil. 2015;12:69. [49] PETERS S, HANDY TC, LAKHANI B, et al. Motor and visuospatial attention and motor planning after stroke: considerations for the rehabilitation of standing balance and gait. Physical therapy. 2015;95(10):1423-1432. [50] MOLTENI F, GASPERINI G, CANNAVIELLO G, et al. Exoskeleton and end-effector robots for upper and lower limbs rehabilitation: narrative review. Pm r. 2018;10(9 Suppl 2):S174-S188. [51] KWONG PWH, NG SSM. Cutoff score of the lower-extremity motor subscale of fugl-meyer assessment in chronic stroke survivors: a cross-sectional study. Arch Phys Med Rehabil. 2019;100(9):1782-1787. |
| [1] | Wu Maodong, Su Qinglun, Huang Yiming, Shen Longying, Lu Yu, Zhao Qin. Correlation between coronal pressure variation and coronal imbalance in adolescent idiopathic scoliosis patients [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 852-856. |
| [2] | Zhang Lili, Zhang Xinglai, Zhang Jie, Zheng Jiejiao. Effect of visual feedback on landing biomechanics in chronic ankle instability patients [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 900-904. |
| [3] | Zhang Zeyi, Yang Yimin, Li Wenyan, Zhang Meizhen. Effect of foot progression angle on lower extremity kinetics of knee osteoarthritis patients of different ages: a systematic review and meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 968-975. |
| [4] | Hu Zhixing, Li Qun, Yang Chao, Wang Xiaoxiao, Fang Luochangting, Hou Wuqiong, Lin Na, Chen Weiheng, Liu Chunfang, Lin Ya. Network meta-analysis of the modeling effects of different factors on rabbit models of steroid-induced osteonecrosis of femoral head [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 976-984. |
| [5] | Dai Xinyu, Yan Jihong, Hua Lingjun, Zheng Xiaohong. Resistance exercise improves body composition in overweight and obese people: an umbrella review [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(2): 267-271. |
| [6] | Ying Chunmiao, Pan Xiaolong, Liu Feixiang, Chen Na, Fan Feiyan, Zhang Yunke. Effect of traditional Chinese medicine and compounds for supplementing qi and activating blood circulation and inducing resuscitation on regulating stem cells to promote nerve repair of acute ischemic stroke [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(1): 121-130. |
| [7] | Yang Ting, Ding Zhibin, Jiang Nan, Han Hongxia, Hou Miaomiao, Ma Cungen, Song Lijuan, Li Xinyi. Astrocytes regulate glial scar formation in cerebral ischemic stroke [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(1): 131-138. |
| [8] | Liu Xinyue, Xing Xinyang, Huo Hongfeng. Differences in human dynamic stability during walking under different cognitive loads [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1335-1339. |
| [9] | Zhong Jiamin, Huang Zhaoxin, Li Longxue, Qu Tongtong, Liu Zhuang, Fu Yifeng, Xiao Xiaofei. Effects of visual factors on balance function in young adults [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1245-1249. |
| [10] | Yu Wenqiang, Ren Fuchao, Shi Guohong, Xu Yuanjing, Liu Tongyou, Xie Youzhuan, Wang Jinwu, . Methods and application of gait analysis of lower limbs after stroke [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1257-1263. |
| [11] | Nie Chenchen, Su Kaiqi, Gao Jing, Fan Yongfu, Ruan Xiaodi, Yuan Jie, Duan Zhaoyuan, Feng Xiaodong. The regulatory role of circular RNAs in cerebral ischemia-reperfusion injury [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1286-1291. |
| [12] | Li Wenjie, You Aijia, Zhou Junli, Fang Sujuan, Li Chun. Effects of different dressings in the treatment of burn wounds: a network meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1141-1148. |
| [13] | Pan Weimin, Wang Bing, Han Yabing, Li Ting, Song Jiaqi, Qin Huasheng, Liu Yang. Effects of blood flow restriction training on muscle strength, muscle mass and physical performance in older adults: a Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(5): 805-812. |
| [14] | Liang Xiao, Zhao Panchao, Li Jiahui, Ji Zhongqiu, Jiang Guiping. Gait and biomechanical characteristics of lower limbs in multi-task walking of 4-6-year-old children [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 505-512. |
| [15] | Li Shihao, Li Qi, Li Zhen, Zhang Yuanyuan, Liu Miaomiao, Ouyang Yi, Xu Weiguo. Plantar pressure and gait analysis in patients with anterior cruciate ligament injury and reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 626-631. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||