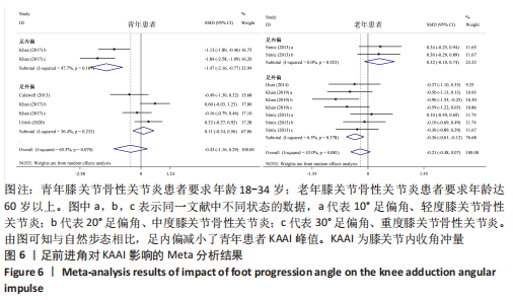
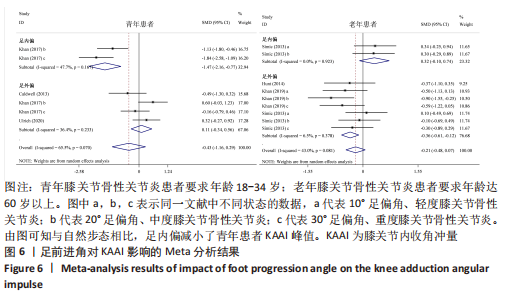
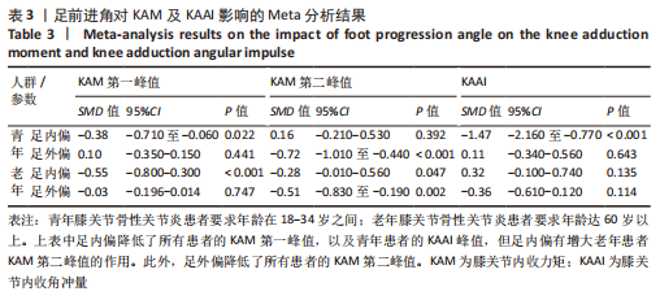
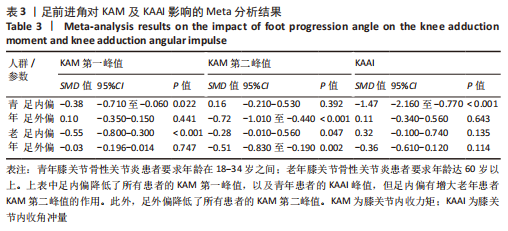
Chinese Journal of Tissue Engineering Research ›› 2024, Vol. 28 ›› Issue (6): 968-975.doi: 10.12307/2023.782
Previous Articles Next Articles
Effect of foot progression angle on lower extremity kinetics of knee osteoarthritis patients of different ages: a systematic review and meta-analysis
Zhang Zeyi1, Yang Yimin1, Li Wenyan2, Zhang Meizhen1
- 1College of Physical Education, Taiyuan University of Technology, Taiyuan 030024, Shanxi Province, China; 2College of Physical Education, Woosuk University, Jeonju 55338, South Korea
-
Received:2022-11-07Accepted:2022-12-24Online:2024-02-28Published:2023-07-13 -
Contact:Zhang Meizhen, PhD, Professor, College of Physical Education, Taiyuan University of Technology, Taiyuan 030024, Shanxi Province, China -
About author:Zhang Zeyi, Master, College of Physical Education, Taiyuan University of Technology, Taiyuan 030024, Shanxi Province, China -
Supported by:The First Batch of New Liberal Arts Research and Reform Practice Project, No. 2021050026 (to ZMZ); Shanxi Provincial Basic Research Program (Free Exploration Project), No. 202103021224109 (to ZMZ); Research Project Supported by Shanxi Scholarship Council of China, No. 2020-032 (to ZMZ); 2021 Shanxi Graduate Education and Teaching Reform Project, No. 2021YJJG067 (to ZMZ); Discipline Construction Funds of Taiyuan University of Technology, No. 2022 (to SDB)
CLC Number:
Cite this article
Zhang Zeyi, Yang Yimin, Li Wenyan, Zhang Meizhen. Effect of foot progression angle on lower extremity kinetics of knee osteoarthritis patients of different ages: a systematic review and meta-analysis[J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 968-975.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
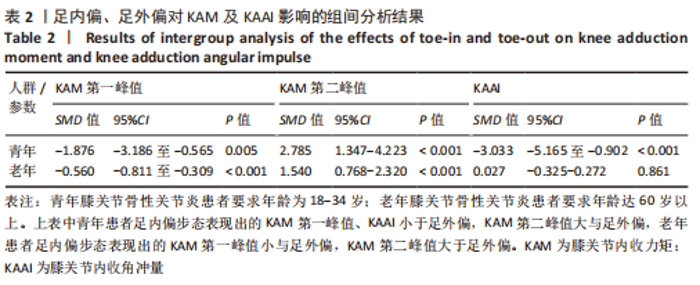
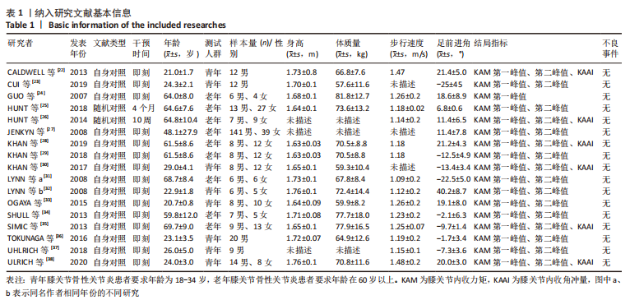
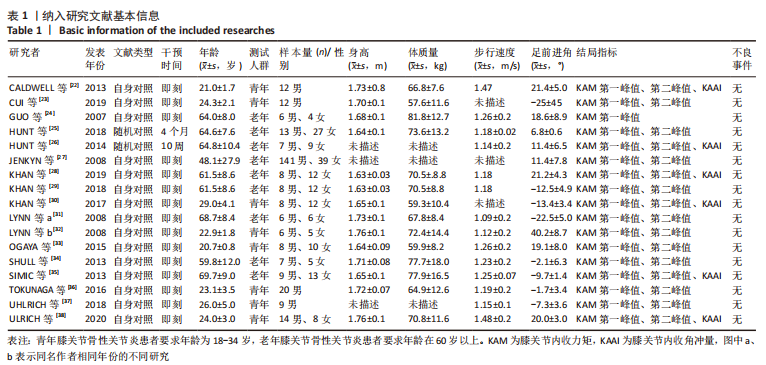
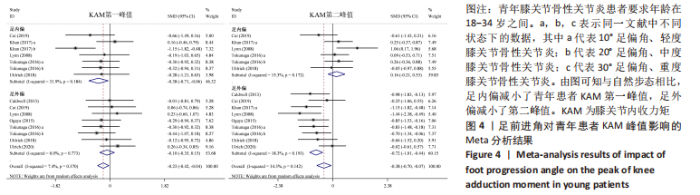
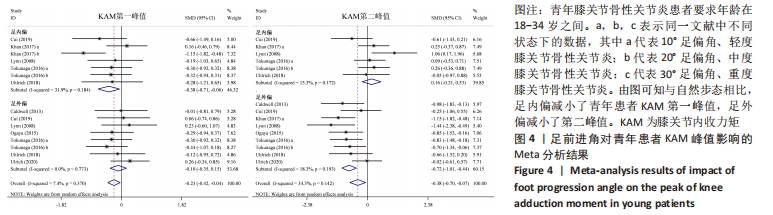
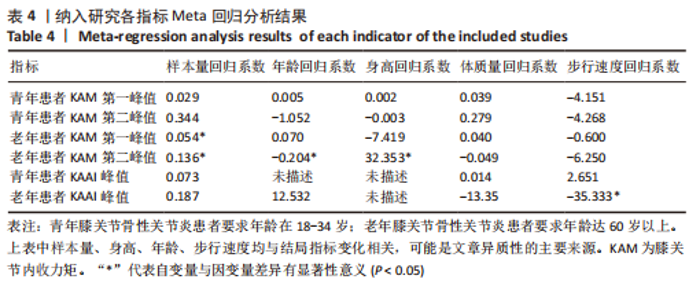
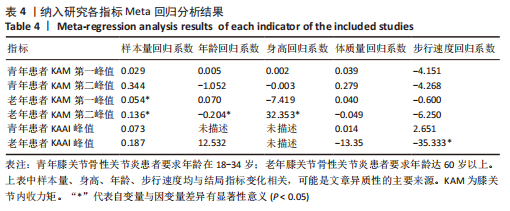
如图4,6,表2,3所示,共有8篇文献分析了足前进角对青年患者KAM第一峰值的影响[22-23,30,32-33,36-38],各文献间的异质性不显著(I2=7.4%,P=0.370)。Meta结果显示,与中立位(SMD=-0.380,95%CI:-0.710至-0.060,P=0.022)和足外偏(SMD=-1.876,95%CI: -3.186至-0.565,P=0.005)相比,足内偏可减小青年患者KAM第一峰值。另有8篇文献分析了足前进角对青年患者KAM第二峰值的影响[22-23,30,32-33,36-38],各文献间的异质性较小(I2=34.3%,P=0.142)。结果发现,与中立位相比,足外偏显著降低了该人群KAM第二峰值(SMD=-0.720,95%CI:-1.010至-1.440,P < 0.001)。此外,青年患者足外偏步态表现出的KAM第二峰值显著小于足内偏(SMD=2.785,95%CI:1.347-4.223,P < 0.001)。有3篇研究分析了足前进角对青年患者KAAI峰值的影响[22,30,38],异质性结果显示I2=65.5%,P=0.070。青年患者足内偏步态表现出的KAAI较中立位(SMD=-1.470,95%CI:-2.160至-0.770,P < 0.001)和足外偏(SMD=-3.033,95%CI:-5.165至-0.902,P < 0.001)更小。"
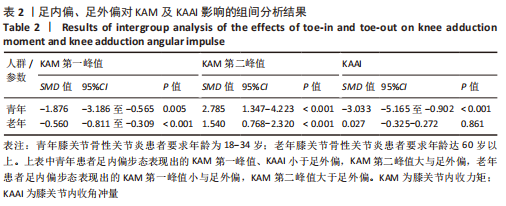
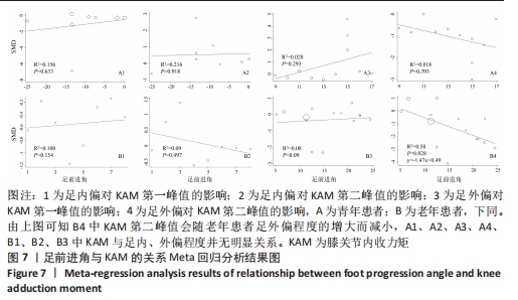
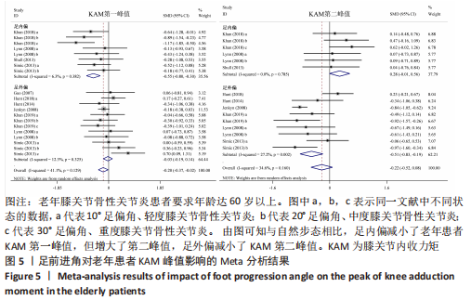
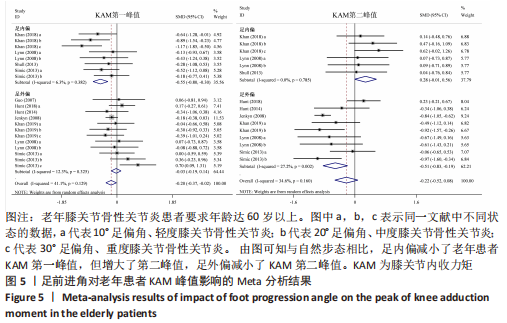
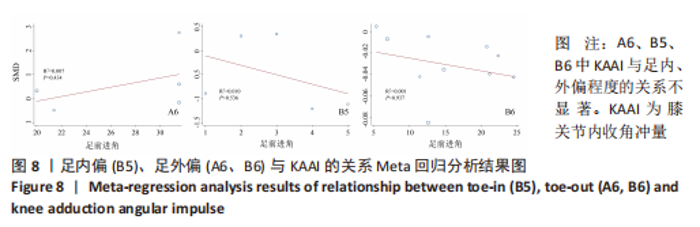
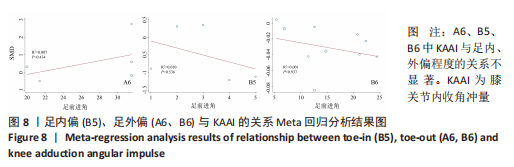
如图5,6,表2,3所示,共有9篇文献分析了足前进角对老年患者KAM第一峰值的影响[24-29,31,34-35],各文献间的异质性不显著(I2=41.1%,P=0.129)。研究发现与中立位(SMD=-0.550,95%CI: -0.800至-0.300,P < 0.001)和足外偏(SMD=-0.560,95%CI:-0.811至-0.309,P < 0.001)相比,足内偏显著减小了该人群KAM第一峰值。另有8篇文献分析了足前进角对老年患者KAM第二峰值的影响[25-29,31,34-35],各文献间的异质性较小(I2=34.6%,P=0.160)。亚组分析和组间分析显示,与中立位相比,足内偏增大了老年患者KAM第二峰值(SMD=0.280,95%CI:-0.010-0.560,P=0.047);足外偏显著减小了老年患者KAM第二峰值(SMD=-0.510,95%CI:-0.830至-0.190,P=0.002),且组间差异显著(SMD=1.540,95%CI:0.768-2.320,P < 0.001)。此外,有3篇文献分析了足前进角对老年患者KAAI峰值的影响[5,7,14],异质性检验结果显示I2=43.0%,P=0.081。结果分析发现,足内偏(SMD=0.320,95%CI: -0.100至-0.740,P=0.135)和足外偏(SMD=-0.360,95%CI:-0.610至-0.120,P=0.114)并未影响老年患者KAAI,组间差异不显著(SMD=-0.027,95%CI:-0.325-0.272,P=0.861)。 2.2.2 足前进角与KAM第一、二峰值以及KAAI的Meta回归结果 如图7,8所示,文章还对不同年龄患者中足前进角大小与KAM双峰、KAAI进行了Meta回归分析,共涉及17篇纳入研究[22-38]。对于老年患者,KAM第二峰值会随足外偏程度的增大而减小(P=0.038,R2=0.58)方程:y=-1.47x+0.49,剩余足前进角大小与KAM、KAAI的回归方程差异不显著(P > 0.05)。"
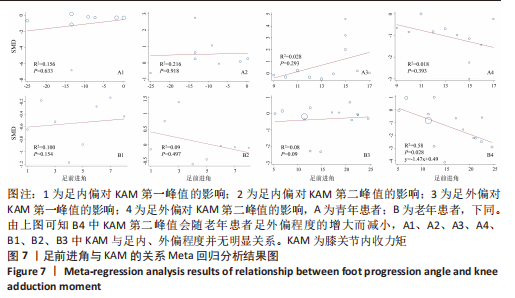
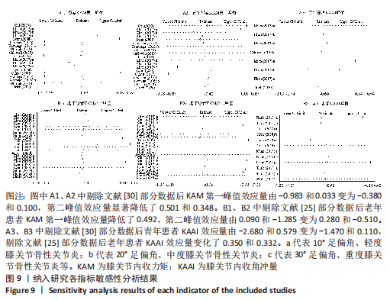
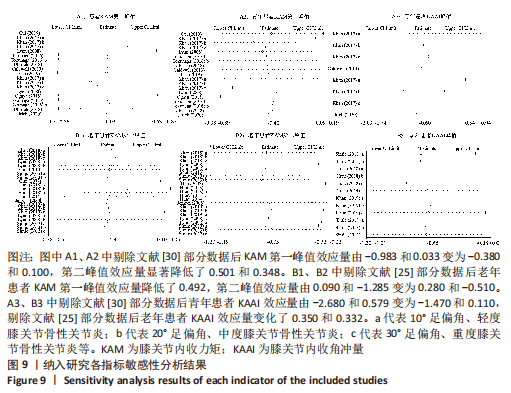
2.4 敏感性分析和Meta回归分析异质性来源结果 敏感性分析结果显示,KHAN等[30]部分数据对青年患者KAM第一峰值异质性的贡献较高,剔除该数据后效应量由-0.983和0.033变为-0.380和0.100,异质性I2由89.4%和91.4%降至31.9%和0%。KHAN等[30]部分数据对青年患者KAM第二峰值的异质性也有较大贡献,剔除该数据后效应量由0.661和-1.068变为0.160和-0.720,异质性由92%和77.5%降至15.3%和18.3%。除此之外,HUNT等[25]部分数据对老年患者KAM第一峰值的异质性的影响较大,剔除该数据后效应量由-0.550和-0.522变为-0.550和-0.030,足外偏异质性由89.4%降至12.3%。HUNT等[25]部分数据对老年患者KAM第二峰值的异质性亦贡献较大,剔除数据后效应量由0.090和-1.285变为0.280和-0.510,异质性由74.7%和92.7%降至0%和27.2%。 在KAAI比较方面,KHAN等[30]部分数据对青年患者KAAI异质性的影响较为明显,删除该数据之后效应量由-2.680和0.579变为-1.470和0.110,异质性由93.4%和88.8%降至47.7%和36.4%。HUNT等[25]部分数据则对老年患者KAAI异质性贡献较大,剔除该数据后效应量由-0.030和-0.028变为0.320和-0.360,异质性降至0%和6.5%,见图9。"
| [1] 罗盛飞,胡志波,王宁华,等.原发性膝骨关节炎易感基因多态性位点的系统综述[J].中国康复理论与实践,2022,28(7):803-808. [2] DRIBAN JB, HARKEY MS, BARBE MF, et al. Risk factors and the natural history of accelerated knee osteoarthritis: a narrative review. BMC Musculoskelet Disord. 2020;21(1):332. [3] PEREIRA D, PELETEIRO B, ARAÚJO J, et al. The effect of osteoarthritis definition on prevalence and incidence estimates: a systematic review. Osteoarthritis Cartilage. 2011;19(11):1270-1285. [4] CHEN H, WU J, WANG Z, et al. Trends and patterns of knee osteoarthritis in China: a longitudinal study of 17.7 million adults from 2008 to 2017. Int J Environ Res Public Health. 2021;18(16):8864. [5] ACKERMAN IN, KEMP JL, CROSSLEY KM, et al. Hip and knee osteoarthritis affects younger people, too. J Orthop Sports Phys Ther. 2017;47(2):67-79. [6] KATZ JN, ARANT KR, LOESER RF. Diagnosis and treatment of hip and knee osteoarthritis: a review. JAMA. 2021; 325(6):568-578. [7] BLAGOJEVIC M, JINKS C, JEFFERY A, et al. Risk factors for onset of osteoarthritis of the knee in older adults: a systematic review and meta-analysis. Osteoarthritis Cartilage. 2010;18(1):24-33. [8] SIMIC M, HARMER AR, AGALIOTIS M, et al. Clinical risk factors associated with radiographic osteoarthritis progression among people with knee pain: a longitudinal study. Arthritis Res Ther. 2021;23(1):160. [9] HUANG XM, YUAN FZ, CHEN YR, et al. Physical therapy and orthopaedic equipment-induced reduction in the biomechanical risk factors related to knee osteoarthritis: a systematic review and Bayesian network meta-analysis of randomised controlled trials. BMJ Open. 2022;12(2):e051608. [10] 汤雨婷,安丙辰,郑洁皎.膝骨关节炎生物力学参数的研究进展[J].中国康复理论与实践, 2020,26(12):1417-1421. [11] SHARMA L, HURWITZ DE, THONAR EJ, et al. Knee adduction moment, serum hyaluronan level, and disease severity in medial tibiofemoral osteoarthritis. Arthritis Rheum. 1998;41(7):1233-1240. [12] BENNELL KL, BOWLES KA, WANG Y, et al. Higher dynamic medial knee load predicts greater cartilage loss over 12 months in medial knee osteoarthritis. Ann Rheum Dis. 2011;70(10): 1770-1774. [13] KROHN K. Footwear alterations and bracing as treatments for knee osteoarthritis. Curr Opin Rheumatol. 2005;17(5):653-656. [14] SHULL P, LURIE K, SHIN M, et al. Haptic gait retraining for knee osteoarthritis treatment. Haptics Symposium. IEEE. 2010;25-26:409-416. [15] SCHACHE AG, FREGLY BJ, CROSSLEY KM, et al. The effect of gait modification on the external knee adduction moment is reference frame dependent. Clin Biomech (Bristol, Avon). 2008;23(5):601-608. [16] FREGLY BJ, REINBOLT JA, ROONEY KL, et al. Design of patient-specific gait modifications for knee osteoarthritis rehabilitation. IEEE Trans Biomed Eng. 2007;54(9):1687-1695. [17] WANG S, MO S, CHUNG RCK, et al. How foot progression angle affects knee adduction moment and angular impulse in patients with and without medial knee osteoarthritis: a meta-analysis. Arthritis Care Res (Hoboken). 2021;73(12):1763-1776. [18] DE CAMPOS D, SHOKUR S, DE LIMA-PARDINI AC, et al. Kinematics predictors of spatiotemporal parameters during gait differ by age in healthy individuals. Gait Posture. 2022;96(7):216-220. [19] MOHER D, LIBERATI A, TETZLAFF J, et al. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6(7):e1000097. [20] BELLAMY N. Validation study of WOMAC: a health status instrument for measuring clinically important patient relevant outcome to antirheumatic drug therapy in patients with osteoarthritis of the hip and knee. J Rheumatol. 1988;15(1):1833-1840. [21] NOMA H, NAGASHIMA K, KATO S, et al. Meta-analysis using flexible random-effects distribution models. J Epidemiol. 2022;32(10):441-448. [22] CALDWELL LK, LAUBACH LL, BARRIOS JA. Effect of specific gait modifications on medial knee loading, metabolic cost and perception of task difficulty. Clin Biomech (Bristol, Avon). 2013; 28(6):649-654. [23] CUI W, WANG C, CHEN W, et al. Effects of toe-out and toe-in gaits on lower-extremity kinematics, dynamics, and electromyography. Appl Sci. 2019; 9(23):1-22. [24] GUO M, AXE MJ, MANAL K. The influence of foot progression angle on the knee adduction moment during walking and stair climbing in pain free individuals with knee osteoarthritis. Gait Posture. 2007;26(3):436-441. [25] HUNT MA, CHARLTON JM, KROWCHUK NM, et al. Clinical and biomechanical changes following a 4-month toe-out gait modification program for people with medial knee osteoarthritis: a randomized controlled trial. Osteoarthritis Cartilage. 2018;26(7):903-911. [26] HUNT MA, TAKACS J. Effects of a 10-week toe-out gait modification intervention in people with medial knee osteoarthritis: a pilot, feasibility study. Osteoarthritis Cartilage. 2014;22(7):904-911. [27] JENKYN TR, HUNT MA, JONES IC, et al. Toe-out gait in patients with knee osteoarthritis partially transforms external knee adduction moment into flexion moment during early stance phase of gait: a tri-planar kinetic mechanism. J Biomech. 2008;41(2):276-283. [28] KHAN SJ, KHAN SS, USMAN J, et al. Combined effects of knee brace, laterally wedged insoles, and toe-out gait on knee adduction moment and fall risk in moderate medial knee osteoarthritis patients. Prosthet Orthot Int. 2019;43(2):148-157. [29] KHAN SJ, KHAN SS, USMAN J, et al. Combined effects of knee brace, laterally wedged insoles and toe-in gait on knee adduction moment and balance in moderate medial knee osteoarthritis patients. Gait Posture. 2018;61(3):243-249. [30] KHAN SS, KHAN SJ, USMAN J. Effects of toe-out and toe-in gait with varying walking speeds on knee joint mechanics and lower limb energetics. Gait Posture. 2017;53(3):185-192. [31] LYNN SK, COSTIGAN PA. Effect of foot rotation on knee kinetics and hamstring activation in older adults with and without signs of knee osteoarthritis. Clin Biomech (Bristol, Avon). 2008; 23(6):779-786. [32] LYNN SK, KAJAKS T, COSTIGAN PA. The effect of internal and external foot rotation on the adduction moment and lateral-medial shear force at the knee during gait. J Sci Med Sport. 2008;11(5):444-451. [33] OGAYA S, NAITO H, IWATA A, et al. Toe-Out Gait Decreases the Second Peak of the Medial Knee Contact Force. J Appl Biomech. 2015;31(4):275-280. [34] SHULL PB, SHULTZ R, SILDER A, et al. Toe-in gait reduces the first peak knee adduction moment in patients with medial compartment knee osteoarthritis. J Biomech. 2013;46(1):122-128. [35] SIMIC M, WRIGLEY TV, HINMAN RS, et al. Altering foot progression angle in people with medial knee osteoarthritis: the effects of varying toe-in and toe-out angles are mediated by pain and malalignment. Osteoarthritis Cartilage. 2013;21(9):1272-1280. [36] TOKUNAGA K, NAKAI Y, MATSUMOTO R, et al. Effect of foot progression angle and lateral wedge insole on a reduction in knee adduction moment. J Appl Biomech. 2016;32(5):454-461. [37] UHLRICH SD, SILDER A, BEAUPRE GS, et al. Subject-specific toe-in or toe-out gait modifications reduce the larger knee adduction moment peak more than a non-personalized approach. J Biomech. 2018;66(1):103-110. [38] ULRICH B, HOFFMANN L, JOLLES BM, et al. Changes in ambulatory knee adduction moment with lateral wedge insoles differ with respect to the natural foot progression angle. J Biomech. 2020;103(4):109655. [39] BIRMINGHAM TB, MARRIOTT KA, LEITCH KM, et al. Association between knee load and pain: within-patient, between-knees, case-control study in patients with knee osteoarthritis. Arthritis Care Res (Hoboken). 2019;71(5):647-650. [40] D’SOUZA N, CHARLTON J, GRAYSON J, et al. Are biomechanics during gait associated with the structural disease onset and progression of lower limb osteoarthritis? A systematic review and meta-analysis. Osteoarthritis Cartilage. 2022;30(3):381-394. [41] SIMIC M, HINMAN RS, WRIGLEY TV, et al. Gait modification strategies for altering medial knee joint load: a systematic review. Arthritis Care Res (Hoboken). 2011;63(3):405-426. [42] WANG S, CHAN KHC, LAM RHM, et al. Effects of foot progression angle adjustment on external knee adduction moment and knee adduction angular impulse during stair ascent and descent. Hum Mov Sci. 2019;64(4):213-220. [43] GOLDRING MB, OTERO M. Inflammation in osteoarthritis. Curr Opin Rheumatol. 2011;23(5): 471-478. [44] IRSIK, SARAH. The effect of toe-in/toe-out variation on locomotion: a comprehensive review. Boone: Appalachian State University. 2017. [45] ROELKER SA, KOEHN RR, CARUTHERS EJ, et al. Effects of age and knee osteoarthritis on the modular control of walking: a pilot study. PLoS One. 2021;16(12):e0261862. [46] LEE HJ, CHOU LS. Balance control during stair negotiation in older adults. J Biomech. 2007; 40(11):2530-2536. [47] HUNT MA, SIMIC M, HINMAN RS, et al. Feasibility of a gait retraining strategy for reducing knee joint loading: increased trunk lean guided by real-time biofeedback. J Biomech. 2011;44(5):943-947. [48] LYNN SK, REID SM, COSTIGAN PA. The influence of gait pattern on signs of knee osteoarthritis in older adults over a 5-11 year follow-up period: a case study analysis. Knee. 2007;14(1):22-28. [49] HART HF, BIRMINGHAM TB, PRIMEAU CA, et al. Associations between cadence and knee loading in patients with knee osteoarthritis. Arthritis Care Res (Hoboken). 2021;73(11):1667-1671. [50] WALLACE IJ, WORTHINGTON S, FELSON DT, et al. Knee osteoarthritis has doubled in prevalence since the mid-20th century. Proc Natl Acad Sci U S A. 2017;114(35):9332-9336. |
| [1] | Hu Zhixing, Li Qun, Yang Chao, Wang Xiaoxiao, Fang Luochangting, Hou Wuqiong, Lin Na, Chen Weiheng, Liu Chunfang, Lin Ya. Network meta-analysis of the modeling effects of different factors on rabbit models of steroid-induced osteonecrosis of femoral head [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 976-984. |
| [2] | Chang Wanpeng, Zhang Zhongwen, Yang Yulin, Zi Yang, Yang Mengqi, Du Bingyu, Wang Nan, Yu Shaohong. Efficacy of rehabilitation exoskeleton robots on post-stroke lower limb motor dysfunction: a Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(2): 321-328. |
| [3] | Shen Feiyan, Yao Jixiang, Su Shanshan, Zhao Zhongmin, Tang Weidong. Knockdown of circRNA WD repeat containing protein 1 inhibits proliferation and induces apoptosis of chondrocytes in knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(在线): 1-6. |
| [4] | Li Xiaomin, Tian Xiangdong, Tan Yetong, Zhu Guangyu, Wang Rongtian, Wang Jian, Xue Zhipeng, Ma Sheng, Hu Yuanyi, Huang Ye, Ding Tiansong. Changes of lower limb force line and knee function after high tibial osteotomy in osteoporotic medial ventricular knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1325-1329. |
| [5] | Zheng Hongrui, Zhang Wenjie, Wang Yunhua, He Bin, Shen Yajun, Fan Lei. Femoral neck system combined with platelet-rich plasma in the treatment of femoral neck fracture [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1390-1395. |
| [6] | Wang Yanjin, Zhou Yingjie, Chai Xubin, Zhuo Hanjie. Meta-analysis of the efficacy and safety of 3D printed porous titanium alloy fusion cage in anterior cervical discectomy and fusion [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1434-1440. |
| [7] | Jiang Xiaocheng, Shi Lu, Wang Yinbin, Li Qiujiang, Xi Chuangzhen, Ma Zefeng, Cai Lijun. Systematical evaluation of bone fusion rate after interbody fusion in patients with osteoporosis and lumbar degenerative disease treated with teriparatide [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1427-1433. |
| [8] | Yu Wenqiang, Ren Fuchao, Shi Guohong, Xu Yuanjing, Liu Tongyou, Xie Youzhuan, Wang Jinwu, . Methods and application of gait analysis of lower limbs after stroke [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1257-1263. |
| [9] | Li Wenjie, You Aijia, Zhou Junli, Fang Sujuan, Li Chun. Effects of different dressings in the treatment of burn wounds: a network meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1141-1148. |
| [10] | Chen Guanting, Zhang Linqi, Li Qingru. Meta-analysis of the value of exosomal miRNA for the diagnosis of chronic kidney disease [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 970-976. |
| [11] | Yan Le, Zhang Huiping, Dai Lintong. Mesenchymal stem cells for allergic rhinitis: a meta-analysis based on animal experiments [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(6): 977-984. |
| [12] | Feng Liang, Gong Shuhui, Huo Hongfeng. Effect of short-foot training on foot and ankle function in patients with flat feet: Meta-analysis and systematic review [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(5): 799-804. |
| [13] | Pan Weimin, Wang Bing, Han Yabing, Li Ting, Song Jiaqi, Qin Huasheng, Liu Yang. Effects of blood flow restriction training on muscle strength, muscle mass and physical performance in older adults: a Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(5): 805-812. |
| [14] | Liang Xiao, Zhao Panchao, Li Jiahui, Ji Zhongqiu, Jiang Guiping. Gait and biomechanical characteristics of lower limbs in multi-task walking of 4-6-year-old children [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 505-512. |
| [15] | Wan Guoli, Shi Chenhui, Wang Weishan, Li Ang, Shi Xunda, Cai Yi. Retrospective analysis of the influencing factors of chronic pain after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 558-564. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||