Chinese Journal of Tissue Engineering Research ›› 2022, Vol. 26 ›› Issue (5): 786-791.doi: 10.12307/2022.128
Previous Articles Next Articles
Femoroacetabular impingement: strength trainings for nerve-muscle, peripheral muscle and core muscle
Lu Qinxue, Xu Ning, Yang Yinglan, Han Qianqian, Duanmu Xianyu, Guo Yuwei, Han Qing
- Shandong University of Traditional Chinese Medicine, Jinan 250355, Shandong Province, China
-
Received:2020-10-16Revised:2020-10-21Accepted:2020-12-21Online:2022-02-18Published:2021-12-02 -
Contact:Xu Ning, MD, Associate professor, Shandong University of Traditional Chinese Medicine, Jinan 250355, Shandong Province, China -
About author:Lu Qinxue, Master candidate, Shandong University of Traditional Chinese Medicine, Jinan 250355, Shandong Province, China -
Supported by:Shandong Provincial Social Science Planning Project, No. 20CZXJ06 (to XN)
CLC Number:
Cite this article
Lu Qinxue, Xu Ning, Yang Yinglan, Han Qianqian, Duanmu Xianyu, Guo Yuwei, Han Qing. Femoroacetabular impingement: strength trainings for nerve-muscle, peripheral muscle and core muscle[J]. Chinese Journal of Tissue Engineering Research, 2022, 26(5): 786-791.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks

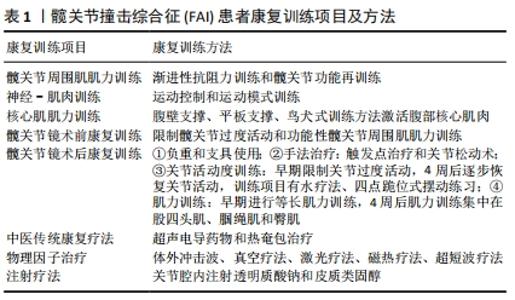
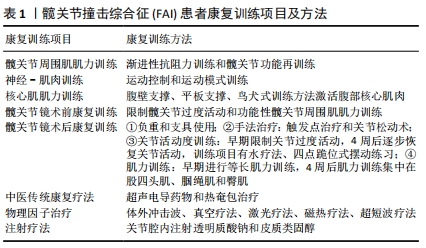
2.1 髋关节周围肌肌力训练 研究发现,FAI患者患侧髋关节周围肌肌力明显下降。CASARTELLI等[9]评估了44例FAI患者和健康受试者髋关节周围肌肌力,发现FAI患者髋内收肌、屈肌、外展肌、外旋肌最大自主等长收缩显著低于对照组,且差异有显著性意义(P < 0.05);对于单侧FAI患者,患侧髋关节周围肌肌力较无症状侧降低。NEPPLE等[10]通过对50例单侧FAI患者髋关节周围肌肌力进行研究,发现46%的患者患侧髋外展肌肌力较无症状侧下降8.7%,42%的患者患侧髋屈肌肌力较无症状侧下降8%(P < 0.05),髋屈肌肌力下降导致髋关节屈曲活动范围平均减少4.3°(P < 0.01)。RUTHERFORD等[11]通过运动捕捉系统测试40例单侧FAI患者与健康受试者行走时表面肌电活动,发现FAI组膝伸肌和屈肌,髋伸肌、屈肌和内收肌的肌力均低于无症状组(P < 0.05)。 除了髋关节周围肌的肌力改变,FAI患者髋关节周围肌的肌肉形态也发生了改变。MALLOY等[12]对50例单侧FAI患者有症状侧和无症状侧髋关节周围肌肌肉横截面积进行比较,发现有症状侧臀大肌、臀小肌和股直肌肌肉横截面积显著低于无症状侧,且差异有显著性意义(P < 0.05)。FAI患者髋关节周围肌肌肉力量下降和肌肉形态改变降低髋关节稳定性,导致下肢生物力学改变,进一步引发髋关节病理性改变。 目前所知,抗阻训练是改善肌力和肌肉耐力最有效的方 法[13]。髋关节周围肌肌力训练可有效减轻FAI患者髋部疼痛,增加髋关节关节活动度,改善患者日常生活活动能力,FAI患者髋关节周围肌肌力训练方法主要包括渐进性抗阻力训练和髋关节功能再训练[14-15]。CASARTELLI等[15]对31例FAI患者进行为期12周渐进性抗阻力训练,每周4次,包括有指导性训练和家庭训练;有指导性训练45-60 min/次,训练项目包括4项髋关节周围肌肌力训练、两项功能性下肢肌力训练、两项核心肌群稳定性训练、两项姿势平衡训练;家庭训练每次15 min,包括一项髋外展肌和髋伸肌肌力训练、一项功能性下肢肌力训练及一项核心肌群稳定性训练;结果显示,FAI患者在治疗第6周时髋部疼痛明显减轻,在治疗结束时和治疗结束后第6周髋关节周围肌肌力评价和髋关节结果评分中的日常生活活动和运动评分均达到各自最小临床重要差异值,且较训练前显著提高(P < 0.01),表明渐进性抗阻力训练短期内可有效减轻FAI患者疼痛,同时对于功能改善具有长期疗效。与单独渐进性抗阻力训练相比,抗阻力训练联合髋关节功能再训练和躯干肌肌力训练临床效果更为显著。KEMP等[14]将24例FAI患者随机分为治疗组和对照组,两组患者均接受手法治疗、渐进性抗阻力训练和健康教育,治疗组同时接受躯干肌肌力训练和髋关节功能再训练,共训练12周,包括8次物理治疗、12次健身活动、2次无监督锻炼,结果显示治疗组国际髋关节评分、髋关节残疾及骨关节炎结果评分(hip disability and osteoarthritis outcome score,HOOS)中生活质量亚量表和疼痛亚量表评分均显著高于对照组,侧桥实验、单腿跳跃实验评分显著提高,治疗组髋关节内收肌和伸展肌肌力增加0.25 N?m/kg,外旋肌肌力增加0.13 N?m/kg,外展肌肌力增加0.22 N?m/kg,髋关节屈曲活动范围增加14°,表明渐进性抗阻力训练联合髋关节功能再训练和躯干肌肌力训练可显著改善FAI患者的髋关节功能,减轻髋部疼痛。除此之外,FAI患者进行髋关节周围肌的肌力训练可有效提高股骨髋臼吻合度,增加髋关节稳定性[19]。 2.2 神经-肌肉训练 研究发现,FAI患者髋关节周围肌神经控制能力下降。ENSKI等[16]对24具新鲜尸体髋臼盂唇进行免疫组学研究发现,银染后可见环层小体、高尔基-马佐尼氏小体、鲁菲尼氏小体和克劳斯小体等感觉神经末梢器官,这些神经末梢被认为在本体感觉和髋关节疼痛中起着潜在的作用。FAI患者髋臼盂唇损伤导致感觉神经末梢受损,引起髋关节疼痛,同时髋臼盂唇损伤降低患者髋关节本体感觉,破坏FAI患者髋关节动静态稳定[17]。 与正常受试者相比,髋深部肌肉协同作用和激活模式发生改变。DIAMOND等[18]通过对15例FAI患者和14例正常受试者表面肌电进行比较发现,与正常受试者相比,FAI患者在步行过程中表现出参与协同作用的髋深部肌肌肉数量减少(P < 0.05)。DIAMOND等[19]对15例FAI患者和14例正常受试者进行对比发现,FAI患者在下蹲和上升过程中髋部所有肌肉均表现出与对照组不同的激活模式(P < 0.05),与正常受试者相比,FAI患者自由下蹲下降过程中梨状肌达到峰值的时间较晚,臀中肌和闭孔内肌激活程度高;在上升过程中FAI患者股方肌激活速度相对较慢,缝匠肌更早降至最低水平;阔筋膜张肌在下降和上升过程中基线激活和峰值激活之间的差异较大。髋深部肌肉改变作为一种保护策略,可减少髋关节功能任务中的撞击[19]。但也有研究指出,髋深部肌肉协同作用和激活模式改变导致髋关节内部负荷分布不均,引发髋臼盂唇损伤和早期髋关节骨关节炎[18]。 理论认为人体存在两个肌肉系统,即局部肌肉系统和全局肌肉系统[20]。髋关节局部肌肉因其靠近关节轴,可维持髋关节稳定,提供关节压缩力,限制股骨平移,保持正常姿势[19]。局部肌肉收缩被认为是一种前馈策略,为肢体运动做好准备,从而稳定和保护一个或多个关节[20]。FAI患者疼痛导致正常的前馈姿势发生改变,同时引起局部肌肉出现萎缩[19],随着髋关节局部肌肉的萎缩,前馈策略作用下降,导致恶性循环。RETCHFORD等[20]推测髋关节的主动稳定性主要由深层局部肌肉调节,因此提出在开始整体肌肉康复之前,可以考虑采取孤立神经-肌肉功能的干预措施,从而有效提高髋关节本体感觉,增强髋关节稳定性,减轻髋部疼痛。 神经-肌肉训练是利用关节对空间位置的感觉信息促进关节周围肌群协调发力的训练方法。除了常规肌力训练,还包括平衡训练、近端控制训练、本体感觉训练、灵敏度训练、运动模式训练[21-22]。髋关节周围肌神经-肌肉训练可有效增加髋关节周围肌肌肉横截面积,改善深层肌肉协同作用,提高FAI患者临床疗效。FAI患者神经-肌肉训练主要有运动控制训练和运动模式训练。髋关节运动控制训练是通过对FAI患者神经肌肉控制能力进行评估后针对性地制定的一类以提高神经肌肉控制为主、强化髋关节局部稳定肌肉及本体感觉、改善肌肉协同能力的一种训练方法[23]。MENDIS等[22]研究发现,腰-骨盆区域的运动控制训练,主要有单腿双腿下蹲、单腿跳跃和踢腿,可有效增加髂腰肌、缝匠肌、臀中肌、梨状肌肌肉横截面积,改善肌肉萎缩,提高骨盆稳定性(P < 0.05)。NARVESON等[24]对急性髋臼损伤合并FAI患者进行关节内皮质类固醇注射联合物理治疗,1次/周。康复训练主要进行动态、静态姿势控制训练及肌肉激活和关节矫正训练,5周后对患者进行评估发现,FAI患者外旋肌肌力较训练前增加50%,表明训练后有较大改善,国际髋关节评分提高了19%,疼痛亚量表评分降低了7.7%。关节内皮质类固醇注射可有效缓解FAI患者早期髋部疼痛,但药物注射疗法长期效果并不理想[25],关节内药物注射联合运动控制训练可有效改善FAI患者早期髋关节疼痛,改善髋关节功能,从而产生长期临床疗效。 运动模式训练主要通过优化功能任务中的生物力学来减少髋关节上的应力[26]。治疗师根据FAI患者的基本功能和引发症状给予特定任务培训,纠正错误下肢运动模式,减少作用于髋关节的应力,减轻髋部疼痛[26]。WILSON等[27]对FAI患者进行7周运动模式训练,并通过三维运动分析系统纠正患者错误运动模式,训练项目包括弓步、蛤壳式运动、桥式运动、下蹲、髋关节伸展和外展练习;训练后患者哥本哈根臀部和腹股沟结果评分从36%提高到61%;骨盆前倾角度和躯干屈曲角度显著降低;躯干和骨盆同步百分比右侧较训练前下降了20%,左侧较训练前下降了27%,表明躯干代偿运动减少,髋部肌肉控制能力改善。 2.3 核心肌肌力训练 研究发现FAI患者存在腰椎韧带紧张和腰腹部肌肉肌力不平衡的问题[28]。刘芳等[29]对30例FAI患者、无症状FAI患者和正常受试者脊柱骨盆生物力学进行研究发现,与正常受试者和无症状FAI患者相比,有症状FAI患者腰椎屈曲程度较低、髋关节屈曲程度较高、坐位时骨盆前倾角度增加 (P < 0.05)。FAI患者腰椎活动度屈曲角度减小,骨盆代偿性前倾,股骨头颈交界处与髋臼过度接触,导致髋关节唇部和软骨损伤。CHAUDHARI等[30]比较了52例FAI患者、髋臼畸形患者和正常受试者的下肢肌肉活性和骨盆活动度,发现在下蹲过程中,FAI组下蹲深度显著低于髋臼畸形组和对照组(P < 0.001);FAI组矢状面骨盆活动度低于髋臼畸形组和正常对照组(P < 0.05)。BAGWELL等[28]对30例FAI患者和正常受试者深蹲和最大高度踏步运动时骨盆协调性进行对比研究,发现FAI组骨盆股骨活动度比值明显低于对照组,相对于股骨屈曲度,骨盆后倾角度较小。在下蹲任务中,正常受试者髋关节每屈曲2°,骨盆后倾大于20°;FAI患者髋关节每屈曲4°,骨盆后倾小于10°。在最大高度踏步任务中,正常受试者髋关节每屈曲3°,骨盆后倾20°;FAI患者髋关节每屈曲4°,骨盆后倾16°。 目前被广泛认可的核心肌包括腰-骨盆-髋关节共同围成部分,主要由腹横肌、多裂肌、腰方肌组成[29]。核心稳定性几乎是所有粗大运动的重要组成部分,核心稳定性训练可有效改善脊柱异常曲度,提高躯干抗外界干扰能力,并为四肢运动提供稳定的基础[30]。FAI患者可通过腹壁支撑、平板支撑、鸟犬式训练方法激活核心肌肉。核心肌激活可稳定腰椎和骨盆,减少腰椎和骨盆代偿性运动,从而增加髋部肌肉募集量。CHAN等[31]研究腹横肌激活对髋部肌肉的影响发现,通过腹壁支撑动作激活腹横肌,在腹横肌激活状态下做蛤壳运动、侧卧位髋关节外展、俯卧位髋关节伸展运动时,双侧内斜肌活性均显著高于自然核心状态下,腹横肌激活增加髋部肌肉募集,髋部肌肉最大自主等长收缩增加0.8%-9.4%(P < 0.05)。AOYAMA等 [32]将20例FAI患者随机分为躯干训练组和对照组,对照组进行盆底肌训练、活动矫正和髋部肌肉控制训练,躯干训练组增加平板支撑训练和鸟犬式训练,每次训练20 min,1次/d。比较训练前和训练8周后临床效果发现,躯干训练组国际髋关节评分较对照组高56.3分,Vail髋关节评分由干预前58.96分提高到81.6分,髋屈肌肌力增加了0.17 N?m/kg,髋外展肌肌力增加了0.15 N?m/kg(P < 0.05)。提示深层肌肉对脊柱骨盆的稳定起重要作用,当深层肌肉出现肌无力时,浅层肌肉会发挥重要作用,因此躯干肌和骨盆浅表肌训练可有效提高FAI患者的临床疗效[32]。 腹横肌是肢体缺乏稳定性和肢体突然运动时首先被激活的肌肉,被认为是关键核心肌肉。多裂肌是肢体运动时第二块被激活的肌肉,中枢神经系统通过腹横肌和多裂肌的共同收缩为下肢运动创造了稳定的基础,因此在核心稳定训练中应注重对腹横肌和多裂肌的训练[33]。 2.4 FAI患者髋关节镜术前和术后康复训练 2.4.1 术前康复训练 髋关节镜术前康复训练是改善FAI患者功能、减轻疼痛的重要手段。KIVLAN等[34]对1 738例髋关节镜患者进行调查发现,80%患者在术前选择进行康复治疗。FAI患者髋关节镜术前训练主要包括限制髋关节过度活动和功能性髋关节周围肌肌力训练[35-36],髋托佩戴可有效降低髋关节屈曲和外展角度,保护髋关节周围软组织[35]。NEWCOMB等[37]对25例FAI患者使用和不使用髋托在单腿下蹲、双腿下蹲、上下楼梯过程中进行运动学分析发现,佩戴髋托时患者髋关节屈曲、内旋、内收角度降低2°-6°,减少了功能性任务中髋部撞击。GUENTHER等[36]在髋关节镜术前10周对FAI患者进行康复训练,训练目的是无痛激活髋关节周围关键肌,改善神经控制,提高肌肉耐力和功能性肌力训练;主要训练项目有桥式运动、蛤壳运动、四点跪位髋关节外展、单腿平衡训练、下蹲和弓步训练、上下台阶、单腿跳跃,每个动作重复10-12次,每周训练三四次。10周后FAI患者髋外展肌肌力增加0.14 N?m/kg,髋内收和内旋肌肌力增加0.13 N?m/kg,HOOS量表中症状、僵硬、日常生活活动、娱乐及运动、疼痛评分较干预前显著提高(P < 0.02)。说明髋关节镜术前肌力训练和再教育可提高FAI患者临床疗效,同时FAI患者术前训练可有效解决腰盆-髋关节复合体内的肌肉失衡和抑制,破坏不利的运动模式[37]。但目前对于髋关节镜术前康复疗效和经济负担的研究较少,因此对于髋关节镜术前康复训练的经济效益有待进一步研究。 2.4.2 术后康复训练 (1)负重训练和支具使用:RATH等[38-39]对26例髋关节镜外科医生关于术后负重方案的调查研究显示,由于手术方案的不同,髋关节镜术后负重方案存在差异。65%的外科医生允许在唇部切除术后立即负重,38%的外科医生允许在唇部修复术后立即负重,其中20磅足底平坦部分负重最为常见;81%的外科医生建议在微骨折手术后3-8周内限制负重,对于软骨缺损手术,根据缺损面积和外侧中心边缘角的不同,建议6周或更长时间不负重。髋关节镜术后髋关节脚趾触摸或非负重等步态模式会导致跟腱和髋屈肌挛缩,引起下肢关节僵硬。 AVNIELI等 [40]对133例FAI患者髋关节镜术后负重情况进行2年随访研究,发现术后即刻负重组和非负重组改良Harris髋关节评分、主观改善率无明显差异(P > 0.1)。NHO等[41]研究表明,负重与非负重组患者髋关节镜术后2年结果指标无明显差异,但术后限制负重会影响FAI患者正常步态模式建立。 髋关节镜术后拐杖和防旋靴使用可有效维持患者部分负重状态[42],纠正异常步态,保护髋关节以及夜间保护作用[43-45]。CVETANOVICH等[45]对FAI患者髋关节镜术后康复方案可变性和全面性进行调查发现,54.8%的医生在髋关节镜术后选择使用支具,限制髋关节外展,支具使用时间为1-6周。 (2)手法治疗:FAI患者髋关节镜术后手法治疗可有效减轻髋部疼痛,增加关节活动度,主要训练项目有触发点治疗和关节松动术。触发点治疗可有效缓解肌肉紧张,减轻髋部疼痛,帮助改善髋关节的活动范围[46]。髋关节镜术后主要对髂腰肌、内收肌、臀中肌、阔筋膜张肌、腰方肌进行触发点治疗,每个触发点治疗时间为30-60 s[47-49]。骨盆松动术和腰椎松动术在髋关节镜术后2-8周内进行,每周3-5次,每次30-60 s,可有效增加腰盆髋复合体灵活性和无痛活动范围[47]。 (3)关节活动度训练:FAI患者髋关节镜术后1-3周应限制髋关节活动范围,屈曲不超过90°,外展和外旋不超过30°,内旋不超过20°,避免主动开链髋屈肌激活运动[49]。髋关节镜术后初期使用冰敷控制肿胀,减少疼痛和关节痉挛,避免深蹲、直腿抬高、长时间坐位动作引起髋屈肌痉挛[40,46];固定自行车训练和关节固定功能训练机应用于髋关节镜术后早期康复,可有效改善FAI患者术后早期被动关节活动度[46];髋关节镜术后4-6周逐渐恢复FAI患者全范围关节活动;水疗法通过浮力减轻下肢重力,改善髋关节活动度[40];四点跪位摆动练习有效牵拉髋关节前囊和后囊,增加髋关节屈伸活动范围[46]。除了髋关节活动度训练以外,踝关节、膝关节和腰背部关节活动度训练也应加入康复训练计划[40]。 (4)肌力训练:髋关节镜术后肌力训练包括髋关节周围肌肌力训练和核心肌肌力训练。FAI患者术后早期肌力训练方式为等长肌力训练,术后第1天立即进行臀肌、股四头肌、腹横肌等长肌力训练[40],臀肌等长训练可有效减轻髋屈肌和内收肌肌张力增加导致的髋前部疼痛,通过腹横肌训练增加躯干核心稳定性,增强对髋关节动态控制的能力。对于髋关节镜术后等张肌力训练时间,ENSEKI等[43]认为髋关节镜术后髋关节、骨盆、躯干周围肌肌力训练应在1周后进行,早期肌力训练应集中在深层核心肌肌力训练,有助于增加腰椎在转移和翻身运动中的稳定性;术后4-8周,肌力训练主要集中在股四头肌、腘绳肌和臀肌训练,训练方式是低阻力和高重复,其中臀中肌在控制骨盆额面稳定性、恢复FAI患者正常步态方面起着重要作用[48]。核心肌力训练可由单平面向多平面推进,稳定面向不稳定面进行训练[50]。 2.5 中医传统康复疗法 中医药是中华民族瑰宝,在治疗FAI方面发挥着积极作用。彭博文等[51]对60例FAI患者内服益肾祛痹汤联合超声电导药物与单纯内服益肾祛痹汤效果进行比较发现,治疗14 d后治疗组患者疼痛数字评分较治疗前降低,疼痛改善优于对照组(P < 0.05)。熊正容[52]将36例FAI患者分为2组,对照组给予红外线照射和口服活血化瘀药,治疗组在此基础上增加热奄包治疗,10 d后发现热奄包治疗可显著减轻患者疼痛,治疗组总有效率为94.4%,对照组有效率为72.2%(P < 0.05)。目前对于中医传统康复疗法治疗FAI的研究较少,但不难看出其在治疗FAI方面有一定的优势。 2.6 物理因子治疗 FAI的物理因子治疗主要有体外冲击波疗法、激光疗法、磁热疗法、超短波疗法,物理因子治疗具有消除关节炎症和肿胀、缓解关节疼痛、增加关节活动度作用。何健东等[53]将44例FAI患者随机分为体外冲击波组和口服塞来昔布胶囊组,体外冲击波组单次治疗冲击量为2 000次,时间间隔5-7 d,13周后发现FAI患者疼痛目测类比评分和髋关节Harris评分较治疗前显著改善(P < 0.05),但体外冲击波在缓解疼痛方面与口服塞来昔布胶囊无明显差异(P > 0.05)。LOPES等[54]采用真空疗法联合激光疗法治疗髋部疼痛患者,每周治疗2次,5周后发现髋关节屈曲、外展、内收关节活动度增加4°-10°,疼痛消失。吕雅[55]对髋关节镜手术失败患者采取银制毫针松解联合激光、磁热疗法、超短波疗法进行治疗,30 d后患者疼痛逐渐消失,功能逐渐恢复。对于FAI合并急性关节损伤时,温热疗法会加重局部反应,激光、超短波等非热效应治疗方法可有效消除炎症、缓解关节肿胀。单独的物理因子治疗FAI在临床康复中并不常见,治疗师多采用物理因子治疗与运动疗法相结合的方法,可有效缩短康复时间,提高康复疗效。 2.7 注射疗法 注射疗法是指在肌肉、神经、骨骼结构注射特定药物以减轻疼痛、改善功能的方法,FAI患者常用关节内注射药物有透明质酸钠和皮质类固醇,透明质酸钠具有增加关节润滑性和黏弹性,减少关节软骨磨损的作用。ABATE等[56]对20例FAI患者在基线和第40天进行超声引导下注射透明质酸钠,6个月后患者目测类比评分、髋关节Harris评分改善,消炎药使用量减少。LEE等[57]将30例FAI患者随机分为透明质酸钠组和皮质类固醇组,2周后通过疼痛数字评分量表进行评估,改善低于2分患者进行交叉注射;研究发现2周后无交叉注射患者中,透明质酸组HOOS评分较类固醇组显著改善(P < 0.05);交叉注射组、首次注射类固醇组疼痛数字评分较首次注射透明质酸钠组显著改善(P < 0.05);表明关节内药物注射可有效减轻FAI患者疼痛,改善髋关节功能。关节内注射透明质酸钠在改善患者功能方面作用更为明显,而关节内注射类固醇对于疼痛的改善效果更快。但KRYCH等 [58]对54例FAI患者进行关节内注射皮质类固醇,比较注射前、注射后麻醉期和注射后14 d FAI患者疼痛数字评分,发现FAI患者注射后麻醉期疼痛数字评分较注射前降低6分,注射14 d后疼痛数字评分增加4分,表明关节内注射皮质类固醇可在短期内减轻FAI患者髋部疼痛,长期疗效仍需进一步大样本量的研究。"

| [1] GRIFFIN DR, DICKENSON EJ, O’DONNELL J, et al. The Warwick Agreement on femoroacetabular impingement syndrome (FAI syndrome): an international consensus statement. Br J Sports Med. 2016;50:1169-1176. [2] SANKAR WN, NEVITT M, PARVIZI J, et al. Femoroacetabular Impingement: Defining the Condition and its Role in the Pathophysiology of Osteoarthritis. J Am Acad Orthop Surg. 2013;21 Suppl 1:S7-S15. [3] BRUNNER R, MAFFIULETTI NA, CASARTELLI NC, et al. Prevalence and Functional Consequences of Femoroacetabular Impingement in Young Male Ice Hockey Players.Am J Sports Med. 2016;44:46-53. [4] MASCARENHAS VV, REGO P, DANTAS P, et al. Imaging prevalence of femoroacetabular impingement in symptomatic patients, athletes, and asymptomatic individuals: A systematic review. Eur J Radiol. 2016;85:73-95. [5] MACK L, VANNATTA N, RASMUSSEN C, et al. Prevalence and Course of Treatment of Common Hip Diagnoses Presenting to a Sports Medicine Clinic. WMJ. 2019;118:65-70. [6] CHEN J, XU L, CHEN ZF, et al. Prevalence of radiographic parameters on CT associated with femoroacetabular impingement in a Chinese asymptomatic population. Acta Radiol. 2020;61(9):1213-1220. [7] EMARA K, SAMIR W, MOTASEM EL H, et al. Conservative treatment for mild femoroacetabular impingement. J Orthop Surg (Hong Kong). 2011;19:41-45. [8] CASARTELLI NC, BIZZINI M, KEMP J, et al. What treatment options exist for patients with femoroacetabular impingement syndrome but without surgical indication? Br J Sports Med. 2018;52:552-553. [9] CASARTELLI NC, MAFFIULETTI NA, ITEM-GLATTHORN JF, et al. Hip muscle weakness in patients with symptomatic femoroacetabular impingement. Osteoarthr Cartil. 2011;19:816-821. [10] NEPPLE JJ, GOLJAN P, BRIGGS KK, et al. Hip Strength Deficits in Patients With Symptomatic Femoroacetabular Impingement and Labral Tears. Arthroscopy. 2015;31:2106-2111. [11] RUTHERFORD DJ, MORESIDE J, WONG I. Differences in Hip Joint Biomechanics and Muscle Activation in Individuals With Femoroacetabular Impingement Compared With Healthy, Asymptomatic Individuals: Is Level-Ground Gait Analysis Enough? Orthop J Sports Med. 2018;6(5):2325967118769829. [12] MALLOY P, STONE AV, KUNZE KN, et al. Patients With Unilateral Femoroacetabular Impingement Syndrome Have Asymmetrical Hip Muscle Cross-Sectional Area and Compensatory Muscle Changes Associated With Preoperative Pain Level. Arthroscopy. 2019;35:1445-1453. [13] STRICKER PR, FAIGENBAUM AD, MCCAMBRIDGE TM, et al. Resistance Training for Children and Adolescents. Pediatrics. 2020;145:e20201011. [14] KEMP JL,COBURN SL,JONES DM, et al. The Physiotherapy for Femoroacetabular Impingement Rehabilitation Study (physioFIRST): A Pilot Randomized Controlled Trial. J Orthop Sports Phys Ther. 2018;48: 307-315. [15] CASARTELLI NC, BIZZINI M, MAFFIULETTI NA, et al. Exercise Therapy for the Management of Femoroacetabular Impingement Syndrome: Preliminary Results of Clinical Responsiveness. Arthritis Care Res (Hoboken). 2019;71:1074-1083. [16] ENSEKI K, HARRIS-HAYES M, WHITE DM, et al. Nonarthritic Hip Joint Pain. J Orthop Sports Phys Ther. 2014;44(6):A1-A32. [17] DRAOVITCH P, EDELSTEIN J, KELLY BT. The layer concept: utilization in determining the pain generators, pathology and how structure determines treatment. Curr Rev Musculoskelet Med. 2012;5(1):1-8. [18] DIAMOND LE, VAN DEN HW, BENNELL KL, et al. Coordination of deep hip muscle activity is altered in symptomatic femoroacetabular impingement. J Orthop Res. 2017;35:1494-1504. [19] DIAMOND LE, VAN DEN HW, BENNELL KL, et al. Deep hip muscle activation during squatting in femoroacetabular impingement syndrome.Clin Biomech (Bristol, Avon). 2019;69:141-147. [20] RETCHFORD TH, CROSSLEY KM, GRIMALDI A, et al. Can local muscles augment stability in the hip? A narrative literature review. J Musculoskelet Neuronal Interact. 2013;13(1):1-12. [21] 季程程,杨鹏飞,张信波,等.神经肌肉训练在前交叉韧带重建术后康复中的应用进展[J].中国康复理论与实践,2020,26(8):917-922. [22] MENDIS MD, HIDES JA. Effect of motor control training on hip muscles in elite football players with and without low back pain. J Sci Med Sport. 2016;19(11):866-871. [23] 王强,孙国栋,马金健,等.基于生物力学及本体感觉分析探讨运动控制训练在颈椎病防治中的应用[J].辽宁中医药大学学报, 2020,22(11):204-209. [24] NARVESON JR, HABERL MD, GRABOWSKI PJ. Management of a Patient With Acute Acetabular Labral Tear and Femoral Acetabular Impingement With Intra-articular Steroid Injection and a Neuromotor Training Program. J Orthop Sports Phys Ther. 2016;46(11):965-975. [25] KRYCH AJ, GRIFFITH TB, HUDGENS JL, et al. Limited therapeutic benefits of intra-articular cortisone injection for patients with femoro-acetabular impingement and labral tear. Knee Surg Sports Traumatol Arthrosc. 2014;22:750-755. [26] HARRIS-HAYES M , CZUPPON S , VAN DILLEN LR , et al. Movement Pattern Training To Improve Function in People With Chronic Hip Joint Pain: A Feasibility Randomized Clinic Trial. J Orthop Sports Phys Ther. 2016:1-48. [27] WILSON DA, BOOYSEN N, DAINESE P, et al. Accuracy of movement quality screening to document effects of neuromuscular control retraining exercises in a young ex-footballer with hip and groin symptoms: A proof of concept case study. Med Hypotheses. 2018;120:116-120. [28] BAGWELL JJ, POWERS CM. Persons with femoroacetabular impingement syndrome exhibit altered pelvifemoral coordination during weightbearing and non-weightbearing tasks. Clin Biomech (Bristol, Avon). 2019;65:51-56. [29] 刘芳,敖丽娟.核心肌稳定性训练对腰痛康复治疗的意义[J].中国康复医学杂志,2017,32(2):231-234. [30] CHAUDHARI AMW, VAN HORN MR, MONFORT SM, et al. Reducing Core Stability Influences Lower Extremity Biomechanics in Novice Runners. Med Sci Sports Exerc. 2020;52:1347-1353. [31] CHAN MK, CHOW KW, LAI AY, et al. The effects of therapeutic hip exercise with abdominal core activation on recruitment of the hip muscles. BMC Musculoskelet Disord. 2017;18:313. [32] AOYAMA M, OHNISHI Y, UTSUNOMIYA H, et al. A Prospective, Randomized, Controlled Trial Comparing Conservative Treatment With Trunk Stabilization Exercise to Standard Hip Muscle Exercise for Treating Femoroacetabular Impingement: A Pilot Study. Clin J Sport Med. 2019;29:267-275. [33] DAFKOU K, KELLIS E, ELLINOUDIS A, et al. The Effect of Additional External Resistance on Inter-Set Changes in Abdominal Muscle Thickness during Bridging Exercise. J Sports Sci Med. 2020;19:102-111. [34] KIVLAN BR, NHO SJ, CHRISTOFORETTI JJ, et al. Multicenter Outcomes After Hip Arthroscopy: Epidemiology (MASH Study Group). What Are We Seeing in the Office, and Who Are We Choosing to Treat? Am J Orthop. 2017;46:35-41. [35] DOMB BG, SGROI TA, VAN DEVENDER JC. Physical Therapy Protocol After Hip Arthroscopy: Clinical Guidelines Supported by 2-Year Outcomes. Sports Health. 2016;8:347-354. [36] GUENTHER JR, COCHRANE CK, CROSSLEY KM, et al. A Pre-Operative Exercise Intervention Can Be Safely Delivered to People with Femoroacetabular Impingement and Improve Clinical and Biomechanical Outcomes. Physiother Can. 2017;69:204-211. [37] NEWCOMB NRA, WRIGLEY TV, HINMAN RS, et al. Effects of a hip brace on biomechanics and pain in people with femoroacetabular impingement. J Sci Med Sport. 2018;21:111-116. [38] RATH E, SHARFMAN ZT, PARET M, et al. Hip arthroscopy protocol: expert opinions on post-operative weight bearing and return to sports guidelines. J Hip Preserv Surg. 2017;4:60-66. [39] ADLER KL, COOK PC, GEISLER PR, et al. Current Concepts in Hip Preservation Surgery: Part II--Rehabilitation.Sports Health. 2016;8:57-64. [40] AVNIELI IB, VIDRA M, FACTOR S, et al. Postoperative Weightbearing Protocols After Arthroscopic Surgery for Femoroacetabular Impingement Does Not Affect Patient Outcome: A Comparative Study With Minimum 2-Year Follow-up. Arthroscopy. 2020;36(1):159-164. [41] NHO S, RASIO J. Editorial Commentary: Rehabilitation After Hip Arthroscopy-Bear in Mind the Bearing of Weight. Arthroscopy. 2020; 36:165-166. [42] MCDONALD J, HERZOG MM, PHILIPPON MJ. Return to play after hip arthroscopy with microfracture in elite athletes. Arthroscopy. 2013;29:330-335. [43] ENSEKI KR, MARTIN R, KELLY BT. Rehabilitation after arthroscopic decompression for femoroacetabular impingement. Clin Sports Med. 2010;29:247-255,viii. [44] REIMAN MP, BOYD J, INGEL N, et al. There Is Limited and Inconsistent Reporting of Postoperative Rehabilitation for Femoroacetabular Impingement Syndrome: A Scoping Review of 169 Studies. J Orthop Sports Phys Ther. 2020;50:252-258. [45] CVETANOVICH GL, LIZZIO V, META F, et al. Variability and Comprehensiveness of North American Online Available Physical Therapy Protocols Following Hip Arthroscopy for Femoroacetabular Impingement and Labral Repair. Arthroscopy. 2017;33:1998-2005. [46] BENNELL KL, O’DONNELL JM, TAKLA A, et al. Efficacy of a physiotherapy rehabilitation program for individuals undergoing arthroscopic management of femoroacetabular impingement - the FAIR trial: a randomised controlled trial protocol. BMC Musculoskelet Disord. 2014; 15:58. [47] TIJSSEN M, VAN CINGEL REH, STAAL JB, et al. Physical therapy aimed at self-management versus usual care physical therapy after hip arthroscopy for femoroacetabular impingement: study protocol for a randomized controlled trial. Trials. 2016;17:91. [48] WAHOFF M, RYAN M. Rehabilitation after hip femoroacetabular impingement arthroscopy. Clin Sports Med. 2011;30(2):463-482. [49] KUHNS BD, WEBER AE, BATKO B, et al. A four-phase physical therapy regimen for returning athletes to sport following hip arthroscopy for femoroacetabular impingement with routine capsular closure. Int J Sports Phys Ther. 2017;12:683-696. [50] SPENCER-GARDNER L, EISCHEN JJ, LEVY BA, et al. A comprehensive five-phase rehabilitation programme after hip arthroscopy for femoroacetabular impingement. Knee Surg Sports Traumatol Arthrosc. 2014;22:848-859. [51] 彭博文,董晓俊.益肾祛痹汤联合超声电导药物透入治疗髋关节撞击综合征的临床研究[J].内蒙古中医药,2019,38(5):99-102. [52] 熊正容.中药热奄包治疗髋关节撞击综合的疗效观察[J]. 现代养生B, 2015,15(12):207-207. [53] 何健东,李明俊,梁笃.体外冲击波疗法治疗股骨髋臼撞击综合征的临床疗效观察[J].实用中西医结合临床,2016,16(5):11-13. [54] LOPES LAB, ALVAREZ C, CAMPOS TYTB, et al. Synergistic effects of vacuum therapy and laser therapy on physical rehabilitation. J Phys Ther Sci. 2019;31:598-602. [55] 吕雅.髋关节撞击综合征术后物理治疗的个案报告[J].中国疗养医学, 2018,27(10):1118-1119. [56] ABATE M, SCUCCIMARRA T, VANNI D, et al. Femoroacetabular impingement: is hyaluronic acid effective? Knee Surg Sports Traumatol Arthrosc. 2014;22:889-892. [57] LEE YK, LEE GY, LEE JW, et al. Intra-Articular Injections in Patients with Femoroacetabular Impingement: a Prospective, Randomized, Double-blind, Cross-over Study. J Korean Med Sci. 2016;31:1822-1827. [58] KRYCH AJ, GRIFFITH TB, HUDGENS JL, et al. Limited therapeutic benefits of intra-articular cortisone injection for patients with femoro-acetabular impingement and labral tear. Knee Surg Sports Traumatol Arthrosc. 2014;22:750-755. [59] EGGER AC, FRANGIAMORE S, ROSNECK J. Femoroacetabular Impingement: A Review. Sports Med Arthrosc Rev. 2016;24:e53-e58. [60] GRIFFIN DR, DICKENSON EJ, WALL PDH, et al. Hip arthroscopy versus best conservative care for the treatment of femoroacetabular impingement syndrome (UK FASHIoN): a multicentre randomised controlled trial. Lancet. 2018;391:2225-2235. [61] PENNOCK AT, BOMAR JD, JOHNSON KP, et al. Nonoperative Management of Femoroacetabular Impingement: A Prospective Study. Am J Sports Med. 2018;46:3415-3422. |
| [1] | Zhu Chan, Han Xuke, Yao Chengjiao, Zhou Qian, Zhang Qiang, Chen Qiu. Human salivary components and osteoporosis/osteopenia [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1439-1444. |
| [2] | Jin Tao, Liu Lin, Zhu Xiaoyan, Shi Yucong, Niu Jianxiong, Zhang Tongtong, Wu Shujin, Yang Qingshan. Osteoarthritis and mitochondrial abnormalities [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1452-1458. |
| [3] | Zhang Lichuang, Xu Hao, Ma Yinghui, Xiong Mengting, Han Haihui, Bao Jiamin, Zhai Weitao, Liang Qianqian. Mechanism and prospects of regulating lymphatic reflux function in the treatment of rheumatoid arthritis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1459-1466. |
| [4] | Wang Jing, Xiong Shan, Cao Jin, Feng Linwei, Wang Xin. Role and mechanism of interleukin-3 in bone metabolism [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(8): 1260-1265. |
| [5] | Zhu Chan, Han Xuke, Yao Chengjiao, Zhang Qiang, Liu Jing, Shao Ming. Acupuncture for Parkinson’s disease: an insight into the action mechanism in animal experiments [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(8): 1272-1277. |
| [6] | An Weizheng, He Xiao, Ren Shuai, Liu Jianyu. Potential of muscle-derived stem cells in peripheral nerve regeneration [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1130-1136. |
| [7] | Fan Yiming, Liu Fangyu, Zhang Hongyu, Li Shuai, Wang Yansong. Serial questions about endogenous neural stem cell response in the ependymal zone after spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1137-1142. |
| [8] | Guo Jia, Ding Qionghua, Liu Ze, Lü Siyi, Zhou Quancheng, Gao Yuhua, Bai Chunyu. Biological characteristics and immunoregulation of exosomes derived from mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1093-1101. |
| [9] | Wu Weiyue, Guo Xiaodong, Bao Chongyun. Application of engineered exosomes in bone repair and regeneration [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1102-1106. |
| [10] | Zhou Hongqin, Wu Dandan, Yang Kun, Liu Qi. Exosomes that deliver specific miRNAs can regulate osteogenesis and promote angiogenesis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1107-1112. |
| [11] | Zhang Jinglin, Leng Min, Zhu Boheng, Wang Hong. Mechanism and application of stem cell-derived exosomes in promoting diabetic wound healing [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1113-1118. |
| [12] | Huang Chenwei, Fei Yankang, Zhu Mengmei, Li Penghao, Yu Bing. Important role of glutathione in stemness and regulation of stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1119-1124. |
| [13] | Hui Xiaoshan, Bai Jing, Zhou Siyuan, Wang Jie, Zhang Jinsheng, He Qingyong, Meng Peipei. Theoretical mechanism of traditional Chinese medicine theory on stem cell induced differentiation [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1125-1129. |
| [14] | Xu Lei, Han Xiaoqiang, Zhang Jintao, Sun Haibiao. Hyaluronic acid around articular chondrocytes: production, transformation and function characteristics [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(5): 768-773. |
| [15] | Li Jiajun, Xia Tian, Liu Jiamin, Chen Feng, Chen Haote, Zhuo Yinghong, Wu Weifeng. Molecular mechanism by which icariin regulates osteogenic signaling pathways in the treatment of steroid-induced avascular necrosis of the femoral head [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(5): 780-785. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||