[1] RACINE HL, SERRAT MA. The Actions of IGF-1 in the Growth Plate and Its Role in Postnatal Bone Elongation. Curr Osteoporos Rep. 2020; 18(3):210-227.
[2] AGIRDIL Y. The growth plate: a physiologic overview. EFORT Open Rev. 2020;5(8):498-507.
[3] MATSUSHITA Y, ONO W, ONO N. Growth plate skeletal stem cells and their transition from cartilage to bone. Bone. 2020;136:115359.
[4] HUNZIKER EB. Elongation of the Long Bones in Humans by the Growth Plates. Nestle NutrInst Workshop Ser. 2018;89:13-23.
[5] MIZUHASHI K, ONO W, MATSUSHITA Y, et al. Resting zone of the growth plate houses a unique class of skeletal stem cells. Nature. 2018;563 (7730):254-258.
[6] SHAW N, ERICKSON C, BRYANT SJ, et al. Regenerative Medicine Approaches for the Treatment of Pediatric Physeal Injuries. Tissue Eng Part B Rev. 2018;24(2):85-97.
[7] EID AM, HAFEZ MA. Traumatic injuries of the distal femoral physis.Retrospective study on 151 cases.Injury. 2002;33(3):251-255.
[8] 陈劲松,王中汉,常非,等.多种特殊状态下关节软骨缺损修复的组织工程技术[J].中国组织工程研究,2020,24(8):1272-1279.
[9] SALTER RB, HARRIS WR. Injuries involving the epiphyseal plate. J Bone Joint Surg Am. 2001;83a(11):1753-1753.
[10] SYURAHBIL AH, MUNAJAT I, MOHD EF, et al. Displaced Physeal and Metaphyseal Fractures of Distal Radius in Children. Can Wire Fixation Achieve Better Outcome at Skeletal Maturity than Cast Alone? Malays Orthop J. 2020;14(2):28-38.
[11] BELLAMY JT, WARD LA, FLETCHER ND. Evaluation of pediatric distal femoral physeal fractures and the factors impacting poor outcome requiring further corrective surgery. J PediatrOrthop B. 2020. doi: 10.1097/BPB.0000000000000733.
[12] STENROOS A, PUHAKKA J, JALKANEN J, et al. Risk of premature physeal closure in fractures of distal tibia. J Pediatr Orthop B. 2020. doi: 10.1097/BPB.0000000000000744.
[13] SHALABY-RANA E, HINDS TS, DEYE K, et al. Proximal femoral physeal fractures in children: a rare abusive injury. PediatrRadiol. 2020;50(8): 1115-1122.
[14] BADINA A, VIALLE R, FITOUSSI F, et al. Case reports: Treatment of traumatic triradiate cartilage epiphysiodesis: what is the role of bridge resection? Clin Orthop Relat Res. 2013;471(11):3701-3705.
[15] DAS P, SINGH YP, MANDAL BB, et al. Tissue-derived decellularized extracellular matrices toward cartilage repair and regeneration. Methods Cell Biol. 2020;157:185-221.
[16] UZ U, GUNHAN K, VATANSEVER S, et al. Novel Simple Strategy for Cartilage Tissue Engineering Using Stem Cells and Synthetic Polymer Scaffold. J Craniofac Surg. 2019;30(3):940-943.
[17] CHEN L, LIU J, GUAN M, et al. Growth Factor and Its Polymer Scaffold-Based Delivery System for Cartilage Tissue Engineering. Int J Nanomedicine. 2020;15:6097-6111.
[18] MATAI I, KAUR G, SEYEDSALEHI A, et al. Progress in 3D bioprinting technology for tissue/organ regenerative engineering. Biomaterials. 2020;226:119536.
[19] ZHAO ZY, FAN CJ, CHEN F, et al. Progress in Articular Cartilage Tissue Engineering: A Review on Therapeutic Cells and Macromolecular Scaffolds. Macromol Biosci. 2020;20(2):1900278.
[20] SABHARWAL S, SABHARWAL S. Growth Plate Injuries of the Lower Extremity: Case Examples and Lessons Learned. Indian J Orthop. 2018;52(5):462-469.
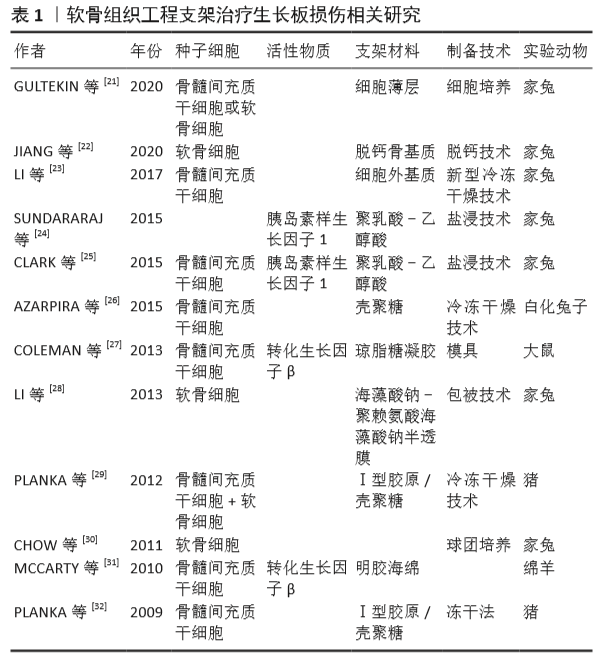
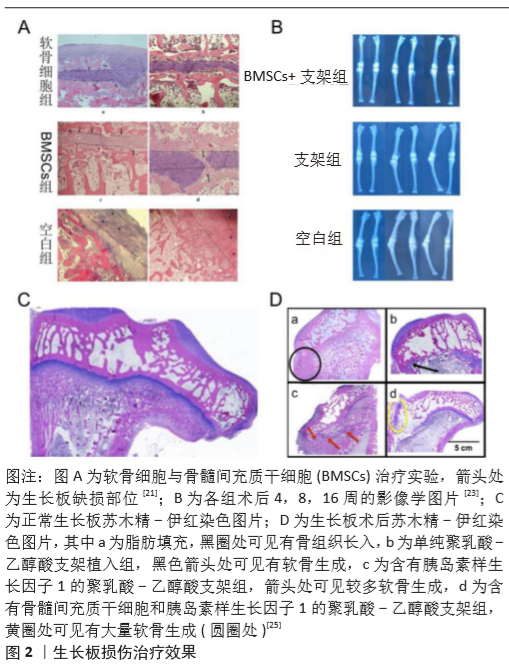
[21] GULTEKIN A, AGIRDIL Y, ONCEL DUMAN B, et al. Comparison of mesenchymal stem cell sheets and chondrocyte sheets in a rabbit growth plate injury model. Turk J Med Sci. 2020;50(4):1082-1096.
[22] JIANG F, QIAO F, HU H, et al. Early Closure of Growth Plate Due to Avascular Necrosis of the Femoral Head After Displaced Fracture of the Femoral Neck in Children. Nanosci Nanotech Let. 2020;12(1):34-38.
[23] LI WC, XU RJ, HUANG JX, et al. Treatment of rabbit growth plate injuries with oriented ECM scaffold and autologous BMSCs. Sci Rep. 2017;7:44140.
[24] SUNDARARAJ SKC, CIEPLY RD, GUPTA G, et al. Treatment of growth plate injury using IGF-I-loaded PLGA scaffolds. J Tissue EngRegen Med. 2015;9(12):E202-E209.
[25] CLARK A, HILT JZ, MILBRANDT TA, et al. Treating Proximal Tibial Growth Plate Injuries Using Poly(Lactic-co-Glycolic Acid) Scaffolds. Biores Open Access. 2015;4(1):65-74.
[26] AZARPIRA MR, SHAHCHERAGHI GH, AYATOLLAHI M, et al. Tissue engineering strategy usingmesenchymal stem cell-based chitosan scafolds in growth plate surgery: a preliminary study in rabbits. Orthop Traumatol Surg Res. 2015;101(5):601-605.
[27] COLEMAN RM, SCHWARTZ Z, BOYAN BD, et al. The Therapeutic Effect of Bone Marrow-Derived Stem Cell Implantation After Epiphyseal Plate Injury Is Abrogated by Chondrogenic Predifferentiation. Tissue Eng Part A. 2013;19(3-4):475-483.
[28] LI WC, XU RJ, XUE YL, et al. Treatment of growth plate injury with microencapsulated chondrocytes.Biotechnol Bioprocess Eng. 2013; 18(4):655-662.
[29] PLANKA L, SRNEC R, RAUSER P, et al. Nanotechnology and mesenchymal stem cells with chondrocytes in prevention of partial growth plate arrest in pigs. Biomed Pap Med FacUnivPalacky Olomouc Czech Repub. 2012;156(2):128-134.
[30] CHOW SKH, LEE KM, QIN L, et al. Restoration of longitudinal growth by bioengineered cartilage pellet in physeal injury is not affected by low intensity pulsed ultrasound. J Biomed Mater Res B ApplBiomater. 2011;99(1):36-44.
[31] MCCARTY RC, XIAN CJ, GRONTHOS S, et al. Application of autologous bone marrow derived mesenchymal stem cells to an ovine model of growth plate cartilage injury. Open Orthop J. 2010;4:204-210.
[32] PLANKA L, STARY D, HLUCILOVA J, et al. Comparison of Preventive and Therapeutic Transplantations of Allogeneic Mesenchymal Stem Cells in Healing of the Distal Femoral Growth Plate Cartilage Defects in Miniature Pigs. Acta Vet Brno. 2009;78(2):293-U122.
[33] CHOI JR, YONG KW, CHOI JY. Effects of mechanical loading on human mesenchymal stem cells for cartilage tissue engineering. J Cell Physiol. 2018;233(3):1913-1928.
[34] ISOBE Y, KOYAMA N, NAKAO K, et al. Comparison of human mesenchymal stem cells derived from bone marrow, synovial fluid, adult dental pulp, and exfoliated deciduous tooth pulp. Int J Oral Maxillofac Surg. 2016;45(1):124-131.
[35] KHALILIFAR MA, ESLAMINEJAD MB, GHASEMZADEH M, et al. In Vitro and In Vivo Comparison of Different Types of Rabbit Mesenchymal Stem Cells for Cartilage Repair. Cell J. 2019;21(2):150-160.
[36] CONTENTIN R, DEMOOR M, CONCARI M, et al. Comparison of the Chondrogenic Potential of Mesenchymal Stem Cells Derived from Bone Marrow and Umbilical Cord Blood Intended for Cartilage Tissue Engineering. Stem Cell Rev Rep. 2020;16(1):126-143.
[37] CARON MM, EMANS PJ, COOLSEN MM, et al. Redifferentiation of dedifferentiated human articular chondrocytes: comparison of 2D and 3D cultures. Osteoarthritis Cartilage. 2012;20(10):1170-1178.
[38] HAMAMOTO S, CHIJLMATSU R, SHIMOMURA K, et al. Enhancement of chondrogenic differentiation supplemented by a novel small compound for chondrocyte-based tissue engineering. J Exp Orthop. 2020;7(1):10.
[39] LEE SU, LEE JY, JOO SY, et al. Transplantation of a Scaffold-Free Cartilage Tissue Analogue for the Treatment of Physeal Cartilage Injury of the Proximal Tibia in Rabbits. Yonsei Med J. 2016;57(2):441-448.
[40] TOMASZEWSKI R, BOHOSIEWICZ J, GAP A, et al. Autogenous cultured growth plate chondrocyte transplantation in the treatment of physeal injury in rabbits. Bone Joint Res. 2014;3(11):310-316.
[41] CHEN MJ, WHITELEY JP, PLEASE CP, et al. Inducing chondrogenesis in MSC/chondrocyte co-cultures using exogenous TGF-β: a mathematical model. J Theor Biol. 2018;439:1-13.
[42] THIELEN NGM, VAN DER KRAAN PM, VAN CAAM APM.TGFbeta/BMP Signaling Pathway in Cartilage Homeostasis.Cells. 2019;8(9):969.
[43] GRAFE I, ALEXANDEr S, PETERSON JR, et al. TGF-beta Family Signaling in Mesenchymal Differentiation. Cold Spring Harb Perspect Biol. 2018; 10(5):a022202.
[44] ROTHWEILER R, BASOLI V, DUTTENHOEFER F, et al. Predicting and Promoting Human Bone Marrow MSC Chondrogenesis by Way of TGFbeta Receptor Profiles: Toward Personalized Medicine. Front Bioeng Biotechnol. 2020;8:618.
[45] WANG W, RIGUEUR D, LYONS KM. TGFbeta as a gatekeeper of BMP action in the developing growth plate.Bone. 2020;137:115439.
[46] CHEN X, ZHANG RH, ZHANG Q, et al. Microtia patients: Auricular chondrocyte ECM is promoted by CGF through IGF-1 activation of the IGF-1R/PI3K/AKT pathway. J Cell Physiol. 2019;234(12):21817-21824.
[47] HEILIG J, PAULSSON M, ZAUCKE F. Lack of the chondrocyte IGF-I receptor leads to perinatal death and alterations in extracellular matrix protein expression in vitro. Bone. 2012;50:S64-S64.
[48] LUI JC, NILSSON O, BARON J. Recent research on the growth plate: Recent insights into the regulation of the growth plate. J MolEndocrinol. 2014;53(1):T1-T9.
[49] COLEMAN RM, CASE ND, GULDBERG RE. Hydrogel effects on bone marrow stromal cell response to chondrogenic growth factors. Biomaterials. 2007;28(12):2077-2086.
[50] CUNNIFFE GM, DIAZ-PAYNO PJ, RAMEY JS, et al. Growth plate extracellular matrix-derived scaffolds for large bone defect healing. Eur Cell Mater. 2017;33:130-142.
[51] SINGH YP, BHARDWAJ N, MANDAL BB. Potential of Agarose/Silk Fibroin Blended Hydrogel for in Vitro Cartilage Tissue Engineering. ACS Appl Mater Interfaces. 2016;8(33):21236-21249.
[52] BONHOME-ESPINOSA AB, CAMPOS F, DURAND-HERRERA D, et al.In vitro characterization of a novel magnetic fibrin-agarose hydrogel for cartilage tissue engineering. J Mech Behav Biomed Mater. 2020; 104:103619.
[53] CHEN F, HUI JH, CHAN WK, et al. Cultured mesenchymalstem cell transfers in the treatment of partial growth arrest. J Pediatr Orthop. 2003;23(4):425-429.
[54] CAMPOS F, BONHOME-ESPINOSA AB, CHATO-ASTRAIN J, et al. Evaluation of Fibrin-Agarose Tissue-Like Hydrogels Biocompatibility for Tissue Engineering Applications. Front Bioeng Biotechnol. 2020;8:596.
[55] SHAMEKHI MA, RABIEE A, MIRZADEH H, et al. Fabrication and characterization of hydrothermal cross-linked chitosan porous scaffolds for cartilage tissue engineering applications. Mater Sci Eng C Mater Biol Appl. 2017;80:532-542.
[56] [56]DEHGHAN-BANIANI D, CHEN Y, WANG D, et al. Injectable in situ forming kartogenin-loaded chitosan hydrogel with tunable rheological properties for cartilage tissue engineering. Colloids Surf B Biointerfaces. 2020;192:111059.
[57] SADEGHIANMARYAN A, NAGHIEH S, SARDROUD HA, et al. Extrusion-based printing of chitosan scaffolds and their in vitro characterization for cartilage tissue engineering. Int J Biol Macromol. 2020;164:3179-3192.
[58] WEI P, XU Y, GU Y, et al. IGF-1-releasing PLGA nanoparticles modified 3D printed PCL scaffolds for cartilage tissue engineering. Drug Deliv. 2020;27(1):1106-1114.
[59] CHOU SF, WOODROW KA. Relationships between mechanical properties and drug release from electrospun fibers of PCL and PLGA blends. J Mech Behav Biomed Mater. 2017;65:724-733.
[60] ABID Z, DALSKOV MOSGAARD M, MANFRONI G, et al. Investigation of Mucoadhesion and Degradation of PCL and PLGA Microcontainers for Oral Drug Delivery. Polymers (Basel). 2019;11(11):1828.
[61] MACHATSCHEK R, LENDLEIN A. Fundamental insights in PLGA degradation from thin film studies. J Control Release. 2020;319:276-284.
[62] STEFANI RM, LEE AJ, TAN AR, et al. Sustained low-dose dexamethasone delivery via a PLGA microsphere-embedded agarose implant for enhanced osteochondral repair. Acta Biomater. 2020;102:326-340.
[63] BOUKARI Y, QUTACHI O, SCURR DJ, et al.A dual-application poly (dl-lactic-co-glycolic) acid (PLGA)-chitosan composite scaffold for potential use in bone tissue engineering. J Biomater Sci Polym Ed. 2017;28(16):1966-1983.
[64] 赵守军,熊文化,许柯.细胞因子基因转染的骨骺干细胞复合明胶-硫酸软骨素-透明质酸钠支架修复大鼠骨骺生长板缺损的实验研究[J].中医正骨,2018,30(2):10-15.
[65] 徐真然,罗飞宏.生长板的局部调控新进展[J].医学综述,2018, 24(19):3772-3776.
|