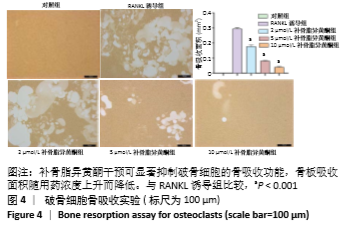
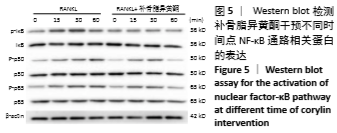
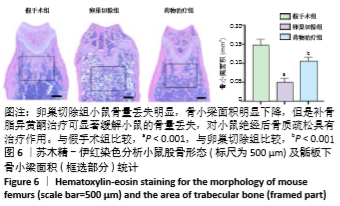
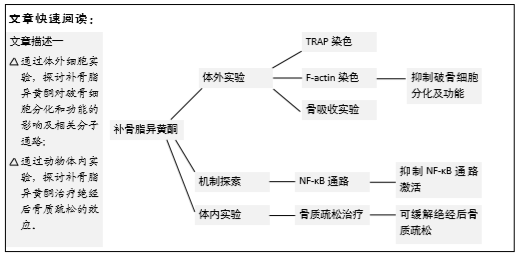
|
[1] SIMS NA, MARTIN TJ. Osteoclasts Provide Coupling Signals to Osteoblast Lineage Cells Through Multiple Mechanisms. Annu Rev Physiol. 2020;82:507-529.
[2] HUANG J, LIN D, WEI Z, et al. Parathyroid Hormone Derivative with Reduced Osteoclastic Activity Promoted Bone Regeneration via Synergistic Bone Remodeling and Angiogenesis. Small. 2020;16(6):e1905876.
[3] HASEGAWA T, KIKUTA J, SUDO T, et al. Identification of a novel arthritis-associated osteoclast precursor macrophage regulated by FoxM1. Nat Immunol. 2019;20(12):1631-1643.
[4] SIPILÄ S, TÖRMÄKANGAS T, SILLANPÄÄ E, et al. Muscle and bone mass in middle-aged women: role of menopausal status and physical activity. J Cachexia Sarcopenia Muscle. 2020 Feb 3. doi: 10.1002/jcsm.12547. [Epub ahead of print]
[5] DE MARTINIS M, SIRUFO MM, GINALDI L. Osteoporosis: Current and emerging therapies targeted to immunological checkpoints. Curr Med Chem. 2019 Jul 30. doi: 10.2174/0929867326666190730113123. [Epub ahead of print]
[6] RUCHLEMER R, AMIT-KOHN M, TVITO A, et al. Bone loss and hematological malignancies in adults: a pilot study. Support Care Cancer. 2018;26(9):3013-3020.
[7] ZEBIC L, PATEL V. Preventing medication-related osteonecrosis of the jaw. BMJ. 2019;365:l1733.
[8] MCCLUNG MR, O’DONOGHUE ML, PAPAPOULOS SE, et al. Odanacatib for the treatment of postmenopausal osteoporosis: results of the LOFT multicentre, randomised, double-blind, placebo-controlled trial and LOFT Extension study. Lancet Diabetes Endocrinol. 2019;7(12):899-911.
[9] VELETIC I, MANSHOURI T, MULTANI AS, et al. Myelofibrosis osteoclasts are clonal and functionally impaired. Blood. 2019;133(21):2320-2324.
[10] OIKAWA T, OYAMA M, KOZUKA-HATA H, et al. Tks5-dependent formation of circumferential podosomes/invadopodia mediates cell-cell fusion. J Cell Biol. 2012;197(4):553-568.
[11] MA QL, FANG L, JIANG N, et al. Bone mesenchymal stem cell secretion of sRANKL/OPG/M-CSF in response to macrophage-mediated inflammatory response influences osteogenesis on nanostructured Ti surfaces. Biomaterials. 2018;154:234-247.
[12] KWON OC, CHOI B, LEE EJ, et al. Negative Regulation of Osteoclast Commitment by Intracellular Protein Phosphatase Magnesium-Dependent 1A. Arthritis Rheumatol. 2020;72(5):750-760.
[13] ETHIRAJ P, OTTINGER AM, SINGH T, et al. Proteasome inhibition suppress microgravity elevated RANK signaling during osteoclast differentiation. Cytokine. 2020;125:154821.
[14] LEE NK, CHOI YG, BAIK JY, et al. A crucial role for reactive oxygen species in RANKL-induced osteoclast differentiation. Blood. 2005;106(3):852-859.
[15] 林瑞民,王大为,熊志立,等.补骨脂中两个黄酮类成分的高效液相色谱测定[J].中国中药杂志,2002,27(9): 669-671.
[16] KLOTZ LH, MCNEILL IY, KEBABDJIAN M, et al. A phase 3, double-blind, randomised, parallel-group, placebo-controlled study of oral weekly alendronate for the prevention of androgen deprivation bone loss in nonmetastatic prostate cancer: the Cancer and Osteoporosis Research with Alendronate and Leuprolide (CORAL) study. Eur Urol. 2013;63(5):927-935.
[17] YU AX, XU ML, YAO P, et al. Corylin, a flavonoid derived from Psoralea Fructus, induces osteoblastic differentiation via estrogen and Wnt/β-catenin signaling pathways. FASEB J. 2020;34(3):4311-4328.
[18] XIN Z, JIN C, CHAO L, et al. A Matrine Derivative M54 Suppresses Osteoclastogenesis and Prevents Ovariectomy-Induced Bone Loss by Targeting Ribosomal Protein S5. Front Pharmacol. 2018;9:22.
[19] CHEN X, ZHI X, WANG J, et al. RANKL signaling in bone marrow mesenchymal stem cells negatively regulates osteoblastic bone formation. Bone Res. 2018;6:34.
[20] CHELLAIAH MA, MOORER MC, MAJUMDAR S, et al. L-Plastin deficiency produces increased trabecular bone due to attenuation of sealing ring formation and osteoclast dysfunction. Bone Res. 2020;8:3.
[21] COLEMAN R, BODY JJ, AAPRO M, et al. Bone health in cancer patients: ESMO Clinical Practice Guidelines. Ann Oncol. 2014;25 Suppl 3:iii124-37.
[22] CAPOZZI A, LELLO S, PONTECORVI A. The inhibition of RANK-ligand in the management of postmenopausal osteoporosis and related fractures: the role of denosumab. Gynecol Endocrinol. 2014;30(6):403-408.
[23] XU R, YALLOWITZ A, QIN A, et al. Targeting skeletal endothelium to ameliorate bone loss. Nat Med. 2018;24(6):823-833.
[24] LEUTNER M, MATZHOLD C, BELLACH L, et al. Diagnosis of osteoporosis in statin-treated patients is dose-dependent. Ann Rheum Dis. 2019;78(12):1706-1711.
[25] RODAN GA, MARTIN TJ. Therapeutic approaches to bone diseases. Science. 2000;289(5484):1508-1514.
[26] 孙燕.中医中药在肿瘤综合治疗中的应用[J].中国中西医结合杂志,1997, 17(6):323-324.
[27] HUANG MY, TU CE, WANG SC, et al. Corylin inhibits LPS-induced inflammatory response and attenuates the activation of NLRP3 inflammasome in microglia. BMC Complement Altern Med. 2018;18(1):221.
[28] CHEN CY, CHEN CC, SHIEH TM, et al. Corylin Suppresses Hepatocellular Carcinoma Progression via the Inhibition of Epithelial-Mesenchymal Transition, Mediated by Long Noncoding RNA GAS5. Int J Mol Sci. 2018;19(2): E380.
[29] CHEN CC, CHEN CY, UENG SH, et al. Corylin increases the sensitivity of hepatocellular carcinoma cells to chemotherapy through long noncoding RNA RAD51-AS1-mediated inhibition of DNA repair. Cell Death Dis. 2018;9(5):543.
[30] CHELLAIAH MA, MA T, MAJUMDAR S. L-plastin phosphorylation regulates the early phase of sealing ring formation by actin bundling process in mouse osteoclasts. Exp Cell Res. 2018;372(1):73-82.
[31] TANG Y, WU X, LEI W, et al. TGF-beta1-induced migration of bone mesenchymal stem cells couples bone resorption with formation. Nat Med. 2009;15(7): 757-765.
[32] CHENG C, WENTWORTH K, SHOBACK DM. New Frontiers in Osteoporosis Therapy. Annu Rev Med. 2020;71:277-288.
[33] SANCAR F. Caution With New Osteoporosis Drug. JAMA. 2019;321(19):1862.
[34] HODSMAN AB, BAUER DC, DEMPSTER DW, et al. Parathyroid hormone and teriparatide for the treatment of osteoporosis: a review of the evidence and suggested guidelines for its use. Endocr Rev. 2005;26(5):688-703.
[35] MCCLUNG MR. Clinical utility of anti-sclerostin antibodies. Bone. 2017;96:3-7.
[36] CLINE-SMITH A, AXELBAUM A, SHASHKOVA E, et al. Ovariectomy Activates Chronic Low-Grade Inflammation Mediated by Memory T Cells, Which Promotes Osteoporosis in Mice. J Bone Miner Res. 2020 Jan 29. doi: 10.1002/jbmr.3966. [Epub ahead of print] |