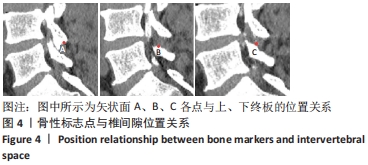
[1] ISSACK PS, CUNNINGHAM ME, PUMBERGER M, et al. Degenerative lumbar spinal stenosis: evaluation and management. J Am Acad Orthop Surg. 2012; 20(8):527-535.
[2] SCHROEDER GD, KURD MF, VACCARO AR. Lumbar spinal stenosis:how is it classified? J Am Acad Orthop Surg. 2016;24(12):843-852.
[3] KATZ JN, HARRIS MB. Clinical practice. Lumbar spinal stenosis. N Engl J Med. 2008;358(8):818-825.
[4] ARABMOTLAGH M, SELLEI RM, VINAS-RIOS JM, et al. Klassifikation und Diagnostik der lumbalen Spinalkanalstenose [Classification and diagnosis of lumbar spinal stenosis]. Orthopade. 2019;48(10):816-823.
[5] WEINSTEIN JN, TOSTESON TD, LURIE JD, et al. Surgical versus nonoperative treatment for lumbar spinal stenosis four-year results of the Spine Patient Outcomes Research Trial. Spine (Phila Pa 1976). 2010;35(14):1329-1338.
[6] ZAINA F, TOMKINS-LANE C, CARRAGEE E, et al. Surgical versus non-surgical treatment for lumbar spinal stenosis. Cochrane Database Syst Rev. 2016;2016(1):CD010264.
[7] BAGLEY C, MACALLISTER M, DOSSELMAN L, et al. Current concepts and recent advances in understanding and managing lumbar spine stenosis. F1000Res. 2019;8:F1000 Faculty Rev-137.
[8] SHIMIZU T, KATO S, DEMURA S, et al. The efficacy of surgical treatment on locomotive syndrome and physical function in patients with lumbar spinal canal stenosis. J Orthop Sci. 2021;26(3):327-331.
[9] KIM N, JUNG SB. Percutaneous Unilateral Biportal Endoscopic Spine Surgery Using a 30-Degree Arthroscope in Patients With Severe Lumbar Spinal Stenosis: A Technical Note. Clin Spine Surg. 2019;32(8):324-329.
[10] KIM JE, CHOI DJ. Unilateral biportal endoscopic decompression by 30° endoscopy in lumbar spinal stenosis: Technical note and preliminary report. J Orthop. 2018;15(2):366-371.
[11] KIM JE, CHOI DJ. Unilateral Biportal Endoscopic Spinal Surgery Using a 30° Arthroscope for L5-S1 Foraminal Decompression. Clin Orthop Surg. 2018; 10(4):508-512.
[12] 朱斌,田大胜,陈磊,等.单边双通道内镜技术在腰椎疾病中的应用研究进展[J].中华骨科杂志,2020,40(15):1030-1038.
[13] 许斌,何鹏.单侧双通道脊柱内镜技术的临床应用[J].医学研究生学报, 2020,33(10):1009-1013.
[14] HEO DH, LEE DC, PARK CK. Comparative analysis of three types of minimally invasive decompressive surgery for lumbar central stenosis: biportal endoscopy, uniportal endoscopy, and microsurgery. Neurosurg Focus. 2019; 46(5):E9.
[15] PRANATA R, LIM MA, VANIA R, et al. Biportal Endoscopic Spinal Surgery versus Microscopic Decompression for Lumbar Spinal Stenosis: A Systematic Review and Meta-Analysis. World Neurosurg. 2020;138:e450-e458.
[16] LIN GX, HUANG P, KOTHEERANURAK V, et al. A Systematic Review of Unilateral Biportal Endoscopic Spinal Surgery: Preliminary Clinical Results and Complications. World Neurosurg. 2019;125:425-432.
[17] 王彬,何鹏,武振方,等.单侧双通道内镜手术与显微内镜手术治疗腰椎管狭窄症的Meta分析[J].中国脊柱脊髓杂志,2021,31(8):719-730.
[18] HEO DH, LEE N, PARK CW, et al. Endoscopic Unilateral Laminotomy with Bilateral Discectomy Using Biportal Endoscopic Approach: Technical Report and Preliminary Clinical Results. World Neurosurg. 2020;137:31-37.
[19] KIM JE, CHOI DJ, PARK EJJ, et al. Biportal Endoscopic Spinal Surgery for Lumbar Spinal Stenosis. Asian Spine J. 2019;13(2):334-342.
[20] KIM SK, KANG SS, HONG YH, et al. Clinical comparison of unilateral biportal endoscopic technique versus open microdiscectomy for single-level lumbar discectomy: a multicenter, retrospective analysis. J Orthop Surg Res. 2018; 13(1):22.
[21] PAO JL, LIN SM, CHEN WC, et al. Unilateral biportal endoscopic decompression for degenerative lumbar canal stenosis. J Spine Surg. 2020; 6(2):438-446.
[22] 田大胜,刘建军,朱斌,等.单边双通道内镜技术治疗腰椎间盘突出症和腰椎椎管狭窄症[J].中华骨科杂志,2020,40(17):1155-1164.
[23] 庹伟,周霖,刘德森,等.单侧双通道内镜技术治疗腰椎管狭窄的初步研究[J].中国微创外科杂志,2021,21(1):56-60.
[24] YAO J, DONG B, SUN J, et al. Accuracy and Reliability of Computer-aided Anatomical Measurements for Vertebral Body and Disc Based on Computed Tomography Scans. Orthop Surg. 2020;12(4):1182-1189.
[25] CHEN YT, WANG MS. Three-dimensional reconstruction and fusion for multi-modality spinal images. Comput Med Imaging Graph. 2004;28(1-2):21-31.
[26] PARK SM, KIM GU, KIM HJ, et al. Is the Use of a Unilateral Biportal Endoscopic Approach Associated with Rapid Recovery After Lumbar Decompressive Laminectomy? A Preliminary Analysis of a Prospective Randomized Controlled Trial. World Neurosurg. 2019;128:e709-e718.
[27] MIN WK, KIM JE, CHOI DJ, et al. Clinical and radiological outcomes between biportal endoscopic decompression and microscopic decompression in lumbar spinal stenosis. J Orthop Sci. 2020;25(3):371-378.
[28] ITO Z, SHIBAYAMA M, NAKAMURA S, et al. Clinical Comparison of Unilateral Biportal Endoscopic Laminectomy versus Microendoscopic Laminectomy for Single-Level Laminectomy: A Single-Center, Retrospective Analysis. World Neurosurg. 2021;148:e581-e588.
[29] FENG Q, ZHANG L, ZHANG M, et al. Morphological parameters of fourth lumbar spinous process palpation: a three-dimensional reconstruction of computed tomography. J Orthop Surg Res. 2020;15(1):227.
[30] DING B, ZHOU T, ZHAO J. A novel system for accurate lumbar spine pedicle screw placement based on three-dimensional computed tomography reconstruction. J Orthop Translat. 2020;23:101-106.
[31] RAN B, LI Q, YU B, et al. Morphometry of lumbar spinous process via three dimensional CT reconstruction in a Chinese population. Int J Clin Exp Med. 2015;8(1):1129-1136.
[32] XU C, HOU Q, CHU Y, et al. How to improve the safety of bicortical pedicle screw insertion in the thoracolumbar vertebrae: analysis base on three-dimensional CT reconstruction of patients in the prone position. BMC Musculoskelet Disord. 2020;21(1):444.
[33] DAI JH, YU ZX, LI X, et al. Morphometric measurement of lower lumbar intervertebral foramina based on digital three-dimensional simulation. Turk Neurosurg. 2020;10.5137/1019-5149.JTN.29654-20.2.
[34] 丁宇,张建军,崔洪鹏,等.精准定位经皮全内镜椎板开窗减压术治疗腰椎管狭窄症[J].中国骨伤,2019,32(10):941-946.
[35] LØNNE G, CHA TD. Minimally Invasive Decompression in Lumbar Spinal Stenosis. JBJS Essent Surg Tech. 2016;6(4):e41.
|