Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (36): 5806-5811.doi: 10.3969/j.issn.2095-4344.2904
Previous Articles Next Articles
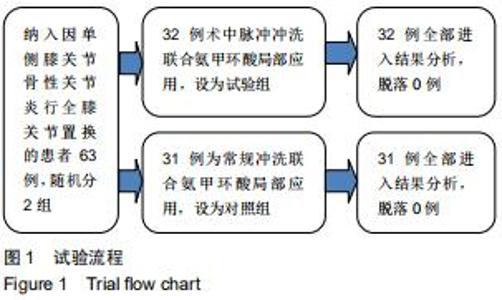
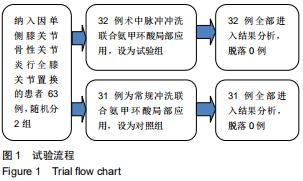
Application of perioperative pulse irrigation combined with tranexamic acid in total knee arthroplasty
Zhou Zhi, Xiong Yaqiong
- Department of Orthopedics, Huaian First Hospital Affiliated to Nanjing Medical University, Huaian 223300, Jiangsu Province, China
-
Received:2020-02-20Revised:2020-02-28Accepted:2020-03-30Online:2020-12-28Published:2020-10-27 -
Contact:Zhou Zhi, Associate chief physician, Department of Orthopedics, Huaian First Hospital Affiliated to Nanjing Medical University, Huaian 223300, Jiangsu Province, China -
About author:Zhou Zhi, MD, Associate chief physician, Department of Orthopedics, Huaian First Hospital Affiliated to Nanjing Medical University, Huaian 223300, Jiangsu Province, China -
Supported by:the National Natural Science Foundation of China, No. 81771985
CLC Number:
Cite this article
Zhou Zhi, Xiong Yaqiong. Application of perioperative pulse irrigation combined with tranexamic acid in total knee arthroplasty[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(36): 5806-5811.
share this article
|
[1] KURTZ S, ONG K, LAU E, et al. Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030.J Bone Joint Surg Am.2007;89(4):780-785.
[2] 李昌钊,陈加荣,李凭跃,等.全膝关节置换术后膝前痛与髌股关节的关系及髌股关节异常的影响因素[J].中华骨科杂志,2019,39(23): 1470-1477.
[3] CHEN TP, CHEN YM, JIAO JB, et al. Comparison of the effectiveness and safety of topical versus intravenous tranexamic acid in primary total knee arthroplasty:a meta-analysis of randomized controlled trials.J Orthop Surg Res.2017;2(1):11.
[4] ZHANG YM, YANG B, SUN XD, et al. Combined intravenous and intra-articular tranexamic acid administration in total knee arthroplasty for preventing blood loss and hyperfibrinolysis:A randomized controlled trial:Erratum.Medicine(Baltimore). 2019; 98(12):e15000.
[5] ZHANG LK, MA JX, KUANG MJ, et al. The efficacy of tranexamic acid using oral administration in total knee arthroplasty :a systematic review and meta-analysis.J Orthop Surg Res. 2017; 12(1):159.
[6] 罗明辉,洪坤豪,潘建科,等.全膝关节置换后应用自体血回输器是否必要:一项Meta分析[J].中国组织工程研究,2016,20(9):1336-1344.
[7] HOLT JB, MILLER BJ, CALLAGHAN JJ, et al. Minimizing blood transfusion in total hip and knee arthroplasty through a multimodal approach.J Arthroplasty.2016;31(2):378-382.
[8] PARTHVI R, MEHRA S. Risk of pulmonary embolism due to tranexamic acid:a case study. Am J Ther.2018;25(4):512-514.
[9] HIIPPALA ST, STRID LJ, WENNERSTRAND MI, et al. Tranexamic acidradically decreases blood loss and transfusions associated with total knee arthroplasty.Anesth Analg.1997;84(4):839-844.
[10] SHENG XU, JERRY YONGQIANGCHEN, QISHIZHENG, et al. The safest and most efficacious route of tranexamic acid administration in total joint arthroplasty: A systematic review and network meta-analysis.Thromb Res.2019;176:61-66.
[11] AGUILERA X, MARTINEZ-ZAPATA MJ, BOSCH A, et al. Efficacy and safety of fibrin glue and tranexamic acid to prevent postoperative blood loss in total knee arthroplasty: a randomized controlled clinical trial.J Bone Joint Surg Am. 2013;95(22): 2001-2007.
[12] BARRAL M, LALANDE L, VISTE A, et al. Bone cement usage modalities at a multi-site university hospital centre.Orthop Traumatol Surg Res.2019;105(2):383-388.
[13] GMSS JB. Estimating allowable blood loss:corrected for dilution. Anaesthesiology. 1983;58(3):277-280.
[14] NADLER SB, HIDALGO JH, BLOCH T. Prediction of blood volume in normal human adults.Surgery.1962;51(2):224-232.
[15] 范霖,杨东,刘凯缘,等.全膝关节置换术中间隙平衡截骨与测量截骨技术的对照研究[J].中华骨科杂志,2019,39(15):935-943.
[16] HASANAIN S, APOSTU D, ALREFAEE A, et al. Comparing the effect of tourniquet vs tourniquet-less in simultaneous bilateral total knee replacements.J Arthroplasty.2018;33(7):2119-2124.
[17] RYU KJ. CORR Insights((R)):does tourniquet use in TKA affect recovery of lower extremity strength and function?a randomized trial.Clin Orthop Relat Res.2016;474(1):78-80.
[18] TOSOUNIDIS T, ADERINTO J, GIANNOUDIS PV. Pipkin type-III fractures of the femoral head:Fix it or replace it.Injury. 2017; 48(11):2375-2378.
[19] FRISCH NB, WESSELL NM, CHARTERS MA, et al. Predictors and complications of blood transfusion in total hip and knee arthroplasty.J Arthroplasty.2014;29(9):189-192.
[20] ROCHE M, LAW TY, ROSAS S, et al. Transfusion requirements following total knee arthroplasty in patients with preexisting blood dyscrasia.Surg Technol Int.2017;30:435-440.
[21] KIM YT, KANG MW, LEE JK, et al. Combined use of topical intraarticular tranexamic acid and dvaroxaban in total knee arthroplasty safely reduces blood loss,transfusion rates and wound complications without increasing the risk of thrombosis. BMC Musculoskelet Disord.2018;19(1):227.
[22] ROYSTON D. Blood-sparing drugs: aprotinin, tranexamic acid,and epsilon-aminocaproic acid.Int Anesthesiol Clin.1995;33(1):155-179.
[23] WANG F, ZHAO KC, ZHAO MM, et al. The efficacy of oral versus intravenous tranexamic acid in reducing blood loss after primary total knee and hip arthroplasty: a meta-analysis.Medicine (Baltimore).2018;97(36):e12270.
[24] 王海若,刘曦,李明晋,等.氨甲环酸静脉滴注联合关节腔注射给药与膝关节镜术后疼痛及早期功能恢复的关系[J].中国组织工程研究, 2019,23(36):5766-5771.
[25] SUN H, DENG J, NING X, et al. Letter to the Editor Regarding "The Efficacy of Tranexamic Acid on Blood Loss of Lumbar Spinal Fusion Surgery: A Meta-Analysis of Randomized Controlled Trials". World Neurosurg.2019;122:708.
[26] MOSKAL JT, CAPPS SG. Meta-analysis of intravenous tranexamic acid in primary total hip arthroplasty.Orthopedics. 2016;39(5):e883-892.
[27] KIM YH, PARK JW, KIM JS, et al. Does tranexamic acid increase the risk of thromboembolism after bilateral simultaneous total knee arthroplasties in Asian population? Arch Orthop Trauma Surg. 2018;138(1):83-89.
[28] MARIANI P, BUTTARO MA, SLULLITEL PA, et al. Transfusion rate using intravenous tranexamic acid in hip revision surgery.Hip Int. 2018;28(2):194-199.
[29] HUANG F, WU D, MA G, et al. The use of tranexamic acid to reduce blood loss and transfusion in major orthopedic surgery:a meta-analysis.J Surg Res.2014;186(1):318-327.
[30] ABEDL MP, CHALMERS BP, TAUNTON MJ, et al. Intravenous versus topical tranexamic acid in total knee arthroplasty:both effective in a randomized clinical trial of 640 patients.J Bone Joint Surg Am.2018;100(12):1023-1029.
[31] YOZAWA S, OGAWA H, MATSUMOTO K, et al. Pedarticular injection of tranexamic acid reduces blood loss and the necessity for allogeneic transfusion after total knee arthroplasty using autologous transfusion:a retrospective observational study.J Arthroplasty.2018;33(1):86-89.
[32] KAZEMI SM, MOSAFFA F, EAJAZI A, et al. The effect of tranexamic acid on reducing blood loss in cementless total hip arthroplasty under epidural anesthesia.Orthopedics.2010; 33(1):17.
[33] 张志权,刘金文,张葆青,等.氨甲环酸静滴联合局部应用对全膝关节置换术失血的影响及其安全性评估[J].现代医院,2018,18(6):886-890.
[34] 张少云,谢锦伟,黄强,等.全膝关节置换术后多次静脉应用氨甲环酸对纤溶活性及炎症反应的影响[J].中华骨科杂志, 2017,37(23): 1483-1489.
[35] 冯贵喜,刘军,张福江,等.氨甲环酸局部应用对单侧全膝关节置换术后隐性失血量的影响[J].中华骨科杂志,2016,36(3):151-155.
[36] MOTE GA,MALAY DS.Efficacy of power-pulsed lavage in lower extremity wound infections: a prospective observational study.J Foot Ankle Surg.2010;49(2):135-142.
[37] NORTON MR, EYRES KS. Irrigation and suction technique to ensure reliable cement penetration for total knee arthroplasty.J Arthroplasty.2000;15(4):468-74. [38] GEORGE MD, BAKER JF, YENCHIH HSU J, et al. Perioperative timing of infliximab and the risk of serious infection after elective hip and knee arthroplasty.Arthritis Care Res. 2017;69(12): 1845-1854. |
| [1] | Zhong Yizheng, Huang Peizhen, Cai Qunbin, Zheng Liqin, He Xingpeng, Dong Hang. Microstructural indexes that determine the trabecular bone maximum stress of micro-finite element models [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1313-1318. |
| [2] | Li Xiaomin, Tian Xiangdong, Tan Yetong, Zhu Guangyu, Wang Rongtian, Wang Jian, Xue Zhipeng, Ma Sheng, Hu Yuanyi, Huang Ye, Ding Tiansong. Changes of lower limb force line and knee function after high tibial osteotomy in osteoporotic medial ventricular knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1325-1329. |
| [3] | Wu Tianliang, Tao Xiuxia, Xu Hongguang. Influence of different bone mineral densities on cage subsidence after stand-alone oblique lateral interbody fusion: three-dimensional finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1352-1358. |
| [4] | Wen Xinghua, Ding Huanwen, Cheng Kai, Yan Xiaonan, Peng Yuanhao, Wang Yuning, Liu Kang, Zhang Huiwu. Three-dimensional finite element model analysis of intramedullary nailing fixation design for large femoral defects in Beagle dogs [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1371-1376. |
| [5] | He Yinhao, Li Xiaosheng, Chen Hongwen, Chen Tiezhu. 3D printed porous tantalum metal in the treatment of developmental dysplasia of the hip: current status and application prospect [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1455-1461. |
| [6] | Dang Yi, Du Chengyan, Yao Honglin, Yuan Nenghua, Cao Jin, Xiong Shan, Zhang Dingmei, Wang Xin. Hormonal osteonecrosis and oxidative stress [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1469-1476. |
| [7] | Sun Jiajia, Zhu Haidi, Lu Yun, Zhang Kai. Comparison of bone metabolism markers between type 2 diabetes mellitus and non-type 2 diabetes mellitus patients with hip fracture [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1156-1160. |
| [8] | Huang Linke, Wei Linhua, Jiang Jie, Liu Qian, Chen Weiwei. Effects of estrogen combined with treadmill exercise on bone mass and articular cartilage in ovariectomized mice [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1166-1171. |
| [9] | Yang Zhishan, Tang Zhenglong. YAP/TAZ, a core factor of the Hippo signaling pathway, is involved in bone formation [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1264-1271. |
| [10] | Bai Yulong, Li Zhonghai, Zhao Yantao, Xia Cencan, Shi Lei. History, current situation and prospect of tissue banks in China [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1306-1312. |
| [11] | Liu Jiaxin, Jia Peng, Men Yutao, Liu Lu, Wang Yeming, Ye Jinduo. Design and optimization of bone trabecular structure with triply periodic minimal surfaces [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 992-997. |
| [12] | Yuan Hucheng, Ding Yongguo, Ma Xuehua, Ma Wenxin, Sun Jianmin, Wang Zili, Jin Weidong. Sustained releasing of pyrazinamide, capreomycin, moxifloxacin and amikacin loaded bone cement in vitro [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1017-1022. |
| [13] | Zhao Wei, Feng Wei, Yang Tieyi, Ren Wei, Wang Yuxin, Lyu Huicheng, Chang Zhiqiang, Feng Xiaodong, Wang Ziheng, Guo Shibing. Antibiotic bone cement intramedullary nail prepared using 3D printed mold for the treatment of long bone infection in lower limbs [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1023-1030. |
| [14] | Zhu Lin, Gu Weiping, Wang Can, Chen Gang. Biomechanical analysis of All-on-Four and pterygomaxillary implants under different maxillary bone conditions [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 985-991. |
| [15] | Sun Jiangwei, Wang Junxiang, Baibujiafu·Yellisi, Dai Huijuan, Nijati·Turson. Three-dimensional finite element analysis of stress distribution in different smooth collar implants [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(7): 1004-1011. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||