Chinese Journal of Tissue Engineering Research ›› 2018, Vol. 22 ›› Issue (14): 2203-2208.doi: 10.3969/j.issn.2095-4344.0767
Previous Articles Next Articles
Artificial cornea preparation using collagen/chondroitin sulfate/fibroblast growth factor composite film
Mao Bao-liang, Hu Bin, Jia Lei, Shan Heng-yue, Li Xiang, Wang Ying, Yuan Wan-juan, Zhang Feng-chao, Chen Jing-hua
- School of Pharmaceutical Science, Jiangnan University, Wuxi 214122, Jiangsu Province, China
-
Received:2017-12-06Online:2018-05-18Published:2018-05-18 -
Contact:Chen Jing-hua, Professor, School of Pharmaceutical Science, Jiangnan University, Wuxi 214122, Jiangsu Province, China -
About author:Mao Bao-liang, School of Pharmaceutical Science, Jiangnan University, Wuxi 214122, Jiangsu Province, China -
Supported by:Jiangnan University Research Program, No. JUSRP115A36, JUSRP51709A; 2017 Student Innovation Program of Jiangnan University, No. 2395210232170990
CLC Number:
Cite this article
Mao Bao-liang, Hu Bin, Jia Lei, Shan Heng-yue, Li Xiang, Wang Ying, Yuan Wan-juan, Zhang Feng-chao, Chen Jing-hua . Artificial cornea preparation using collagen/chondroitin sulfate/fibroblast growth factor composite film[J]. Chinese Journal of Tissue Engineering Research, 2018, 22(14): 2203-2208.
share this article
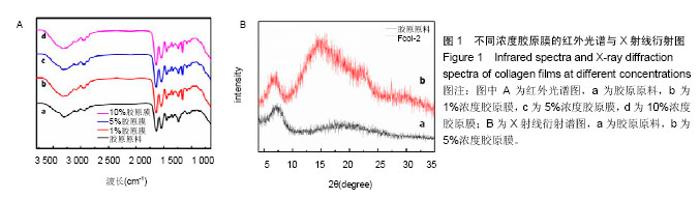
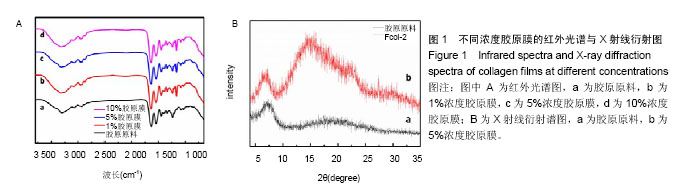
2.1 胶原膜的结构表征 酰胺Ⅰ、Ⅱ、Ⅲ为胶原纤维的特征指纹,1 634 cm-1吸收峰对应酰胺Ⅰ带的-CO伸缩振动,1 544 cm-1处对应酰胺Ⅱ带-NH弯曲振动,1 240 cm-1处则对应酰胺Ⅲ带-NH的变形振动。764,862 cm-1处特征谱带分别归属为咪唑的C-N-C及其面外的弯曲振动;1 032 cm-1为-CN的伸缩振动(图1A)。胶原原料与胶原再生膜FCol-1、FCol-2和FCol-3的红外谱图一致,表明胶原在[BMIM]Cl溶剂中未发生化学反应。另外,胶原具有完整的三螺旋结构时,I1240/1450≥1。根据红外谱图,计算胶原及再生膜的I1240/1450值分别为0.972,1.030、1.015和1.025,表明再生膜成分保持三螺旋构象[16,20]。 图1B中胶原的X射线衍射谱图主要有2个衍射峰,2θ=7.6°处的尖峰为晶区产生的衍射峰,代表组成胶原纤维的分子链间距离。2θ=14°-27°的宽峰为胶原纤维内部多种结构层次引起的漫散射。再生胶原膜FCol-2的X射线衍射谱图尖峰强度减小,且左移至2θ=7.2°,表明胶原分子链间距离增加,但有序结构未明显破坏[21-22]。"
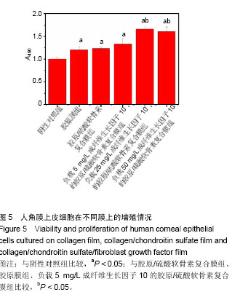
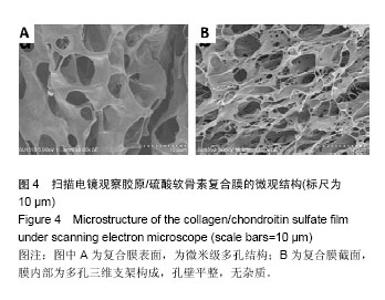
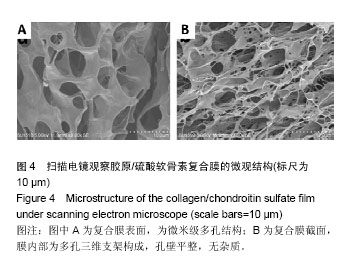
2.5 胶原/硫酸软骨素复合膜上硫酸软骨素的交联度 天青Ⅰ-硫酸软骨素复合物显色反应的标准曲线为y= 0.008 12x+0.187 3(R2=0.995 2),硫酸软骨素线性范围为0-1.0 mg/L。复合膜Col/CS-1、Col/CS-2和 Col/CS-3上硫酸软骨素结合率分别为4.5%、17.7%和23.1%[26-27]。2.6 细胞增殖实验结果 MTT实验结果表明,各实验组细胞增殖A值均高于阴性对照组(P < 0.05),表明胶原基膜对细胞无毒副作用,且可促进细胞的生长和增殖[9,18];负载 5 mg/L成纤维生长因子10的胶原/硫酸软骨素复合膜、胶原/硫酸软骨素复合膜、胶原膜上的细胞增殖A值低于负载25,50 mg/L成纤维生长因子10的胶原/硫酸软骨素复合膜(P < 0.05),其余组间两两比较差异均无显著性意义,见图5。"
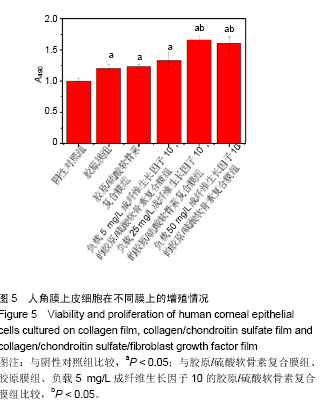
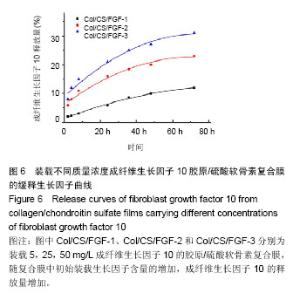
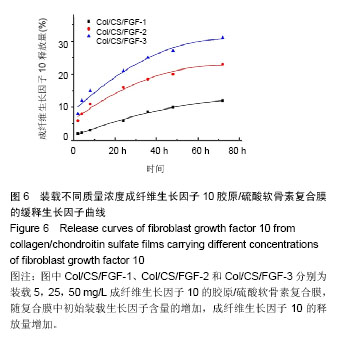
考虑到降低生长因子的用量,最终确定复合膜上成纤维生长因子10的最优负载质量浓度为25 mg/L[28]。 2.7 生长因子缓释实验结果 图6为装载不同质量浓度成纤维生长因子10复合膜在72 h内的释放曲线,可见成纤维生长因子10的释放量,随复合膜中初始装载生长因子含量的增加而增加。同时,Col/CS/FGF-1、Col/CS/FGF-2和Col/CS/FGF-3复合膜上的成纤维生长因子10释放缓慢,并在72 h时分别达到11%、23%和30%,释放行为符合药代动力学过程。成纤维生长因子10能有效促进角膜伤口愈合,然而直接在伤口应用成纤维生长因子10,会导致生长因子短期内失活和因高剂量导致的不良反应。实验制备的Col/CS/FGF复合膜能有效装载成纤维生长因子10,起到稳定作用,避免其因聚集导致的不良反应[27-28]。"
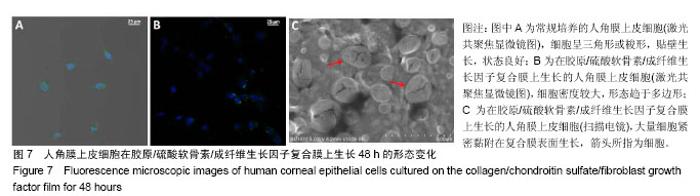
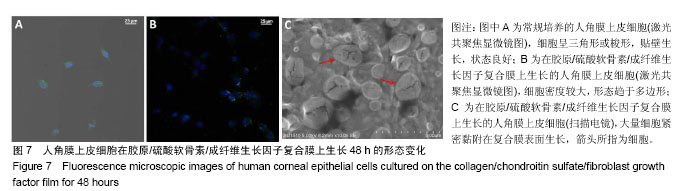
2.8 细胞黏附实验结果 图7示角膜上皮细胞在胶原/硫酸软骨素/成纤维生长因子复合膜上的生长情况,蓝色荧光标记为细胞核,绿色荧光标记为细胞膜。图7A为细胞培养48 h的未加胶原基膜的空白对照样,可以看到细胞呈三角形或梭形,贴壁生长,状态良好。在相同条件下,图7B中细胞在Col/CS/FGF-2复合膜上的生长密度明显增加,且细胞形态也趋于多边形[4],结果说明胶原/硫酸软骨素/成纤维生长因子复合膜能促进角膜上皮细胞的生长增殖,与MTT结果一致。同时,细胞在胶原基膜上贴附生长良好,细胞分布均匀,没有发生团聚现象。图7C示出角膜上皮细胞在Col/CS/FGF-2复合膜上黏附生长的扫描电镜图,红色箭头所指为细胞,可见在复合膜上种植细胞并培养72 h后,大量细胞紧密黏附在复合膜表面生长,表明该负载生长因子的胶原基复合膜具有良好生物相容性,能够促进细胞增 殖[15]。由此说明,实验采用具有完整三螺旋结构、免疫原性的胶原原料,通过简单、经济的方法制备出的胶原/硫酸软骨素/成纤维生长因子复合膜,具有良好生物相容性,无细胞毒性,且能促进人角膜上皮细胞的生长和增殖。"
| [1] Mirabelli P,Mukwaya A,Lennikov A,et al.Genome-wide expression differences in anti-Vegf and dexamethasone treatment of inflammatory angiogenesis in the rat cornea.Sci Rep.2017;7(1):7616.[2] Meek KM,Knupp C.Corneal structure and transparency.Prog Retin Eye Res.2015;49(2):1-16.[3] Stafiej P,Kung F,Thieme D,et al.Adhesion and metabolic activity of human corneal cells on PCL based nanofiber matrices. Mater Sci Eng C Mater Biol Appl.2017;71:764-777.[4] Riau AK,Mondal D,Yam GHF,et al.Surface modification of PMMA to improve adhesion to corneal substitutes in a synthetic core-skirt keratoprosthesis.ACS Appl MaterInterfaces.2015;7(39): 21690-21702.[5] Hemalatha T,Yadav S,Krithiga G,et al.Chitosan as a matrix for grafting methyl methacrylate: synthesis, characterization and evaluation of grafts for biomedical applications.Polym Bull(Berl). 2016;73(11): 3105-3117.[6] Yawon H,Gonhyung K.Evaluation of stability and biocompatibility of PHEMA-PMMA keratoprosthesis by penetrating keratoplasty in rabbits. Lab Anim Res.2016;32(4):181-186.[7] 李明.多孔n-HA/PVA/CF(PEEK)复合水凝胶的制备与性能研究[D].深圳:深圳大学化学与化工学院,2015:1-86.[8] Kharaghani D,Meskinfam M,Rezaeikanavi M,et al.Synthesis and characterization of hybrid nanocomposite via biomimetic method as an artificial cornea.Invest Ophth Vis Sci.2015;56(7):5024.[9] Chaiyasan W,Praputbut S,Kompella UB,et al.Penetration of mucoadhesive chitosan-dextran sulfate nanoparticles into the porcine cornea.Colloids Surf B Biointerfaces.2017;149:288-296.[10] Huang X,Wang R,Lu T,et al.Heparin-like chitosan hydrogels with tunable welling behavior, prolonged clotting times, and prevented contact activation and complement activation.Biomacromolecules. 2016;17(12):4011-4020.[11] Jamard M,Hoare T,Sheardown H.Nanogels of methylcellulose hydrophobized with N-tert-butylacrylamide for ocular drug delivery. Drug Deliv Transl Res.2016;6(6):648-659.[12] Tummala GK,Joffre T,Lopes VR,et al.Hyperelastic nanocellulose- reinforced hydrogel of high water content for ophthalmic applications. ACS Biomater Sci Eng.2016;2(11):2072-2079.[13] Sepulveda RV,Valente FL,Reis ECC,et al.Bacterial cellulose and bacterial cellulose/polycaprolactone composite as tissue substitutes in rabbits' cornea.Pesquisa Vet Brasil.2016;36:986-992.[14] Patchan MW,Chae JJ,Lee JD,et al.Evaluation of the biocompatibility of regenerated cellulose hydrogels with high strength and transparency for ocular applications.J Biomater Appl. 2015;30(7):1049-1059.[15] Rudisill SG,DiVito MD,Hubel A,et al.In vitro collagen fibril alignment via incorporation of nanocrystalline cellulose.Acta Biomaterialia.2015; 12(1):122-128.[16] Zhao X,Song W,Liu S,et al.Corneal regeneration by utilizing collagen based materials.Sci China-Chem.2016;59(12):1548-1553.[17] Mohamed-Noriega K,Butron-Valdez K,Vazquez-Galvan J,et al.Corneal melting after collagen cross-linking for keratoconus in a thin cornea of a diabetic patient treated with topical nepafenac: a case report with a literature review.Case Rep Ophthalmol.2017;7(1):119-124.[18] Zhao X,Long K,Liu Y,et al.To prepare the collagen-based artificial cornea with improved mechanical and biological property by ultraviolet-A/riboflavin crosslinking.J Appl Polym Sci.2017;134(38): 45226.[19] Medeiros CS,Giacomin NT,Bueno RL,et al.Accelerated corneal collagen crosslinking: Technique, efficacy, safety, and applications.J Cataract Refract Surg.2016;42(12):1826-1835.[20] Hu C,Yu L,Wei M.Biomimetic intrafibrillar silicification of collagen fibrils through a one-step collagen self-assembly/ silicification approach.RSC Adv.2017;7(55):34624-34632.[21] 刘洁,赵世玉,徐洲,等.胶原在两种离子液体[BMIM]Cl 和[BMIM]Ac 中的溶解及再生结构比较[J].化工学报,2015,66(6):2196-2204.[22] Li C,Liao H,Zhang X,et al.Preparation of cationic modified collagen extracted from leather wastes and their application in dye flocculation.J Appl Polymr Sci.2017;134:45363.[23] Younesi M,Donmez BO,Islam A,et al.Heparinized collagen sutures for sustained delivery of PDGF-BB: delivery profile and effects on tendon-derived cells in-vitro.Acta Biomaterialia.2016;41:100-109.[24] Hariya T,Tanaka Y,Yokokura S,et al.Transparent, resilient human amniotic membrane laminates for corneal transplantation.Biomaterials. 2016;101:76-85.[25] Chae JJ,Choi JS,Lee JD,et al.Physical and biological characterization of the gamma-irradiated human cornea.Cornea. 2015;34(10):1287-1294.[26] Pospichal R,Nesmerak K,Rychlovsky P,et al.Determination of chondroitin sulfate by thiazine dyes using flow injection analysis with spectrophotometric detection.Anal Lett.2007;40(6):1167-1175.[27] Ribeiro AM,Figueiras A,Veiga F.Improvements in topical ocular drug delivery systems: hydrogels and contact lenses.J Pharm Pharm Sci. 2015;18(5):683-695.[28] Cai J,Dou G,Zheng L,et al.Pharmacokinetics of topically applied recombinant human keratinocyte growth factor-2 in alkali-burned and intact rabbit eye.Exp Eye Res.2015;136:93-99. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Shen Jinbo, Zhang Lin. Micro-injury of the Achilles tendon caused by acute exhaustive exercise in rats: ultrastructural changes and mechanism [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1190-1195. |
| [3] | Liang Xueqi, Guo Lijiao, Chen Hejie, Wu Jie, Sun Yaqi, Xing Zhikun, Zou Hailiang, Chen Xueling, Wu Xiangwei. Alveolar echinococcosis protoscolices inhibits the differentiation of bone marrow mesenchymal stem cells into fibroblasts [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 996-1001. |
| [4] | Duan Liyun, Cao Xiaocang. Human placenta mesenchymal stem cells-derived extracellular vesicles regulate collagen deposition in intestinal mucosa of mice with colitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1026-1031. |
| [5] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [6] | Yang Xin, Jin Zhe, Feng Xu, Lu Bing. The current situation of knowledge and attitudes towards organ, eye tissue, body donation of residents in Shenyang [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 779-784. |
| [7] | Xu Dongzi, Zhang Ting, Ouyang Zhaolian. The global competitive situation of cardiac tissue engineering based on patent analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 807-812. |
| [8] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [9] | Chang Wenliao, Zhao Jie, Sun Xiaoliang, Wang Kun, Wu Guofeng, Zhou Jian, Li Shuxiang, Sun Han. Material selection, theoretical design and biomimetic function of artificial periosteum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 600-606. |
| [10] | Liu Liu, Zhou Qingzhu, Gong Zhuo, Liu Boyan, Yang Bin, Zhao Xian. Characteristics and manufacturing techniques of collagen/inorganic materials for constructing tissue-engineered bone [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 607-613. |
| [11] | Liu Fei, Cui Yutao, Liu He. Advantages and problems of local antibiotic delivery system in the treatment of osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 614-620. |
| [12] | Li Xiaozhuang, Duan Hao, Wang Weizhou, Tang Zhihong, Wang Yanghao, He Fei. Application of bone tissue engineering materials in the treatment of bone defect diseases in vivo [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 626-631. |
| [13] | Zhang Zhenkun, Li Zhe, Li Ya, Wang Yingying, Wang Yaping, Zhou Xinkui, Ma Shanshan, Guan Fangxia. Application of alginate based hydrogels/dressings in wound healing: sustained, dynamic and sequential release [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 638-643. |
| [14] | Chen Jiana, Qiu Yanling, Nie Minhai, Liu Xuqian. Tissue engineering scaffolds in repairing oral and maxillofacial soft tissue defects [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 644-650. |
| [15] | Xing Hao, Zhang Yonghong, Wang Dong. Advantages and disadvantages of repairing large-segment bone defect [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 426-430. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||