Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (4): 564-569.doi: 10.3969/j.issn.2095-4344.2370
Previous Articles Next Articles
Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots
Wu Zijian1, Hu Zhaoduan1, Xie Youqiong1, Wang Feng1, Li Jia1, Li Bocun2, Cai Guowei2, Peng Rui1
- 1Hubei University of Traditional Chinese Medicine, Wuhan 430065, Hubei Province, China; 2Department of Acupuncture, Union Hospital, Tongji Medical College, Huazhong University of Science and Technology, Wuhan 430020, Hubei Province, China
-
Received:2020-05-25Revised:2020-05-26Accepted:2020-06-18Online:2021-02-08Published:2020-11-21 -
Contact:Peng Rui, Professor, Doctoral supervisor, Hubei University of Traditional Chinese Medicine, Wuhan 430065, Hubei Province, China -
About author:Wu Zijian, Doctoral candidate, Hubei University of Traditional Chinese Medicine, Wuhan 430065, Hubei Province, China -
Supported by:the National Natural Science Foundation of China, No. 81774410
CLC Number:
Cite this article
Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
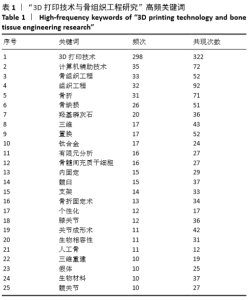
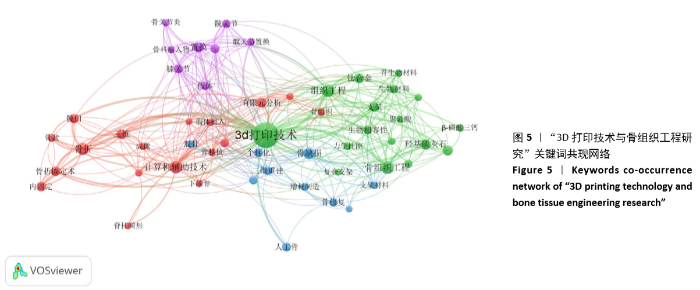
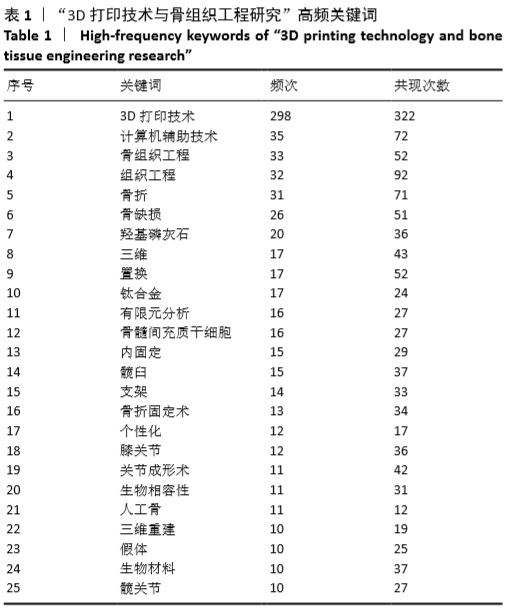
2.5 关键词的共现可视化分析 关键词共现可视化分析展现的是3D打印与骨组织工程相关文献中关键词的出现频次及相互关系,将关键词共现的阈值设置为5,即当其出现频 次≥5时才纳入共现分析。对于意义相同但表述有差异的关键词进行了近义词合并后,出现频率>5的关键词共53个。单纯的频次分析结果显示,出现频率排名前10的关键词分别为:3D打印技术、计算机辅助技术、骨组织工程、组织工程、骨折、骨缺损、羟基磷灰石、三维、置换、钛合金。出现10次以上的高频关键词见表1。关键词共现网络形成了4个聚类,各聚类之间的联系密切,其研究主题分别为骨组织工程支架材料、3D打印相关技术及其在骨科的应用、3D打印与关节置换、其他,见图5、表2。 2.5.1 骨组织工程支架材料 骨组织工程研究主要集中在种子细胞、支架材料和骨的构建3个方面[15],其中支架材料为种子细胞的再生提供良好的场地,高孔隙率材料可促进种子细胞黏附和增殖,提高活性,在骨组织工程中充当最基本的构架角色,所以支架材料也一直是骨组织工程研究重点[16-17]。传统的生物材料包括生物陶瓷、玻璃、金属和高分子材料等[10]。羟基磷灰石和磷酸三钙属于人工合成的无机材料[18],羟基磷灰石是目前组织工程骨支架材料研究的热点,与骨组织的主要无机成分相同,具有良好的生物相容性和骨诱导性,但将其制成多孔材料后其抗弯强度与韧性较差,不能满足人体承重部分骨代替的要求[19],所以在单独应用方面受到一定限制,需要通过与其他材料复合以提高整体性能。目前已研制出了羟基磷灰石复合金属镁、羟基磷灰石复合聚己内酯、羟基磷灰石复合胶原蛋白等多种具有良好生物特性的羟基磷灰石复合材料组织工程骨支架,同时有研究已开始应用3D 打印技术制作具有更优异生物特性的羟基磷灰石组织工程骨支架[20]。磷酸三钙是磷酸钙陶瓷的一种,具有良好的骨传导性和孔隙率,能够促进再生组织血管化[21],但是在体内降解较快,所以磷酸三钙同样需要与聚苯乙烯[22]、硫酸钙基粉末等材料复合以提高性能[23],合成的磷酸三钙材料可以通过3D打印技术生产出类似骨小梁显微结构的支架。聚乳酸和聚己内酯属于人工合成有机高分子材料,具有性质稳定、降解周期可调节、易于加工、生物兼容性好等优点,能满足骨组织工程的要求[24]。聚乳酸在体内水解生成乳酸,易于参加体内代谢,可以较好地修复骨缺损。聚己内酯在体内降解速率较低,但药物渗透性较高,适用于构建长期植入给药装置[25]。聚乳酸和聚己内酯及其复合物支架材料已被广泛应用在临床医学领域[22]。胶原属于天然的高分子材料,是骨骼中主要的有机成分,与无机材料共同应用于骨支架材料时能够锁住钙质,增强骨组织的韧性,而且胶原具有较好的骨诱导性,能促进种子细胞向成骨细胞分化[27]。钛合金材料密度低、强度高,具有较好的耐蚀性、抗疲劳性和生物相容性,是最有吸引力的生物金属材料之一,目前3D打印的钛合金支架已在脊柱、关节和肿瘤骨科的骨修复中广泛应用[28]。 采用传统生物材料对骨组织进行修复之后易产生的契合度差、磨损、腐蚀等问题,特别是无法形成具有生物功能的骨组织长期困扰着临床医师,容易导致术后近、远期疗效不确切,极大影响着患者的生活质量[29]。随着材料工程的不断发展,骨组织工程支架材料的选择多不局限应用单一的材料,而是倾向于将不同性能的材料复合,以寻找生物安全性和相容性高、可塑性和机械性能良好、结构和孔隙率合适的理想骨支架材料。 2.5.2 3D打印技术 3D打印技术依靠计算机辅助成像,以生物材料为打印介质,能够快速、精确地复制和重建缺损组织或器官的复杂结构[30]。首先需要获取患者病变/缺损组织的断层扫描或磁共振成像数据,利用计算机辅助设计建立图像模型,然后将相关数据输送到3D打印机中,打印机按照预设的路径将三维模型用合适的生物材料逐层打印堆积起来,最终形成与组织一致的三维支架[31]。常见的3D打印技术包括:熔融沉积建模、光固化成型、选择性激光烧结、立体平版印刷、选择性激光熔化、喷墨3D打印、黏附液滴和粉末床基础增材制造、数字激光加工、连续液体界面生产等[32-33]。3D打印的最大优点在于能够精确、快速实现支架复杂的宏观外形与内部微细结构的一体化构建,可以实现针对特定患者、特定组织器官的个性化生产,这是传统支架成型方法无法做到的[34]。 2.5.3 3D打印技术在骨科的应用 与其他器官和组织相比,骨的结构与功能相对较简单,因此骨组织工程近年来取得了迅速发展[35]。相对于其他组织修复方式,3D打印的骨组织具有稳定性好、连续性佳、术后并发症少等优势[36]。石磊 等[37]对15例脊柱肿瘤患者行全椎体切除及3D打印人工椎体重建,术后评估人工椎体稳定情况、相邻椎体骨长入情况及患者生存情况,结果表明利用3D打印个体化人工椎体进行脊柱肿瘤切除后重建可以精确恢复脊柱连续性,利于相邻骨的长入,术后近、远期稳定性均良好。另外,不同的材料具有不同的生物特性,3D打印技术可根据患者病情量身定制专属材料和特需规格,以促进患者愈合,恢复应力平衡。鲁亚杰等[38]利用3D打印假体复合β-磷酸三钙生物陶瓷重建下肢骨肉瘤切除后大段骨缺损,所有安装假体均未发生无菌性松动、假体周围感染、假体断裂等并发症,术后9个月假体断端与骨整合良好。刘宏伟等[39]对高能电子束熔融3D打印个性化股骨假体和临床4种类型标准化假体(SR组配柄、柱形柄、矩形柄、锥形柄)进行了三维有限元分析(生物模拟力学),结果显示相比于其他4种假体,3D打印个性化股骨假体对股骨近端的应力遮挡更低,界面应力比SR组配柄更均匀,在缓慢行走时3D打印假体产生的初始微动略高于其他假体,但不会影响骨长入。3D打印技术除了应用在骨组织工程构建外,还应用于骨科术前规划、手术模拟和术中特异性定位导航等方面。孙果梅等[40]对应用了3D打印技术的84项骨科手术进行了安全性和有效性分析,结果表明3D打印技术在关节、足跟、脊柱和四肢骨的手术中均有应用,Meta分析显示,3D打印技术在减少手术时间、术中出血量和术中射线暴露次数,提高术后功能评分,减少术后并发症方面效果显著,证明在骨科手术中运用3D打印技术具有重要的临床意义。 2.5.4 3D打印与关节置换 对发生于髋关节和膝关节骨肿瘤、骨坏死、病情严重的晚期骨关节炎和先天性髋关节发育不良的患者,大多需行关节置换手术,传统的人工关节假体基本能取得满意效果,但关节畸形和严重骨丢失时传统假体无法与病损的骨性结构良好匹配,术后患者关节功能恢复仍有受到影响[41-42]。目前,3D打印膝关节假体已被应用于股骨远端和胫骨近端肿瘤及全膝关节置换术后感染所致的严重膝关节骨缺损重建[43]。研究表明,在进行膝关节翻修手术时使用独特形状和高孔隙率的3D打印假体,其胫骨和股骨多孔结构能诱导骨长入,术后6个月随访显示患者膝关节功能良好[44]。受臼杯假体材料、匹配度和臼杯安装位置等因素影响导致的臼杯假体周围松动,是造成关节置换手术翻修的重要原因,故目前打造具有超多孔界面、有利于骨长入和软组织附着的人工髋臼杯,是3D打印技术应用于人工关节植入物中的研究热点[45]。程文俊等[46]进行全髋关节置换时使用3D打印钛合金骨小梁金属臼杯,术后6个月臼杯稳定、骨长入优异,无松动及骨溶解。夏志勇等[47]应用3D打印钛合金臼杯、垫片对15例患者行单侧髋关节置换翻修术,术后12-18个月随访显示3D打印假体内有骨小梁通过,稳定性好,短期疗效满意。"
| [1] TANG D, TARE RS, YANG LY, et al. Biofabrication of Bone Tissue: Approaches, Challenges and Translation for Bone Regeneration.Biomaterials. 2016;83: 363-382. [2] ASHMAN O,PHILLIPS AM.Treatment of non-unions with bone defects: which option and why? Injury.2013;44 Suppl 1:S43-45. [3] 左进富,孙淼,韩宁宁,等.3D生物打印在组织工程中的应用[J].组织工程与重建外科杂志,2019,15(3):201-203. [4] CRANE GM, ISHAUG SL, MIKOS AG. Bone tissue engineering.Nat Med.1996; 1(12):1322-1324. [5] ZHANG C, WANG J, FENG H, et al. Replacement of segmental bone defects using porous bioceramic cylinders: A biomechanical and X-ray diffraction study.Biomed Mater Res.2001;54(3):407-411. [6] 党文涛.3D打印生物陶瓷支架用于骨组织修复和治疗[D].北京:中国科学院大学(中国科学院上海硅酸盐研究所),2019. [7] 燕朋程,王东.3D打印在组织工程骨预制及其骨缺损修复的作用探讨[J].临床医药文献电子杂志,2019,6(12):188. [8] HITESH L, MOHIT KP. 3D Printing and Its Applications in Orthopaedic Trauma: A Technological Marvel.Clin Orthop Trauma.2018;9(3):260-268. [9] BRUNELLO G, SIVOLELLA S, MENEGHELLO R, et al. Powder-based 3D Printing for Bone Tissue Engineering.Biotechnol Adv.2016;34(5):740-753. [10] ZHANG L, YANG GJ, JOHNSON BN, et al. Three-dimensional (3D) Printed Scaffold and Material Selection for Bone Repair.Acta Biomater.2019; 84: 16-33. [11] OWEN T, JACQUELINE KM, YI L, et al. The Applications of 3D Printing for Craniofacial Tissue Engineering.Micromachines(Basel).2019;10(7):480. [12] 党莹,李月,李瑞玉,等.骨组织工程支架材料在骨缺损修复及3D打印技术中的应用[J]. 中国组织工程研究,2017,21(14): 2266-2273. [13] 余文,卢世璧,孟昊业,等.3D打印生物陶瓷在骨组织工程中的研究现状[J].中国矫形外科杂志,2018,26(14):1306-1310. [14] VAN EN, WALTMAN L. Software survey: VOSviewer, a computer program for bibliometric mapping.Scientometrics.2010;84(2):523-538. [15] 毛天球,杨维东,陈富林,等.组织工程骨的研究[J].中国修复重建外科杂志,2003,17(2):122-124. [16] 杨志明.组织工程骨的研究成果及存在的问题[J].中国修复重建外科杂志,2005,19(2):87-89. [17] JAKUS AE, GEISENDORFER NR, LEWIS PL, et al. 3D-printing Porosity: A New Approach to Creating Elevated Porosity Materials and Structures.Acta Biomater. 2018;72:94-109. [18] 李亚莹,白艳洁,曹婷.羟基磷灰石在硬组织修复中的应用进展[J].中国美容整形外科杂志,2020,31(3):190-191,199-200. [19] SHIMOMURA K, MORIGUCHI Y, NANSAI R, et al. Comparison of 2 different formulations of artificial bone for a hybrid implant with a tissue-engineered construct derived from synovial mesenchymal stem cells: a study using a rabbit osteochondral defect model.Am J Sports Med.2017;45(3):666-675. [20] 柴乐,全仁夫,黄小龙.羟基磷灰石构建组织工程骨支架的研究进展[J].中医正骨,2018, 30(1):44-46,50. [21] 刘洋,王欢,朱晔,等.骨组织工程支架材料研究进展[J].临床口腔医学杂志,2019,35(10):637-639. [22] TERRANOVA L, DRAGUSIN DM, MALLET R, et al. Repair of calvarial bone defects in mice using electrospun polystyrene scaffolds combined with β-TCP or gold nanoparticles. Micron.2017;93:29-37. [23] ZHOU Z, BUCHANAN F, MITCHELL C, et al. Printability of calcium phosphate: Calcium sulfate powders for the application of tissue engineered bone scaffolds using the 3D printing technique.Mater Sci Eng C Mater Biol Appl. 2014;38(1):1-10. [24] MEYER U, JOOS U, WIESMANN HP. Biological and biophysical principles in extracorporal bone tissue engineering: Part III.Int J Oral Maxil Surg.2004; 33(7):635-641. [25] DANG HP, SHABAB T, SHAFIEE A, et al. 3D Printed Dual Macro-, Microscale Porous Network as a Tissue Engineering Scaffold With Drug Delivering Function. Biofabrication.2019;11(3):035014. [26] 杨振磊,卢剑,蒋尧传.骨组织工程高分子材料和复合材料的研究进展[J].临床医学工程, 2013,20(11):1460-1461. [27] CHEN GC, LV YG, DONG CJ, et al. Effect of Internal Structure of Collagen/Hydroxyapatite Scaffold on the Osteogenic Differentiation of Mesenchymal Stem Cells.Curr Stem Cell Res Ther.2015;10(2):99-108. [28] 李晓宇,宋超伟,费琦,等.骨修复3D打印钛合金支架材料的研究进展[J].临床和实验医学杂志,2019,18(2):222-225. [29] TACK P, VICTOR J, GEMMEL P, et al. 3D-printing Techniques in a Medical Setting: A Systematic Literature Review.Biomed Eng Online.2016;15(1):115. [30] XIONG L, LI XY, LI H, et al. The Efficacy of 3D Printing-Assisted Surgery for Traumatic Fracture: A Meta-Analysis.Postgard Med.2019;95(1126):414-419. [31] LEONG KF, CHEAH CM, CHUA CK. Solid freeform fabrication of three-dimensional scaffolds for engineering replacement tissues and organs.Biomaterials.2003;24:2363-2378. [32] 田冶,曾庆慧,胡相华,等.3D打印技术及在组织工程领域的研究进展[J].中国医疗器械信息,2015,21(8):7-12. [33] WANG C, HUANG W, ZHOU Y, et al. 3D printing of bone tissue engineering scaffoldsBioact Mater. 2020;5(1):82-91. [34] 王镓垠,柴磊,刘利彪,等.人体器官3D打印的最新进展[J].机械工程学报,2014,50(23):119-127. [35] YU W, SUN X, MENG HY, et al. 3D printed porous ceramic scaffolds for bone tissue engineering: a review.Biomater Sci.2017;5(9):1690-1698. [36] SERRANO C, BRINK HV, PINEAU J, et al. Benefits of 3D Printing Applications in Jaw Reconstruction: A Systematic Review and Meta-Analysis.Craniomaxillofac Surg.2019;47(9):1387-1397. [37] 石磊,栗向东,李小康,等.新型3D打印个体化人工椎体在脊柱重建中的初步研究[J].中华骨科杂志,2020,40(6):335-343. [38] 鲁亚杰,龙作尧,李明辉,等.下肢骨肉瘤切除后大段骨缺损患者的3D打印假体复合β-TCP生物陶瓷重建[J].中国骨与关节杂志,2019,8(1):21-26. [39] 刘宏伟,蒋俊锋,张云坤,等.金属3D打印个性化股骨假体和4种类型标准化假体的生物力学对比[J].中国组织工程研究,2019,23(32): 5151-5157. [40] 孙果梅,刘群,刘永章.3D打印在骨科手术中的安全性和有效性:系统综述和Meta分析[J].中国医疗设备,2020,35(4):142-148. [41] 张常贵,杨柳,段小军.3D打印技术在关节外科的临床应用进展[J].中国矫形外科杂志, 2019,27(16):1497-1501. [42] JOHANN H, THOMAS JH, WARWICK R, et al. 3D-printed Patient-specific Guides for Hip Arthroplasty.Am Acad Orthop Surg.2018;26(16):342-348. [43] 余昆,韩文锋,张叶兵,等.3D打印技术在人工全膝关节置换术中的应用及进展[J].华南国防医学杂志,2019,33(3):217-220. [44] YIN Q, LIU WANG S. Application of customized augments fabricated by rapid prototyping for severe bone defects of the knee.Chin Med J (Engl). 2014;127(15):2870-2871. [45] 徐辉.3D打印假体在人工关节置换中的应用[J].中华损伤与修复杂志(电子版),2016,11(4):244-247. [46] 程文俊,王俊文,焦竞,等.3D打印钛合金骨小梁金属臼杯在初次全髋关节置换术应用的临床和影像学评估:5年临床随访[J].中华创伤骨科杂志,2018,20(12):1066-1071. [47] 夏志勇,马康康,李凯,等. 3D打印钛合金骨小梁金属臼杯、垫块在全髋关节置换翻修术中的应用[J]. 中国骨与关节损伤杂志,2017,32(2):121-124. [48] 陈勇跃,田文芳,吴金红.主题领域研究热点跟踪及趋势预测的可视化分析方法研究[J].情报理论与实践,2017,40(6):117-121. [49] 薛晓丽,武夷山.跨学科研究的文献计量及可视化分析[J].情报杂志, 2014(7):122-127. [50] MA HS, FENG C, CHANG J, et al. 3D-printed Bioceramic Scaffolds: From Bone Tissue Engineering to Tumor Therapy.Acta Biomater.2018;79:37-59. [51] 郑荣桥,何星.三维打印材料在骨组织工程中的研究进展[J].广东化工, 2018,45(7):151-152. [52] 张强,朱婵.近5年骨质疏松英文文献的计量学及可视化分析:Web of Science来源数据[J].中国组织工程研究, 2020, 24(17): 2752-2758. |
| [1] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [2] | Jiang Yong, Luo Yi, Ding Yongli, Zhou Yong, Min Li, Tang Fan, Zhang Wenli, Duan Hong, Tu Chongqi. Von Mises stress on the influence of pelvic stability by precise sacral resection and clinical validation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1318-1323. |
| [3] | Lu Dezhi, Mei Zhao, Li Xianglei, Wang Caiping, Sun Xin, Wang Xiaowen, Wang Jinwu. Digital design and effect evaluation of three-dimensional printing scoliosis orthosis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1329-1334. |
| [4] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [5] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [6] | Wei Wei, Li Jian, Huang Linhai, Lan Mindong, Lu Xianwei, Huang Shaodong. Factors affecting fall fear in the first movement of elderly patients after total knee or hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1351-1355. |
| [7] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [8] | Xiao Guoqing, Liu Xuanze, Yan Yuhao, Zhong Xihong. Influencing factors of knee flexion limitation after total knee arthroplasty with posterior stabilized prostheses [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1362-1367. |
| [9] | Huang Zexiao, Yang Mei, Lin Shiwei, He Heyu. Correlation between the level of serum n-3 polyunsaturated fatty acids and quadriceps weakness in the early stage after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1375-1380. |
| [10] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [11] | Wang Haiying, Lü Bing, Li Hui, Wang Shunyi. Posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis: prediction of functional prognosis of patients based on spinopelvic parameters [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1393-1397. |
| [12] | Lü Zhen, Bai Jinzhu. A prospective study on the application of staged lumbar motion chain rehabilitation based on McKenzie’s technique after lumbar percutaneous transforaminal endoscopic discectomy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1398-1403. |
| [13] | Chen Xinmin, Li Wenbiao, Xiong Kaikai, Xiong Xiaoyan, Zheng Liqin, Li Musheng, Zheng Yongze, Lin Ziling. Type A3.3 femoral intertrochanteric fracture with augmented proximal femoral nail anti-rotation in the elderly: finite element analysis of the optimal amount of bone cement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1404-1409. |
| [14] | Du Xiupeng, Yang Zhaohui. Effect of degree of initial deformity of impacted femoral neck fractures under 65 years of age on femoral neck shortening [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1410-1416. |
| [15] | Zhang Shangpu, Ju Xiaodong, Song Hengyi, Dong Zhi, Wang Chen, Sun Guodong. Arthroscopic suture bridge technique with suture anchor in the treatment of acromioclavicular dislocation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1417-1422. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||