Chinese Journal of Tissue Engineering Research ›› 2024, Vol. 28 ›› Issue (19): 2981-2987.doi: 10.12307/2024.179
Previous Articles Next Articles
Vitamin D3 attenuates high-glucose exposure-induced oxidative stress to promote osteogenic differentiation of human umbilical cord mesenchymal stem cells
Xie Ting1, Liu Tingting1, Zeng Xuehui1, Li Yamin1, Zhou Panghu2, Yi Nianhua1
- 1Department of Women’s Health Care, Maternal and Child Health Hospital of Hubei Province, Wuhan 430070, Hubei Province, China; 2Department of Orthopedics, Renmin Hospital of Wuhan University, Wuhan 430060, Hubei Province, China
-
Received:2023-05-08Accepted:2023-07-08Online:2024-07-08Published:2023-09-25 -
Contact:Yi Nianhua, Master, Chief physician, Department of Women’s Health Care, Maternal and Child Health Hospital of Hubei Province, Wuhan 430070, Hubei Province, China Zhou Panghu, PhD, Chief physician, Doctoral supervisor, Department of Orthopedics, Renmin Hospital of Wuhan University, Wuhan 430060, Hubei Province, China -
About author:Xie Ting, Master, Associate chief physician, Department of Women’s Health Care, Maternal and Child Health Hospital of Hubei Province, Wuhan 430070, Hubei Province, China -
Supported by:Hubei Provincial Key Research and Development Program, No. 2021BCA147 (to ZPH)
CLC Number:
Cite this article
Xie Ting, Liu Tingting, Zeng Xuehui, Li Yamin, Zhou Panghu, Yi Nianhua. Vitamin D3 attenuates high-glucose exposure-induced oxidative stress to promote osteogenic differentiation of human umbilical cord mesenchymal stem cells[J]. Chinese Journal of Tissue Engineering Research, 2024, 28(19): 2981-2987.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
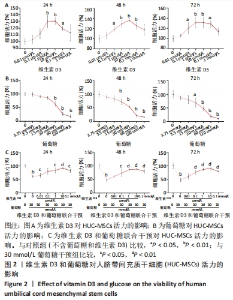
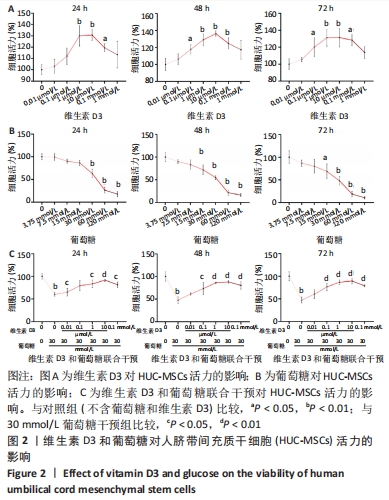
2.2 维生素D3和葡萄糖对人脐带间充质干细胞活力的影响 CCK-8检测结果表明,维生素D3在0.1 μmol/L-0.1 mmol/L范围内均能显著促进HUC-MSCs的增殖,见图2A。而葡萄糖干预以浓度依赖性在15-120 mmol/L范围内抑制HUC-MSCs生长,见图2B。结合前期文献调研结果,30 mmol/L葡萄糖能够有效模拟体外实验的高糖培养条件[21-22]。因此,在接下来的研究中,采用30 mmol/L葡萄糖干预并探究维生素D3的治疗作用。CCK-8实验结果表明,0.1 μmol/L-0.1 mmol/L维生素D3能够逆转高糖诱导的HUC-MSCs增殖抑制,且10 μmol/L维生素D3组的细胞活力最高,见图2C。根据以上研究结果,接下来的研究采用30 mmol/L葡萄糖来干预模拟高糖环境,并探索10 μmol/L维生素D3对高糖暴露后HUC-MSCs的影响。"
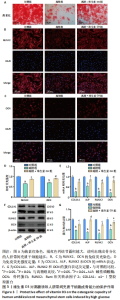
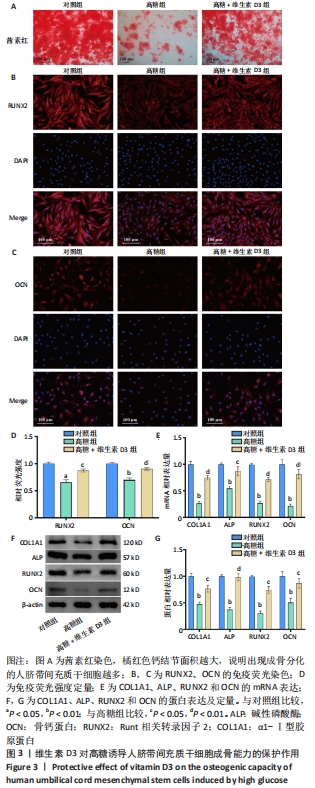
2.3 维生素D3对高糖诱导HUC-MSCs成骨能力的保护作用 茜素红染色结果显示,HUC-MSCs在成骨分化诱导14 d后,出现了大量橘红色钙结节,表明HUC-MSCs出现了成骨表型;而在高糖培养基中培养的HUC-MSCs橘红色钙结节数量显著减少、范围显著缩小,表明HUC-MSCs成骨分化受抑制,而补充维生素D3可以逆转高糖对成骨分化的不良影响,见图3A。免疫荧光染色结果显示,高糖组RUNX2和OCN的荧光强度均显著下调,而维生素D3干预增强了RUNX2和OCN的荧光表达,见图3B-D。RT-qPCR和免疫印迹结果显示,与对照组相比,高糖组成骨相关COL1A1、ALP、RUNX2和OCN的mRNA及蛋白表达下调,而维生素D3干预可以恢复其表达,见图3E-G。以上实验结果表明,高糖损害了HUC-MSCs的成骨分化潜能,而维生素D3减轻了高糖的危害。"
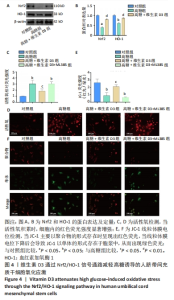
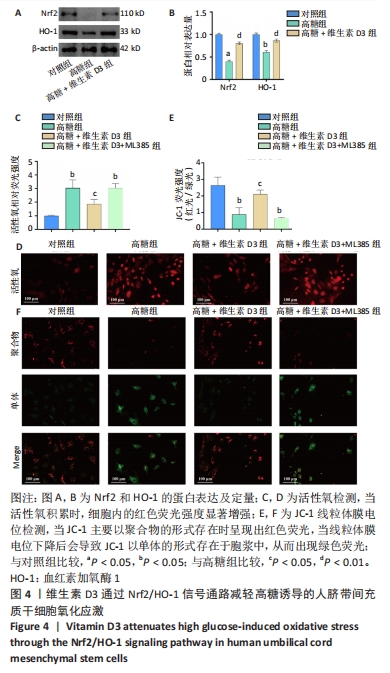
2.4 维生素D3通过Nrf2/HO-1信号通路减轻高糖诱导的HUC-MSCs氧化应激 研究表明,高糖诱导的氧化应激是干细胞功能障碍的关键机制之一,而氧化应激诱导的线粒体功能障碍和活性氧积聚会引发骨质疏松[23-26]。Nrf2/HO-1信号通路是调节氧化应激的重要通路[14,27]。通过免疫印迹实验发现,与对照组相比,高糖组Nrf2和HO-1蛋白的表达显著下降,而维生素D3处理增加了细胞中Nrf2和HO-1蛋白的表达,见图4A,B。为了进一步验证维生素D3对Nrf2/HO-1信号通路的调节作用,对HUC-MSCs使用Nrf2信号通路特异性抑制剂ML385干预[14]。活性氧检测结果表明,高糖显著增加了HUC-MSCs的荧光强度,而维生素D3降低了活性氧的产生,但加入ML385后维生素D3的治疗作用消失,见图4C,D。线粒体膜电位检测结果表明,高糖环境中HUC-MSCs呈现出较强的绿色荧光和较弱的红色荧光,表明线粒体膜电位下降,细胞处于早期凋亡阶段,见图4E,F。维生素D3干预提高了未加入ML385的HUC-MSCs的红色荧光强度,降低了绿色荧光强度,见图4E,F。以上研究结果表明,维生素D3减轻了高糖诱导的HUC-MSCs的活性氧积累和线粒体功能障碍。"
| [1] 中国老年2型糖尿病防治临床指南编写组,中国老年医学学会老年内分泌代谢分会,中国老年保健医学研究会老年内分泌与代谢分会,等.中国老年2型糖尿病防治临床指南(2022年版)[J].中华内科杂志,2022,61(1):12-50. [2] LORENTZON M, ABRAHAMSEN B. Osteoporosis epidemiology using international cohorts. Curr Opin Rheumatol. 2022;34(5):280-288. [3] 嵇星辰,王明欣,陈少华,等.中国绝经后2型糖尿病患者骨质疏松影响因素的Meta分析[J].中国全科医学,2023,26(4):504-511. [4] 柳飞扬,吴坚.糖尿病合并骨质疏松的中医研究进展[J].中国骨质疏松杂志,2023,29(1):124-128. [5] 邴学震,金智生.糖尿病性骨质疏松的中医认识及临床治疗现状[J].中国中医基础医学杂志,2019,25(11):1623-1626. [6] CAVATI G, PIRROTTA F, MERLOTTI D, et al. Role of Advanced Glycation End-Products and Oxidative Stress in Type-2-Diabetes-Induced Bone Fragility and Implications on Fracture Risk Stratification. Antioxidants (Basel). 2023;12(4):928. [7] MOHSIN S, BANIYAS MM, ALDARMAKI RS, et al. An update on therapies for the treatment of diabetes-induced osteoporosis. Expert Opin Biol Ther. 2019;19(9):937-948. [8] NAPOLI N, CHANDRAN M, PIERROZ DD, et al. Mechanisms of diabetes mellitus-induced bone fragility. Nat Rev Endocrinol. 2017;13(4):208-219. [9] MARINO S, AKEL N, LI S, et al. Reversal of the diabetic bone signature with anabolic therapies in mice. Bone Res. 2023;11(1):19. [10] CHIODINI I, GAUDIO A, PALERMO A, et al. Management of bone fragility in type 2 diabetes: Perspective from an interdisciplinary expert panel. Nutr Metab Cardiovasc Dis. 2021;31(8):2210-2233. [11] YAHAO G, XINJIA W. The Role and Mechanism of Exosomes from Umbilical Cord Mesenchymal Stem Cells in Inducing Osteogenesis and Preventing Osteoporosis. Cell Transplant. 2021;30: 9636897211057465. [12] WANG Q, XIA Q, MENG M, et al. miR-153-3p inhibits osteogenic differentiation of BMSCs by down-regulating the expression of RUNX2 in a high glucose environment. Am J Transl Res. 2022;14(10):7027-7039. [13] KLABKLAI P, PHETFONG J, TANGPORNCHAROEN R, et al. Annexin A2 Improves the Osteogenic Differentiation of Mesenchymal Stem Cells Exposed to High-Glucose Conditions through Lessening the Senescence. Int J Mol Sci. 2022;23(20):12521. [14] CHEN B, HE Q, YANG J, et al. Metformin suppresses Oxidative Stress induced by High Glucose via Activation of the Nrf2/HO-1 Signaling Pathway in Type 2 Diabetic Osteoporosis. Life Sci. 2023;312:121092. [15] KODA S, WADA K, YAMAKAWA M, et al. Associations of Plasma 25-Hydroxy Vitamin D and Dietary Vitamin D Intake with Insulin Resistance in Healthy Japanese Women. J Nutr Sci Vitaminol (Tokyo). 2023;69(1):46-52. [16] AVILA CASTILLO A, HAGEMANN T, HOFFMANN A, et al. Associations between vitamin D, immunoglobulin E concentrations, and obesity. Front Nutr. 2023;10:1147407. [17] SHARAFI SM, YAZDI M, GOODARZI-KHOIGANI M, et al. Effect of Vitamin D Supplementation on Serum 25-Hydroxyvitamin D and Homeostatic Model of Insulin Resistance Levels in Healthy Pregnancy: A Systematic Review and Meta-Analysis. Iran J Med Sci. 2023;48(1):4-12. [18] ZHAN D, ZHAO J, SHI Q, et al. 25-hydroxyvitamin D3 inhibits oxidative stress and ferroptosis in retinal microvascular endothelial cells induced by high glucose through down-regulation of miR-93. BMC Ophthalmol. 2023;23(1):22. [19] SLOBOGEAN GP, BZOVSKY S, O’HARA NN, et al. Effect of Vitamin D3 Supplementation on Acute Fracture Healing: A Phase II Screening Randomized Double-Blind Controlled Trial. JBMR Plus. 2022;7(1): e10705. [20] 中华医学会骨质疏松和骨矿盐疾病分会.维生素D及其类似物的临床应用共识[J].中华内分泌代谢杂志,2018,34(3):187-200. [21] KIM SY, LEE JY, PARK YD, et al. Hesperetin alleviates the inhibitory effects of high glucose on the osteoblastic differentiation of periodontal ligament stem cells. PLoS One. 2013;8(6):e67504. [22] ELUMALAI S, KARUNAKARAN U, MOON JS, et al. High glucose-induced PRDX3 acetylation contributes to glucotoxicity in pancreatic β-cells: Prevention by Teneligliptin. Free Radic Biol Med. 2020;160:618-629. [23] ZHAO D, LIU D, SHI W, et al. Association between Maternal Blood Glucose Levels during Pregnancy and Birth Outcomes: A Birth Cohort Study. Int J Environ Res Public Health. 2023;20(3):2102. [24] WANG Y, ZHANG L, WU Y, et al. Peptidome analysis of umbilical cord mesenchymal stem cell (hUC-MSC) conditioned medium from preterm and term infants. Stem Cell Res Ther. 2020;11(1):414. [25] TOZOUR JN, DELAHAYE F, SUZUKI M, et al. Intrauterine Hyperglycemia Is Associated with an Impaired Postnatal Response to Oxidative Damage. Stem Cells Dev. 2018;27(10):683-691. [26] HUANG Z, CHEN G, WU H, et al. Ebselen restores peri-implantitis-induced osteogenic inhibition via suppressing BMSCs ferroptosis. Exp Cell Res. 2023;427(2):113612. [27] KOU Y, RONG X, TANG R, et al. Eldecalcitol prevented OVX-induced osteoporosis through inhibiting BMSCs senescence by regulating the SIRT1-Nrf2 signal. Front Pharmacol. 2023;14:1067085. [28] XIAOLING G, SHUAIBIN L, KAILU L. MicroRNA-19b-3p promotes cell proliferation and osteogenic differentiation of BMSCs by interacting with lncRNA H19. BMC Med Genet. 2020;21(1):11. [29] ZHAO G, LUO WD, YUAN Y, et al. LINC02381, a sponge of miR-21, weakens osteogenic differentiation of hUC-MSCs through KLF12-mediated Wnt4 transcriptional repression. J Bone Miner Metab. 2022;40(1):66-80. [30] MI B, YAN C, XUE H, et al. Inhibition of Circulating miR-194-5p Reverses Osteoporosis through Wnt5a/β-Catenin-Dependent Induction of Osteogenic Differentiation. Mol Ther Nucleic Acids. 2020;21:814-823. [31] KAWABATA T, TOKUDA H, KUROYANAGI G, et al. Incretin accelerates platelet-derived growth factor-BB-induced osteoblast migration via protein kinase A: The upregulation of p38 MAP kinase. Sci Rep. 2020; 10(1):2341. [32] SUN X, KOMATSU T, LIM J, et al. Nutrient-dependent requirement for SOD1 in lifespan extension by protein restriction in Drosophila melanogaster. Aging Cell. 2012;11(5):783-793. [33] LIU Y, WANG N, ZHANG S, et al. Autophagy protects bone marrow mesenchymal stem cells from palmitate‑induced apoptosis through the ROS‑JNK/p38 MAPK signaling pathways. Mol Med Rep. 2018; 18(2):1485-1494. [34] LIU B, GAN X, ZHAO Y, et al. Inhibition of HMGB1 reduced high glucose-induced BMSCs apoptosis via activation of AMPK and regulation of mitochondrial functions. J Physiol Biochem. 2021;77(2):227-235. [35] GAO C, QIAO J, LI SS, et al. The levels of bone turnover markers 25(OH)D and PTH and their relationship with bone mineral density in postmenopausal women in a suburban district in China. Osteoporos Int. 2017;28(1):211-218. [36] WATERHOUSE M, EBELING PR, MCLEOD DSA, et al. The effect of monthly vitamin D supplementation on fractures: a tertiary outcome from the population-based, double-blind, randomised, placebo-controlled D-Health trial. Lancet Diabetes Endocrinol. 2023;11(5): 324-332. [37] UENISHI K, TOKIWA M, KATO S, et al. Stimulation of intestinal calcium absorption by orally administrated vitamin D3 compounds: a prospective open-label randomized trial in osteoporosis. Osteoporos Int. 2018;29(3):723-732. [38] MANOJ P, DERWIN R, GEORGE S. What is the impact of daily oral supplementation of vitamin D3 (cholecalciferol) plus calcium on the incidence of hip fracture in older people? A systematic review and meta-analysis. Int J Older People Nurs. 2023;18(1):e12492. [39] ELSAYYAD NME, GOMAA I, SALEM MA, et al. Efficient lung-targeted delivery of risedronate sodium/vitamin D3 conjugated PAMAM-G5 dendrimers for managing osteoporosis: Pharmacodynamics, molecular pathways and metabolomics considerations. Life Sci. 2022;309:121001. [40] XIONG Y, ZHANG Y, XIN N, et al. 1α,25-Dihydroxyvitamin D3 promotes bone formation by promoting nuclear exclusion of the FoxO1 transcription factor in diabetic mice. J Biol Chem. 2017;292(49): 20270-20280. |
| [1] | Wang Wen, Zheng Pengpeng, Meng Haohao, Liu Hao, Yuan Changyong. Overexpression of Sema3A promotes osteogenic differentiation of dental pulp stem cells and MC3T3-E1 [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 993-999. |
| [2] | Wang Shanshan, Shu Qing, Tian Jun. Physical factors promote osteogenic differentiation of stem cells [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 1083-1090. |
| [3] | Xie Ting, Liu Tingting, Zeng Xuehui, Li Yamin, Zhou Panghu, Yi Nianhua. Fucoxanthin alleviates glucocorticoid-induced osteoblast apoptosis by activating nuclear factor erythroid-2-related factor 2 [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(23): 3609-3614. |
| [4] | Han Yue, Wang Yufei, Liu Wanqing, Dong Ming, Niu Weidong. Effects of icariin on proliferation and differentiation of MC3T3-E1 cells in an inflammatory environment [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(23): 3709-3714. |
| [5] | Yuan Changshen, Liao Shuning, Li Zhe, Wu Siping, Chen Lewei, Liu Jinyi, Li Yanhong, Duan Kan. Machine learning combined with bioinformatics to identify and validate key genes for cellular senescence in osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(20): 3196-3202. |
| [6] | Wang Qian, Lu Ziang, Li Lihe, Lyu Chaoliang, Wang Meng, Zhang Cunxin. Sinomenine effectively inhibits interleukin-1beta-induced apoptosis in nucleus pulposus cells [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(2): 224-230. |
| [7] | Wu Yaru, Mi Yan, Wei Kaiyue, Gao Heping, Zhang Dingyu, Wang Caili. Regulatory effect of human umbilical cord mesenchymal stem cells on intestinal barrier function in diabetic nephropathy rats [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(19): 2967-2973. |
| [8] | Gou Qiutong, Luo Wenhao, Wang Pin, Lan Yuyan, Liu Min, Huang Haixia. Berberine promotes osteogenic differentiation of bone marrow mesenchymal stem cells in a high-glucose environment [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(19): 2974-2980. |
| [9] | Guo Qin, Wu Minmin, Tao Ying. Oxidized high-density lipoprotein promotes rat ovarian granulosa cell apoptosis through reactive oxygen species-initiated p38 signaling pathway [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(19): 3055-3060. |
| [10] | Song Yue, Shu Qing, Jia Shaohui, Tian Jun. Photobiomodulation-induced osteogenic differentiation of mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(19): 3069-3075. |
| [11] | Xie Heng, Gu Ye, Gu Yingchu, Wu Zerui, Fang Tao, Wang Qiufei, Peng Yuqin, Geng Dechun, Xu Yaozeng. Ferroptosis in bone diseases: therapeutic targets of osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(16): 2613-2618. |
| [12] | Bian Lu, Xia Dandan, Qian Yuan, Shi Wen, Que Yunduan, Lyu Long, Xu Aihua, Shi Wentao. Effects of nano-zirconium dioxide on osteogenic differentiation of ectomesenchymal stem cells in nasal mucosa [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(15): 2346-2350. |
| [13] | Zhai Haoyan, Zhao Yuan, Fan Dengying, Liu Chunyan. The role of reactive oxygen species in periodontitis and periodontal tissue regeneration [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(14): 2254-2260. |
| [14] | Wang Zhen, Xu Shunen, Tang Geng, Luo Siwei, Teng Jianxiang, Xie Mengli, He Jialin, Ye Chuan. Biocompatibility and electrical output performance of composite piezoelectric film and osteogenic differentiation of rabbit bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(13): 1969-1975. |
| [15] | Liu Zhong, Li Kewei, Wang Min, Liu Wenhui, Zhang Leilei, Guo Song, Qian Hui, Fu Qiang. Effects of micro-electric field on proliferation and osteogenic differentiation of human umbilical cord mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(13): 1983-1988. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||