Chinese Journal of Tissue Engineering Research ›› 2023, Vol. 27 ›› Issue (3): 413-419.doi: 10.12307/2023.022
Previous Articles Next Articles
Application of 3D printing technology in the precise and personalized treatment of cleft lip and palate
Jiang Haifang1, 2, Liu Rong3, Hu Peng1, 2, Chen Wei1, 2, Wei Zairong1, 2, Yang Chenglan1, 2, Nie Kaiyu1, 2
- 1Department of Burn and Plastic Surgery, Affiliated Hospital of Zunyi Medical University, Zunyi 563000, Guizhou Province, China; 2Collaborative Innovation Center of Tissue Injury Repair and Regenerative Medicine, Zunyi Medical University, Zunyi 563000, Guizhou Province, China; 3Institute of Medical Innovation and Transformation, Puren Hospital, Wuhan University of Science and Technology, Wuhan 430081, Hubei Province, China
-
Received:2021-11-11Accepted:2022-01-20Online:2023-01-28Published:2022-05-20 -
Contact:Nie Kaiyu, Master, Chief physician, Professor, Department of Burn and Plastic Surgery, Affiliated Hospital of Zunyi Medical University, Zunyi 563000, Guizhou Province, China; Collaborative Innovation Center of Tissue Injury Repair and Regenerative Medicine, Zunyi Medical University, Zunyi 563000, Guizhou Province, China -
About author:Jiang Haifang, Master candidate, Physician, Department of Burn and Plastic Surgery, Affiliated Hospital of Zunyi Medical University, Zunyi 563000, Guizhou Province, China; Collaborative Innovation Center of Tissue Injury Repair and Regenerative Medicine, Zunyi Medical University, Zunyi 563000, Guizhou Province, China -
Supported by:General Project of Natural Science Foundation of Hubei Province, No. 2020CFB548 (to LR); Hubei Provincial Key Experiment Open Fund Project for Occupational Hazard Identification and Control in 2021, No. OHIC2021G06 (to LR); Medical Research Project of Wuhan Municipal Health Commission, No. WZ20C29 (to LR)
CLC Number:
Cite this article
Jiang Haifang, Liu Rong, Hu Peng, Chen Wei, Wei Zairong, Yang Chenglan, Nie Kaiyu. Application of 3D printing technology in the precise and personalized treatment of cleft lip and palate[J]. Chinese Journal of Tissue Engineering Research, 2023, 27(3): 413-419.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks

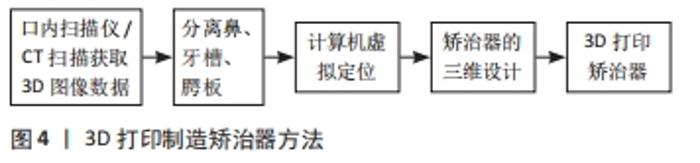
2.1 3D打印技术与唇腭裂 3D打印技术诞生于1988年[40],因其具有快速成型、精准以及个体化等优势,其被迅速运用于医学领域。自1992年STOKER等[41]首次将该技术引入整形外科,经过相关文献检索,3D打印技术最早于2006年运用于唇腭裂的精准测量上。与此同时,2006年,MIRONOV等[42]首次系统介绍生物打印这一概念,直至2017年,HIXON等[18]开始利用3D生物打印制作唇腭裂植入骨。目前3D打印技术开始广泛运用于唇腭裂治疗,其已涵盖了教育、术前设计、矫正塑形、手术模拟以及生物植入物各个方面。 2.2 3D打印在唇腭裂术前正畸及塑形中的应用 唇腭裂患者大部分存在鼻子、嘴唇和上颌弓扭曲严重和不对称的问题,单纯的手术治疗无法拥有理想的治疗效果。由此,1950年时MCNEIL[43]提出术前正畸作为唇腭裂的一种辅助治疗手段。随着研究深入方法改进,1993年,GRAYSON[44]首次提出术前鼻牙槽术前矫治器,它是由腭板、牙槽板以及附上的鼻支架组成。作为一种广泛使用的术前正畸方法,鼻牙槽成型术有着能让缩窄齿槽及腭部裂隙,恢复正常牙弓,延长鼻小柱,改善鼻部形态,并允许在最小张力下进行手术修复等优点。值得一提的是,传统鼻牙槽矫治器存在一些缺陷与不足。近年来随着计算机辅助技术的发展,3D打印的出现解决了传统矫治器存在的问题,还结合不同材料进行制作矫治器,提升了综合治疗效果[16,24,26,29,33-34,35-36,45-48],见表1。"
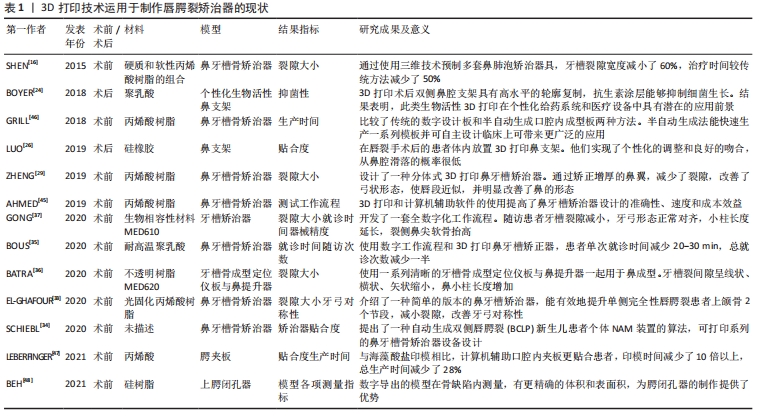
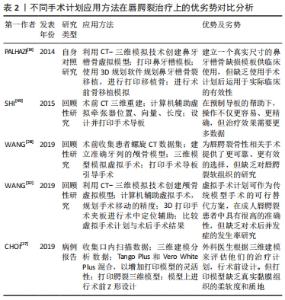
随着数字化技术的不断进步,鼻牙槽矫治器还不断创新结合各类新型工具方法,如计算机辅助方法、半自动算法和全数字化工作流程等。2019年,ZHENG等[29]设计了一种分体式鼻牙槽矫治器,其将成型板和鼻矫治器分开,有效矫正了增厚的鼻翼,减少了裂隙,改善了上颌弓以及鼻的形态。2020年,EL-GHAFOUR等[33]提出计算机辅助3D打印鼻牙槽骨矫治器,其数字可视化操作,能准确反映小儿裂区的解剖结构,为患者提供更加准确性和灵活性的设备。同年,SCHIEBL等[34]基于半自动算法对24例双侧唇腭裂患儿进行矫治器制作,随访结果表明不仅提高治疗效果,还避免了矫治器脱离上颌骨,减少了溃疡、呼吸困难等并发症。伴随着数字化技术的不断发展,在以上基础上,GONG等[37]开发了一套全数字化工作流程,用于个性化设计和制造连续系列的定制鼻牙槽骨成型器械。6个月后随访患者牙槽裂隙减小,牙弓形态正常对齐,鼻部形态明显改善。 在治疗时间与成本上,传统PNAM的典型方法是每周逐一手工修改单个器具,这意味着时间与成本高昂,尤其对居住偏远的患者大大减低了医从性。2015年,SHEN等[16]使用3D打印技术预制系列鼻牙槽骨成型器,随访发现患儿平均牙槽裂隙宽度减小了60%,治疗时间较传统方法减少了50%。随着技术迭代更新,2020年,BOUS等[35]3D打印进一步结合数字工作流程制造鼻牙槽矫正器,统计得出每次就诊时间减少20-30 min,总就诊次数减少50%。 3D打印鼻牙槽矫治器潜力是巨大的,解决了传统矫治器许多问题,但目前研究也仍存在一些潜在的弊端:①矫治器材料强度、硬度、贴合度等性质未有进一步研究;②矫治器尚无统一的制作标准及规范;③目前许多研究未针对单侧或双侧唇腭裂患者、裂隙大小等方面进行进一步的纵向研究。 2.3 3D打印在唇腭裂手术计划与模拟中的应用 唇腭裂患者的组织畸形修复一直是外科医师面临的一大挑战。通常,外科医生行唇腭裂修复术,都是使用自身经验进行手术,手术结果常良莠不齐。计算机辅助3D打印手术计划可显著简化诊断评估,并可同时模拟不同的手术过程,使得经验医学向精准医学转变成为了可能[14,27-28,32,49],见表2。 "
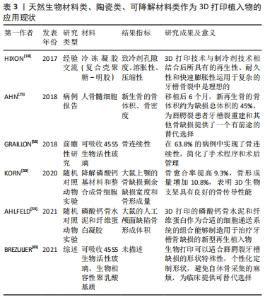
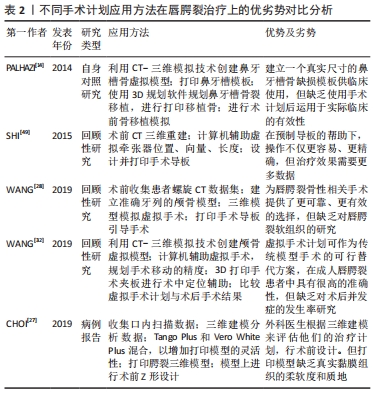

在手术指南上,2014年,PAHAZI等[14]利用3D打印模板进行模拟规划手术,克服了既往二维图像弊端,可视化复杂的牙槽骨解剖缺损,允许外科医生创建精确的解剖模型。在原有基础上,2015年,SHI等[49]利用矢状劈开截骨术与快速成型手术导板一起进行下颌牵引,对6例患儿进行术前设计和制造手术导板,使得操作更简单、精确。 在手术技术上,鉴于既往术者模拟练习的有效模型大多为尸体标本,但由于伦理限制现今可供医学使用的尸体标本已大幅减少,增加了术者习得及模拟手术的难度。而3D打印模型行术前模拟,能有效帮助术者预设计手术的技术细节,包括解剖面积和皮瓣的大小,降低了手术难度,提升了手术精准性。2019年,CHOI等[27]在3D打印模型上根据术前计划进行了一系列的手术模拟,包括Z形设计、刀片切开、皮瓣剥离和抬高以及黏膜修复等。 在转移工具上,2019年,WANG等[28]为80例唇腭裂患者设计制造不同的3D打印手术导板引导截骨,明显缩短了术前的计划步骤和手术时间。同年,还有学者将3D打印技术与计算机辅助虚拟手术进一步结合,辅助90例患者的治疗[32],该研究通过3D夹板进行术中固定与精准定位,使虚拟手术成功转移到实际手术中,较上次研究更深入,更好地帮助了虚拟技术向现实操作的转换,并且此次研究对虚拟手术计划结果与术后手术结果进行比较,得出二者差异可以忽略不计。 2.4 唇腭裂治疗中的3D打印植入物 重建牙槽骨的连续性是唇腭裂治疗中关键且极具挑战的一步[50-51]。据KASIRI等[51]相关研究发现,唇腭裂患儿牙槽骨缺损的平均体积约为620 mm3。因此,针对唇腭裂牙槽骨缺损的修复,简单的手术闭合是不够的,这就需要添加材料来填补这些关键缺陷。这些修复材料可以是天然来源的,例如自体移植物或同种异体移植物。自体骨采集部位最常见的是髂嵴[25,52]。然而,这种方法具有很大的不足,第一是患儿自体骨不足;第二是自体骨移植后第一年的高吸收率限制了其的修复效果;第三是采集自体骨具有诸多并发症,如术后疼痛、行走困难、神经损伤、血肿、感染和动脉伤口等[53-55]。 为了克服这些限制,人们一直在寻找替代自体骨移植的方法[56-57]。现今,具有可定制形状、生物相容性和生物降解性的支架已相继应用于临床[18,25,30,58-60],见表3。 "
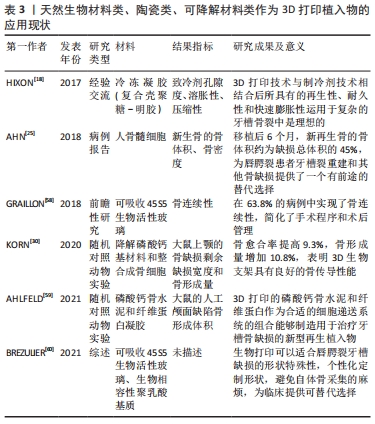


3D生物打印技术的产生为临床植入物带来了曙光。针对唇腭裂中并发的牙槽骨裂这种复杂的几何缺损,2017年,HIXON等[18]将3D打印技术与制冷剂技术相结合,制作了不同几何形状的支架。通过检验得出此支架能2 min快速填充各类复杂缺损,持久耐用且具有生物活性。由于理想生物材料稀缺,为突破这一关卡,2018年,AHN等[25]首次使用植入髂骨骨髓细胞的打印生物可吸收聚己内酯支架治疗牙槽骨缺损,此再生病例为世界上第一例。在移植后6个月,患者新再生骨的骨体积约为缺损总体积的45%,骨密度约为周围骨的75%。与此同时,更多的生物材料也相继在临床中应用,同年,GRAILLON等[58]采用人工合成的生物活性玻璃骨替代物对58例患者进行牙槽骨移植,移植后1年内2/3的病例中实现了骨连续性,获得令人满意的粘膜愈合、牙齿萌出,同时减少了止痛剂使用、缩短了平均3 d的住院时间。 此外,由于牙槽裂或腭裂的复杂性,无法通过任何临床前模型完全显示。因此许多研究者除了在临床使用研究骨移植这一课题,还人工制造了大鼠上颚的骨缺损进行动物实验,以期进行更深入的研究,攻克唇腭裂患者骨移植这一难题。2019年,KORN等[30]基于3D打印生物可降解磷酸钙基材料和整合成骨细胞的新治疗概念,进行了骨缺损移植实验。12周后随访数据显示:骨愈合率提高9.3%,骨形成量增加10.8%。2020年,AHLFELD等[59]将具有骨传导性的磷酸钙骨水泥和可作为细胞传递系统纤维蛋白凝胶进行组合用作于3D打印材料,12周后骨形成明显增加。以上研究预示着将会有更多、更优质的新型再生植入物将能于人工牙槽骨缺损修补。 近年来,3D生物打印支架为牙槽裂重建和其他骨缺损提供了一种组织工程替代方案。但大部分试验中只用于1-3例临床患者,未来研究应进一步扩大患者特异性的样本量以及涵盖更多的生物材料特性研究,例如支架孔隙度、结构特性、细胞相容性和最佳细胞接种浓度等。此外,还应增加更多新型生物材料的研究,如聚己内酯和磷酸三钙共混支架。 2.5 3D打印在唇腭裂术后正畸中的应用 手术治疗可以在一定程度上矫正患儿组织畸形,但无法完全矫正畸形组织,且随着患者年龄增长,组织会随之改变,所以术后的正畸治疗对于患者的组织形态功能恢复也非常关键。在临床中多以鼻子的畸形问题尤为明显,因此大部分患者术后都需要鼻孔支具,来帮助重建的鼻孔在愈合过程中保持形状。目前有两种类型的鼻支架:成品和基于石膏模型的定制支架。成品容易获得,但其形状标准化,提供较差的吻合和支撑,导致其从鼻腔滑脱[61]。基于鼻腔石膏模型的支架可以更好地吻合鼻子形态,但制作过程冗长复杂,人工成本高,无法在术前制作,关键支撑位置也无法根据需要进行调整。目前,唇裂术后鼻支架的使用难以满足临床需求。 因此,迫切需要一种新的方法来制作个性化的鼻支架。此类支架应吻合良好、易于制作,而3D打印是一个很好的选择。3D打印可以基于患者的三维模型,进行精准个性化的鼻托制造[62-64]。随着技术的不断进步,3D打印器具还可以装载生物活性剂以进行局部递送,使生物活性剂在体内精准局部释放,减少了相关并发症,更安全可靠[65-66]。 2018年,LUO等[26]在10例唇裂术后患者应用了3D打印鼻支架,随访6个月发现3D打印的支架能良好吻合鼻腔,不容易从鼻腔滑落,且未出现鼻黏膜刺激性症状。同年,BOYER等[24]等制造了一种个性化生物活性鼻支架,用聚乙烯吡咯烷酮-青霉素混合包被3D打印鼻支架,抗菌试验提示平均抑制区达到(15.15±0.99) mm。由以上研究结果可以得知,3D支架仍具有高水平的鼻腔轮廓一致性,贴合度高,且生物活性3D打印在个性化给药系统和医疗设备中具有良好的应用前景。 2.6 3D打印在唇腭裂手术培训与教育中的应用 与其他重建手术相比,一方面唇腭裂手术内部解剖复杂且其涉及人体面部,对人的形象外观具有较大的影响,另一方面涉及面部且多为婴幼儿患者,可操作与学习资源少,导致此类手术掌握相对困难[67-69]。随着在 3D打印技术的发展,3D打印实体模型优势明显,不仅有助于初学者了解唇腭裂解剖畸形,评估唇腭裂裂隙尺寸,还能感觉患者组织脆弱性,进行真实的切开、解剖操作和缝合组织。2016年,LIOUFAS等[17,67]发现3D打印的实物模型能够有效复制人体组织,打印相似度高、解剖准确可靠的模型。2017年,ALALI等[20]将3D打印模型教学与传统教学对比,课后测试正确率提高了44.65%。因此,在医学教育中使用 3D 打印模型来作为可视化工具,进行手术培训意义重大。 3D打印模型的教育用途不仅限于医学工作者,他们也可以作为医患沟通的工具[23,70]。目前临床使用三维超声为手术团队提供了必要的术前信息,但当前的三维重建模式主要限于在二维表面上显示。 相比之下,3D 打印的真实模型为外科医生和患者父母提供了更好的信息,通过3D打印模型能够进行更好地沟通,全面了解解剖结构和手术程序。有研究通过调查问卷证明了3D模型有效地帮助了患者父母全面了解唇裂和腭裂、腭咽功能障碍和言语障碍和牙槽骨缺损[71-72]。多项研究证明,通过3D打印模型进行的医患沟通,更好地影响患者的家庭关系,正确引导了患者及家属后续所需要的唇腭裂治疗,首诊率与持续就诊率均较前提高,也间接减少了患儿的缀学概率[20,23,73-74]。 "

| [1] STONE C. Cleft lip and palate: etiology, epidemiology, preventive and intervention strategies. Anat Physiol. 2013;4(3):1-5. [2] KALASKAR R, KALASKAR A, NAQVI FS, et al. Prevalence and evaluation of environmental risk factors associated with cleft lip and palate in a central Indian population. Pediatr Dent. 2013;35(3):279-283. [3] FAN D, WU S, LIU L, et al. Prevalence of non-syndromic orofacial clefts: based on 15, 094, 978 Chinese perinatal infants. Oncotarget. Oncotarget. 2018;9(17): 13981-13990. [4] 孙凤霞,申铁兵.非综合征性唇腭裂流行病学的研究进展[J].口腔颌面外科杂志,2014,24(2):154-157. [5] MOSMULLER D, MAAL TJ, PRAHL C, et al. Comparison of two- and three-dimensional assessment methods of nasolabial appearance in cleft lip and palate patients: Do the assessment methods measure the same outcome. J Craniomaxillofac Surg. 2017;45(8):1220-1226. [6] GATTANI S, JU X, GILLGRASS T, et al. An innovative assessment of the dynamics of facial movements in surgically managed unilateral cleft lip and palate using 4D imaging. Cleft Palate Craniofac J. 2020;57(2):1-9. [7] 姚金凤,邓梦昭,谢添,等.口腔数字化设计在唇腭裂患者前牙美学修复中的应用研究[J].华西口腔医学杂志,2021,39(5):582-590. [8] 李彪,姜腾飞,沈舜尧,等.3D打印个体化钛板在正颌手术中的应用及其准确性评价[J].中国口腔颌面外科杂志,2016,14(5):6. [9] 王敏娇,蔡鸣,姜闻博,等.双侧完全性唇腭裂鼻畸形患儿唇裂术后个性化鼻模的计算机辅助设计和制作 [J].组织工程与重建外科杂志,2021,17(2):118-121. [10] 张天嘉,王旭东.3D打印导板和个性化钛板在正颌外科合并肋骨移植术中的应用[C].第十四次中国口腔颌面外科学术会议论文汇编,2018,1(1):651-652. [11] GIANNETTI S, BIZZOTTO N, STANCATI A, et al. Minimally invasive fixation in tibial plateau fractures using an pre-operative and intra-operative real size 3D printing. Injury. 2017;48(3):784-788. [12] OOSTERKAMP BCM, MEER WJVD, RUTENFRANS M, et al. Reliability of linear measurements on a virtual bilateral cleft lip and palate model. Cleft Palate Craniofac J. 2006;43(5):519-523. [13] YU Q, GONG X, WANG G M, et al. A novel technique for presurgical nasoalveolar molding using computer-aided reverse engineering and rapid prototyping. J Craniofac Surg. 2011;22(1):142-148. [14] PALHAZI P, NEMES B, SWENNEN G, et al. Three-dimensional simulation of the nasoalveolar cleft defect. Cleft Palate Craniofac J. 2014;51(5):593-596. [15] ZHENG Y, LU B, ZHANG J, et al. CAD/CAM silicone simulator for teaching cheiloplasty: description of the technique. Br J Oral Maxillofac Surg. 2015;53(2): 194-196. [16] SHEN C, YAO CA, MAGEE W 3rd, et al. Presurgical nasoalveolar molding for cleft lip and palate: the application of digitally designed molds. Plast Reconstr Surg. 2015;135(6):1007e-1015e. [17] LIOUFAS PA, QUAYLE MR, LEONG JC, et al. 3D printed models of cleft palate pathology for surgical education. Plast Reconstr Surg Glob Open. 2016;4(9):e1029. [18] HIXON KR, MELVIN AM, LIN AY, et al. Cryogel scaffolds from patient-specific 3D-printed molds for personalized tissue-engineered bone regeneration in pediatric cleft-craniofacial defects. J Biomater Appl. 2017;32(5):598-611. [19] KASAVEN CP, MCINTYRE GT, MOSSEY PA. Accuracy of both virtual and printed 3-dimensional models for volumetric measurement of alveolar clefts before grafting with alveolar bone compared with a validated algorithm: a preliminary investigation. Br J Oral Maxillofac Surg. 2017;55(1):31-36. [20] ALALI AB, GRIFFIN MF, CALONGE WM, et al. Evaluating the use of cleft lip and palate 3D-printed models as a teaching aid. J Surg Educ. 2018;75(1):200-208. [21] DU F, LI B, YIN N, et al. Volumetric analysis of alveolar bone defect using three-dimensional-printed models versus computer-aided engineering. J Craniofac Surg. 2017;28(2):383-386. [22] REIGHARD CL, GREEN K, ROONEY DM, et al. Development of a novel, low-cost, high-fidelity cleft lip repair surgical simulatorusing computer-aided design and 3-Dimensional printing. JAMA Facial Plastic Surg. 2018;12(1):77-79. [23] NICOT R, COULY G, FERRI J, et al. Three-dimensional printed haptic model from a prenatal surface-rendered oropalatal sonographic view: a new tool in the surgical planning of cleft lip/palate. Int J Oral Maxillofac Surg. 2018;47(1):44-47. [24] BOYER CJ, WOERNER JE, GALEA C, et al. Personalized bioactive nasal supports for postoperative cleft rhinoplasty. J Oral Maxillofac Surg. 2018;76(7):1562 e1-1562 e5. [25] AHN G, LEE JS, YUN WS, et al. Cleft alveolus reconstruction using a three-dimensional printed bioresorbable scaffold with human bone marrow cells. J Craniofac Surg. 2018;29(7):1880-1883. [26] LUO D, LI T, WANG H, et al. Three-dimensional printing of personalized nasal stents for patients with cleft lip. Cleft Palate Craniofac J. 2019;56(4):521-524. [27] CHOI YS, SHIN HS. Preoperative planning and simulation in patients with cleft palate using intraoral three-dimensional scanning and printing. J Craniofac Surg. 2019;30(7):2245-2248. [28] WANG Y, ZHANG Z, LIU Y, et al. Virtual Surgical Planning Assisted Management for Cleft-Related Maxillary Hypoplasia. J Craniofac Surg. 2019;30(6):1745-1749. [29] ZHENG J, HE H, KUANG W, et al. Presurgical nasoalveolar molding with 3D printing for a patient with unilateral cleft lip, alveolus, and palate. Am J Orthod Dentofacial Orthop. 2019;156(3):412-419. [30] KORN P, AHLFELD T, LAHMEYER F, et al. 3D printing of bone grafts for cleft alveolar osteoplasty - in vivo evaluation in a preclinical model. Front Bioeng Biotechnol. 2020;8:217. [31] RIEDLE H, BURKHARDT AE, SEITZ V, et al. Design and fabrication of a generic 3D-printed silicone unilateral cleft lip and palate model. J Plast Reconstr Aesthet Surg. 2019;72(10):1669-1674. [32] WANG Y, LI J, XU Y, et al. Accuracy of virtual surgical planning-assisted management for maxillary hypoplasia in adult patients with cleft lip and palate. J Plast Reconstr Aesthet Surg. 2020;73(1):134-140. [33] EL-GHAFOUR MA, ABOULHASSAN MA, FAYED MMS, et al. Effectiveness of a novel 3D-Printed Nasoalveolar Molding Appliance(D-NAM) on improving the maxillary arch dimensions in unilateral cleft lip and palate infants: a randomized controlled trial. Cleft Palate Craniofac J. 2020;57(12):1370-1381. [34] SCHIEBL J, BAUER FX, GRILL F, et al. RapidNAM: algorithm for the semi-automated generation of nasoalveolar molding device designs for the presurgical treatment of bilateral cleft lip and palate. IEEE Trans Biomed Eng. 2020;67(5):1263-1271. [35] BOUS RM, KOCHENOUR N, VALIATHAN M. A novel method for fabricating nasoalveolar molding appliances for infants with cleft lip and palate using 3-dimensional workflow and clear aligners. Am J Orthod Dentofacial Orthop. 2020;158(3):452-458. [36] BATRA P, GRIBEL BF, ABHINAV BA, et al. OrthoAligner “NAM”: A Case Series of Presurgical Infant Orthopedics (PSIO) Using Clear Aligners. Cleft Palate Craniofac J. 2020;57(5):646-655. [37] GONG X, DANG R, XU T, et al. Full digital workflow of nasoalveolar molding treatment in infants with cleft lip and palate. J Craniofac Surg. 2020;31(2):367-371. [38] XEPAPADEAS AB, WEISE C, FRANK K, et al. Technical note on introducing a digital workflow for newborns with craniofacial anomalies based on intraoral scans- part II: 3D printed Tubingen palatal plate prototype for newborns with Robin sequence. BMC Oral Health. 2020;20(1):171. [39] EL-ASHMAWI NA, FAYED MMS, EL-BEIALY A, et al. Evaluation of the clinical effectiveness of nasoalveolar molding (NAM) using grayson method versus computer-aided design NAM (CAD/NAM) in infants with bilateral cleft lip and palate:a randomized clinical trial. Cleft Palate Craniofac J. 2021. doi:10.1177/1055665621990152. [40] JACOBS PF. Rapid prototyping & manufacturing-fundamentals of stereo lithography. Soci of Manu Eng, 1992. [41] STOKER NG, MANKOVICH NJ, VALENTINO D. Stereolithographic models for surgical planning: preliminary report. J Oral Maxillofac Surg. 1992;50(5):466-471. [42] MIRONOV V, REIS N, DERBY B. Bioprinting: a beginning. Tissue Eng. 2006;12(4):631-634. [43] MCNEIL CK. Orthodontic procedures in the treatment of congenital cleft palate. Dent Rec. 1950;70(5):126-132. [44] GRAYSON B. Presurgical nasoalveolar molding in infants with cleft lip and palate. Cleft Palate Craniofac J. 1999. [45] AHMED MK, AHSANUDDIN S, RETROUVEY JM, et al. Fabrication of nasoalveolar molding devices for the treatment of cleft lip and palate, using stereolithography additive manufacturing processes and computer-aided design manipulation software. J Craniofac Surg. 2019;30(8):2604-2608. [46] GRILL FD, RITSCHL LM, BAUER FX, et al. A semi-automated virtual workflow solution for the design and production of intraoral molding plates using additive manufacturing:the first clinical results of a pilot-study. Sci Rep. 2018;8(1):30-45. [47] LEBERFINGER A N, JONES C M, MACKAY D R, et al. Computer-aided design and manufacture of intraoral splints: a potential role in cleft care. J Surg Res. 2021; 261:173-178. [48] BEH YH, FAROOK TH, JAMAYET NB, et al. Evaluation of the differences between conventional and digitally developed models used for prosthetic rehabilitation in a case of untreated palatal cleft. Cleft Palate Craniofac J. 2021;58(3):386-390. [49] SHI L, LIU W, YIN L, et al. Surgical guide assistant mandibular distraction osteogenesis and sagittal split osteotomy in the treatment of hemifacial microsomia. J Craniofac Surg. 2015;26(2):498-500. [50] 蔡鸣,赵欣然,蒋胜杰,等.三维打印手术导板在偏颌畸形正颌外科治疗中的初步应用[J].中华医学美学美容杂志,2020,26(1):36-39. [51] KASIRI N, BAYANI M, MOHAMMAD-RABEI E, et al. Correlation between alveolar cleft volume and alveolar bone quality in patients with unilateral cleft lip and palate: a cone-beam computed tomography study. J Stomatol Oral Maxillofac Surg. 2021. doi:10.1016/j.jormas. 2021.06.013. [52] CHANG DK, KANACK M, PRETORIUS D, et al. Ultrasound evaluation of primary alveolar grafting in cleft lip/palate treatment: development of a novel sonographic grading system. Cleft Palate Craniofac J. 2016;53(5):614-621. [53] SEQUERA-RAMOS L, RUBY JM, JACKSON OA, et al. Continuous transversalis fascia plane catheter infusion in a pediatric patient undergoing alveolar cleft repair with iliac crest bone graft: a case report. A A Pract. 2019;13(5):162-165. [54] CHANG BL, WILSON AJ, CHIN BC, et al. Influence of standardized orientation on patient perception of perioperative care following alveolar cleft repair: a survey based study of patients treated in a large academic medical center. Cleft Palate Craniofac J. 2016;54(3):287-294. [55] TACHE A, MOMMAERTS MY. Pain management at iliac donor sites after grafting of alveolar clefts. Int J Oral Maxillofac Surg. 2022;51(1):62-69. [56] LIANG F, LELAND H, JEDRZEJEWSKI B, et al. Alternatives to autologous bone graft in alveolar cleft reconstruction. J Craniofac Surg. 2018;23(6):323-333. [57] WU C, PAN W, FENG C, et al. Grafting materials for alveolar cleft reconstruction:a systematic review and best-evidence synthesis. Int J Oral Maxillofac Surg. 2017; 47(3):345-356. [58] GRAILLON N, DEGARDIN N, FOLETTI JM, et al. Bioactive glass 45S5 ceramic for alveolar cleft reconstruction, about 58 cases. J Craniomaxillofac Surg. 2018;46(10):1772-1776. [59] AHLFELD T, LODE A, RICHTER RF, et al. Toward biofabrication of resorbable implants consisting of a calcium phosphate cement and fibrin-A characterization in vitro and in vivo. Int J Mol Sci. 2021;22(3):243-254. [60] BRÉZULIER D, CHAIGNEAU L, JEANNE S, et al. The challenge of 3D bioprinting of composite natural polymers pla/bioglass: trends and benefits in cleft palate surgery. Biomedicines. 2021;9(11):1553. [61] 周侠,马莲.可吸收材料内固定用于单侧唇裂鼻畸形二期修复手术的效果[J].中华医学美学美容杂志,2019,25(2):129-132. [62] CHAE MP, ROZEN WM, MCMENAMIN PG, et al. Emerging applications of bedside 3d printing in plastic surgery. Front Surg. 2015;2(2):18-25. [63] WU CS. Modulation, functionality, and cytocompatibility of three-dimensional printing materials made from chitosan-based polysaccharide composites. Mater Sci Eng C Mater Biol Appl. 2016;69:27-36. [64] MARRO A, BANDUKWALA T, MAK W. Three-dimensional printing and medical imaging:a review of the methods and applications. Curr Probl Diagn Radiol. 2016; 45(1):2-9. [65] YUE J, ZHAO P, GERASIMOV JY, et al. 3D-printable antimicrobial composite resins. Adv Funct Mater. 2015;25(43):6756-6767. [66] SANDLER N, SALMELA I, FALLARERO A, et al. Towards fabrication of 3D printed medical devices to prevent biofilm formation. Int J Pharm. 2014;459(1-2):62-64. [67] COTE V, SCHWARTZ M, ARBOUIN VARGAS JF, et al. 3-Dimensional printed haptic simulation model to teach incomplete cleft palate surgery in an international setting. Int J Pediatr Otorhinolaryngol. 2018;113(1):292-197. [68] ZHENG Y, LU B, ZHANG J, et al. CAD/CAM silicone simulator for teaching cheiloplasty:description of the technique. Br J Oral Maxillofac Surg. 2015;53(2): 194-196. [69] REIGHARD CL, GREEN K, ROONEY DM, et al. Development of a novel, low-cost, high-fidelity cleft lip repair surgical simulator using computer-aided design and 3-Dimensional printing. JAMA Facial Plast Surg. 2018;21(1):77-79. [70] LOU Y, CAI L, WANG C, et al. Comparison of traditional surgery and surgery assisted by three dimensional printing technology in the treatment of tibial plateau fractures. Int Orthop. 2017;41(9):1875-1880. [71] CHOU PY, HALLAC RR, SHIH E, et al. 3D-printed models of cleft lip and palate for surgical training and patient education. Cleft Palate Craniofac J. 2018;55(3):323-327. [72] CHOU PY, DENADAI R, HALLAC RR, et al. Comparative volume analysis of alveolar defects by 3D simulation. J Clin Med. 2019;8(9):1401. [73] SCHLUND M, LEVAILLANT JM, NICOT R. Three-dimensional printing of prenatal ultrasonographic diagnosis of cleft lip and palate:presenting the needed “know-how” and discussing its use in parental education. Cleft Palate Craniofac J. 2020; 57(8):1041-1044. [74] COTÉ J, THOMAS B, MARVIN J. Improved maternal bonding with the use of 3D-printed models in the setting of a facial cleft. J 3D Print Med. 2018;2(3):97-102. [75] LIAW CY, GUVENDIREN M. Current and emerging applications of 3D printing in medicine. Biofabrication. 2017;9(2):102-121. [76] 王亚男,王芳辉,汪中明,等.4D打印的研究进展及应用展望[J].航空材料学报,2018,38(2):70-76. [77] 宋波,卓林蓉,温银堂,等.4D打印技术的现状与未来[J].电加工与模具, 2018,6(1):1-7, 30. |
| [1] | Wang Menghan, Qi Han, Zhang Yuan, Chen Yanzhi. Three kinds of 3D printed models assisted in treatment of Robinson type II B2 clavicle fracture [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1403-1408. |
| [2] | Yang Yufang, Yang Zhishan, Duan Mianmian, Liu Yiheng, Tang Zhenglong, Wang Yu. Application and prospects of erythropoietin in bone tissue engineering [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1443-1449. |
| [3] | Wang Shanshan, Shu Qing, Tian Jun. Physical factors promote osteogenic differentiation of stem cells [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(7): 1083-1090. |
| [4] | Ning Tianliang, Wang Kun, Wang Lingbiao, Han Pengfei. Finite element analysis on correction effect of varus foot orthosis based on the three-point force principle [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 891-899. |
| [5] | Shen Ziqing, Xia Tian, Shan Yibo, Zhu Ruijun, Wan Haoxin, Ding Hao, Pan Shu, Zhao Jun. Vascularized tracheal substitutes constructed by exosome-load hydrogel-modified 3D printed scaffolds [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(5): 697-705. |
| [6] | Zhu Liwei, Wang Jiangyue, Bai Ding. Application value of nanocomposite gelatin methacryloyl hydrogels in different bone defect environments [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(5): 753-758. |
| [7] | Wang Jiani, Chen Junyu. Angiogenesis mechanism of metal ions and their application in bone tissue engineering [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(5): 804-812. |
| [8] | Li Yulin, Yu Haipeng, Tang Huajing, Zhang Zitong, Lin Xingnan. The mechanism, safety and application of berberine in promoting bone regeneration [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(35): 5702-5708. |
| [9] | Liu Penghui, Wu Fan, Wang Zejie, Wu Gaoyi, Zhou Libo. Constructing an animal model of temporomandibular joint osteoarthritis in Sprague-Dawley rats by digital technology [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(35): 5642-5648. |
| [10] | Shang Yonghui, Li Shuai, Liu Yicong, Zhao Qihang, Liu Wen. Three-dimensional finite element study on the effect of posterior tooth forward movement on temporomandibular joint stress in orthodontic reduction patients [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(34): 5516-5520. |
| [11] | Zhang Aili, Huang Jiazheng, Fan Wen, Li Yihuan, Li Shuang, Gan Xuewen, Xiong Ying. Establishing equivalent model to verify the precision of personalized bone model rapidly [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(30): 4795-4799. |
| [12] | Kong Xiangyu, Wang Xing, Pei Zhiwei, Chang Jiale, Li Siqin, Hao Ting, He Wanxiong, Zhang Baoxin, Jia Yanfei. Biological scaffold materials and printing technology for repairing bone defects [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(3): 479-485. |
| [13] | Li Zhiyao, Hu Zheng, Li Xuan, Lu Peijun. Effects of enamel adhesives with different components on Porphyromonas gingivalis and Streptococcus mutans [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(3): 329-335. |
| [14] | Xu Xiaodong, Zhou Jiping, Zhang Qi, Feng Chen, Zhu Mianshun, Shi Hongcan. 3D printing process of gelatin/oxidized nanocellulose skin scaffold with high elastic modulus and high porosity [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(3): 398-403. |
| [15] | Gao Xueyu, Zhang Wentao, Sun Tianze, Zhang Jing, Li Zhonghai. Application of metal ions in bone tissue engineering [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(3): 439-444. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||