Design
Imaging experiment.
Time and setting
It was completed in the Digital Medical Center of Inner Mongolia Medical University in June, 2018.
Patients
A 17-year-old female patient (163 cm, 52 kg) who visited the Department of Spine Surgery (Exclusion of other spinal disorders (congenital spina bifida, spinal trauma, tumors, and tuberculosis), the Second Affiliated Hospital of Inner Mongolia Medical University for AIS was selected.
All experiments were approved by the Ethics Committee of Inner Mongolia Medical University in April 2014 (approval No. 20140408). Informed consent was provided by the patient and her parents to volunteer as a research subject. Cobb angle of major thoracic scoliosis was 58°, and that of compensatory lumbar scoliosis was 32°. The scoliosis was classified as Lenke typeI, King type II, and PUMC type IIb. Risser sign was grade 3. The patient had no previous history of spinal trauma or surgery. Full-length standing anteroposterior and lateral radiographs and supine side-bending radiographs were taken. Spine and spinal cord abnormalities were excluded by whole-spine MRI. Finally, AIS was confirmed by the above imaging results as well as medical history.
CT scanner and computer
A 16-slice GE Medical System Brilliance CT scanner was used with the following scan parameters: slice thickness 1.0 mm, tube voltage 200 mA, voltage 120 kv, and scan range C7-S1. A total of 578 slices were scanned. Images were processed and stored in the CT workstation, and then saved in DICOM format on a removable hard disk.
An Acer Desktop PC (CPU: Intel E6600; CPU clock speed: 3.2 GHz; internal memory: 4 GB DDR3 1333 MHz; video memory: 1G; hard drive: 1T; 21.5” LCD screen; operating system: Windows XP) was used.
3D image analysis software
Mimics 16.01 software (Materialise, Belgium) was provided by the Digital Medical Center of Inner Mongolia Medical University.
Data output, import, and reconstruction
Images of each slice were analyzed and compared using the imaging workstation. Gray scale was adjusted in bone window. The resulting clear images were stored on the removable hard drive. Next, the images were imported from the removable hard drive into Mimics 16.01, and registered in anterior, posterior, left, and right directions. Bone tissues were displayed by setting the threshold. Bone tissue boundaries automatically identified by the software were added and removed by the Graphical Editing function. Cavities in the cancellous bone were filled. Finally, modified images of each slice were superimposed using the 3D reconstruction function to reconstruct the 3D images of T1-T12 vertebrae and the corresponding costal heads. In addition, the relevant parameters were measured using the 3D measurement tool of the software (Mimics16.0, University of Louvain, Belgien).
Screw modeling
The STL file of a vertebral screw (Weigao posterior thoracolumbar fixation system, provided by Shandong Weigao Orthopedic Device Company Limited; Figure 1) with a diameter of 5.0 mm and length 50.0 mm constructed in reverse engineering design software was imported into the model. 3D registration was performed by 3D rotation of thoracic pedicle-rib unit, and the bony model was transparentized. The screw position was then registered based on the boundary structure of the mask (Figure 1, Table 1).
.jpg)
Preoperative simulation design of screw diameter and 3D printing navigation template of screw in pedicle unit fixation for idiopathic scoliosis
The width at the narrowest point of pedicle in each fixed segment was measured via 3D rotation of a single vertebra to different angles. The measured width was the diameter of the selected screw. According to the measurement results, the parameters of screw diameter were designed, and the 3D vertebrae model was imported to simulate screw placement and observe whether the pedicle unit was penetrated and navigation templates of screw were printed by Dimension Elite (SD Co., USA).
Preoperative simulation design of screw length in pedicle fixation for idiopathic scoliosis
The direction of screw placement was adjusted via 3D rotation of a single vertebra to different angles, so that the axis of the screw was coincident with the axis of pedicle, and the leading edge of the screw reached, but not penetrated the cortex of anterior vertebral edge. The effective fixation length traveled by the screw was measured using the 3D measurement tool.
The direction of screw placement was adjusted
via 3D rotation of a single vertebra to different angles, so that the axis of the screw was coincident with the axis of pedicle, and the leading edge of the screw reached, but not penetrated the cortex of anterior vertebral edge. As measured by the “Measure 3D distance” function, the angle between the screw axis and the sagittal plane was the lateral angle, and that to the horizontal plane was the upward (downward) angle (
Figures 2-
5).
.jpg)
.jpg)
Clinical operation
Preoperative individualized operation planning
Totally 24 screws were inserted into thoracic pedicles of T1-T12 with the assistance of preoperative 3D digital reconstruction: T2 1 screw, T3 1 screw, T4 2 screws, T5 1 screw, T6 1 screw, T7 2 screws, T8 2 screws, T9 2 screws, T10 2 screws, T11 2 screws,T12 2 screws, L1 2 screws, L2 2 screws and L3 2 screws.
Internal fixation devices and operation parameter
Two internal fixation systems were used: China Great Wall and Weigao pedicle screw systems. The diameter and length of screws were 3.5-10.0 mm and 20-100 mm, respectively (
Table 2).
.jpg)
Operation procedure
Thoracolumbar thin-section scanning was performed using the 16-slice GE Medical System Brilliance CT scanner at a tube voltage of 200 mA, voltage of 120 kV, and thickness of 0.625 mm. Screws were placed according to the plan developed from 3D digital reconstruction simulation (including screw depth, lateral angle, screw diameter selection, and other parameters) and navigation template of screw.
Evaluation methods
The fixation process and intraoperative and postoperative symptoms were recorded. Four grades were defined according to the screw position
[10]: Grade I: the screw was completely within the pedicle; grade II: the screw penetrated the pedicle wall by < 2 mm; grade III: the screw penetrated the pedicle wall by ≥ 2 mm but < 4 mm; and grade IV: the screw penetrated the pedicle wall by ≥ 4 mm. Grades I, II, and II screws that penetrated from the lateral pedicle wall but entered into the vertebral body from the medial sternocostal joint were acceptable. Grade III screws that penetrated from the medial, upper, and lower pedicle walls and grade IV screws were unacceptable.
Main outcome
The number of cases of screw penetrating cortical bone was observed.
.jpg)
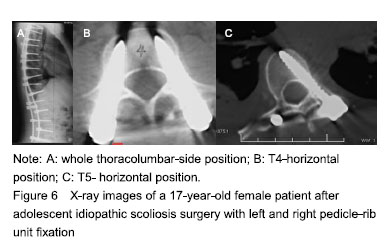
.jpg)
.jpg)
.jpg)
.jpg)
.jpg) #br#
#br#
#br#
#br#